Abstract
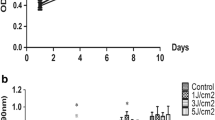
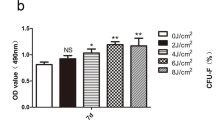
There are few studies on the effect of low-energy LED red light on periodontal tissue regeneration in an inflammatory environment. In this study, Cell Counting Kit-8 (CCK-8) assays were used to detect the effects of TNF-α at three different concentrations (0, 10 ng/ml, and 20 ng/ml) on the proliferation of human periodontal ligament stem cells (hPDLSCs), and 10 ng/ml was selected as the subsequent experimental stimulation concentration. CCK-8 assays were used to detect the effect of LED red light with energy density of 1 J/ cm2, 3 J/ cm2, and 5 J/cm2 on the proliferation of hPDLSCs. The promotion effect of energy density of 5 J/cm2 on the proliferation of hPDLSCS was the most obvious (p < 0.05). Set CON group, ODM group, ODM + 10 ng/ml TNF-α group, and ODM + 10 ng/ml TNF-α + 5 J/ cm2 LED red light group. Alkaline phosphatase staining and activity detection, alizarin red staining and calcium nodules quantitative detection of osteoblast differentiation products, real-time fluorescence quantitative PCR detection of osteoblast gene expression (Runx2, Col-I, OPN, OCN). The results showed that ODM showed the strongest osteoblast ability, followed by ODM + 10 ng/ml TNF-α + 5 J/ cm2 LED red light group. The osteoblast ability of ODM + 10 ng/ml TNF-α was decreased, but was not found in CON group. Western blot was used to detect the expression of NF-κB pathway protein and osteoblast-related proteins (Runx2, Col-I, OPN, OCN) after addition of PDTC inhibitor. The results showed that the expression of p-IκBα was increased and the expression of IκBα was decreased (p < 0.05). The expression of osteoblast protein increased after the addition of inhibitor (p < 0.05). Therefore, in an inflammatory environment constructed by 10 ng/ml TNF-α, 5 J/cm2 LED red light can upregulate the proliferation and osteogenesis of hPDLSCs by inhibiting NF-κB signaling pathway.





Similar content being viewed by others
Data availability
The data that support the findings of this study are available on request from the corresponding author Yao Wang, upon reasonable request.
References
Martignago CCS, Tim CR, Assis L et al (2020) Effects of red and near-infrared LED light therapy on full-thickness skin graft in rats. Lasers Med Sci 35(1):157–164. https://doi.org/10.1007/s10103-019-02812-6
Ren C, McGrath C, Gu M et al (2020) Low-level laser-aided orthodontic treatment of periodontally compromised patients: a randomised controlled trial. Lasers Med Sci 35(3):729–739. https://doi.org/10.1007/s10103-019-02923-0
Lee KD, Chiang MH, Chen PH et al (2019) The effect of low-level laser irradiation on hyperglycemia-induced inflammation in human gingival fibroblasts. Lasers Med Sci 34(5):913–920. https://doi.org/10.1007/s10103-018-2675-6
Zhu T, Wu Y, Zhou X, Yang Y, Wang Y (2019) Irradiation by blue light-emitting diode enhances osteogenic differentiation in gingival mesenchymal stem cells in vitro. Lasers Med Sci 34(7):1473–1481. https://doi.org/10.1007/s10103-019-02750-3
Yang Y, Zhu T, Wu Y et al (2020) Irradiation with blue light-emitting diode enhances osteogenic differentiation of stem cells from the apical papilla. Lasers Med Sci 35(9):1981–1988. https://doi.org/10.1007/s10103-020-02995-3
Liu N, Lu W, Qu X, Zhu C (2022) LLLI promotes BMSC proliferation through circRNA_0001052/miR-124-3p. Lasers Med Sci 37(2):849–856. https://doi.org/10.1007/s10103-021-03322-0
Sabino VG, Ginani F, da Silva TN et al (2020) Laser therapy increases the proliferation of preosteoblastic MC3T3-E1 cells cultured on poly(lactic acid) films. J Tissue Eng Regen Med 14(12):1792–1803. https://doi.org/10.1002/term.3134
Barolet D, Roberge CJ, Auger FA et al (2009) Regulation of skin collagen metabolism in vitro using a pulsed 660 nm LED light source: clinical correlation with a single-blinded study. J Invest Dermatol 129(12):2751–2759. https://doi.org/10.1038/jid.2009.186
Sacono NT, Costa CA, Bagnato VS et al (2008) Light-emitting diode therapy in chemotherapy-induced mucositis. Lasers Surg Med 40(9):625–633. https://doi.org/10.1002/lsm.20677
Sakamoto FH, Izikson L, Tannous Z et al (2012) Surgical scar remodelling after photodynamic therapy using aminolaevulinic acid or its methylester: a retrospective, blinded study of patients with field cancerization. Br J Dermatol 166(2):413–416. https://doi.org/10.1111/j.1365-2133.2011.10576.x
Kömerik N, Nakanishi H, MacRobert AJ et al (2003) In vivo killing of Porphyromonas gingivalis by toluidine blue-mediated photosensitization in an animal model. Antimicrob Agents Chemother 47(3):932–940. https://doi.org/10.1128/AAC.47.3.932-940.2003
Wu Y, Zhu T, Yang Y et al (2021) Irradiation with red light-emitting diode enhances proliferation and osteogenic differentiation of periodontal ligament stem cells. Lasers Med Sci 36(7):1535–1543. https://doi.org/10.1007/s10103-021-03278-1
Hamblin MR (2017) Mechanisms and applications of the anti-inflammatory effects of photobiomodulation. AIMS Biophys 4(3):337–361. https://doi.org/10.3934/biophy.2017.3.337
Feng F, Akiyama K, Liu Y et al (2010) Utility of PDL progenitors for in vivo tissue regeneration: a report of 3 cases. Oral Dis 16(1):20–28. https://doi.org/10.1111/j.1601-0825.2009.01593.x
Tan J, Zhou L, Xue P et al (2016) Tumor Necrosis Factor-α Attenuates the Osteogenic Differentiation Capacity of Periodontal Ligament Stem Cells by Activating PERK Signaling. J Periodontol 87(8):e159–e171. https://doi.org/10.1902/jop.2016.150718
Li X, Chen D, Jing X et al (2020) DKK1 and TNF-alpha influence osteogenic differentiation of adBMP9-infected-rDFCs. Oral Dis 26(2):360–369. https://doi.org/10.1111/odi.13235
Zhu W, Qiu Q, Luo H et al (2020) High Glucose Exacerbates TNF-α-Induced Proliferative Inhibition in Human Periodontal Ligament Stem Cells through Upregulation and Activation of TNF Receptor 1. Stem Cells Int 2020:4910767. https://doi.org/10.1155/2020/4910767
Zhang J, Li ZG, Si YM et al (2014) The difference on the osteogenic differentiation between periodontal ligament stem cells and bone marrow mesenchymal stem cells under inflammatory microenviroments. Differentiation 88(4–5):97–105. https://doi.org/10.1016/j.diff.2014.10.001
Zhu W, Tan Y, Qiu Q et al (2013) Comparison of the properties of human CD146+ and CD146- periodontal ligament cells in response to stimulation with tumour necrosis factor α. Arch Oral Biol 58(12):1791–1803. https://doi.org/10.1016/j.archoralbio.2013.09.012
Kong X, Liu Y, Ye R et al (2013) GSK3β is a checkpoint for TNF-α-mediated impaired osteogenic differentiation of mesenchymal stem cells in inflammatory microenvironments. Biochim Biophys Acta 1830(11):5119–5129. https://doi.org/10.1016/j.bbagen.2013.07.027
Varfolomeev E, Vucic D (2018) Intracellular regulation of TNF activity in health and disease. Cytokine 101:26–32. https://doi.org/10.1016/j.cyto.2016.08.035
Shu C, Hou L, Chen Q et al (2022) Irradiation with a red light-emitting diode enhances the proliferation of stem cells of apical papilla via the ERK5 signalling pathway. Lasers Med Sci 37(4):2259–2268. https://doi.org/10.1007/s10103-021-03492-x
Hu C, Li L (2018) Preconditioning influences mesenchymal stem cell properties in vitro and in vivo. J Cell Mol Med 22(3):1428–1442. https://doi.org/10.1111/jcmm.13492
Yan W, Cao Y, Yang H et al (2019) CB1 enhanced the osteo/dentinogenic differentiation ability of periodontal ligament stem cells via p38 MAPK and JNK in an inflammatory environment. Cell Prolif 52(6):e12691. https://doi.org/10.1111/cpr.12691
Ma Yu, Li S-H, Ding X-X et al (2018) Effects of tumor necrosis factor-α on osteogenic differentiation and Notch signaling pathway in human periodontal ligament stem cells. Hua Xi Kou Qiang Yi Xue Za Zhi 36(2):184–189. https://doi.org/10.7518/hxkq.2018.02.013
Si D, Su B, Zhang J et al (2022) Low-level laser therapy with different irradiation methods modulated the response of bone marrow mesenchymal stem cells in vitro. Lasers Med Sci 37(9):3509–3516. https://doi.org/10.1007/s10103-022-03624-x
Lesniewski A, Estrin N, Romanos GE (2022) Comparing the Use of Diode Lasers to Light-Emitting Diode Phototherapy in Oral Soft and Hard Tissue Procedures: A Literature Review. Photobiomodul Photomed Laser Surg 40(8):522–531. https://doi.org/10.1089/photob.2021.0171
Rahmati A, Abbasi R, Najafi R et al (2022) Effect of diode low level laser and red light emitting diode irradiation on cell proliferation and osteogenic/odontogenic differentiation of stem cells from the apical papilla. BMC Oral Health 22(1):543. https://doi.org/10.1186/s12903-022-02574-8
Silveira PC, Ferreira KB, da Rocha FR et al (2016) Effect of Low-Power Laser (LPL) and Light-Emitting Diode (LED) on Inflammatory Response in Burn Wound Healing. Inflammation 39(4):1395–1404. https://doi.org/10.1007/s10753-016-0371-x
Guimaraes DM, Ota TMN, Da Silva DAC et al (2021) Low-level laser or LED photobiomodulation on oral mucositis in pediatric patients under high doses of methotrexate: prospective, randomized, controlled trial. Support Care Cancer 29(11):6441–6447. https://doi.org/10.1007/s00520-021-06206-9
DE Oliveira MF, Johnson DS, Demchak T et al (2022) Low-intensity LASER and LED (photobiomodulation therapy) for pain control of the most common musculoskeletal conditions. Eur J Phys Rehabil Med 58(2):282–289. https://doi.org/10.23736/S1973-9087.21.07236-1
Rosa CB, Habib FA, de Araújo TM et al (2014) Effect of the laser and light-emitting diode (LED) phototherapy on midpalatal suture bone formation after rapid maxilla expansion: a Raman spectroscopy analysis. Lasers Med Sci 29(3):859–867. https://doi.org/10.1007/s10103-013-1284-7
Wang L, Liu C, Song Y et al (2022) The effect of low-level laser irradiation on the proliferation, osteogenesis, inflammatory reaction, and oxidative stress of human periodontal ligament stem cells under inflammatory conditions. Lasers Med Sci 37(9):3591–3599. https://doi.org/10.1007/s10103-022-03638-5
Meng T, Zhou Y, Li J et al (2018) Azithromycin Promotes the Osteogenic Differentiation of Human Periodontal Ligament Stem Cells after Stimulation with TNF-α. Stem Cells Int 2018:7961962. https://doi.org/10.1155/2018/7961962
Huang TY, Shahrousvand M, Hsu YT et al (2021) Polycaprolactone/Polyethylene Glycol Blended with Dipsacus asper Wall Extract Nanofibers Promote Osteogenic Differentiation of Periodontal Ligament Stem Cells. Polymers (Basel) 13(14):2245. https://doi.org/10.3390/polym13142245
Wang M, Li J, Ye Y et al (2020) SHED-derived conditioned exosomes enhance the osteogenic differentiation of PDLSCs via Wnt and BMP signaling in vitro. Differentiation 111:1–11. https://doi.org/10.1016/j.diff.2019.10.003
Barnabei L, Laplantine E, Mbongo W et al (2021) NF-κB: At the Borders of Autoimmunity and Inflammation. Front Immunol 12:716469. https://doi.org/10.3389/fimmu.2021.716469
Chen F, Castranova V (2007) Nuclear factor-kappaB, an unappreciated tumor suppressor. Cancer Res 67(23):11093–11098. https://doi.org/10.1158/0008-5472.CAN-07-1576
Agnihotri P, Deka H, Chakraborty D, et al. (2023) Anti-inflammatory potential of selective small compounds by targeting TNF-α & NF-kB signaling: a comprehensive molecular docking and simulation study. J Biomol Struct Dyn 1–14. https://doi.org/10.1080/07391102.2023.2196692
Zein R, Selting W, Hamblin MR (2018) Review of light parameters and photobiomodulation efficacy: dive into complexity. J Biomed Opt 23(12):1–17. https://doi.org/10.1117/1.JBO.23.12.120901
Ferino A, Rapozzi V, Xodo LE (2020) The ROS-KRAS-Nrf2 axis in the control of the redox homeostasis and the intersection with survival-apoptosis pathways: Implications for photodynamic therapy. J Photochem Photobiol B 202:111672. https://doi.org/10.1016/j.jphotobiol.2019.111672
Song S, Xiao X, Guo D et al (2017) Protective effects of Paeoniflorin against AOPP-induced oxidative injury in HUVECs by blocking the ROS-HIF-1α/VEGF pathway. Phytomedicine 34:115–126. https://doi.org/10.1016/j.phymed.2017.08.010
Hamblin MR (2018) Mechanisms and Mitochondrial Redox Signaling in Photobiomodulation. Photochem Photobiol 94(2):199–212. https://doi.org/10.1111/php.12864
Li Y, Qiao Y, Wang H et al (2021) Intraperitoneal injection of PDTC on the NF-kB signaling pathway and osteogenesis indexes of young adult rats with anterior palatal suture expansion model. PLoS One 16(7):e0243108. https://doi.org/10.1371/journal.pone.0243108
Funding
This work was supported by the Sichuan science and technology plan joint innovation special task project(2022YFS0634); Sichuan Province Medical Research Project (S21015) and University-level scientific research project of Southwest Medical University (2021ZKMS013).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in the study were in accordance with the Ethics Committee of the Affiliated Hospital of Stomatology Southwest Medical University Certificate (contract grant 20211119003) and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Consent to participate
Informed consent was obtained from legal guardians.
Consent for publication
Patients signed informed consent regarding publishing their data.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, Y., Yang, J., Jiang, B. et al. Low-energy LED red light inhibits the NF-κB pathway and promotes hPDLSCs proliferation and osteogenesis in a TNF-α environment in vitro. Lasers Med Sci 38, 240 (2023). https://doi.org/10.1007/s10103-023-03880-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10103-023-03880-5