Abstract
Objective
To develop and validate a radiomic prediction model using initial noncontrast computed tomography (CT) at admission to predict in-hospital mortality in patients with traumatic brain injury (TBI).
Methods
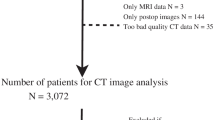
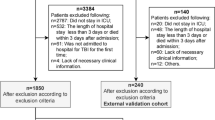
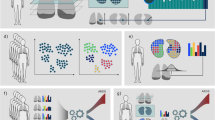
A total of 379 TBI patients from three cohorts were categorized into training, internal validation, and external validation sets. After filtering the unstable features with the minimum redundancy maximum relevance approach, the CT-based radiomics signature was selected by using the least absolute shrinkage and selection operator (LASSO) approach. A personalized predictive nomogram incorporating the radiomic signature and clinical features was developed using a multivariate logistic model to predict in-hospital mortality in patients with TBI. The calibration, discrimination, and clinical usefulness of the radiomics signature and nomogram were evaluated.
Results
The radiomic signature consisting of 12 features had areas under the curve (AUCs) of 0.734, 0.716, and 0.706 in the prediction of in-hospital mortality in the internal and two external validation cohorts. The personalized predictive nomogram integrating the radiomic and clinical features demonstrated significant calibration and discrimination with AUCs of 0.843, 0.811, and 0.834 in the internal and two external validation cohorts. Based on decision curve analysis (DCA), both the radiomic features and nomogram were found to be clinically significant and useful.
Conclusion
This predictive nomogram incorporating the CT-based radiomic signature and clinical features had maximum accuracy and played an optimized role in the early prediction of in-hospital mortality. The results of this study provide vital insights for the early warning of death in TBI patients.






Similar content being viewed by others
References
GBD 2015 Disease and Injury Incidence and Prevalence Collaborators (2016) Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet 388(10053):1545–1602
Khellaf A, Khan DZ, Helmy A (2019) Recent advances in traumatic brain injury. J Neurol 266(11):2878–2889
Cheng P et al (2017) Trends in traumatic brain injury mortality in China, 2006–2013: a population-based longitudinal study. PLoS Med 14(7):e1002332
Jiang JY et al (2019) Traumatic brain injury in China. Lancet Neurol 18(3):286–295
Dijkland SA et al (2020) Prognosis in moderate and severe traumatic brain injury: a systematic review of contemporary models and validation studies. J Neurotrauma 37(1):1–13
Retel HI et al (2020) Prognostic research in traumatic brain injury: markers, modeling, and methodological principles. J Neurotrauma 38:2502–2513
Perel P et al (2008) Predicting outcome after traumatic brain injury: practical prognostic models based on large cohort of international patients. BMJ 336(7641):425–429
Steyerberg EW et al (2008) Predicting outcome after traumatic brain injury: development and international validation of prognostic scores based on admission characteristics. PLoS Med 5(8):e165 (discussion e165)
Carney N et al (2017) Guidelines for the management of severe traumatic brain injury, fourth edition. Neurosurgery 80(1):6–15
Katsnelson M et al (2012) Are initial radiographic and clinical scales associated with subsequent intracranial pressure and brain oxygen levels after severe traumatic brain injury? Neurosurgery 70(5):1095–105 (discussion 1105)
Nelson DW et al (2010) Extended analysis of early computed tomography scans of traumatic brain injured patients and relations to outcome. J Neurotrauma 27(1):51–64
Huang YH et al (2012) Rotterdam computed tomography score as a prognosticator in head-injured patients undergoing decompressive craniectomy. Neurosurgery 71(1):80–85
Raj R et al (2014) Predicting outcome in traumatic brain injury: development of a novel computerized tomography classification system (Helsinki computerized tomography score). Neurosurgery 75(6):632–46 (discussion 646-7)
Chesnut RM et al (2018) A method of managing severe traumatic brain injury in the absence of intracranial pressure monitoring: the imaging and clinical examination protocol. J Neurotrauma 35(1):54–63
Gillies RJ, Kinahan PE, Hricak H (2016) Radiomics: images are more than pictures, they are data. Radiology 278(2):563–577
Zhang B et al (2017) Radiomics features of multiparametric MRI as novel prognostic factors in advanced nasopharyngeal carcinoma. Clin Cancer Res 23(15):4259–4269
Sauerbrei W, Boulesteix AL, Binder H (2011) Stability investigations of multivariable regression models derived from low- and high-dimensional data. J Biopharm Stat 21(6):1206–1231
Robin X et al (2011) pROC: an open-source package for R and S+ to analyze and compare ROC curves. BMC Bioinformatics 12:77
Mercier F et al (2019) From waterfall plots to spaghetti plots in early oncology clinical development. Pharm Stat 18(5):526–532
Kalpakis K et al (2015) Permutation entropy analysis of vital signs data for outcome prediction of patients with severe traumatic brain injury. Comput Biol Med 56:167–174
Guiza F et al (2013) Novel methods to predict increased intracranial pressure during intensive care and long-term neurologic outcome after traumatic brain injury: development and validation in a multicenter dataset. Crit Care Med 41(2):554–564
Li Z et al (2018) Admission circulating monocytes level is an independent predictor of outcome in traumatic brain injury. Brain Inj 32(4):515–522
Lu HY et al (2015) Predicting long-term outcome after traumatic brain injury using repeated measurements of Glasgow Coma Scale and data mining methods. J Med Syst 39(2):14
Cole JH, Leech R, Sharp DJ (2015) Prediction of brain age suggests accelerated atrophy after traumatic brain injury. Ann Neurol 77(4):571–581
Majdan M et al (2015) Glasgow coma scale motor score and pupillary reaction to predict six-month mortality in patients with traumatic brain injury: comparison of field and admission assessment. J Neurotrauma 32(2):101–108
Brown AW et al (2019) Predictive utility of an adapted Marshall head CT classification scheme after traumatic brain injury. Brain Inj 33(5):610–617
Nourallah B, Menon DK, Zeiler FA (2018) Midline shift is unrelated to subjective pupillary reactivity assessment on admission in moderate and severe traumatic brain injury. Neurocrit Care 29(2):203–213
Dolmans R et al (2020) Routine blood tests for severe traumatic brain injury: can they predict outcomes? World Neurosurg 136:e60–e67
Yuan Q et al (2018) Prognostic value of coagulation tests for in-hospital mortality in patients with traumatic brain injury. Scand J Trauma Resusc Emerg Med 26(1):3
Rubin ML et al (2019) Prognosis of six-month Glasgow Outcome Scale in severe traumatic brain Injury using hospital admission characteristics, injury severity characteristics, and physiological monitoring during the first day post-injury. J Neurotrauma 36(16):2417–2422
Rosa MJ et al (2016) Contusion contrast extravasation depicted on multidetector computed tomography angiography predicts growth and mortality in traumatic brain contusion. J Neurotrauma 33(11):1015–1022
Orito K et al (2018) Predictive value of leakage signs for pure brain contusional hematoma expansion. J Neurotrauma 35(5):760–766
Yue JK et al (2019) Association between plasma GFAP concentrations and MRI abnormalities in patients with CT-negative traumatic brain injury in the TRACK-TBI cohort: a prospective multicentre study. Lancet Neurol 18(10):953–961
Taylor M et al (2020) A systematic review of risk prediction models for perioperative mortality after thoracic surgery. Interact Cardiovasc Thorac Surg 32:333–342
Shi HY et al (2013) In-hospital mortality after traumatic brain injury surgery: a nationwide population-based comparison of mortality predictors used in artificial neural network and logistic regression models. J Neurosurg 118(4):746–752
van der Ploeg T, Nieboer D, Steyerberg EW (2016) Modern modeling techniques had limited external validity in predicting mortality from traumatic brain injury. J Clin Epidemiol 78:83–89
Lambin P et al (2017) Radiomics: the bridge between medical imaging and personalized medicine. Nat Rev Clin Oncol 14(12):749–762
Mayerhoefer ME et al (2020) Introduction to radiomics. J Nucl Med 61(4):488–495
Kniep HC et al (2019) Radiomics of brain MRI: utility in prediction of metastatic tumor type. Radiology 290(2):479–487
Qiu W et al (2019) Radiomics-based intracranial thrombus features on CT and CTA predict recanalization with intravenous alteplase in patients with acute ischemic stroke. AJNR Am J Neuroradiol 40(1):39–44
Nawabi J et al (2020) Neoplastic and non-neoplastic acute intracerebral hemorrhage in CT brain scans: machine learning-based prediction using radiomic image features. Front Neurol 11:285
Zhang J et al (2020) Differentiating the pathological subtypes of primary lung cancer for patients with brain metastases based on radiomics features from brain CT images. Eur Radiol 31:1022–1028
Funding
We gratefully acknowledge the following funding source: the National Natural Science Foundation of China (81772111 and 81871458), the China Postdoctoral Science Foundation (No. 2017M611585), the Biomedical and Engineering Cross Youth Fund of Shanghai Jiao Tong University (No. YG2021QN43), and the Shanghai Science Committee (No.19411968200).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethical approval
In this study, all patients enrolled in this study have signed the broad consent, which permits the researchers to engage in research use of identifiable biospecimens and identifiable data during the pre-operative period and future follow-up without the requirement to obtain additional consent for future storage, maintenance, or research uses, so long as the future activities are within the scope of the broad consent. The study protocol and the application form were fully reviewed, and we have certified that this study did not raise any issues of patient risk or cause any harm to patient. We have also certified that the study was strictly in accordance with the Declaration of Helsinki and International Ethical Guidelines for Health-related Research Involving Humans.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zheng, Rz., Zhao, Zj., Yang, Xt. et al. Initial CT-based radiomics nomogram for predicting in-hospital mortality in patients with traumatic brain injury: a multicenter development and validation study. Neurol Sci 43, 4363–4372 (2022). https://doi.org/10.1007/s10072-022-05954-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-022-05954-8