Abstract
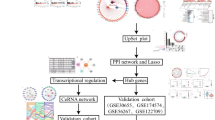
To investigate the molecular mechanism of communication network factor 1 (CCN1) regulating pentylenetetrazol (PTZ)-induced epileptogenesis, deepen the understanding of epilepsy seizure pathogenesis, and provide new drug action targets for its clinical prevention and treatment. Differentially expressed genes (DEGs) on microarrays GSE47516 and GSE88992 were analyzed online using GEO2R. Pathway enrichment and protein–protein interaction network (PPI) analysis of DEGs were carried out using Metascape. Brain tissue samples of severe traumatic brain injury patients (named Healthy group) and refractory epilepsy patients (named Epilepsy group) were obtained and analyzed by qRT-PCR and immunohistochemistry (IHC) staining. A PTZ-induced epilepsy mouse model was established and verified. Morphological changes of neurons in mouse brain tissue were detected using hematoxylin and eosin (HE) staining. qRT-PCR was conducted to detect the mRNA expressions of apoptosis-associated proteins Bax, Caspase-3 and bcl2. TUNEL staining was performed to detect brain neuron apoptosis. The levels of myocardial enzymology, GSH, MDA and ROS in blood of mouse were detected by biochemical assay. CCN1 expression was increased in epilepsy brain tissue samples. CCN1 decreasing effectively prolongs seizure incubation period and decreases seizure duration. Silencing of CCN1 also reduces neuronal damage and apoptosis, decreases mRNA and protein expression of proapoptotic proteins Bax and Caspase-3, increases mRNA expression of antiapoptotic protein Bcl2. Moreover, decrease of CCN1 decreases myocardial enzymatic indexes CK and CK-MB levels, reduces myocardial tissue hemorrhage, and relieves oxidative stress response in hippocampal and myocardial tissue. CCN1 expression is increased in epileptic samples. CCN1 decreasing protects brain tissue by attenuating oxidative stress and inhibiting neuronal apoptosis triggered by PTZ injection, which probably by regulating Nrf2/HO-1 pathway.
Graphical Abstract







Similar content being viewed by others
Data Availability
The data supporting this study's findings are available from the corresponding author upon reasonable request.
References
Chan KY, Jang MJ, Yoo BB, Greenbaum A, Ravi N, Wu W-L, Sánchez-Guardado L, Lois C, Mazmanian SK, Deverman BE, Gradinaru V (2017) Engineered AAVs for efficient noninvasive gene delivery to the central and peripheral nervous systems. Nat Neurosci 20(8):1172–1179. https://doi.org/10.1038/nn.4593
Chatterjee D, Marmion DJ, McBride JL, Manfredsson FP, Butler D, Messer A, Kordower JH (2022) Enhanced CNS transduction from AAV.PHP.eB infusion into the cisterna magna of older adult rats compared to AAV9. Gene Ther 29(6):390–397. https://doi.org/10.1038/s41434-021-00244-y
Chen CC, Kim KH, Lau LF (2016) The matricellular protein CCN1 suppresses hepatocarcinogenesis by inhibiting compensatory proliferation. Oncogene 35(10):1314–1323. https://doi.org/10.1038/onc.2015.190
Dąbrowska K, Skowrońska K, Popek M, Albrecht J, Zielińska M (2021) The role of Nrf2 transcription factor and Sp1-Nrf2 protein complex in glutamine transporter SN1 regulation in mouse cortical astrocytes exposed to ammonia. Int J Mol Sci 22(20):11233. https://doi.org/10.3390/ijms222011233
Devinsky O, Hesdorffer DC, Thurman DJ, Lhatoo S, Richerson G (2016) Sudden unexpected death in epilepsy: epidemiology, mechanisms, and prevention. Lancet Neurol 15(10):1075–1088. https://doi.org/10.1016/S1474-4422(16)30158-2
Doyle T, Moncorgé O, Bonaventure B, Pollpeter D, Lussignol M, Tauziet M, Apolonia L, Catanese M-T, Goujon C, Malim MH (2018) The interferon-inducible isoform of NCOA7 inhibits endosome-mediated viral entry. Nat Microbiol 3(12):1369–1376. https://doi.org/10.1038/s41564-018-0273-9
Farrell JS, Wolff MD, Teskey GC (2017) Neurodegeneration and pathology in epilepsy: clinical and basic perspectives. Adv Neurobiol 15:317–334. https://doi.org/10.1007/978-3-319-57193-5_12
Fialho GL, Wolf P, Walz R, Lin K (2021) SUDEP—more attention to the heart? A narrative review on molecular autopsy in epilepsy. Seizure 87:103–106. https://doi.org/10.1016/j.seizure.2021.03.010
French J, Friedman D (2018) The evolving landscape of epilepsy neuropathology. Lancet Neurol 17(3):202–203. https://doi.org/10.1016/S1474-4422(17)30429-5
Guo P, Ma Y, Deng G, Li L, Gong Y, Yang F, You Y (2021) CYR61, regulated by miR-22-3p and MALAT1, promotes autophagy in HK-2 cell inflammatory model. Transl Androl Urol 10(8):3486–3500. https://doi.org/10.21037/tau-21-623
Guo Z, Zhang H, Fu Y, Kuang J, Zhao B, Zhang L, Lin J, Lin S, Wu D, Xie G (2023) Cancer-associated fibroblasts induce growth and radioresistance of breast cancer cells through paracrine IL-6. Cell Death Discov 9(1):6. https://doi.org/10.1038/s41420-023-01306-3
Heuser K, Enger R (2021) Astrocytic Ca signaling in epilepsy. Front Cell Neurosci 15:695380. https://doi.org/10.3389/fncel.2021.695380
Hsu P-L, Su B-C, Kuok Q-Y, Mo F-E (2013) Extracellular matrix protein CCN1 regulates cardiomyocyte apoptosis in mice with stress-induced cardiac injury. Cardiovasc Res 98(1):64–72. https://doi.org/10.1093/cvr/cvt001
Jin R, Li Y, Jin H, Yoon HS, Choi JS, Kim J, Yoon HJ, Yoon KC (2022) Melatonin type 2 receptor activation regulates blue light exposure-induced mouse corneal epithelial damage by modulating impaired autophagy and apoptosis. Int J Mol Sci 23(19):11341. https://doi.org/10.3390/ijms231911341
Joensuu T, Tegelberg S, Reinmaa E, Segerstråle M, Hakala P, Pehkonen H, Korpi ER, Tyynelä J, Taira T, Hovatta I, Kopra O, Lehesjoki A-E (2014) Gene expression alterations in the cerebellum and granule neurons of Cstb(−/−) mouse are associated with early synaptic changes and inflammation. PLoS ONE 9(2):e89321. https://doi.org/10.1371/journal.pone.0089321
Jun J-I, Lau LF (2010) The matricellular protein CCN1 induces fibroblast senescence and restricts fibrosis in cutaneous wound healing. Nat Cell Biol 12(7):676–685. https://doi.org/10.1038/ncb2070
Kalozoumi G, Kel-Margoulis O, Vafiadaki E, Greenberg D, Bernard H, Soreq H, Depaulis A, Sanoudou D (2018) Glial responses during epileptogenesis in Mus musculus point to potential therapeutic targets. PLoS ONE 13(8):e0201742. https://doi.org/10.1371/journal.pone.0201742
Kang J, Bishayee K, Huh S-O (2021) Azoxystrobin impairs neuronal migration and induces ROS dependent apoptosis in cortical neurons. Int J Mol Sci 22(22):12495. https://doi.org/10.3390/ijms222212495
Kim K-H, Won JH, Cheng N, Lau LF (2018) The matricellular protein CCN1 in tissue injury repair. J Cell Commun Signal 12(1):273–279. https://doi.org/10.1007/s12079-018-0450-x
Koyuncuoğlu T, Vızdıklar C, Üren D, Yılmaz H, Yıldırım Ç, Atal SS, Akakın D, Kervancıoğlu Demirci E, Yüksel M, Yeğen BÇ (2017) Obestatin improves oxidative brain damage and memory dysfunction in rats induced with an epileptic seizure. Peptides 90:37–47. https://doi.org/10.1016/j.peptides.2017.02.005
Lai C-C, Tang C-Y, Fu S-K, Tseng W-C, Tseng K-W (2022) Effects of swimming training on myocardial protection in rats. Biomed Rep 16(3):19. https://doi.org/10.3892/br.2022.1502
Li H, Li T, Wang H, He X, Li Y, Wen S, Peng R, Nie Y, Lu Y, Yang H, Ye Y, Shi G, Chen Y (2021) Diabetes promotes retinal vascular endothelial cell injury by inducing CCN1 expression. Front Cardiovasc Med 8:689318. https://doi.org/10.3389/fcvm.2021.689318
Lin S, Ye M-Y, Fu Q-Y, Pan C-L, Liu Y-J, Zheng L-M, Hong Q, Chen Y-H (2023) Cholic acid exposure during late pregnancy causes placental dysfunction and fetal growth restriction by reactive oxygen species-mediated activation of placental GCN2/eIF2α pathway. FASEB J 37(3):e22820. https://doi.org/10.1096/fj.202202126R
Manford M (2017) Recent advances in epilepsy. J Neurol 264(8):1811–1824. https://doi.org/10.1007/s00415-017-8394-2
Palfi A, Chadderton N, Millington-Ward S, Post I, Humphries P, Kenna PF, Farrar GJ (2022) AAV-PHP.eB transduces both the inner and outer retina with high efficacy in mice. Mol Ther Methods Clin Dev 25:236–249. https://doi.org/10.1016/j.omtm.2022.03.016
Peng L, Lu Y, Gu Y, Liang B, Li Y, Li H, Ke Y, Zhu H, Li Z (2023) Mechanisms of action of Lycium barbarum polysaccharide in protecting against vitiligo mice through modulation of the STAT3-Hsp70-CXCL9/CXCL10 pathway. Pharm Biol 61(1):281–287. https://doi.org/10.1080/13880209.2022.2163406
Pitkanen A, Nissinen J, Nairismagi J, Lukasiuk K, Grohn OH, Miettinen R, Kauppinen R (2002) Progression of neuronal damage after status epilepticus and during spontaneous seizures in a rat model of temporal lobe epilepsy. Prog Brain Res 135:67–83. https://doi.org/10.1016/S0079-6123(02)35008-8
Racine RJ (1972) Modification of seizure activity by electrical stimulation. II. Motor seizure. Electroencephalogr Clin Neurophysiol 32(3):281–294. https://doi.org/10.1016/0013-4694(72)90177-0
Rong S, Wan D, Fan Y, Liu S, Sun K, Huo J, Zhang P, Li X, Xie X, Wang F, Sun T (2019) Amentoflavone affects epileptogenesis and exerts neuroprotective effects by inhibiting NLRP3 inflammasome. Front Pharmacol 10:856. https://doi.org/10.3389/fphar.2019.00856
Shimada T, Yoshida T, Yamagata K (2016) Neuritin mediates activity-dependent axonal branch formation in part via FGF signaling. J Neurosci 36(16):4534–4548. https://doi.org/10.1523/JNEUROSCI.1715-15.2016
Su B-C, Hsu P-L, Mo F-E (2020) CCN1 triggers adaptive autophagy in cardiomyocytes to curb its apoptotic activities. J Cell Commun Signal 14(1):93–100. https://doi.org/10.1007/s12079-019-00534-6
Thom M (2018) New perspectives in epilepsy neuropathology. Neuropathol Appl Neurobiol 44(1):3–5. https://doi.org/10.1111/nan.12464
Vezzani A, French J, Bartfai T, Baram TZ (2011) The role of inflammation in epilepsy. Nat Rev Neurol 7(1):31–40. https://doi.org/10.1038/nrneurol.2010.178
Vicente-Gutiérrez C, Jiménez-Blasco D, Quintana-Cabrera R (2021) Intertwined ROS and metabolic signaling at the neuron-astrocyte interface. Neurochem Res 46(1):23–33. https://doi.org/10.1007/s11064-020-02965-9
Wang C, Feng X, Su D, Chen Z, Wang S, Tang M, Huang M, Nie L, Zhang H, Li S, Yin L, Johnson RL, Hart T, Chen J (2022) Integrated screens uncover a cell surface tumor suppressor gene KIRREL involved in Hippo pathway. Proc Natl Acad Sci USA 119(25):e2121779119. https://doi.org/10.1073/pnas.2121779119
Wang L, Zhou B-Q, Li Y-H, Jiang Q-Q, Cong W-H, Chen K-J, Wen X-M, Wu Z-Z (2023) Lactoferrin modification of berberine nanoliposomes enhances the neuroprotective effects in a mouse model of Alzheimer’s disease. Neural Regen Res 18(1):226–232. https://doi.org/10.4103/1673-5374.344841
Wojtas MN, Pandey RR, Mendel M, Homolka D, Sachidanandam R, Pillai RS (2017) Regulation of m6A transcripts by the 3’→5’ RNA helicase YTHDC2 is essential for a successful meiotic program in the mammalian germline. Mol Cell 68(2):374. https://doi.org/10.1016/j.molcel.2017.09.021
Yang N, Guan Q-W, Chen F-H, Xia Q-X, Yin X-X, Zhou H-H, Mao X-Y (2020) Antioxidants targeting mitochondrial oxidative stress: promising neuroprotectants for epilepsy. Oxid Med Cell Longev 2020:6687185. https://doi.org/10.1155/2020/6687185
Yang W, Bai J, Song X, Zhang S, Chen N, You T, Yi K, Li Z, Xie D, Xie X (2021) CCN1 gene polymorphisms associated with congenital heart disease susceptibility in Northwest Chinese population from different high-altitude areas. Environ Sci Pollut Res Int 28(40):56927–56937. https://doi.org/10.1007/s11356-021-14428-x
Yoshida Y, Togi K, Matsumae H, Nakashima Y, Kojima Y, Yamamoto H, Ono K, Nakamura T, Kita T, Tanaka M (2007) CCN1 protects cardiac myocytes from oxidative stress via beta1 integrin-Akt pathway. Biochem Biophys Res Commun 355(3):611–618
Yu Y, Oh S-Y, Kim HY, Choi J-Y, Jo SA, Jo I (2022) Valproic acid-induced CCN1 promotes osteogenic differentiation by increasing CCN1 protein stability through HDAC1 inhibition in tonsil-derived mesenchymal stem cells. Cells 11(3):534. https://doi.org/10.3390/cells11030534
Zhao G, Huang B-L, Rigueur D, Wang W, Bhoot C, Charles KR, Baek J, Mohan S, Jiang J, Lyons KM (2018) CYR61/CCN1 regulates sclerostin levels and bone maintenance. J Bone Miner Res 33(6):1076–1089. https://doi.org/10.1002/jbmr.3394
Acknowledgements
None.
Funding
This study was supported by National Natural Science Foundation of China (Grant no: 82001379, 81771403 and 81974205), Natural Science Foundation of Hunan Province, China (Grant No: 2020JJ5952) and Natural Science Foundation of Zhejiang Province, China (Grant no: LZ20H090001).
Author information
Authors and Affiliations
Contributions
YL performed the experiments and wrote the paper. SH and YZ coordinated the animal experiment. HhZ collected the samples and assisted with the experiments. HtZ conceived the study, designed the experiments, and revised the paper. All the authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors have not disclosed any competing interests.
Ethical Approval and Consent to Participate
All the procedures were approved by the Medical Ethics Committee of Xiangya Hospital of Central South University (approval number: 202009499). All the animal experimental procedures were approved by the Experimental Animal Welfare Ethics Committee of Xiangya Hospital of Central South University (approval number: 2020sydw0635).
Consent for Publication
Consent for publication was obtained from the participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liao, Y., Huang, S., Zhang, Y. et al. Decrease of Cellular Communication Network Factor 1 (CCN1) Attenuates PTZ-Kindled Epilepsy in Mice. Cell Mol Neurobiol 43, 4279–4293 (2023). https://doi.org/10.1007/s10571-023-01420-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10571-023-01420-x