Abstract
Purpose
To describe the clinical and imaging features in a series of patients diagnosed with macular coloboma (MC) and intrachoroidal cavitation (ICC).
Methods
Patients diagnosed with MC based on clinical examination between June 2017 and July 2021 were retrieved from the electronic medical record system and were included in the study. Colour fundus photographs, optical coherence tomography (OCT) and Multicolour® imaging scans of these patients were analysed.
Results
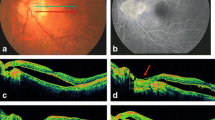
We identified 16 eyes of 11 patients with MC on fundus examination. Based on OCT imaging features, conforming variant of MC was seen in 9 (56%) eyes and non-conforming variant in 7 (44%) eyes. No eyes with MC in the study showed features of both conforming and non-conforming varieties simultaneously. In the non-conforming variety of MC with presence of intercalary membrane break, ICC was identified in 5 (71%) of these eyes. ICC in MC appeared as flat, dark greenish areas with or without an orange-coloured boundary abutting the margin of the coloboma on Multicolour® imaging.
Conclusion
In 31% eyes, ICC was seen in non-conforming type of MC and was well-identified on Multicolour® imaging. It appears that presence of intercalary membrane break and detachment are prerequisites for developing ICC.





Similar content being viewed by others
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Coloboma of macula. https://www.orpha.net/consor/cgi-bin/OC_Exp.php?lng=EN&Expert=98945. Accessed 19 Dec 2021
Hou X, Guo Y, Liu J et al (2021) A systematic review of the clinical manifestations and diagnostic methods for macular coloboma. Curr Eye Res 46:913–918. https://doi.org/10.1080/02713683.2020.1853779
Oh JY, Yu YS, Hwang J-M, Park KH (2007) Optical coherence tomographic finding in a case of macular coloboma. Korean J Ophthalmol 21:175. https://doi.org/10.3341/kjo.2007.21.3.175
Panagiotidis D, Karagiannis D, Theodossiadis P et al (2010) Atypical macular coloboma in a patient with adult vitelliform dystrophy. Can J Ophthalmol 45:544–545. https://doi.org/10.3129/i09-277
El Bahloul M, Younes S, Zahir F et al (2019) La dystrophie maculaire de la Caroline du Nord : à propos d’un cas. J Fr Ophtalmol 42:e73–e77. https://doi.org/10.1016/j.jfo.2018.05.011
Han IC, Critser DB, Stone EM (2018) Swept-source OCT of a macular coloboma in NMNAT1-leber congenital amaurosis. Ophthalmol Retina 2:1040. https://doi.org/10.1016/j.oret.2018.07.009
Langwińska-Wośko E, Szulborski K, Broniek-Kowalik K (2010) Late onset cone dystrophy. Doc Ophthalmol 120:215–218. https://doi.org/10.1007/s10633-010-9214-5
Mathew DJ (2015) Bilateral macular colobomata: temporal dragging of optic disc. Indian J Ophthalmol 63:348–350. https://doi.org/10.4103/0301-4738.158090
Hayasaka Y, Hayasaka S (2004) Bilateral congenital macular coloboma in a boy with Down syndrome. Eur J Ophthalmol 14:565–567. https://doi.org/10.1177/112067210401400619
Plaza-Ramos P, Tabuenca-Del Barrio L, Zubicoa-Eneriz A, Goldaracena-Tanco B (2018) Michaelis-Manz syndrome: a case report. An Sist Sanit Navar 41:393–396. https://doi.org/10.23938/ASSN.0377
Loh RC, Tan DS (1970) An unusual case of progeria-like dwarfism with bilateral macular coloboma. Am J Ophthalmol 70:968–974. https://doi.org/10.1016/0002-9394(70)92476-1
Amouyal F, Courjaret J-C, Denis D, Matonti F (2014) Colobome maculaire de Sorsby: fond d’œil et OCT spectral-domain. J Fr Ophtalmol 37:754. https://doi.org/10.1016/j.jfo.2014.03.009
Khan AO, Patel N, Ghazi NG et al (2018) Familial non-syndromic macular pseudocoloboma secondary to homozygous CLDN19 mutation. Ophthalmic Genet 39:577–583. https://doi.org/10.1080/13816810.2018.1498528
Wei Y-H, Yang C-M, Chen M-S et al (2009) Peripapillary intrachoroidal cavitation in high myopia: reappraisal. Eye 23:141–144. https://doi.org/10.1038/sj.eye.6702961
Venkatesh R, Jain K, Aseem A et al (2020) Intrachoroidal cavitation in myopic eyes. Int Ophthalmol 40:31–41. https://doi.org/10.1007/s10792-019-01146-0
Schoenberger SD, Agarwal A (2013) Intrachoroidal cavitation in North Carolina macular dystrophy. JAMA Ophthalmol 131:1073. https://doi.org/10.1001/jamaophthalmol.2013.1598
Markan A, Jain M, Singh R (2020) Secondary intrachoroidal cavitation in a case of iridofundal coloboma. Med Hypotheses 143:110085. https://doi.org/10.1016/j.mehy.2020.110085
Chung CY, Li SH, Li KKW (2017) Focal choroidal excavation—morphological features and clinical correlation. Eye 31:1373–1379. https://doi.org/10.1038/eye.2017.71
Mann IC (1927) On certain abnormal conditions of the macular region usually classed as colobomata. Br J Ophthalmol 11:99–116. https://doi.org/10.1136/bjo.11.3.99
Schubert HD (2005) Structural organization of choroidal colobomas of young and adult patients and mechanism of retinal detachment. Trans Am Ophthalmol Soc 103:457–472
Lingam G (2013) Pattern of blood vessels in eyes with coloboma. Indian J Ophthalmol 61:743. https://doi.org/10.4103/0301-4738.122910
Chen T-C, Yang C-H, Sun J-P et al (2015) Macular retinal detachment associated with intrachoroidal cavitation in myopic patients. Graefes Arch Clin Exp Ophthalmol 253:1437–1446. https://doi.org/10.1007/s00417-014-2829-6
Akimoto M, Akagi T, Okazaki K, Chihara E (2012) Recurrent macular detachment and retinoschisis associated with intrachoroidal cavitation in a normal eye. Case Rep Ophthalmol 3:169–174. https://doi.org/10.1159/000339292
Feng HL, Sharma S, Stinnett S et al (2019) Identification of posterior segment pathology with en face retinal imaging using multicolor confocal scanning laser ophthalmoscopy. Retina (Philadelphia, Pa) 39:972–979. https://doi.org/10.1097/IAE.0000000000002111
Acknowledgements
We would like to thank our technicians, Mr Abhishek, Mr Deekshit, Mr Manjunath and Mr Madhu for their contribution in acquiring the images and providing them to us for analysis in this study.
Funding
No funding has been obtained for this research work.
Author information
Authors and Affiliations
Contributions
RV and JC contributed to conceptualising the study, data acquisition, analysing the data, statistics and results, interpreting the findings, and writing and reviewing the manuscript. AG, ROH, and NR involved in data acquisition and analysing the data. NKY involved in reviewing the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interests.
Ethics approval and consent to participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee (Narayana Nethralaya institutional review board – (C-2021-07-003) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards”.
Consent for publication
Informed consent was obtained from all individual participants included in the study. The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given his consent for his/her images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Human and animal rights
This article does not contain any studies with animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Venkatesh, R., Agrawal, R., Reddy, N.G. et al. Intercalary membrane break and detachment causes intrachoroidal cavitation in macular coloboma. Int Ophthalmol 42, 2581–2589 (2022). https://doi.org/10.1007/s10792-022-02306-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-022-02306-5