Abstract
Purpose
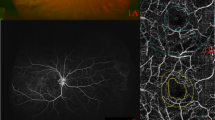
To examine the macular microstructure in macular edema (ME) due to retinal vein occlusion (RVO) in terms of ischemic or nonischemic type to determine whether and how ischemia affects macular microstructure.
Methods
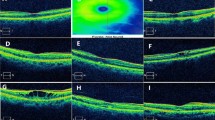
This retrospective, nonrandomized study included 75 newly diagnosed RVO cases (group 1: 55 nonischemic RVO cases and group 2: 20 ischemic RVO cases) with evidence of center-involving ME without any treatment. Quantitative measures on spectral-domain optical coherence tomography images were performed. Central subfield thickness (CST) was collected in the central 1 mm from the thickness map. The following items were evaluated in a 3-mm-wide area (perifoveal ETDRS circle) centered on the fovea: disorganization of the retinal inner layers (DRIL), disrupted external limiting membrane (ELM) and ellipsoid zone disruption (EZD). The microstructural changes were measured manually.
Results
Baseline characteristics, such as age, sex, study eye, and RVO risk factors, were similar between the groups (P > 0.05). CST was 554.15 ± 191.45 µm for group 1 and 769.90 ± 290.00 µm for group 2 (P: 0.001). The extent of DRIL was 1864.09 ± 941.70 µm and 2447.25 ± 492.59 µm for groups 1 and 2, respectively (P: 0.010). The disrupted ELM length was 1700 (0–3000) µm for group 1 and 2725 (300–3000) µm for group 2 (P: 0.027). The EZD length was 1453.09 ± 870.38 µm for group 1 and 1846.00 ± 926.54 µm for group 2 (P: 0.093).
Conclusions
Ischemic RVOs cause greater macular edema and greater disruption in the macular microstructure compared to nonischemic RVOs, especially in terms of DRIL and ELM.

Similar content being viewed by others
References
Rogers S, McIntosh RL, Cheung N, Lim L, Wang JJ, Mitchell P, Kowalski JW, Nguyen H, Wong TY, International Eye Disease Consortium (2010) The prevalence of retinal vein occlusion: pooled data from population studies from the United States, Europe, Asia, and Australia. Ophthalmology 17:313–319
Hayreh SS (1983) Classification of central retinal vein occlusion. Ophthalmology 90:458–474
Munk MR, Sacu S, Huf W, Sulzbacher F, Mittermüller TJ, Eibenberger K, Rezar S, Bolz M, Kiss CG, Simader C, Schmidt-Erfurth U (2014) Differential diagnosis of macular edema of different pathophysiologic origins by spectral domain optical coherence tomography. Retina 34(11):2218–2232
Mimouni M, Segev O, Dori D, Geffen N, Flores V, Segal O (2017) Disorganization of the retinal inner layers as a predictor of visual acuity in eyes with macular edema secondary to vein occlusion. Am J Ophthalmol 182:160–167
Tang F, Qin X, Lu J, Song P, Li M, Ma X (2019) Optical cohorence tomography predictors of short-term visual acuity in eyes with macular edema secondary to retinal vein occlusion treated with intravitreal conbercept. Retina. https://doi.org/10.1097/IAE.0000000000002444
Liu H, Li S, Zhang Z, Shen J (2018) Predicting the visual acuity for retinal vein occlusion after ranibizumab therapy with an original ranking for macular microstructure. Exp Ther Med 15(1):890–896
Chan EW, Eldeeb M, Sun V, Thomas D, Omar A, Kapusta MA, Galic IJ, Chen JC (2019) Disorganization of retinal inner layers and ellipsoid zone disruption predict visual outcomes in central retinal vein occlusion. Ophthalmol Retina 3(1):83–92
Kang JW, Lee H, Chung H, Kim HC (2014) Correlation between optical coherence tomographic hyperreflective foci and visual outcomes after intravitreal bevacizumab for macular edema in branch retinal vein occlusion. Graefes Arch Clin Exp Ophthalmol 252(9):1413–1421
Balci Ö, Öngör E (2004) Retinal Vein Occlusions. Turk J Ophthalmol 34:445–455
The Central Vein Occlusion Study Group N report (1995) A randomized clinical trial of early panretinal photocoagulation for ischemic central vein occlusion. Ophthalmology 102:1434–1444
The Branch Vein Occlusion Study Group (1984) Argon laser photocoagulation for macular edema in branch vein occlusion. Am J Ophthalmol 98:271–282
Sun JK, Lin MM, Lammer J, Prager S, Sarangi R, Silva PS, Aiello LP (2014) Disorganization of the retinal inner layers as a predictor of visual acuity in eyes with center-involved diabetic macular edema. JAMA Ophthalmol 132:1309–1316
Polat N (2018) Optical coherence tomographic comparison of naive macular edema due to ischemic and non-ischemic retinal vein occlusion. In: Retinal Vein Occlusion session-2018 EVRS meeting (Prague- CZECH REPUBLIC). https://www.evrs.eu/optical-coherence-tomographic-comparison-of-naive-macular-edema-due-to-ischemic-and-non-ischemic-retinal-vein-occlusion
Prasad PS, Oliver SC, Coffee RE, Hubschman JP, Schwartz SD (2010) Ultra wide-field angiographic characteristics of branch retinal and hemicentral retinal vein occlusion. Ophthalmology 117:780–784
Singer M, Tan CS, Bell D, Sadda SR (2014) Area of peripheral retinal nonperfusion and treatment response in branch and central retinal vein occlusion. Retina 34:1736–1742
Thomas AS, Thomas MK, Finn AP, Fekrat S (2019) Use of ischemic index on widefield flourescein angiography to characterize a retinal vein occlusion as ischemic or nonischemic. Retina 39(6):1033–1038
Ota M, Tsujikawa A, Murakami T, Yamaike N, Sakamoto A, Kotera Y, Miyamoto K, Kita M, Yoshimura N (2008) Foveal photoreceptor layer in eyes with persistent cystoid macular edema associated with branch retinal vein occlusion. Am J Ophthalmol 145(2):273–280
Shin HJ, Chung H, Kim HC (2011) Association between integrity of foveal photoreceptor layer and visual outcome in retinal vein occlusion. Acta Ophthalmol 89:e35–e40
Ota M, Tsujikawa A, Kita M, Miyamoto K, Sakamoto A, Yamaike N, Kotera Y, Yoshimura N (2008) Integrity of foveal photoreceptor layer in central retinal vein occlusion. Retina 28:1502–1508
Ko J, Kwon OW, Byeon SH (2014) Optical coherence tomography predicts visual outcome in acute central retinal vein occlusion. Retina 34:1132–1141
Wolf-Schnurrbusch UEK, Ghanem R, Rothenbuehler SP, Enzmann V, Framme C, Wolf S (2011) Predictors of short-term visual outcome after anti-VEGF therapy of macular edema due to central retinal vein occlusion. Invest Ophthalmol Vis Sci 52:3334–3337
Oishi A, Hata M, Shimozono M, Mandai M, Nishida A, Kurimoto Y (2010) The significance of external limiting membrane status for visual acuity in age-related macular degeneration. Am J Ophthalmol 150:27–32
Roberts P, Mittermueller TJ, Montuoro A, Sulzbacher F, Munk M, Sacu S, Schmidt-Erfurth U (2014) A quantitative approach to identify morphological features relevant for visual function in ranibizumab therapy of neovascular AMD. Invest Ophthalmol Vis Sci 55:6623–6630
Daruich A, Matet A, Moulin A, Kowalczuk L, Nicolas M, Sellam A, Rothschild PR, Omri S, Gélizé E, Jonet L et al (2018) Mechanisms of macular edema: beyond the surface. Prog Retin Eye Res 63:20–68
Hasegawa T, Ueda T, Okamoto M, Ogata N (2014) Presence of foveal bulge in optical coherence tomographic images in eyes with macular edema associated with branch retinal vein occlusion. Am J Ophthalmol 157(2):390–396
Xu HZ, Le YZ (2011) Significance of outer blood-retina barrier breakdown in diabetes and ischemia. Invest Ophthalmol Vis Sci 52:2160–2164
Sakamoto A, Tsujikawa A, Ota M, Yamaike N, Kotera Y, Miyamoto K, Kita M, Yoshimura N (2009) Evaluation of potential visual acuity in eyes with macular oedema secondary to retinal vein occlusion. Clin Experiment Ophthalmol 37:208–216
Ota M, Tsujikawa A, Murakami T, Kita M, Miyamoto K, Sakamoto A, Yamaike N, Yoshimura N (2007) Association between integrity of foveal photoreceptor layer and visual acuity in branch retinal vein occlusion. Br J Ophthalmol 91:1644–1649
Kang HM, Chung EJ, Kim YM, Koh HJ (2013) Spectral-domain optical coherence tomography (SD-OCT) patterns and response to intravitreal bevacizumab therapy in macular edema associated with branch retinal vein occlusion. Graefes Arch Clin Exp Ophthalmol 251:501–508
Tao LW, Wu Z, Guymer RH, Luu CD (2016) Ellipsoid zone on optical coherence tomography: a review. Clin Exp Ophthalmol 44:422–430
Chatziralli IP, Sergentanis TN, Sivaprasad S (2016) Hyperreflective foci as an independent visual outcome predictor in macular edema due to retinal vascular diseases treated with intravitreal dexamethasone or ranibizumab. Retina 36:2319–2328
Segal O, Barayev E, Nemet AY, Geffen N, Vainer I, Mimouni M (2016) Prognostic value of hyperreflective foci in neovascular age-related macular degeneration treated with bevacizumab. Retina 36:2175–2182
Framme C, Wolf S, Wolf-Schnurrbusch U (2010) Small dense particles in the retina observable by spectral-domain optical coherence tomography in age-related macular degeneration. Invest Ophthalmol Vis Sci 51:5965–5969
Tsujikawa A, Sakamoto A, Ota M, Kotera Y, Oh H, Miyamoto K, Kita M, Yoshimura N (2010) Serous retinal detachment associated with retinal vein occlusion. Am J Ophthalmol 149(2):291–301
Kitagawa S, Yasuda S, Ito Y, Ueno S, Iwase T, Terasaki H (2018) Better prognosis for eyes with preserved foveal depression after intravitreal ranibizumab for macular edema secondary to central retinal vein occlusion. Retina 38(7):1354–1360
Franze K, Grosche J, Skatchkov SN, Schinkinger S, Foja C, Schild D, Uckermann O, Travis K, Reichenbach A, Guck J (2007) Muller cells are living optical fibers in the vertebrate retina. Proc Natl Acad Sci 104:8287–8292
Fujihara-Mino A, Mitamura Y, Inomoto N, Sano H, Akaiwa K, Semba K (2016) Optical coherence tomography parameters predictive of visual outcome after anti-VEGF therapy for retinal vein occlusion. Clin Ophthalmol 10:1305–1313
Battaglia Parodi M, Iacono P, Scaramuzzi M, Bandello F (2017) Outer retinal layer changes after dexamethasone implant for central retinal vein occlusion. Retina 37(10):1888–1895
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Polat, N., Yoloğlu, S. Optical coherence tomographic comparison of naive macular edema due to ischemic and nonischemic retinal vein occlusion. Int Ophthalmol 40, 2085–2093 (2020). https://doi.org/10.1007/s10792-020-01385-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-020-01385-6