Abstract
Objectives
To reveal the differences by comparing the magnetic resonance imaging (MRI) findings of patients with clinically symptomatic sacroiliitis with those undergoing sacroiliac imaging for other reasons using the Canadian Spondyloarthritis Research Consortium-Sacroiliac Inflammatory Scoring System (SPARCC-SIS).
Methods
In this retrospective single-center study, sacroiliac MRIs performed between 2017 and 2023 were evaluated from the database. The SPARCC-SIS scoring system is used to evaluate and grade the inflammation of the sacroiliac joints. Mild inflammation is indicated by a score below 24, moderate by a score of 24–48, and severe by a score above 49. Additionally, structural defects of the sacroiliac joint, such as erosion, sclerosis, and ankylosis, were observed. After MRI evaluation, clinically symptomatic (group 1) and non-symptomatic (group 2) patients were divided into two groups. The clinical and laboratory findings of the patients and MRI findings were compared. The patient’s age, gender, clinical information from hospital records, acute phase reactants (APRs), and the presence of the Human Leukocyte Antigen (HLA-B27) gene (if applicable) were thoroughly recorded.
Results
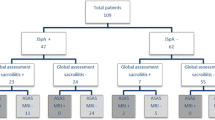
One hundred thirty-six children who performed sacroiliac MRI for any indication were included in the study. The APRs positivity, presence of HLA-B27, and SPARCC scoring system were significantly higher in 24 patients with clinical sacroiliitis (group 1) than in 112 patients without sacroiliitis (group 2). In our study, the most common MRI findings in children were bone marrow edema, capsulitis, synovitis, and erosion, while chronic structural changes such as sclerosis and ankylosing were rare.
Conclusion
In this study, the SPARCC scoring method, which shows the severity of sacroiliac joint inflammation, correlates with the clinical diagnosis of sacroiliitis. In cases with suspected sacroiliitis, except for extraordinary reasons, it can be evaluated with MRI without contrast material and can be graded to guide the clinician in treatment and approach.
Key points |
• Since the SPARCC scoring method, which shows the severity of sacroiliac joint inflammation, will guide the clinician, its use in the pediatric population will be beneficial and feasible. • Non-contrast scans are often sufficient to assess inflammation in the sacroiliac joint. In the evaluation of sacroiliac MRI in children, evaluation can be made without contrast. • Since chronic changes in the sacroiliac joint are very rare in children, evaluation with radiography or CT may not be needed. |




Similar content being viewed by others
References
Pagnini I, Savelli S, Matucci-Cerinic M, Fonda C, Cimaz R, Simonini G (2010) Early predictors of juvenile sacroiliitis in enthesitis-related arthritis. J Rheumatol 37:2395–401. https://doi.org/10.3899/jrheum.100090
Stoll ML, Bhore R, Dempsey-Robertson M, Punaro M (2010) Spondyloarthritis in a pediatric population: risk factors for sacroiliitis. J Rheumatol 37:2402–8. https://doi.org/10.3899/jrheum.100014
Bollow M, Biedermann T, Kannenberg J et al (1998) Use of dynamic magnetic resonance imaging to detect sacroiliitis in HLA-B27 positive and negative children with juvenile arthritides. J Rheumatol 25:556–564
Puhakka KB, Jurik AG, Egund N et al (2003) Imaging of sacroiliitis in early seronegative spondyloarthropathy. Assessment of abnormalities by MR in comparison with radiography and CT. Acta Radiol 44:218–29. https://doi.org/10.1080/j.1600-0455.2003.00034.x
Herregods N, Maksymowych WP, Jans L et al (2021) Atlas of MRI findings of sacroiliitis in pediatric sacroiliac joints to accompany the updated preliminary OMERACT pediatric JAMRIS (Juvenile Idiopathic Arthritis MRI Score) scoring system: part I: active lesions. Semin Arthritis Rheum 51:1089–1098. https://doi.org/10.1016/j.semarthrit.2021.07.003
Tasar S, Ciraci S, Yilmaz PD, Oysu AS, Bukte Y, Sozeri B (2023) Efficacy of diffusion-weighted imaging in sacroiliac joint MRI in children. North Clin Istanb 10:131–8. https://doi.org/10.14744/nci.2023.90907
Lovell DJ, Brunner HI (2021) Evolution in the understanding of pediatric-onset axial spondyloarthritis. Arthritis Care Res (Hoboken) 73:921–3. https://doi.org/10.1002/acr.24536
Vittecoq O, Said LA, Michot C et al (2000) Evolution of chronic recurrent multifocal osteitis toward spondyloarthropathy over the long term. Arthritis Rheum 43:109–19. https://doi.org/10.1002/1529-0131(200001)43:1%3c109::AID-ANR14%3e3.0.CO;2-3
Smith JA, Burgos-Vargas R (2021) Outcomes in juvenile-onset spondyloarthritis. Front Med (Lausanne) 8:680916. https://doi.org/10.3389/fmed.2021.680916
Maksymowych WP, Inman RD, Salonen D et al (2005) Spondyloarthritis Research Consortium of Canada magnetic resonance imaging index for assessment of sacroiliac joint inflammation in ankylosing spondylitis. Arthritis Rheum 53:703–9. https://doi.org/10.1002/art.21445
MacKay JW, Aboelmagd S, Gaffney JK (2015) Correlation between clinical and MRI disease activity scores in axial spondyloarthritis. Clin Rheumatol 34:1633–8. https://doi.org/10.1007/s10067-015-2936-8
Avar-Aydin PO, Ozcakar ZB, Kaynak Sahap S, Aydin F, Cakar N et al (2023) Childhood-onset sacroiliitis: causes and correlation between clinical findings and magnetic resonance imaging. J Clin Rheumatol 29(5):e71–e77. https://doi.org/10.1097/RHU.0000000000001955
Panwar J, Tse SML, Lim L, Tolend MA, Radhakrishnan S, Salman M et al (2019) Spondyloarthritis Research Consortium of Canada scoring system for sacroiliitis in juvenile spondyloarthritis/enthesitis-related arthritis: a reliability, validity, and responsiveness study. J Rheumatol 46(6):36–44. https://doi.org/10.3899/jrheum.180222
Weiss PF, Maksymowych WP, Lambert RG et al (2018) Feasibility and reliability of the Spondyloarthritis Research Consortium of Canada sacroiliac joint inflammation score in children. Arthritis Res Ther 20:56. https://doi.org/10.1186/s13075-018-1543-x
Petty RE, Southwood TR, Manners P et al (2004) International League of Associations for Rheumatology. International League of Associations for Rheumatology classification of juvenile idiopathic arthritis: second revision, Edmonton, 2021. J Rheumatol 31:390–392
Roderick MR, Ramanan AV (2013) Chronic recurrent multifocal osteomyelitis. Adv Exp Med Biol 764:99–107. https://doi.org/10.1007/978-1-4614-4726-9_7
Brewerton DA, Hart FD, Nicholls A, Caffrey M, James DC et al (1973) Ankylosing spondylitis and HL-A 27. Lancet 1:904–7. https://doi.org/10.1016/s0140-6736(73)91360-3
Brown MA, Kenna T, Wordsworth BP (2016) Genetics of ankylosing spondylitis–insights into pathogenesis. Nat Rev Rheumatol 12:81–91. https://doi.org/10.1038/nrrheum.2015.133
Kavadichanda CG, Seth G, Kumar G, Gulati R, Negi VS (2019) Clinical correlates of HLA-B*27 and its subtypes in enthesitis-related arthritis variant of juvenile idiopathic arthritis in south Indian Tamil patients. Int J Rheum Dis 22:1289–96. https://doi.org/10.1111/1756-185X.13551
Goirand M, Breton S, Chevallier F et al (2018) Clinical features of children with enthesitis-related juvenile idiopathic arthritis/juvenile spondyloarthritis followed in a French tertiary care pediatric rheumatology center. Pediatr Rheumatol Online J 16:21. https://doi.org/10.1186/s12969-018-0238-9
Poddubnyy D, Rudwaleit M, Haibel H, Listing J, Märker-Hermann E et al (2011) Rates and predictors of radiographic sacroiliitis progression over 2 years in patients with axial spondyloarthritis. Ann Rheum Dis 70:1369–74. https://doi.org/10.1136/ard.2010.145995
Gezmis E, Donmez FY, Agildere M (2013) Diagnosis of early sacroiliitis in seronegative spondyloarthropathies by DWI and correlation of clinical and laboratory findings with ADC values. Eur J Radiol 82:2316–21. https://doi.org/10.1016/j.ejrad.2013.08.032
Puhakka KB, Jurik AG, Schiottz-Christensen B, Hansen GV, Egund N et al (2004) Magnetic resonance imaging of sacroiliitis in early seronegative spondyloarthropathy. Abnormalities correlated to clinical and laboratory findings. Rheumatol (Oxford) 43:234–7. https://doi.org/10.1093/rheumatology/keh008
Clara Lin, MacKenzie John D, Courtier Jesse L, Gu Jeffrey T, Diana M (2014) Magnetic resonance imaging findings in juvenile spondyloarthropathy and effects of treatment observed on subsequent imaging. Pediatr Rheumatol 12:25. https://doi.org/10.1186/1546-0096-12-25
Aquino MR, Tse SM, Gupta S, Rachlis AC, Stimec J (2015) Whole-body MRI of juvenile spondyloarthritis: protocols and pictorial review of characteristic patterns. Pediatr Radiol 45:754–62. https://doi.org/10.1007/s00247-015-3319-7
Weber U, Maksymowych WP, Jurik AG et al (2009) Validation of whole-body against conventional magnetic resonance imaging for scoring acute inflammatory lesions in the sacroiliac joints of patients with spondylarthritis. Arthritis Rheum 61:893–9. https://doi.org/10.1002/art.24542
Chary-Valckenaere I, d’Agostino MA, Loeuille D (2011) Role for imaging studies in ankylosing spondylitis. Joint Bone Spine 78:138–43. https://doi.org/10.1016/j.jbspin.2010.07.008
Van den Berg R, van der Heijde DM (2010) How should we diagnose spondyloarthritis according to the ASAS classification criteria: a guide for practicing physicians. Pol Arch Med Wewn 120:452–457 (PMID: 21102381)
Maksymowych WP, Wichuk S, Chiowchanwisawakit P et al (2015) Development and preliminary validation of the spondyloarthritis research consortium of Canada magnetic resonance imaging sacroiliac joint structural score. J Rheumatol 42:79–86. https://doi.org/10.3899/jrheum.140519
Heuft-Dorenbosch L, Weijers R, Landewé R, van der Linden S, van der Heijde D (2006) Magnetic resonance imaging changes of sacroiliac joints in patients with recent-onset inflammatory back pain: inter-reader reliability and prevalence of abnormalities. Arthritis Res Ther 8:R11. https://doi.org/10.1186/ar1859
de Hooge M, van den Berg R, Navarro-Compán V et al (2013) Magnetic resonance imaging of the sacroiliac joints in the early detection of spondyloarthritis: no added value of gadolinium compared with short tau inversion recovery sequence. Rheumatol (Oxford) 52:1220–4. https://doi.org/10.1093/rheumatology/ket012
Weiss PF, Xiao R, Biko DM, Johnson AM, Chauvin NA (2015) Detection of inflammatory sacroiliitis in children with magnetic resonance imaging: is gadolinium contrast enhancement necessary? Arthritis Rheumatol 67:2250–6. https://doi.org/10.1002/art.39159
Jaremko JL, Liu L, Winn NJ, Ellsworth JE, Lambert RGW (2014) Diagnostic utility of magnetic resonance imaging and radiography in juvenile spondyloarthritis: evaluation of the sacroiliac joints in controls and affected subjects. J Rheumatol 41:963–70. https://doi.org/10.3899/jrheum.131064
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bozbeyoğlu, S.G., Öztürk, K. Effective diagnosis of sacroiliitis in children: evaluating magnetic resonance imaging with the Canadian scoring system. Clin Rheumatol 43, 2125–2131 (2024). https://doi.org/10.1007/s10067-024-06979-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-024-06979-4