Abstract
Purpose
To compare the progression of posterior vitreous detachment (PVD) after cataract surgery in eyes with high myopia with that in eyes without high myopia.
Study design
Prospective observational study.
Methods
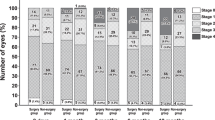
Eighty eyes of 80 patients with high myopia and 160 eyes of 160 patients without high myopia scheduled for phacoemulsification were recruited. PVD status was examined using swept-source optical coherence tomography at 2 days postoperatively (baseline) and at 3, 6, and 12 months postbaseline and classified into 5 stages: 0 (no PVD), 1 (paramacular PVD), 2 (perifoveal PVD), 3 (peripapillary PVD), and 4 (complete PVD). The PVD stage and incidence of progression to complete PVD of the 2 groups were compared.
Results
The mean PVD stage did not differ significantly between the groups at baseline or at 3 months postbaseline but was significantly more progressed in the high myopia group than in the nonhigh myopia group at 6 months and 12 months postbaseline (P ≤ 0.0201). The Kaplan–Meier survival rate for complete PVD was significantly lower in the high myopia group (P = 0.0129). After adjusting for age, sex, and baseline PVD stage, the hazard ratio for complete PVD was 1.68-fold higher in the high myopia group than in the nonhigh myopia group (P = 0.0326, 95% CI 1.04–2.70).
Conclusion
After cataract surgery, PVD progressed significantly faster in eyes with high myopia than in eyes without high myopia, and the relative risk for complete PVD was 1.68-fold higher in eyes with high myopia, suggesting that highly myopic eyes are at considerably high risk for retinal disease postoperatively.



Similar content being viewed by others
References
Gishti O, van den Nieuwenhof R, Verhoekx J, van Overdam K. Symptoms related to posterior vitreous detachment and the risk of developing retinal tears: a systematic review. Acta Ophthalmol. 2019;97:347–52.
Sarrafizadeh R, Hassan TS, Ruby AJ, Williams GA, Garretson BR, Capone A Jr, et al. Incidence of retinal detachment and visual outcome in eyes presenting with posterior vitreous separation and dense fundus-obscuring vitreous hemorrhage. Ophthalmology. 2001;108:2273–8.
Byer NE. Natural history of posterior vitreous detachment with early management as the premier line of defense against retinal detachment. Ophthalmology. 1994;101:1503–14.
Mitry D, Singh J, Yorston D, Siddiqui MA, Wright A, Fleck BW, et al. The predisposing pathology and clinical characteristics in the Scottish retinal detachment study. Ophthalmology. 2011;118:1429–34.
Yamada N, Kishi S. Tomographic features and surgical outcomes of vitreomacular traction syndrome. Am J Ophthalmol. 2005;139:112–7.
Johnson MW, Van Newkirk MR, Meyer KA. Perifoveal vitreous detachment is the primary pathogenic event in idiopathic macular hole formation. Arch Ophthalmol. 2001;119:215–22.
la Cour M, Friis J. Macular holes: classification, epidemiology, natural history and treatment. Acta Ophthalmol Scand. 2002;80:579–87.
Ripandelli G, Coppé AM, Parisi V, Olzi D, Scassa C, Chiaravalloti A, et al. Posterior vitreous detachment and retinal detachment after cataract surgery. Ophthalmology. 2007;114:692–7.
Mirshahi A, Höhn F, Lorenz K, Hattenbach LO. Incidence of posterior vitreous detachment after cataract surgery. J Cataract Refract Surg. 2009;35:987–91.
Ivastinovic D, Schwab C, Borkenstein A, Lackner EM, Wedrich A, Velikay-Parel M. Evolution of early changes at the vitreoretinal interface after cataract surgery determined by optical coherence tomography and ultrasonography. Am J Ophthalmol. 2012;153:705–9.
Hayashi S, Yoshida M, Hayashi K, Tsubota K. Progression of posterior vitreous detachment after cataract surgery. Eye (Lond). 2021. https://doi.org/10.1038/s41433-021-01732-6.
Chan CK, Lawrence FC. Macular hole after laser in situ keratomileusis and photorefractive keratectomy. Am J Ophthalmol. 2001;131:666–7.
Crim N, Esposito E, Monti R, Correa LJ, Serra HM, Urrets-Zavalia JA. Myopia as a risk factor for subsequent retinal tears in the course of a symptomatic posterior vitreous detachment. BMC Ophthalmol. 2017;17:226.
Gaucher D, Haouchine B, Tadayoni R, Massin P, Erginay A, Benhamou N, et al. Long-term follow-up of high myopic foveoschisis: natural course and surgical outcome. Am J Ophthalmol. 2007;143:455–62.
Shimada N, Tanaka Y, Tokoro T, Ohno-Matsui K. Natural course of myopic traction maculopathy and factors associated with progression or resolution. Am J Ophthalmol. 2013;156:948–57.
Akiba J. Prevalence of posterior vitreous detachment in high myopia. Ophthalmology. 1993;100:1384–8.
Itakura H, Kishi S, Li D, Nitta K, Akiyama H. Vitreous changes in high myopia observed by swept-source optical coherence tomography. Invest Ophthalmol Vis Sci. 2014;55:1447–52.
Hayashi K, Manabe SI, Hirata A, Yoshimura K. Posterior vitreous detachment in highly myopic patients. Invest Ophthalmol Vis Sci. 2020;61:33.
Takahashi H, Tanaka N, Shinohara K, Yokoi T, Yoshida T, Uramoto K, et al. Ultra-widefield optical coherence tomographic imaging of posterior vitreous in eyes with high myopia. Am J Ophthalmol. 2019;206:102–12.
Hayashi K, Yoshida M, Hayashi S, Yoshimura K. Short-term changes in prediction error after cataract surgery in eyes receiving 1 of 3 types of single-piece acrylic intraocular lenses. Am J Ophthalmol. 2020;219:12–20.
Hayashi K, Sato T, Manabe SI, Hirata A. Sex-related differences in the progression of posterior vitreous detachment with age. Ophthalmol Retina. 2019;3:237–43.
Itakura H, Kishi S. Evolution of vitreomacular detachment in healthy subjects. JAMA Ophthalmol. 2013;131:1348–52.
Yao Y, Lu Q, Wei L, Cheng K, Lu Y, Zhu X. Efficacy and complications of cataract surgery in high myopia. J Cataract Refract Surg. 2021;47:1473–80.
Qureshi MH, Steel DHW. Retinal detachment following cataract phacoemulsification: a review of the literature. Eye (Lond). 2020;34:616–31.
Lin JY, Ho WL, Ger LP, Sheu SJ. Analysis of factors correlated with the development of pseudophakic retinal detachment: a long-term study in a single medical center. Graefes Arch Clin Exp Ophthalmol. 2013;251:459–65.
Acknowledgements
The authors thank Dr Koji Yonemoto (Ryukyu University, Naha, Japan) for assistance with the statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
K. Hayashi, None; M. Yoshida, None; S. Hayashi, None; A. Hirata, None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Corresponding Author: Ken Hayashi
About this article
Cite this article
Hayashi, K., Yoshida, M., Hayashi, S. et al. Posterior vitreous detachment after cataract surgery in eyes with high myopia: an optical coherence tomography study. Jpn J Ophthalmol 66, 167–172 (2022). https://doi.org/10.1007/s10384-022-00903-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-022-00903-6