Abstract
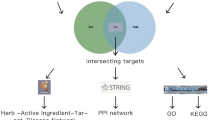
This study was to evaluate the potential mechanism of action of Artemisia annua L. (A. annua) in the treatment of acute myocardial infarction (AMI) using network pharmacology, molecular docking and in vivo experiments. 22 active chemical compounds and 193 drug targets of A. annua were screened using the Traditional Chinese Medicine System Pharmacological (TCMSP) database. 3876 disease targets were also collected. Then 158 intersection targets between AMI and A. annua were obtained using R 4.2.0 software. String database was used to construct the protein–protein interaction (PPI) network and 6 core targets (MAPK1, TP53, HSP90AA1, RELA, AKT1, and MYC) were screened. Gene Ontology (GO) enrichment analysis and Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway analysis were performed using the R package. GO enrichment results were mainly related to cell responses to chemical stress and cell membrane microregions. KEGG pathways were mainly involved in lipids, atherosclerosis and fluid shear stress. In addition, molecular docking between A. annua active compounds and core targets showed high binding activity. As for in vivo validation, A. annua extract showed significant effects on improving post-infarction ventricular function, delaying ventricular remodeling, and reducing myocardial fibrosis and apoptosis. This study has revealed the potential components and molecular mechanisms of A. annua in the treatment of AMI. Our work also showed that A. annua has great effect on reducing myocardial fibrosis and scar area after infarction.










Similar content being viewed by others
Availability of data and materials
The data used to support the findings of this study are available from the corresponding author upon request.
Abbreviations
- A. annua :
-
Artemisia annua L.
- ADME:
-
Absorption, distribution, metabolism, excretion
- AGEs:
-
Advanced glycation end products
- AMI:
-
Acute myocardial infarction
- BP:
-
Biological process
- BC:
-
Betweenness centrality
- CC:
-
Cellular component
- CVD:
-
Cardiovascular disease
- DC:
-
Degree centrality
- DL:
-
Drug-likeness
- DTBT:
-
Door-to-balloon time
- DTNT:
-
Door-to-needle time
- EC:
-
Eigenvector centrality
- EF:
-
Ejection fraction
- FS:
-
Fractional shortening
- GO:
-
Gene ontology
- I/R:
-
Ischemia–reperfusion
- KEGG:
-
Kyoto encyclopedia of genes and genomes
- LAC:
-
Local average-connectivity-based centrality
- LAD:
-
Left anterior descending coronary artery
- LV:
-
Left Ventricular function
- LVEDP:
-
LV end-diastolic pressure
- LVSP:
-
Peak systolic LV pressure
- MF:
-
Molecular function
- MMP-2:
-
Matrix metalloproteinase-2
- MPTPs:
-
Mitochondrial permeability transition pores
- NC:
-
Network centrality
- OB:
-
Oral Bioavailability
- OMIM:
-
Online Mendelian inheritance in man
- PPI:
-
Protein–protein interaction
- STRING:
-
Search tool for the retrieval of interacting genes database
- TCM:
-
Traditional Chinese medicine
- TCMSP:
-
Traditional Chinese medicine systems pharmacology database and analysis platform
- TGF-β1:
-
Transforming growth factor-β1
References
Zhao D, Liu J, Wang M, Zhang X, Zhou M (2019) Epidemiology of cardiovascular disease in China: current features and implications. Nat Rev Cardiol 16(4):203–212. https://doi.org/10.1038/s41569-018-0119-4
Chen W-W, Gao R-L, Liu L-S, Zhu M-L, Wang W, Wang Y-J, Wu Z-S, Li H-J, Gu D-F, Yang Y-J (2017) China cardiovascular diseases report 2015: a summary. J Geriatr Cardiol 14(1):1–10. https://doi.org/10.11909/j.issn.1671-5411.2017.01.012
Wan X, Ren H, Ma E, Yang G (2018) Mortality trends for ischemic heart disease in China: an analysis of 102 continuous disease surveillance points from 1991 to 2009. BMC Public Health 18(1):1–9. https://doi.org/10.1186/s12889-017-4558-3
Li H, Ge J (2015) Cardiovascular diseases in China: current status and future perspectives. IJC Heart Vasc 6:25–31
Wu Y, Benjamin EJ, MacMahon S (2016) Prevention and control of cardiovascular disease in the rapidly changing economy of China. Circulation 133(24):2545–2560. https://doi.org/10.1161/CIRCULATIONAHA.115.008728
Li J, Li X, Wang Q, Hu S, Wang Y, Masoudi FA, Spertus JA, Krumholz HM, Jiang L (2015) ST-segment elevation myocardial infarction in China from 2001 to 2011 (the China PEACE-Retrospective Acute Myocardial Infarction Study): a retrospective analysis of hospital data. Lancet (London, England) 385(9966):441–451. https://doi.org/10.1016/S0140-6736(14)60921-1
Zhang Q, Zhao D, Xie W, Xie X, Guo M, Wang M, Wang W, Liu W, Liu J (2016) Recent trends in hospitalization for acute myocardial infarction in Beijing: increasing overall burden and a transition from ST-segment elevation to non-ST-segment elevation myocardial infarction in a population-based study. Medicine. https://doi.org/10.1097/MD.0000000000002677
Liu S, Li Y, Zeng X, Wang H, Yin P, Wang L, Liu Y, Liu J, Qi J, Ran S (2019) Burden of cardiovascular diseases in China, 1990–2016: findings from the 2016 global burden of disease study. JAMA Cardiol 4(4):342–352. https://doi.org/10.1001/jamacardio.2019.0295
Ma LY, Chen WW, Gao RL, Liu LS, Zhu ML, Wang YJ, Wu ZS, Li HJ, Gu DF, Yang YJ, Zheng Z, Hu SS (2020) China cardiovascular diseases report 2018: an updated summary. J Geriatr Cardiol 17(1):1–8. https://doi.org/10.11909/j.issn.1671-5411.2020.01.001
Collet JP, Thiele H, Barbato E, Barthélémy O, Bauersachs J, Bhatt DL, Dendale P, Dorobantu M, Edvardsen T, Folliguet T, Gale CP, Gilard M, Jobs A, Jüni P, Lambrinou E, Lewis BS, Mehilli J, Meliga E, Merkely B, Mueller C, Roffi M, Rutten FH, Sibbing D, Siontis GCM (2021) 2020 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Eur Heart J 42(14):1289–1367. https://doi.org/10.1093/eurheartj/ehaa575
Dhaliwal H, Kirshenbaum LA, Randhawa AK, Singal PK (1991) Correlation between antioxidant changes during hypoxia and recovery on reoxygenation. Am J Physiol 261(3):632–638. https://doi.org/10.1152/ajpheart.1991.261.3.H632
Kalogeris T, Baines CP, Krenz M, Korthuis RJ (2016) Ischemia/reperfusion. Compr Physiol 7(1):113. https://doi.org/10.1002/cphy.c160006
Hausenloy DJ, Yellon DM (2013) Myocardial ischemia-reperfusion injury: a neglected therapeutic target. J Clin Invest 123(1):92–100. https://doi.org/10.1172/JCI62874
Park CY, Choi E, Yang HJ, Ho SH, Park SJ, Park KM, Kim SH (2020) Efficacy of Artemisia annua L. extract for recovery of acute liver failure. Food Sci Nutr 8(7):3738–3749. https://doi.org/10.1002/fsn3.1662
Brown GD (2010) The biosynthesis of artemisinin (Qinghaosu) and the phytochemistry of Artemisia annua L. (Qinghao). Molecules 15(11):7603–7698. https://doi.org/10.3390/molecules15117603
Xiaoyan L, Jianguo C, Guozheng H, Qingjie Z, Jingshan S (2019) Biological activities of artemisinin derivatives beyond malaria. Curr Top Med Chem 19(3):205–222. https://doi.org/10.2174/1568026619666190122144217
Feng X, Cao S, Qiu F, Zhang B (2020) Traditional application and modern pharmacological research of Artemisia annua L. Pharmacol Ther 216:107650
Brisibe EA, Umoren UE, Brisibe F, Magalhäes PM, Ferreira JF, Luthria D, Wu X, Prior RL (2009) Nutritional characterisation and antioxidant capacity of different tissues of Artemisia annua L. Food Chem 115(4):1240–1246. https://doi.org/10.1016/J.FOODCHEM.2009.01.033
Ryu J-H, Lee S-J, Kim M-J, Shin J-H, Kang S-K, Cho K-M, Sung N-J (2011) Antioxidant and anticancer activities of Artemisia annua L. and determination of functional compounds. J Korean Soc Food Sci Nutr 40(4):509–516. https://doi.org/10.3746/jkfn.2011.40.4.509
Yang M, Guo M-y, Luo Y, Yun M-d, Yan J, Liu T, Xiao C-h (2017) Effect of Artemisia annua extract on treating active rheumatoid arthritis: a randomized controlled trial. Chin J Integr Med 23:496–503. https://doi.org/10.1007/s11655-016-2650-7
Wang X, Wang T, Ding S, Ma Y-L (2021) Xin Su Ning—a review of basic and clinical pharmacology integrated with traditional Chinese medicine antiarrhythmic theory. Front Pharmacol. https://doi.org/10.3389/fphar.2021.657484
Kadioglu O, Klauck SM, Fleischer E, Shan L, Efferth T (2021) Selection of safe artemisinin derivatives using a machine learning-based cardiotoxicity platform and in vitro and in vivo validation. Arch Toxicol 95(7):2485–2495. https://doi.org/10.1007/s00204-021-03058-4
Gu Y, Wang X, Yuan M, Wu G, Hu J, Tang Y, Huang C (2012) Artemisinin attenuates post-infarct myocardial remodeling by down-regulating the NF-κB pathway. Tohoku J Exp Med 3:227. https://doi.org/10.1620/tjem.227.161
Wang F, Gao Q, Yang J, Wang C, Fu L (2020) Artemisinin suppresses myocardial ischemia–reperfusion injury via NLRP3 inflammasome mechanism. Mol Cell Biochem. https://doi.org/10.1007/s11010-020-03842-3
Wang Y, Fan X, Qu H, Gao X, Cheng Y (2012) Strategies and techniques for multi-component drug design from medicinal herbs and traditional Chinese medicine. Curr Top Med Chem 12(12):1356–1362. https://doi.org/10.2174/156802612801319034
Zhang R, Zhu X, Bai H, Ning K (2019) Network pharmacology databases for traditional Chinese medicine: review and assessment. Fron Pharmacol 10:123. https://doi.org/10.3389/fphar.2019.00123
Shao L, Zhang B (2013) Traditional Chinese medicine network pharmacology: theory, methodology and application. Chin J Nat Medicines 11(2):110–120. https://doi.org/10.1016/S1875-5364(13)60037-0
Wang Y, Jafari M, Tang Y, Tang J (2019) Predicting Meridian in Chinese traditional medicine using machine learning approaches. PLoS Comput Biol 15(11):e1007249. https://doi.org/10.1371/journal.pcbi.1007249
Nogales C, Mamdouh ZM, List M, Kiel C, Casas AI, Schmidt H (2021) Network pharmacology: curing causal mechanisms instead of treating symptoms - ScienceDirect. Trends Pharmacol Sci 43(2):136–150. https://doi.org/10.1016/j.tips.2021.11.004
Wang Y, Zhou Z, Chen L, He X, Li H, Huang Y, Pu Y, Luo H (2022) Efficacy of Duhuo Jisheng decoction in treating ankylosing spondylitis: clinical evidence and potential mechanisms. Evid Based Complement Altern 2022:1–12. https://doi.org/10.1155/2022/3305773
Ziaurrehman T, Umair S, Andreas S, Krister W, Tang J, Markus VK (2020) Exploration of databases and methods supporting drug repurposing: a comprehensive survey. Briefings Bioinf 22(2):1656–1678. https://doi.org/10.1093/bib/bbaa003
Ru J, Li P, Wang J, Zhou W, Li B, Huang C, Li P, Guo Z, Tao W, Yang Y (2014) TCMSP: a database of systems pharmacology for drug discovery from herbal medicines. J Cheminf 6(1):1–6. https://doi.org/10.1186/1758-2946-6-13
UniProt: the Universal Protein Knowledgebase in 2023 (2023). Nucleic Acids Res 51(D1):D523-D531. https://doi.org/10.1093/nar/gkac1052
Marilyn S, Irina D, Justin A, Naomi R, Tsippi IS, Michael S, Noam N, Iris B, Tirza D, Hagit K (2010) GeneCards Version 3: the human gene integrator. Database 2010:baq020. https://doi.org/10.1093/database/baq020
Joanna A, Bocchini CA, Scott AF, Ada H (2009) McKusick’s Online Mendelian Inheritance in Man (OMIM®). Nucleic Acids Res 37(Database):D793–D796. https://doi.org/10.1093/nar/gku1205
Klein TE, Altman RB (2004) PharmGKB: the pharmacogenetics and pharmacogenomics knowledge base. Pharmacogenom J 4(1):1. https://doi.org/10.1038/sj.tpj.6500230
Zhu F, Shi Z, Qin C, Tao L, Liu X, Xu F, Zhang L, Song Y, Liu X, Zhang J, Han B (2012) Therapeutic target database update 2012: a resource for facilitating target-oriented drug discovery. Nucleic Acids Res 40(D1):D1128–D1136
Wishart DS, Craig K, Guo AC, Cheng D, Savita S, Dan T, Bijaya G, Murtaza H (2008) DrugBank: a knowledgebase for drugs, drug actions and drug targets. Nucleic Acids Res 36(1):901–906. https://doi.org/10.1093/nar/gkm958
Kohl M, Wiese S, Warscheid B (2011) Cytoscape: software for visualization and analysis of biological networks. Methods Mol Biol 696:291–303. https://doi.org/10.1007/978-1-60761-987-1_18
Damian S, Andrea F, Michael K, Milan S, Alexander R, Pablo M, Tobias D, Manuel S, Jean M, Peer B (2011) The STRING database in 2011: functional interaction networks of proteins, globally integrated and scored. Nucleic Acids Res 39:561–568. https://doi.org/10.1093/nar/gkq973
Scott DE, Bayly AR, Abell C, Skidmore J (2016) Small molecules, big targets: drug discovery faces the protein–protein interaction challenge. Nat Rev Drug Discov 15(8):533–550
Tang Y, Li M, Wang J, Pan Y, Wu F-X (2015) CytoNCA: a cytoscape plugin for centrality analysis and evaluation of protein interaction networks. Biosystems 127:67–72. https://doi.org/10.1016/j.biosystems.2014.11.005
Carlson M, Falcon S, Pages H, Li N (2019) org. Hs. eg. db: Genome wide annotation for Human. R package version 3(2):3.
Ashburner M, Ball CA, Blake JA, Botstein D, Butler H, Cherry JM, Davis AP, Dolinski K, Dwight SS, Eppig JT, Harris MA (2000) Gene Ontology: tool for the unification of biology. Nat Genet 25(1):25–29. https://doi.org/10.1038/75556
Kanehisa G (2000) KEGG: kyoto encyclopedia of genes and genomes. Nucleic Acids Res 28(1):27–30. https://doi.org/10.1093/nar/28.1.27
Patil PP, Patil VS, Khanal P, Darasaguppe HR, Charla R, Bhatkande A, Patil BM, Roy S (2022) Network pharmacology and in vitro testing of Theobroma cacao extract’s antioxidative activity and its effects on cancer cell survival. PLoS ONE 17(4):e0259757. https://doi.org/10.1371/journal.pone.0259757
Wang Y, Xiao J, Suzek TO, Zhang J, Wang J, Bryant SH (2019) PubChem: a public information system for analyzing bioactivities of small molecules. Nucleic Acids Res 37:W623–W633. https://doi.org/10.1093/nar/gkp456
Buntrock RE (2002) ChemOffice Ultra 7.0. J Chem Inf Comput Sci 42(6):1505–1506. https://doi.org/10.1021/ci025575p
Rose PW, Prlić A, Altunkaya A, Bi C, Bradley AR, Christie CH, Costanzo LD, Duarte JM, Dutta S, Feng Z (2016) The RCSB protein data bank: integrative view of protein, gene and 3D structural information. Nucleic Acids Res 5(D1):D271–D281. https://doi.org/10.1093/nar/gkw1000
DeLano WL (2002) Pymol: an open-source molecular graphics tool. C Newsl Protein Crystallogr 40(1):82–92
Jiang K, Tu Z, Chen K, Xu Y, Chen F, Xu S, Shi T, Qian J, Shen L, Hwa J, Wang D, Xiang Y (2022) Gasdermin D inhibition confers antineutrophil-mediated cardioprotection in acute myocardial infarction. J Clin Invest. https://doi.org/10.1172/jci151268
Ibanez B, James S, Agewall S, Antunes MJ, Bucciarelli-Ducci C, Bueno H, Caforio AL, Crea F, Goudevenos JA, Halvorsen S (2018) 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation: the Task Force for the management of acute myocardial infarction in patients presenting with ST-segment elevation of the European Society of Cardiology (ESC). Eur Heart J 39(2):119–177. https://doi.org/10.1093/eurheartj/ehx393
Boateng S, Sanborn T (2013) Acute myocardial infarction. Disease-a-month 59(3):83–96
Cao Q, Du H, Fu X, Duan N, Liu C, Li X (2020) Artemisinin attenuated atherosclerosis in high-fat diet-fed ApoE-/- mice by promoting macrophage autophagy through the AMPK/mTOR/ULK1 pathway. J Cardiovasc Pharmacol 75(4):321–332. https://doi.org/10.1097/fjc.0000000000000794
Aktaş I, Özmen Ö, Tutun H, Yalçın A, Türk A (2020) Artemisinin attenuates doxorubicin induced cardiotoxicity and hepatotoxicity in rats. Biotech Histochem 95(2):121–128. https://doi.org/10.1080/10520295.2019.1647457
Jia L, Jing Y, Wang D, Cheng S, Fu C, Chu X, Yang C, Jiang B, Xin S (2022) Through network pharmacology and molecular docking to explore the underlying mechanism of Artemisia annua L. treating in abdominal aortic aneurysm. Front Physiol 13:1034014. https://doi.org/10.3389/fphys.2022.1034014
Patel RV, Mistry BM, Shinde SK, Syed R, Singh V, Shin H-S (2018) Therapeutic potential of quercetin as a cardiovascular agent. Eur J Med Chem 155:889–904. https://doi.org/10.1016/j.ejmech.2018.06.053
Wu YT, Chen L, Tan ZB, Fan HJ, Xie LP, Zhang WT, Chen HM, Li J, Liu B, Zhou YC (2018) Luteolin inhibits vascular smooth muscle cell proliferation and migration by inhibiting TGFBR1 signaling. Front Pharmacol 9:1059. https://doi.org/10.3389/fphar.2018.01059
Dong LY, Li S, Zhen YL, Wang YN, Shao X, Luo ZG (2013) Cardioprotection of vitexin on myocardial ischemia/reperfusion injury in rat via regulating inflammatory cytokines and MAPK pathway. Am J Chin Med 41(06):1251–1266. https://doi.org/10.1142/S0192415X13500845
Hernandez-Resendiz S, Prunier F, Girao H, Dorn G, Hausenloy DJ (2020) Targeting mitochondrial fusion and fission proteins for cardioprotection. J Cell Mol Med 24(12):6571–6585. https://doi.org/10.1111/jcmm.15384
Ambrose JA, Singh M (2015) Pathophysiology of coronary artery disease leading to acute coronary syndromes. F1000Prime Rep 7:08. https://doi.org/10.12703/p7-08
Kennon AM, Stewart JA Jr (2021) RAGE differentially altered in vitro responses in vascular smooth muscle cells and adventitial fibroblasts in diabetes-induced vascular calcification. Front Physiol 12:676727. https://doi.org/10.3389/fphys.2021.676727
Gao X, Zhang H, Schmidt AM, Zhang C (2008) AGE/RAGE produces endothelial dysfunction in coronary arterioles in Type 2 diabetic mice. Am J Physiol 295(2):H491–H498. https://doi.org/10.1152/ajpheart.00464.2008
Suchal K, Malik S, Khan SI, Malhotra RK, Goyal SN, Bhatia J, Kumari S, Ojha S, Arya DS (2017) Protective effect of mangiferin on myocardial ischemia-reperfusion injury in streptozotocin-induced diabetic rats: role of AGE-RAGE/MAPK pathways. Sci Rep 7:42027. https://doi.org/10.1038/srep42027
Li Q, Liu Y, Xia X, Sun H, Gao J, Ren Q, Zhou T, Ma C, Xia J, Yin C (2021) Activation of macrophage TBK1-HIF-1α-mediated IL-17/IL-10 signaling by hyperglycemia aggravates the complexity of coronary atherosclerosis: an in vivo and in vitro study. FASEB J 35(5):e21609. https://doi.org/10.1096/fj.202100086RR
Zhan B, Xu Z, Zhang Y, Wan K, Deng H, Wang D, Bao H, Wu Q, Hu X, Wang H, Huang X, Cheng X (2020) Nicorandil reversed homocysteine-induced coronary microvascular dysfunction via regulating PI3K/Akt/eNOS pathway. Biomed Pharmacother 127:110121. https://doi.org/10.1016/j.biopha.2020.110121
Karar J, Maity A (2011) PI3K/AKT/mTOR pathway in angiogenesis. Front Mol Neurosci 4:51. https://doi.org/10.3389/fnmol.2011.00051
Sevim Bayrak C, Zhang P, Tristani-Firouzi M, Gelb BD, Itan Y (2020) De novo variants in exomes of congenital heart disease patients identify risk genes and pathways. Genome Med 12(1):9. https://doi.org/10.1186/s13073-019-0709-8
Dhanasekaran R, Deutzmann A, Mahauad-Fernandez WD, Hansen AS, Gouw AM, Felsher DW (2022) The MYC oncogene—the grand orchestrator of cancer growth and immune evasion. Nat Rev Clin Oncol 19(1):23–36. https://doi.org/10.1038/s41571-021-00549-2
Dang CV (2012) MYC on the path to cancer. Cell 149(1):22–35. https://doi.org/10.1016/j.cell.2012.03.003
Chen H, Liu H, Qing G (2018) Targeting oncogenic Myc as a strategy for cancer treatment. Signal Transduct Target 3(1):5. https://doi.org/10.1038/s41392-018-0008-7
Zeng Y, Du WW, Wu Y, Yang Z, Awan FM, Li X, Yang W, Zhang C, Yang Q, Yee A, Chen Y, Yang F, Sun H, Huang R, Yee AJ, Li RK, Wu Z, Backx PH, Yang BB (2017) A circular RNA binds to and activates AKT phosphorylation and nuclear localization reducing apoptosis and enhancing cardiac repair. Theranostics 7(16):3842–3855. https://doi.org/10.7150/thno.19764
Somanath PR, Razorenova OV, Chen J, Byzova TV (2006) Akt1 in endothelial cell and angiogenesis. Cell Cycle 5(5):512–518. https://doi.org/10.4161/cc.5.5.2538
DeBosch B, Treskov I, Lupu TS, Weinheimer C, Kovacs A, Courtois M, Muslin AJ (2006) Akt1 is required for physiological cardiac growth. Circulation 113(17):2097–2104. https://doi.org/10.1161/CIRCULATIONAHA.105.595231
Ackah E, Yu J, Zoellner S, Iwakiri Y, Skurk C, Shibata R, Ouchi N, Easton RM, Galasso G, Birnbaum MJ (2005) Akt1/protein kinase Bα is critical for ischemic and VEGF-mediated angiogenesis. J Clin Invest 115(8):2119–2127. https://doi.org/10.1172/JCI24726
Gu Y, Wang X, Wang X, Yuan M, Wu G, Hu J, Tang Y, Huang C (2012) Artemisinin attenuates post-infarct myocardial remodeling by down-regulating the NF-κB pathway. Tohoku J Exp Med 227(3):161–170. https://doi.org/10.1620/tjem.227.161
Wang F, Gao Q, Yang J, Wang C, Cao J, Sun J, Fan Z, Fu L (2020) Artemisinin suppresses myocardial ischemia–reperfusion injury via NLRP3 inflammasome mechanism. Mol Cell Biochem 474(1):171–180. https://doi.org/10.1007/s11010-020-03842-3
Acknowledgements
Deng Liang and Duan Yixuan contributed to the preliminary data analysis, interpretation, and manuscript writing. Liu Chang, Sun Jingjing and Zhao Sihai participated in the manuscript submission and editing. Deng Jie participated in research design. All authors contributed to the final approval of manuscript.
Funding
This study was supported by Shannxi Social Development Funding (grant No.2017SF-134) and Shannxi Science Funding (grant No.2020JQ-553) and Xi’an Jiaotong University Funding (grant No.YXJLRH2022073).
Author information
Authors and Affiliations
Contributions
Deng Liang and Duan Yixuan contributed to the preliminary data analysis, interpretation, and manuscript writing. Liu Chang, Sun Jingjing and Zhao Sihai participated in the manuscript submission and editing. Deng Jie participated in research design. All authors contributed to the final approval of manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical approval and consent to participate.
This research was approved by Xi’an Jiaotong University Committee on Animal Care (Shaanxi, China).
Research involving human participants or Animals
All experiments were carried out in accordance with the guide for the care and use of Laboratory Animals (Department of Health and Human Services, Publication No. [NIH] 86–23), and were approved by Xi’an Jiaotong University Committee on Animal Care (Shaanxi, China).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liang, D., Yixuan, D., Chang, L. et al. Mechanism of Artemisia annua L. in the treatment of acute myocardial infarction: network pharmacology, molecular docking and in vivo validation. Mol Divers (2023). https://doi.org/10.1007/s11030-023-10750-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11030-023-10750-3