Abstract
Background
New York City began public reporting of restaurant sanitary inspection grades in 2010. The policy’s impact on the incidence of foodborne illness has not been previously studied.
Methods
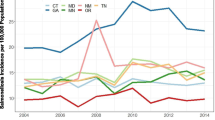
We used a retrospective cohort design to evaluate whether the introduction of sanitary grades in 2010 reduced the incidence of Salmonellosis. To estimate the policy impact, we performed a difference-in-differences analysis in which in New York City was compared to a “synthetic control group” consisting of a weighted sample of comparison geographies. We evaluated reported Salmonellosis cases from April 2003 through December 2015 from the National Notifiable Diseases Surveillance System (NNDS) (National Notifiable Diseases Surveillance System, Weekly Tables of Infectious Disease Data n.d.). Our main outcome measure was quarterly risk-adjusted cases of reported Salmonellosis per 100,000 residents.
Results
Results of our difference-in-differences analysis found that the New York City restaurant sanitary grades program was associated with a non-significant reduction in risk-adjusted cases of reported Salmonellosis per 100,000 (−0.31, 95% confidence interval = (−1.41, 0.80)). This finding was robust across all specifications.
Conclusions
Consistent with recent evidence that public reporting has had little impact on public health, public reporting of restaurant sanitary inspection grades did not appear to decrease the incidence of Salmonellosis.

Similar content being viewed by others
References
2010 Census Urban and Rural Classification and Urban Area Criteria. (n.d.). Retrieved from https://www.census.gov/geo/reference/ua/urban-rural-2010.htm
Abadie A, Gardeazabal J (2003) The economic costs of conflict: a case study of the Basque Country. Am Econ Rev 93(1):113–132
Abadie A, Diamond A, Hainmueller J (2010) Synthetic control methods for comparative case studies: estimating the effect of California’s tobacco control program. J Am Stat Assoc 105(490):493–505. https://doi.org/10.1198/jasa.2009.ap08746
Abadie A, Diamond A, & Hainmueller J. (2014). SYNTH: Stata module to implement synthetic control methods for comparative case Studies. Retrieved from https://econpapers.repec.org/RePEc:boc:bocode:s457334
Angelo KM, Nisler AL, Hall AJ, Brown LG, Gould LH (2017) Epidemiology of restaurant-associated foodborne disease outbreaks, United States, 1998–2013. Epidemiol Infect 145(3):523–534. https://doi.org/10.1017/S0950268816002314
Angulo FJ, Jones TF (2006) Eating in restaurants: a risk factor for foodborne disease? Clin Infect Dis 43(10):1324–1328. https://doi.org/10.1086/508540
Cameron AC, Miller DL (2015) A Practioner’s guide to cluster-robust inference. J Hum Resour 50(2):317–372
Cost Estimates of Foodborne Illnesses. (n.d.). Retrieved from https://www.ers.usda.gov/data-products/cost-estimates-of-foodborne-illnesses/cost-estimates-of-foodborne-illnesses/#ValueofStatistical Life
County Intercesal Datasets: 2000 - 2010. (n.d.). Retrieved from https://www.census.gov/data/datasets/time-series/demo/popest/intercensal-2000-2010-counties.html
Donald SG, Lang K (2007) Inference with difference-in-differences and other panel data. Rev Econ Stat 89(2):221–233
Doorduyn Y, Van Den Brandhof WE, Van Duynhoven YTHP, Wannet WJB, & Van Pelt W. (2006). Risk factors for Salmonella Enteritidis and typhimurium (DT104 and non-DT104) infections in the Netherlands: predominant roles for raw eggs in Enteritidis and sandboxes in typhimurium infections. Epidemiology and Infection. Cambridge, UK. https://doi.org/10.1017/S0950268805005406
Farley T (2011) Restaurant letter grading: the first year. New York City Department of Health andMental Hygiene
Fleetwood J, Rahman S, Holland D, Millson D, Thomson L, Poppy G (2019) As clean as they look? Food hygiene inspection scores, microbiological contamination, and foodborne illness. Food Control 96:76–86
Flood S, King M, Ruggles S, & Warren JR. (2017) Integrated public use microdata series, current population survey: version 5.0. [dataset]. Minneapolis: University of Minnesota. https://doi.org/10.18128/D030.V5.0
Hirth R. (2015). Gaming of quality ratings: evidence from dynamic staffing patterns. Academy Health Annual Research Meeting. Retrieved from https://academyhealth.confex.com/academyhealth/2015arm/meetingapp.cgi/Paper/2237
Ho DE (2012) Fudging the nudge: information disclosure and restaurant grading. Yale Law J 122:574–688
Ibrahim A, Dimick J, Sinha S, Hollingsworth J, Nuliyalu U, Ryan A (2018) Association of coded severity with readmission reduction after the hospital readmissions reduction program. JAMA IM 178(2):290–292
Jin GZ, Leslie P (2003) The effect of information on product quality: evidence from restaurant hygiene grade cards. Q J Econ 118(2):409–451. https://doi.org/10.1162/003355303321675428
Kolstad JT, Chernew ME (2009) Quality and consumer decision making in the market for health insurance and health care services. Med Care Res Rev 66(1_suppl):28S–52S. https://doi.org/10.1177/1077558708325887
Labor Force Data by County. (n.d.). Washington, DC. Retrieved from https://www.bls.gov/lau/#cntyaa
Marshall MN, Shekelle PG, Davies HTO, Smith PC (2003) Public reporting on quality in the United States and the United Kingdom. Health Aff 22(3):134–148
Meltzer R, Rothbart M, Schwartz A, Calabrese T, Silver D, Mijanovich T, Weinstein M (2019) What are the financial implications of public disclosure? Evidence from New York’s restaurant food safety grading policy. Public Finance Rev 47(1):170–201. https://doi.org/10.1177/1091142117715112
National Notifiable Diseases Surveillance System, Weekly Tables of Infectious Disease Data. (n.d.). Atlanta, GA. Retrieved from https://wonder.cdc.gov/mmwr/mmwrmorb.asp
Newman KL, Leon JS, Rebolledo PA, Scallan E (2015) The impact of socioeconomic status on foodborne illness in high-income countries: a systematic review. Epidemiol Infect 143(12):2473–2485. https://doi.org/10.1017/S0950268814003847
Quarterly Census of Employment and Wages. (n.d.). Retrieved from https://www.bls.gov/cew/datatoc.htm
Ryan A, Detsky A (2015) Grade pending: lessons for hospital quality reporting from the new York City restaurant sanitation inspection program. J Hosp Med 10(2):116–119
Ryan A, Nallamothu BK, Dimick JB (2012) Medicare’s public reporting initiative on hospital quality had modest or no impact on mortality from three key conditions. Health Aff 31(3):585–592
Ryan A, Burgess JF, Dimick J (2015) Why we should not be indifferent to specification choices for difference-in-differences. Health Services Research Methods 50(4):1211–1235
Salmonella. (n.d.). Altanta, GA. Retrieved from https://www.cdc.gov/salmonella/reportspubs/surveillance.html
Scallan E, Jones TF, Cronquist A, Thomas S, Frenzen P, Hoefer D, Medus C, Angula FJ (2007) Factors associated with seeking medical care and submitting a stool sample in estimating the burden of foodborne illness. Foodborne Pathog Dis 3(4):432–438
Scallan E, Hoekstra RM, Angulo FJ, Tauxe RV, Widdowson MA, Roy SL, Jones JL, Griffin PM (2011) Foodborne illness acquired in the United States-major pathogens. Emerg Infect Dis 17(1):7–15. https://doi.org/10.3201/eid1701.P11101
Scott E (2003) Food safety and foodborne disease in 21st century homes. Can J Infect Dis 14(5):277–280
State Intercersal Datasets: 2000 - 2010. (n.d.). Retrieved from https://www.census.gov/data/datasets/time-series/demo/popest/intercensal-2000-2010-state.html
Varga C, Pearl DL, McEwen SA, Sargeant JM, Pollari F, & Guerin MT (2015a) Area-level global and local clustering of human Salmonella Enteritidis infection rates in the city of Toronto, Canada, 2007-2009. BMC Infect Dis 15(359). https://doi.org/10.1186/s12879-015-1106-6
Varga C, Pearl DL, McEwen SA, Sargeant JM, Pollari F, Guerin MT (2015b) Spatial-temporal epidemiology of human Salmonella Enteritidis infections with major phage types (PTs 1, 4, 5b, 8, 13, and 13a) in Ontario, Canada, 2008–2009. BMC Public Health, London. https://doi.org/10.1186/s12889-015-2592-6
Werner R, Konetzka RT, Stuart EA, Norton E, Polsky D, Park J (2009) The impact of public reporting on quality of post-acute care. Health Serv Res 44:1169–1187
Wong MR, McKelvey W, Ito K, Schiff C, Jacobson JB, Kass D (2015) Impact of a letter-grade program on restaurant sanitary conditions and diner behavior in New York City. Am J Public Health. https://doi.org/10.2105/AJPH.2014.302404
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
AMR and SK conceived the study design. AMR supervised the study. JE completed the analyses. SK and AMR led the writing of the manuscript. All authors assisted with the study concept, analysis plan, and contributed to the writing of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare they have no competing interests to disclose. Sam Krinsky's work on this study was conducted independently of his employment with the City of New York.
Ethical approval
This was an observational study which used publicly available datasets.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOC 152 kb)
Rights and permissions
About this article
Cite this article
Krinsky, S., Errickson, J. & Ryan, A.M. Grade pending: the effect of the New York City restaurant sanitary grades inspection program on Salmonellosis. J Public Health (Berl.) 30, 1171–1177 (2022). https://doi.org/10.1007/s10389-020-01384-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-020-01384-y