Abstract
Introduction
Hereditary hemorrhagic telangiectasia (HHT) is a rare genetic disease with prevalence of approximately 1 in 5000–10,000. We evaluated the prevalence and association of cerebrovascular and cardiovascular comorbidities in HHT patients using national database.
Methods
Retrospective observational study was performed using National Inpatient Sampling (NIS) database for the year 2014. HHT patients and comorbidities were identified using ICD-9 codes. Univariate and multivariate analyses were performed using SAS.
Results
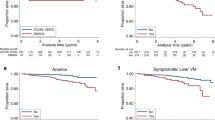
Prevalence of HHT was 0.0119% with predominance in White population. Mean age of HHT patients was 59 years. Increased proportion of HHT patients had hypertension (46.8% vs 42%), anemia (28.9% vs 15.1%), chronic pulmonary disease (24.8% vs 16.4%), congestive heart failure (15.7% vs 7.5%), liver disease (7.9% vs 2.8%), migraine (4.5% vs 1.5%), and cerebrovascular malformations (0.8% vs 0.03%), whereas chronic kidney disease (12.7% vs 12.2%), headaches (1.3% vs 1.1%), seizures (0.7% vs 0.9%), transient ischemic attacks (1.06% vs 1.03%), ischemic (1.2% vs 1.0%), and hemorrhagic (0.5% vs 0.3%) strokes were similar to those without HHT. Multivariable model shows increase in cerebrovascular malformations (OR 11.04, CI 2.49–22.26, p < 0.0001), migraine (OR 3.23, CI 2.30–4.52, p < 0.0001), chronic blood loss anemia (OR 6.83, CI 5.36–8.71, p < 0.0001), congestive heart failure (OR 1.55, CI 1.26–1.91, p < 0.0001), chronic pulmonary disease (OR 1.30, CI 1.09–1.56, p = 0.0038), and hepatic disease (OR 2.63, CI 2.01–3.45, p < 0.0001) in HHT patients as compared to non-HHT patients.
Conclusion
There is a need for a large prospective registry of HHT patients that can corroborate these associations and burden of cerebrovascular and cardiovascular diseases.

Similar content being viewed by others
References
Shovlin CL, Guttmacher AE, Buscarini E, Faughnan ME, Hyland RH, Westermann CJ, Kjeldsen AD, Plauchu H (2000) Diagnostic criteria for hereditary hemorrhagic telangiectasia (Rendu-Osler-Weber syndrome). Am J Med Genet 91(1):66–67
Iyer VN, Brinjikji W, Apala D, Pannu BS, Kotecha A, Leise MD, Kamath PS, Misra S, Lanzino G, Krowka MJ (2018) Impact of age on outcomes in hospitalized patients with hereditary hemorrhagic telangiectasia. Advances in hematology 2018
Latino GA, Brown D, Glazier RH, Weyman JT, Faughnan ME (2014) Targeting under-diagnosis in hereditary hemorrhagic telangiectasia: a model approach for rare diseases? Orphanet Journal of Rare Diseases 9(1):115
Donaldson JW, McKeever TM, Hall IP, Hubbard RB, Fogarty AW (2015) Complications and mortality in hereditary hemorrhagic telangiectasia A population-based study. Neurology 84(18):1886–1893
Grosse SD, Boulet SL, Grant AM, Hulihan MM, Faughnan ME (2014) The use of US health insurance data for surveillance of rare disorders: hereditary hemorrhagic telangiectasia. Genetics in medicine : official journal of the American College of Medical Genetics 16(1):33–39. https://doi.org/10.1038/gim.2013.66
McDonald J, Wooderchak-Donahue W, VanSant WC, Whitehead K, Stevenson DA, Bayrak-Toydemir P (2015) Hereditary hemorrhagic telangiectasia: genetics and molecular diagnostics in a new era. Front Genet 6:1
Kawasaki K, Freimuth J, Meyer DS, Lee MM, Tochimoto-Okamoto A, Benzinou M, Clermont FF, Wu G, Roy R, Letteboer TG (2014) Genetic variants of Adam17 differentially regulate TGFβ signaling to modify vascular pathology in mice and humans. Proceedings of the National Academy of Sciences:201318761
Fernández-L A, Sanz-Rodriguez F, Blanco FJ, Bernabéu C, Botella LM (2006) Hereditary hemorrhagic telangiectasia, a vascular dysplasia affecting the TGF-β signaling pathway. Clin Med Res 4(1):66–78
Leitão P, Carvalho A, Guerra C, Gonçalves J, Ramos I (2018) Congestive cirrhosis in Osler-Weber-Rendu syndrome: A rare case report. Radiology case reports 13 (1): 51–54
Ev E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP (2007) Strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ 335(7624):806–808. https://doi.org/10.1136/bmj.39335.541782.AD
Farooqui M, Qeadan F, Vigil C, Suriya S, Robinson M, Quadri S, Wegele A, Torbey M, Zafar A (2019) Congestive Heart Failure is Strongly Associated with Hereditary Hemorrhagic Telangiectasia (HHT): Analysis of a Large National Database (P5. 3-018). AAN Enterprises,
Nishida T, Faughnan ME, Krings T, Chakinala M, Gossage JR, Young WL, Kim H, Pourmohamad T, Henderson KJ, Schrum SD (2012) Brain arteriovenous malformations associated with hereditary hemorrhagic telangiectasia: gene–phenotype correlations. Am J Med Genet A 158(11):2829–2834
Fulbright RK, Chaloupka JC, Putman CM, Sze GK, Merriam MM, Lee GK, Fayad PB, Awad IA, White RI (1998) MR of hereditary hemorrhagic telangiectasia: prevalence and spectrum of cerebrovascular malformations. Am J Neuroradiol 19(3):477–484
Puente R, Bueno J, Salcedo M, Cuesta J, Marques SJHG (2016) Epidemiology of Hereditary Haemorrhagic Telangiectasia (HHT) in Spain 5(173):2–7
Kim H, Nelson J, Krings T, ter Brugge KG, McCulloch CE, Lawton MT, Young WL, Faughnan ME, Group BHI, Chakinala M (2015) Hemorrhage rates from brain arteriovenous malformation in patients with hereditary hemorrhagic telangiectasia. Stroke 46(5):1362–1364
Sopeña B, Pérez-Rodríguez MT, Portela D, Rivera A, Freire M, Martínez-Vázquez C (2013) High prevalence of pulmonary hypertension in patients with hereditary hemorrhagic telangiectasia. European Journal of Internal Medicine 24(3):e30–e34
Buscarini E, Leandro G, Conte D, Danesino C, Daina E, Manfredi G, Lupinacci G, Brambilla G, Menozzi F, De Grazia F, Gazzaniga P, Inama G, Bonardi R, Blotta P, Forner P, Olivieri C, Perna A, Grosso M, Pongiglione G, Boccardi E, Pagella F, Rossi G, Zambelli A (2011) Natural history and outcome of hepatic vascular malformations in a large cohort of patients with hereditary hemorrhagic teleangiectasia. Dig Dis Sci 56 (7): 2166–2178. https://doi.org/10.1007/s10620-011-1585-2
Kasthuri RS, Montifar M, Nelson J, Kim H, Lawton MT, Faughnan ME (2017) Prevalence and predictors of anemia in hereditary hemorrhagic telangiectasia. 92 (10):E591-E593. doi:10.1002/ajh.24832
Garcia-Tsao G, Korzenik JR, Young L, Henderson KJ, Jain D, Byrd B, Pollak JS, White RI Jr (2000) Liver disease in patients with hereditary hemorrhagic telangiectasia. N Engl J Med 343(13):931–936. https://doi.org/10.1056/nejm200009283431305
Morine KJ, Qiao X, Paruchuri V, Aronovitz MJ, Mackey EE, Buiten L, Levine J, Ughreja K, Nepali P, Blanton RM, Karas RH, Oh SP, Kapur NK (2017) Conditional knockout of activin like kinase-1 (ALK-1) leads to heart failure without maladaptive remodeling. Heart Vessel 32(5):628–636. https://doi.org/10.1007/s00380-017-0955-x
Cho D, Kim S, Kim M, Seo YH, Kim W, Kang SH, Park S-M, Shim W (2012) Two cases of high output heart failure caused by hereditary hemorrhagic telangiectasia. Korean circulation journal 42(12):861–865
Sabba C, Pasculli G, Suppressa P, D'ovidio F, Lenato GM, Resta F, Assennato G, Guanti G (2006) Life expectancy in patients with hereditary haemorrhagic telangiectasia. Journal of the Association of Physicians 99 (5): 327–334
Post MC, Letteboer TG, Mager JJ, Plokker TH, Kelder JC, Westermann CJ (2005) A pulmonary right-to-left shunt in patients with hereditary hemorrhagic telangiectasia is associated with an increased prevalence of migraine. Chest 128(4):2485–2489
Tillet E, Bailly S (2015) Emerging roles of BMP9 and BMP10 in hereditary hemorrhagic telangiectasia. Front Genet 5:456
Upton PD, Morrell NW (2009) TGF-β and BMPR-II pharmacology—implications for pulmonary vascular diseases. Curr Opin Pharmacol 9(3):274–280
Acknowledgements
The authors would like to thank the Clinical and Translational Science Center (CTSC) at the University of New Mexico for their support and statistical services.
Availability of data and material
All the data will be made available from the corresponding author upon reasonable request.
Author information
Authors and Affiliations
Contributions
CV, AW, and MR contributed in the literature search and initial preparation of the manuscript. FQ contributed in the statistical expertise and editing of the manuscript. MF, SS, AI, and AZ contributed in the concept, design, manuscript drafting, and editing. SAQ, JRL, SOG, and MT contributed in the critical review of the manuscript.
Corresponding author
Ethics declarations
Ethics statement
This secondary analysis of publicly available de-identified data was approved by the Ethics committee of the University of New Mexico
Informed consent
Not applicable.
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Farooqui, M., Suriya, S., Qeadan, F. et al. Cerebrovascular and cardiovascular disease burden in patients with hereditary hemorrhagic telangiectasia. Neurol Sci 42, 5117–5122 (2021). https://doi.org/10.1007/s10072-021-05135-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-021-05135-z