Abstract
Purpose
To examine the changes in the pelvic floor structure caused by pregnancy and delivery.
Methods
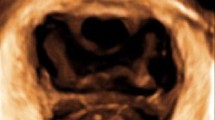
A total of 141 nulliparous women were examined with three-dimensional transperineal ultrasound (3D-TPU) at the 24th and 34th weeks of gestation, 5th day postpartum, and 1 month postpartum. Puborectalis muscle trauma was diagnosed and the area of levator hiatus (ALH) was measured.
Results
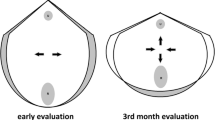
One hundred and five normal vaginal deliveries, 19 vacuum/forceps deliveries, and 17 cesarean deliveries were included. In the normal delivery group, the rate of puborectalis muscle trauma was low and showed no significant change between the 24th and 34th weeks of gestation (12.5% vs. 17.2%, p = 0.42). The rate of trauma significantly increased to 70.2% at the 5th day postpartum (p < 0.001). There was no significant difference between the rates at the 5th day postpartum and 1 month postpartum (73.7%, p = 0.60). The same trend was found in the vacuum/forceps group. In the cesarean section group, no significant change was observed throughout pregnancy and postpartum periods. In the normal delivery group, ALH significantly increased between the 24th and 34th week (14.1 ± 2.6 cm2 vs. 14.6 ± 3.4 cm2, p = 0.007). ALH markedly increased to 20.9 ± 4.8 cm2 at the 5th day postpartum (p < 0.001). ALH at 1 month postpartum decreased to 17.0 ± 4.3 cm2 (p < 0.001), but did not return to the value at the 24th week (p < 0.001).
Conclusions
Vaginal childbirth results in enlargement of the levator hiatus. Pelvic floor muscles in pregnant women are affected not only by mechanical damage associated with delivery but also by physiologic changes during pregnancy. The effects of pregnancy and delivery on pelvic floor muscles may persist after delivery.




Similar content being viewed by others
References
Halban J, Tandler J. Anatomie und aetiologie des genitalprolapse beim weibe. Wilhelm Braumuller, Vienna, 1907 [trans: Porges RF, Porges JC]. Obstet Gynecol. 1960;15:790.
Dietz HP, Simpson J. Levator trauma is associated with pelvic organ prolapse. BJOG. 2008;115:979–84.
Wong V, Shek K, Goh J, et al. Is levator avulsion a predictor for cystocele recurrence following anterior compartment mesh? Neurourol Urodyn. 2011;30:879–80.
Dietz HP, Chantarasorn V, Shek KL. Levator avulsion is a risk factor for cystocele recurrence. Ultrasound Obstet Gynecol. 2010;36:76–80.
Model A, Shek KL, Dietz HP. Levator defects are associated with prolapse after pelvic floor surgery. Eur J Obstet Gynecol Reprod Biol. 2010;153:220–3.
Weemhoff M, Vergeldt T, Notten K, et al. Avulsion of puborectalis muscle and other risk factors for cystocele recurrence: a 2-year follow-up study. Int Urogynecol J. 2012;23:65–71.
Morgan D, Larson K, Lewicky-Gaupp C, et al. Vaginal support as determined by levator ani defect status 6 weeks after primary surgery for pelvic organ prolapse. Int J Gynaecol Obstst. 2011;114:141–4.
Dietz HP. Ultrasound imaging of the pelvic floor. Part II: three-dimensional or volume imaging. Ultrasound Obstet Gynecol. 2004;23:615–25.
Valsky D, Lipschuetz M, Bord A, et al. Fetal head circumference and length of second stage of labor are risk factors for levator ani muscle injury, diagnosed by 3-dimensional transperineal ultrasound in primiparous women. Am J Obstet Gynecol. 2009;201(91):e1-7.
Dietz HP, Moegni F, Shek KL. Diagnosis of levator avulsion injury: a comparison of three methods. Ultrasound Obstet Gynecol. 2012;40:693–8.
Shek KL, Dietz HP. The effect of childbirth on hiatal dimensions. Obstet Gynecol. 2009;113:1272–8.
Handa VL, Blomquist JL, Knoepp LR, et al. Pelvic floor disorders 5–10 years after vaginal or cesarean childbirth. Obstet Gynecol. 2011;118:777–84.
Dietz HP, Bennett MJ. The effect of childbirth on pelvic organ mobility. Obstet Gynecol. 2003;102:223–8.
Glazener C, Elders A, MacArthur C, et al. Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse. BJOG. 2013;120:161–8.
Gyhagen M, Bullarbo M, Nielsen T, et al. The prevalence of urinary incontinence 20 years after childbirth:a national cohort study in singleton primiparae after vaginal or caesarean delivery. BJOG. 2013;120:144–51.
Leijonhufvud A, Lundholm C, Cnattingius S, et al. Risks of stress urinary incontinence and pelvic organ prolapse surgery in relation to mode of childbirth. Am J Obstet Gynecol. 2011;204(70):e1-7.
Rortveit G, Daltveit A, Hannestad Y, et al. Urinary incontinence after vaginal delivery or cesarean section. Engl J Med. 2003;348:900–7.
White RD, McQuown D, McCarthy TA, et al. Real-time ultrasonography in the evaluation of urinary stress incontinence. Am J Obstet Gynecol. 1980;138:235–7.
Dietz HP, Shek C, Clarke B. Biometry of the pubovisceral muscle and levator hiatus by three-dimensional pelvic floor ultrasound. Ultrasound Obstet Gynecol. 2005;25:580–5.
Lowder JL, Debes KM, Moon DK, et al. Biomechanical adaptations of the rat vagina and supportive tissues in pregnancy to accommodate delivery. Obstet Gynecol. 2007;109:136–43.
Siafarikas F, Stær-Jensen J, Hilde G, et al. Levator hiatus dimensions in late pregnancy and the process of labor: a 3- and 4-dimensional transperineal ultrasound study. Am J Obstet Gynecol. 2014;210(484):e1-7.
Valsky DV, Lipschuetz M, Cohen SM, et al. Persistence of levator ani sonographic defect detected by three-dimensional transperineal sonography in primiparous women. Ultrasound Obstet Gynecol. 2015;46:724–9.
García-Mejido JA, Fernández-Palacín A, Barby MJB, et al. A comparable rate of levator ani muscle injury in operative vaginal delivery (forceps and vacuum) according to the characteristics of the instrumentation. Acta Obstet Gynecol Scand. 2019;98:729–36.
Acknowledgements
We would like to thank Honorary Professor Ichiro Nagata, Department of Obstetrics, National Defense Medical College, and Dr. Koichi Kobayashi, Assistant Director, Tokyo Yamate Medical Center, and Director of the Department of Obstetrics and Gynecology, for their advice regarding the study design and analysis of the results.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical considerations
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (Institutional Review Board of Nerima Hikarigaoka Hospital) and with the Helsinki Declaration of 1964 and later versions.
Informed consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Nishibayashi, M., Okagaki, R. Ultrasonographic evaluation of pelvic floor structure at antepartum and postpartum periods using three-dimensional transperineal ultrasound. J Med Ultrasonics 48, 345–351 (2021). https://doi.org/10.1007/s10396-021-01100-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10396-021-01100-7