Abstract
Background
In patients with chronic pancreatitis (CP), pain relief is a dilemma. Antioxidants with pregabalin therapy have been reported to be useful. Hence, this study was carried out to determine the efficacy of the combination of antioxidant and pregabalin therapy in reducing pain in patients with CP.
Methods
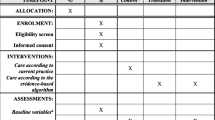
This was a prospective, double blind, superiority, and randomized trial in patients with CP. The treatment group received pregabalin with antioxidants therapy for 8 weeks, and a similar placebo was administered to the controls. Primary outcome was to determine the change in maximum pain intensity assessed by visual analog scale (VAS) and Izbicki pain score. Secondary outcomes were the number of painful days, opioid and non-opioid requirements, improvement in quality of life, number of hospital admission, and overall patient satisfaction.
Results
A total of 90 patients were randomized to 45 in each arm. Demographic profile and baseline pain score were comparable. Patients in treatment group when compared to placebo group had a significant reduction in pain intensity (VAS score 2 ± 0.8 vs. 1.3 ± 0.9; p = 0.007), non-opioid analgesic requirement in days (54.4±2.9 vs. 55.7±1.5; p = 0.014), and number of hospital admissions (0.2 ± 0.5 vs. 0.6 ± 0.7; p = 0.002), respectively. Significant proportion of patients was satisfied in the treatment group compared to placebo group (18% vs. 11%; p = 0.03).
Conclusion
The combination of pregabalin and antioxidant significantly reduces the pain, requirement of non-opioid analgesics, and the number of hospital admissions in patients with CP. It also significantly improves the overall patient satisfaction.
Clinical Trials Register Number
CTRI/2017/05/008492.

Similar content being viewed by others
References
Talukdar R, Lakhtakia S, Nageshwar Reddy D, et al. Ameliorating effect of antioxidants and pregabalin combination in pain recurrence after ductal clearance in chronic pancreatitis: results of a randomized, double blind, placebo-controlled trial. J Gastroenterol Hepatol.. 2016;31:1654–1662.
Thuluvath PJ, Imperio D, Nair S, Cameron JL. Chronic pancreatitis. Long-term pain relief with or without surgery, cancer risk, and mortality. J Clin Gastroenterol.. 2003;36:159–165.
Ammann RW, Akovbiantz A, Largiader F, Schueler G. Course and outcome of chronic pancreatitis. Longitudinal study of a mixed medical-surgical series of 245 patients. Gastroenterology.. 1984;86:820–828.
Jupp J, Fine D, Johnson CD. The epidemiology and socioeconomic impact of chronic pancreatitis. Best Pract Res Clin Gastroenterol.. 2010;24:219–231.
Talukdar R, Reddy DN. Pain in chronic pancreatitis: managing beyond the pancreatic duct. World J Gastroenterol.. 2013;19:6319–6328.
Fitzsimmons D, Kahl S, Butturini G, et al. Symptoms and quality of life in chronic pancreatitis assessed by structured interview and the EORTC QLQ-C30 and QLQ-PAN26. Am J Gastroenterol.. 2005;100:918–926.
Braganza JM, Lee SH, McCloy RF, McMahon MJ. Chronic pancreatitis. Lancet.. 2011;377:1184–1197.
Kirk GR, White JS, McKie L, et al. Combined antioxidant therapy reduces pain and improves quality of life in chronic pancreatitis. J Gastrointest Surg.. 2006;10:499–503.
Talukdar R, Murthy HVV, Reddy DN. Role of methionine containing antioxidant combination in the management of pain in chronic pancreatitis: a systematic review and meta-analysis. Pancreatology.. 2015;15:136–144.
Poulsen JL, Olesen SS, Malver LP, Frøkjær JB, Drewes AM. Pain and chronic pancreatitis: a complex interplay of multiple mechanisms. World J Gastroenterol.. 2013;19:7282–7291.
Siriwardena AK, Mason JM, Sheen AJ, Makin AJ, Shah NS. Antioxidant therapy does not reduce pain in patients with chronic pancreatitis: the ANTICIPATE study. Gastroenterology.. 2012;143(655–663):e1.
Singh VK, Yadav D, Garg PK. Diagnosis and management of chronic pancreatitis: a review. JAMA.. 2019;322:2422–2434.
Hasin DS, O’Brien CP, Auriacombe M, et al. DSM-5 criteria for substance use disorders: recommendations and rationale. Am J Psychiatry.. 2013;170:834–851.
Bhardwaj P, Garg PK, Maulik SK, Saraya A, Tandon RK, Acharya SK. A randomized controlled trial of antioxidant supplementation for pain relief in patients with chronic pancreatitis. Gastroenterology.. 2009;136:149–159.
Bloechle C, Izbicki JR, Knoefel WT, Kuechler T, Broelsch CE. Quality of life in chronic pancreatitis–results after duodenum-preserving resection of the head of the pancreas. Pancreas.. 1995;11:77–85.
Pezzilli R, Morselli-Labate AM, Fantini L, Campana D, Corinaldesi R. Assessment of the quality of life in chronic pancreatitis using Sf-12 and EORTC Qlq-C30 questionnaires. Dig Liver Dis.. 2007;39:1077–1086.
Aaronson NK, Ahmedzai S, Bergman B, et al. The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst.. 1993;85:365–376.
Keller CE, Mel Wilcox C, Gudleski GD, Branham S, Lackner JM. Beyond abdominal pain: pain beliefs, pain affect, and distress as determinants of quality of life in patients with chronic pancreatitis. J Clin Gastroenterol.. 2018;52:563–568.
Norman G. Likert scales, levels of measurement and the “laws” of statistics. Adv Health Sci Educ Theory Pract.. 2010;15:625–632.
Luetmer PH, Stephens DH, Ward EM. Chronic pancreatitis: reassessment with current CT. Radiology.. 1989;171:353–357.
Ewald N, Kaufmann C, Raspe A, Kloer HU, Bretzel RG, Hardt PD. Prevalence of diabetes mellitus secondary to pancreatic diseases (type 3c). Diabetes Metab Res Rev.. 2012;28:338–342.
Daeppen J-B, Faouzi M, Sanchez N, Rahhali N, Bineau S, Bertholet N. Quality of life depends on the drinking pattern in alcohol-dependent patients. Alcohol Alcohol.. 2014;49:457–465.
Olesen SS, Graversen C, Bouwense SA, Wilder-Smith OHG, van Goor H, Drewes AM. Is timing of medical therapy related to outcome in painful chronic pancreatitis? Pancreas.. 2016;45:381–387.
Gurusamy KS, Lusuku C, Davidson BR. Pregabalin for decreasing pancreatic pain in chronic pancreatitis. Cochrane Database Syst Rev.. 2016;2:CD011522.
Olesen SS, Bouwense SAW, Wilder-Smith OHG, van Goor H, Drewes AM. Pregabalin reduces pain in patients with chronic pancreatitis in a randomized, controlled trial. Gastroenterology.. 2011;141:536–543.
Funding
Intramural research Grant received from Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER).
Author information
Authors and Affiliations
Contributions
SS contributed to conceptualization, validation, supervision, and writing review and editing; AO contributed to data collection, formal analysis, investigation, and writing original draft; AA contributed to methodology, validation, and writing review and editing; BSR contributed to data collection, formal analysis, investigation, and writing original draft; KMA contributed to data collection and writing original draft; CV contributed to formal analysis, supervision, and writing review and editing; CP contributed to formal analysis, supervision, and writing review and editing; MP contributed to methodology, validation, and writing review and editing; and VK contributed to formal analysis, supervision, validation, and writing review and editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical statement
Institute ethics committee approval obtained. Approval Number JIP/IEC/2016/1034.
Informed consent
Informed consent was obtained from all the study participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sureshkumar, S., Omang, A., Anandhi, A. et al. Efficacy of Pregabalin and Antioxidants Combination in Reducing Pain in Chronic Pancreatitis: A Double Blind Randomized Trial. Dig Dis Sci 66, 4017–4025 (2021). https://doi.org/10.1007/s10620-020-06711-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06711-7