Abstract
Purpose
Ventricular premature depolarizations (VPD) commonly arise from the septal anterior right ventricular outflow tract (sRVOT), the left coronary cusp (LCC), and the distal great cardiac vein (dGCV), and share common ECG characteristics. To assess the diagnostic accuracy of non-invasive electroanatomic mapping (NIEAM) in differentiating VPD origin between sRVOT, LCC and dGCV and quantify its clinical utility in eliminating unnecessary mapping and ablation.
Methods
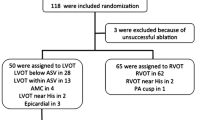
ECGs and NIEAMs (CardioInsight, Medtronic) from 32 patients (56.3 ± 15.2 years) undergoing ablation for VPDs originating from sRVOT, LCC, or dGCV were blindly reviewed for their diagnostic accuracy in predicting the SOO. A 2-step algorithm using NIEAM-based activation timing of the superior basal septum of < 22.5 ms and lateral mitral annulus of > 60.5 ms was compared with subjective ECG evaluation, the maximum deflection index (MDI), and the V2 transitional ratio in predicting SOO. We calculated the mapping and ablation time that could have been avoided had the operators relied on activation timing by NIEAM in designing their mapping and ablation strategy.
Results
NIEAM was superior to subjective ECG evaluation, MDI, and V2 transition ratio in predicting the SOO yielding a sensitivity and specificity of 96.9% and 98.4% respectively. Using NIEAM in determining the SOO would have obviated 22 ± 4.5 min of mapping in the wrong chamber and prevented unnecessary ablation of 4.5 ± 1.8 min.
Conclusion
NIEAM has high diagnostic accuracy in differentiating between sRVOT, LCC, and dGCV VPDs, and can significantly reduce mapping time, obviating the need for unnecessary access and ablation.




Similar content being viewed by others
Abbreviations
- ECG:
-
Electrocardiogram
- EPS:
-
Electrophysiology study
- GCV:
-
Great cardiac vein
- LCC:
-
Left coronary cusp
- LVS:
-
Left ventricular summit
- MDI:
-
Maximum deflection index
- NIEAM:
-
Non-invasive electroanatomic mapping
- RVOT:
-
Right ventricular outflow tract
- SoV:
-
Sinuses of Valsalva
- SOO:
-
Site of origin
- VPD:
-
Ventricular premature depolarization
References
Obel OA, d’Avila A, Neuzil P, Saad EB, Ruskin JN, Reddy VY. Ablation of left ventricular epicardial outflow tract tachycardia from the distal great cardiac vein. J Am Coll Cardiol. 2006;48:1813–7.
Yamada T, McElderry HT, Doppalapudi H, Okada T, Murakami Y, Yoshida Y, et al. Idiopathic ventricular arrhythmias originating from the left ventricular summit: anatomic concepts relevant to ablation. Circ Arrhythm Electrophysiol. 2010;3:616–23.
Mountantonakis SE, Frankel DS, Tschabrunn CM, Hutchinson MD, Riley MP, Lin D, et al. Ventricular arrhythmias from the coronary venous system: prevalence, mapping, and ablation. Heart Rhythm. 2015;12(6):1145–53.
Yarlagadda RK, Iwai S, Stein KM, Markowitz SM, Shah BK, Cheung JW, et al. Reversal of cardiomyopathy in patients with repetitive monomorphic ventricular ectopy originating from the right ventricular outflow tract. Circulation. 2005;112:1092–7.
Takemoto M, Yoshimura H, Ohba Y, Matsumoto Y, Yamamoto U, Mohri M, et al. Radiofrequency catheter ablation of premature ventricular complexes from right ventricular outflow tract improves left ventricular dilation and clinical status in patients without structural heart disease. J Am Coll Cardiol. 2005;45(8):1259–65.
Bogun F, Crawford T, Reich S, Koelling TM, Armstrong W, Good E, et al. Radiofrequency ablation of frequent, idiopathic premature ventricular complexes: comparison with a control group without intervention. Heart Rhythm. 2007;4:863–7.
Baman TS, Lange DC, Ilg KJ, Gupta SK, Liu TY, Alguire C, et al. Relationship between burden of premature ventricular complexes and left ventricular function. Heart Rhythm. 2010;7:865–9.
Mountantonakis SE, Frankel DS, Gerstenfeld EP, Dixit S, Lin D, Hutchinson MD, et al. Reversal of outflow tract ventricular premature depolarization-induced cardiomyopathy with ablation: effect of residual arrhythmia. Heart Rhythm. 2011;8(10):1608–14.
Cakulev I, Sahadevan J, Arrude M, et al. Confirmation of novel noninvasive high-density electrocardiographic mapping with electrophysiology study: implications for therapy. Circ Arrhythm Electrophysiol. 2013;6:68–75.
Lin D, Ilkhanoff L, Gerstenfeld E, Dixit S, Beldner S, Bala R, et al. Twelve-lead electrocardiographic characteristics of the aortic cusp region guided by intracardiac echocardiography and electroanatomic mapping. Heart Rhythm. 2008;5(5):663–9.
Jamil-Copley S, Bokan R, Kojodjojo P, Qureshi N, Koa-Wing M, Hayat S, et al. Noninvasive electrocardiographic mapping to guide ablation of outflow tract ventricular arrhythmias. Heart Rhythm. 2014;11(4):587–94.
Erkapic D, Greiss H, Pajitnev D, et al. Clinical impact of a novel three-dimensional electrocardiographic imaging for non-invasive mapping of ventricular arrhythmias—a prospective randomized trial. Europace. 2015;17:591–7.
Wissner E, Revishvili A, Metzner A, et al. Noninvasive epicardial and endocardial mapping of premature ventricular contractions. Europace. 2017;19:843–9.
Mountantonakis SE, Vaishnav AS, Jacobson JD, et al. Conduction patterns of idiopathic arrhythmias from the endocardium and epicardium of outflow tracts: new insights with noninvasive electroanatomic mapping. Heart Rhythm. 2019. https://doi.org/10.1016/j.hrthm.2019.04.026.
Bazan V, Bala R, Garcia FC, Sussman JS, Gerstenfeld EP, Dixit S, et al. Twelve-lead ECG features to identify ventricular tachycardia arising from the epicardial right ventricle. Heart Rhythm. 2006;3(10):1132–9.
Bazan V, Gerstenfeld EP, Garcia FC, Bala R, Rivas N, Dixit S, et al. Site-specific twelve-lead ECG features to identify an epicardial origin for left ventricular tachycardia in the absence of myocardial infarction. Heart Rhythm. 2007;4:1403–10.
Siontis KC, Madhavan M, Kapa S, Asirvatham SJ, Noseworthy PA. QRS complex maximum deflection index in aortic cusp premature ventricular complexes. Int J Cardiol Heart Vasc. 2015;7:6–8.
Betensky BP, Park RE, Marchlinski FE, et al. The V(2) transition ratio: a new electrocardiographic criterion for distinguishing left from right ventricular outflow tract tachycardia origin. J Am Coll Cardiol. 2011;57(22):2255–62.
Funding
This study was financially supported by Medtronic External Funding (Minneapolis, MN).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Mountantonakis Speakers Honoraria. Dr. Skipitaris, Medtronic Advisory Board. The remaining authors have nothing to disclose.
Ethical approval
This study was approved by our institutional review board.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mountantonakis, S.E., Coleman, K.M., Vaishnav, A.S. et al. Non-invasive electroanatomic mapping to reduce mapping time during catheter ablation of outflow tract ventricular premature depolarizations. J Interv Card Electrophysiol 60, 295–302 (2021). https://doi.org/10.1007/s10840-020-00731-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-020-00731-z