Abstract
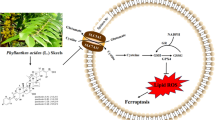
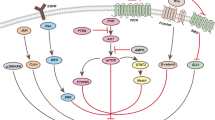
Acute myeloid leukemia (AML) is a malignant cancer of the hematopoietic system. Although the effectiveness of arsenic compounds has been recognized and applied clinically, some patients are still found resistant to this chemotherapy. In this study, we investigated that a synthetic thyroid hormone analog (TA), 2-iodo-4-nitro-1-(o-tolyloxy) benzene, had a strong apoptosis effect on U937 cells. U937 cells were treated with TA, and examinted the generation of reactive oxygen species (ROS), dysfunction of mitochondria, expression of pro-apoptosis and anti-apoptosis, and cleavage of caspase-3 and Poly (ADP-ribose) polymerase (PARP). Further, it is also evaluated that insight molecular mechanism and signaling pathways involved in the study. It is found that TA significantly induced apoptosis in U937 cells through production of ROS, dysfunction of mitochondria, and activation of caspase cascade. It was also observed that MAPK signaling pathway including ERK, JNK, and P38 signals are involved in the induction of apoptosis. Moreover, marked activation of autophagy and ER stress markers such as LC3, P62, Beclin1 and GRP78, CHOP were observed, respectively. Pretreatment with ER stress inhibitor tauroursodeoxycholic acid (TUDCA) and autophagy inhibitor 3-Methyladenine (3-MA) have successfully attenuated and aggravated TA-induced apoptosis, respectively. We further confirmed the active involvement of ER stress and autophagy signals. In conclusion, TA induced apoptosis through ER stress and activation of autophagy, and the latter is not conducive to TA-induced cell death. Our results may provide a new insight into the strategic development of novel therapy for the treatment of AML.






Similar content being viewed by others
Data availability
All data generated or analysed during this study are included in this published article [and its supplementary information files].
References
Meyers J, Yu Y, Kaye JA, Davis KL (2013) Medicare fee-for-service enrollees with primary acute myeloid leukemia: An analysis of treatment patterns, survival, and healthcare resource utilization and costs. Appl Health Econ Health Policy 11:275–286. https://doi.org/10.1007/s40258-013-0032-2
Buki KG, Kirsten E, Bauer PI et al (1997) Inhibition of migration of MDA-MB-231 cells by methyl-3,5-diiodo-4-(4′-methoxyphenoxy) benzoate (DIME). Int J Oncol 11:1247–1250. https://doi.org/10.3892/ijo.11.6.1247
Chen X, Pine P, Knapp AM et al (1998) Oncocidin A1: A novel tubulin-binding drug with antitumor activity against human breast and ovarian carcinoma xenografts in nude mice. Biochem Pharmacol 56:623–633. https://doi.org/10.1016/S0006-2952(98)00210-X
Evano G, Blanchard N, Toumi M (2008) Copper-mediated coupling reactions and their applications in natural products and designed biomolecules synthesis. Chem Rev 108:3054–3131. https://doi.org/10.1021/cr8002505
Boelaert K, Franklyn JA (2005) Thyroid hormone in health and disease. J Endocrinol 187:1–15. https://doi.org/10.1677/joe.1.06131
Lin HY, Tang HY, Shih A et al (2007) Thyroid hormone is a MAPK-dependent growth factor for thyroid cancer cells and is anti-apoptotic. Steroids 72:180–187. https://doi.org/10.1016/j.steroids.2006.11.014
Tang HY, Lin HY, Zhang S et al (2004) Thyroid hormone causes mitogen-activated protein kinase-dependent phosphorylation of the nuclear estrogen receptor. Endocrinology 145:3265–3272. https://doi.org/10.1210/en.2004-0308
Muñoz A, Bernal J (1997) Biological activities of thyroid hormone receptors. Eur J Endocrinol 137:433–445. https://doi.org/10.1530/eje.0.1370433
Goldar S, Khaniani MS, Derakhshan SM, Baradaran B (2015) Molecular mechanisms of apoptosis and roles in cancer development and treatment. Asian Pacific J Cancer Prev 16:2129–2144. https://doi.org/10.7314/APJCP.2015.16.6.2129
Signore M, Ricci-Vitiani L, De Maria R (2013) Targeting apoptosis pathways in cancer stem cells. Cancer Lett 332:374–382. https://doi.org/10.1016/j.canlet.2011.01.013
Sun L, Cui ZG, Zakki SA et al (2018) Mechanistic study of nonivamide enhancement of hyperthermia-induced apoptosis in U937 cells. Free Radic Biol Med 120:147–159. https://doi.org/10.1016/j.freeradbiomed.2018.03.017
Zakki SA, Cui ZG, Sun L et al (2018) Baicalin augments hyperthermia-induced apoptosis in U937 cells and modulates the MAPK pathway via ROS generation. Cell Physiol Biochem 45:2444–2460. https://doi.org/10.1159/000488263
Brewer JW, Diehl JA (2000) PERK mediates cell-cycle exit during the mammalian unfolded protein response. Proc Natl Acad Sci U S A 97:12625–12630. https://doi.org/10.1073/pnas.220247197
Høyer-Hansen M, Jäättelä M (2007) Connecting endoplasmic reticulum stress to autophagy by unfolded protein response and calcium. Cell Death Differ 14:1576–1582. https://doi.org/10.1038/sj.cdd.4402200
Feng QW, Cui ZG, Jin YJ et al (2019) Protective effect of dihydromyricetin on hyperthermia-induced apoptosis in human myelomonocytic lymphoma cells. Apoptosis 24:290–300. https://doi.org/10.1007/s10495-019-01518-y
Zhang Z, Zhang L, Zhou L et al (2019) Redox signaling and unfolded protein response coordinate cell fate decisions under ER stress. Redox Biol. https://doi.org/10.1016/j.redox.2018.11.005
Brenner C, Cadiou H, Vieira HLA et al (2000) Bcl-2 and Bax regulate the channel activity of the mitochondrial adenine nucleotide translocator. Oncogene 19:329–336. https://doi.org/10.1038/sj.onc.1203298
Légiot A, Céré C, Dupoiron T et al (2019) Mitochondria-associated membranes (MAMs) are involved in bax mitochondrial localization and cytochrome c release. Microb Cell 6:257–266. https://doi.org/10.15698/mic2019.05.678
Eisenberg-Lerner A, Bialik S, Simon HU, Kimchi A (2009) Life and death partners: apoptosis, autophagy and the cross-talk between them. Cell Death Differ 16:966–975. https://doi.org/10.1038/cdd.2009.33
Chen Y, Zhang W, Guo X et al (2019) The crosstalk between autophagy and apoptosis was mediated by phosphorylation of Bcl-2 and beclin1 in benzene-induced hematotoxicity. Cell Death Dis. https://doi.org/10.1038/s41419-019-2004-4
Darling NJ, Cook SJ (2014) The role of MAPK signalling pathways in the response to endoplasmic reticulum stress. Biochim Biophys Acta Mol Cell Res 1843:2150–2163. https://doi.org/10.1016/j.bbamcr.2014.01.009
Wu YT, Tan HL, Shui G et al (2010) Dual role of 3-methyladenine in modulation of autophagy via different temporal patterns of inhibition on class I and III phosphoinositide 3-kinase. J Biol Chem 285:10850–10861. https://doi.org/10.1074/jbc.M109.080796
Shah S, Lockhart AC, Saito WY et al (2001) The novel tubulin-binding drug BTO-956 inhibits R3230Ac mammary carcinoma growth and angiogenesis in fischer 344 rats. Clin Cancer Res 7:2590–2596
Calabrese V, Scapagnini G, Ravagna A et al (2004) Increased expression of heat shock proteins in rat brain during aging: Relationship with mitochondrial function and glutathione redox state. Mech Ageing Dev 125:325–335. https://doi.org/10.1016/j.mad.2004.01.003
Chen HH, Chen YT, Huang YW et al (2012) 4-Ketopinoresinol, a novel naturally occurring ARE activator, induces the Nrf2/HO-1 axis and protects against oxidative stress-induced cell injury via activation of PI3K/AKT signaling. Free Radic Biol Med 52:1054–1066. https://doi.org/10.1016/j.freeradbiomed.2011.12.012
Schmidt-Rohr K (2020) Oxygen is the high-energy molecule powering complex multicellular life: fundamental corrections to traditional bioenergetics. ACS Omega 5:2221–2233. https://doi.org/10.1021/acsomega.9b03352
Finley LWS, Carracedo A, Lee J et al (2011) SIRT3 opposes reprogramming of cancer cell metabolism through HIF1α destabilization. Cancer Cell 19:416–428. https://doi.org/10.1016/j.ccr.2011.02.014
Prola A, Da Silva JP, Guilbert A et al (2017) SIRT1 protects the heart from ER stress-induced cell death through eIF2α deacetylation. Cell Death Differ 24:343–356. https://doi.org/10.1038/cdd.2016.138
Shi T, Wang F, Stieren E, Tong Q (2005) SIRT3, a mitochondrial sirtuin deacetylase, regulates mitochondrial function and thermogenesis in brown adipocytes. J Biol Chem 280:13560–13567. https://doi.org/10.1074/jbc.M414670200
Ibrahim IM, Abdelmalek DH, Elfiky AA (2019) GRP78: a cell’s response to stress. Life Sci 226:156–163. https://doi.org/10.1016/j.lfs.2019.04.022
Marciniak SJ, Yun CY, Oyadomari S et al (2004) CHOP induces death by promoting protein synthesis and oxidation in the stressed endoplasmic reticulum. Genes Dev 18:3066–3077. https://doi.org/10.1101/gad.1250704
Nakagawa T, Zhu H, Morishima N et al (2000) Caspase-12 mediates endoplasmic-reticulum-specific apoptosis and cytotoxicity by amyloid-β. Nature 403:98–103. https://doi.org/10.1038/47513
Marchi S, Patergnani S, Pinton P (2014) The endoplasmic reticulum-mitochondria connection: one touch, multiple functions. Biochim Biophys Acta Bioenerg 1837:461–469. https://doi.org/10.1016/j.bbabio.2013.10.015
Martinou JC, Youle RJ (2011) Mitochondria in apoptosis: Bcl-2 family members and mitochondrial dynamics. Dev Cell 21:92–101. https://doi.org/10.1016/j.devcel.2011.06.017
Gonzalvez F, Bessoule JJ, Rocchiccioli F et al (2005) Role of cardiolipin on tBid and tBid/Bax synergistic effects on yeast mitochondria. Cell Death Differ 12:659–667. https://doi.org/10.1038/sj.cdd.4401585
Fang H, Harned TM, Kalous O et al (2011) Synergistic activity of fenretinide and the Bcl-2 family protein inhibitor ABT-737 against human neuroblastoma. Clin Cancer Res 17:7093–7104. https://doi.org/10.1158/1078-0432.CCR-11-0578
Colié S, Van Veldhoven PP, Kedjouar B et al (2009) Disruption of sphingosine 1-phosphate lyase confers resistance to chemotherapy and promotes oncogenesis through Bcl-2/Bcl-xL upregulation. Cancer Res 69:9346–9353. https://doi.org/10.1158/0008-5472.CAN-09-2198
Scherr AL, Gdynia G, Salou M et al (2016) Bcl-xL is an oncogenic driver in colorectal cancer. Cell Death Dis 7:1–10. https://doi.org/10.1038/cddis.2016.233
Jazirehi AR, Vega MI, Chatterjee D et al (2004) Inhibition of the Raf-MEK1/2-ERK1/2 signaling pathway, BCL-xL down-regulation, and chemosensitization of non-Hodgkin’s lymphoma B cells by rituximab. Cancer Res 64:7117–7126. https://doi.org/10.1158/0008-5472.CAN-03-3500
Tsujimoto Y, Shimizu S (2005) Another way to die: autophagic programmed cell death. Cell Death Differ 12:1528–1534. https://doi.org/10.1038/sj.cdd.4401777
Amaravadi R, Kimmelman AC, White E (2016) Recent insights into the function of autophagy in cancer. Genes Dev 30:1913–1930. https://doi.org/10.1101/gad.287524.116
McKnight NC, Yue Z (2013) Beclin 1, an essential component and master regulator of PI3K-III in health and disease. Curr Pathobiol Rep 1:231–238. https://doi.org/10.1007/s40139-013-0028-5
Storniolo A, Alfano V, Carbotta S et al (2018) IRE1α deficiency promotes tumor cell death and eIF2α degradation through PERK dipendent autophagy. Cell Death Discov 4:3. https://doi.org/10.1038/s41420-017-0002-9
Gardner BM, Walter P (2011) Unfolded proteins are Ire1-activating ligands that directly induce the unfolded protein response. Science 333(6051):1891–1894. https://doi.org/10.1126/science.1209126
Wei Y, Sinha S, Levine B (2008) Dual role of JNK1-mediated phosphorylation of Bcl-2 in autophagy and apoptosis regulation. Autophagy 4:949–951. https://doi.org/10.4161/auto.6788
Ron D, Hubbard SR (2008) How IRE1 reacts to ER stress. Cell 132:24–26. https://doi.org/10.1016/j.cell.2007.12.017
Ji S, Sun R, Xu K et al (2019) Prodigiosin induces apoptosis and inhibits autophagy via the extracellular signal-regulated kinase pathway in K562 cells. Toxicol In Vitro 60:107–115. https://doi.org/10.1016/j.tiv.2019.05.003
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, YL., Zhou, DJ., Cui, ZG. et al. The molecular mechanism of a novel derivative of BTO-956 induced apoptosis in human myelomonocytic lymphoma cells. Apoptosis 26, 219–231 (2021). https://doi.org/10.1007/s10495-021-01664-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10495-021-01664-2