Abstract
Purpose
To present updated risk factors, anatomical and visual outcomes and a surgical approach to posteriorly dislocated intraocular lenses (IOL).
Methods
A retrospective case series review of patients presenting with posteriorly dislocated IOL to the vitreous was performed. All cases were managed surgically with pars plana vitrectomy (PPV) followed by IOL repositioning and refixation or IOL exchange. Clinical characteristics, risk factors for IOL dislocation, visual outcomes and intraoperative and postoperative complications were investigated.
Results
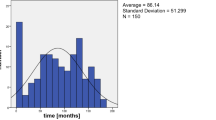
Forty patients with posteriorly dislocated IOL underwent 3-port PPV and lens retrieval at an average of 6.5 years after cataract surgery. The main causes of IOL dislocation were previous PPV, myopia, pseudoexfoliation syndrome, ocular trauma and recurrent intravitreal injections. The existing IOL was repositioned and secured in 90% of the cases. Visual acuity improved in 34 patients, maintained in 5 and deteriorated in 1. All IOLs were central and stable at final follow-up.
Conclusion
Posterior intraocular lens dislocation is becoming more prevalent. The main underlying causes found in this series were previous vitrectomy, myopia and recurrent intra-vitreal substance injections. Visual acuity improved in most cases after lens repositioning; however visual outcome is often limited due to associated ocular co-morbidities despite adequate lens position. Despite complete lack of zonular support, a posteriorly dislocated IOL can often be preserved by repositioning and fixation of the lens in the posterior chamber. Pathologies primarily associated with this type of lens malposition include history of vitrectomy, high myopia and multiple intravitreal substance injections.


Similar content being viewed by others
References
Ascaso FJ, Huerva V, Grzybowski A (2015) Epidemiology, etiology, and prevention of late IOL-capsular bag complex dislocation: review of the literature. J Ophthalmolog 2015:805–706
Davis D, Brubaker J, Espandar L, Stringham J, Crandall A, Werner L, Mamalis N (2009) Late in-the-bag spontaneous intraocular lens dislocation; evaluation of 86 consecutive cases. Ophthalmology 116:664–670
Jakobsson G, Zetterberg M, Lundström M, Stenevi U, Grenmark R, Sundelin K (2010) Late dislocation of in-the-bag and out-of-the bag intraocular lenses: ocular and surgical characteristics and time to lens repositioning. J Cataract Refract Surg 36:1637–1644
Dabrowska-Kloda K, Kloda T, Boudiaf S, Jakobsson G, Stenevi U (2015) Incidence and risk factors of late in-the-bag intraocular lens dislocation: evaluation of 140 eyes between 1992 and. J Cataract Refract Surg 41:1376–1382
Kristianslund O, Råen M, Østern AE, Drolsum L (2017) Late in-the-bag intraocular lens dislocation: a randomized clinical trial comparing lens repositioning and lens exchange. Ophthalmology 124:151–159
Jakobsson G, Zetterberg M, Sundelin K, Stenevi U (2013) Surgical repositioning of intraocular lenses after late dislocation: complications, effect on intraocular pressure, and visual outcomes. J Cataract Refract Surg 39:1879–1885
Soiberman U, Gehlbach PL, Murakami P, Stark WJ (2015) Pars plana vitrectomy and iris suture fixation of posteriorly dislocated intraocular lenses. J Cataract Refract Surg 41:1454–1460
Degenring RF, Sauder G (2006) Vitreous prolapse and IOL dislocation during intravitreal injection of triamcinolone acetonide. Graefe’s Arch Clin Exp Ophthalmol 244:1043–1044
Gimbel HV, Condon GP, Kohnen T, Olson RJ, Halkiadakis I (2005) Late in-the-bag intraocular lens dislocation: incidence, prevention, and management. J Cataract Refract Surg 31:2193–2204
Hayashi K, Ogawa S, Manabe S, Hirata A, Yoshimura K (2016) A classification system of intraocular lens dislocation sites under operating microscopy, and the surgical techniques and outcomes of exchange surgery. Graefes Arch Clin Exp Ophthalmol 254:505–513
Rey A, Jürgens I, Dyrda A, Maseras X, Morilla A (2016) Surgical outcome of late in-the-bag intraocular lens dislocation treated with pars plana vitrectomy. Retina 36:576–581
Bieliński P, Jasielska M, Wyszyńska A, Winiarczyk M, Mackiewicz J (2019) Pars plana vitrectomy with transscleral fixation of posterior chamber lens in the treatment of post-traumatic lens dislocation. Int Ophthalmol 39(2):455–460
Bajgai P, Tigari B, Singh R (2018) Outcomes of 23- and 25-gauge transconjunctival sutureless vitrectomies for dislocated intraocular lenses. Int Ophthalmol 38(6):2295–2301
Siepser SB (1994) The closed chamber slipping suture technique for iris repair. Ann Ophthalmol 26:71–72
McCannel MA (1976) A retrievable suture idea for anterior uveal problems. Ophthalmic Surg 7:98–103
Faria MY, Ferreira NP, Canastro M (2017) Management of dislocated intraocular lenses with iris suture. Eur J Ophthalmol 27:45–48
Mello MO Jr, Scott IU, Smiddy WE, Flynn HW Jr, Feuer W (2000) Surgical management and outcomes of dislocated intraocular lenses. Ophthalmology 107:62–67
Kokame GT, Yanagihara RT, Shantha JG, Kaneko KN (2018) Long term outcome of pars plana vitrectomy and sutured scleral-fixated posterior chamber intraocular lens implantation or repositioning. Am J Ophthalmol 189:10–16
Sommer A, Belkin A, Ofir S, Assia E (2017) Profile of patients presenting for cataract surgery in a public hospital: a 15 year perspective. Isr Med Assoc J 19:109–113
Matsumoto M, Yamada K, Uematsu M, Fujikawa A, Tsuiki E, Kumagami T, Suzuma K, Kitaoka T (2012) Spontaneous dislocation of in-the-bag intraocular lens primarily in cases with prior vitrectomy. Eur J Ophthalmol 22:363–367
Koike T, Baba T, Nizawa T, Oshitari T, Yamamoto S (2017) Characteristics of patients with spontaneous dislocation of in-the-bag intraocular lens after pars plana vitrectomy. Jpn J Ophthalmol 61:267–270
Masket S, Osher RH (2002) Late complications with intraocular lens dislocation after capsulorhexis in pseudoexfoliation syndrome. J Cataract Refract Surg 28:1481–1484
Lorente R, de Rojas V, Vazquez de Parga P, Moreno C, Landaluce ML, Domínguez R, Lorente B (2010) Management of late spontaneous in-the-bag intraocular lens dislocation: retrospective analysis of 45 cases. J Cataract Refract Surg 36:1270–1282
Jehan FS, Mamalis N, Crandall AS (2001) Spontaneous late dislocation of intraocular lens within the capsular bag in pseudoexfoliation patients. Ophthalmology 108:1727–1231
Liu E, Cole S, Werner L, Hengerer F, Mamalis N, Kohnen T (2015) Pathologic evidence of pseudoexfoliation in cases of in-the-bag intraocular lens subluxation or dislocation. J Cataract Refract Surg 41:929–935
Werner L, Zaugg B, Neuhann T, Burrow M, Tetz M (2012) In-the-bag capsular tension ring and intraocular lens subluxation or dislocation: a series of 23 cases. Ophthalmology 119:266–271
Ahmed II, Cionni RJ, Kranemann C, Crandall AS (2005) Optimal timing of capsular tension ring implantation: Miyake-Apple video analysis. J Cataract Refract Surg 31:1809–1813
Ahmed II, Chen SH, Kranemann C, Wong DT (2005) Surgical repositioning of dislocated capsular tension rings. Ophthalmology 112:1725–1733
Scharioth GB, Prasad S, Georgalas I, Tataru C, Pavlidis M (2010) Intermediate results of sutureless intrascleral posterior chamber intraocular lens fixation. J Cataract Refract Surg 36(2):254–259
Soiberman U, Qing P, Yassine D, Murakami P, Stark WJ (2015) Iris suture fixation of subluxated intraocular lenses. Am J Ophthalmol 159:353–359
Solomon K, Gussler JR, Gussler C, Van Meter WS (1993) Incidence and management of complications of transsclerally sutured posterior chamber lenses. J Cataract Refract Surg 19:488–493
Bande MF, García-Garcés I, Paniagua L, Ruiz-Oliva F, Piñeiro A, Blanco-Teijeiro MJ (2017) Evaluation of vitrectomy and reimplantation following late dislocation of intraocular lens-capsular bag complex: a 3-year follow-up study. Retina 37:925–929
Funding
This study was not funded.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Author Sara Sella declares that she has no conflict of interest. Author Alxendar declares that he has no conflict of interest. Author Shira Sheen-Ophir declares that she has no conflict of interest. Author Joseph R. Ferencz declares that he has no conflict of interest. Author Prof. Ehud I Assia is a consultant to Hanita Lenses, Biotechnology General, Vision Care, IOPtima, APX Ophthalmology, Visidome, CorNeat Vision. Author Yokrat Ton declares that she has no conflict of interest.
Ethical approval
Research number 0173-15 MMC was approved by IRB, Meir Medical Center, Kfar Saba Israel. As retrospective research no inform consent indicated per IRB.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 20750 kb)
Rights and permissions
About this article
Cite this article
Sella, S., Rubowitz, A., Sheen-Ophir, S. et al. Pars plana vitrectomy for posteriorly dislocated intraocular lenses: risk factors and surgical approach. Int Ophthalmol 41, 221–229 (2021). https://doi.org/10.1007/s10792-020-01570-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-020-01570-7