Summary
Background
To primarily measure the visual acuity (VA) outcomes and, secondarily, the baseline characteristics and complication rate of YAG anterior capsulotomy (AC, YAGAC) compared to surgical anterior capsulectomy in patients with anterior capsular contraction syndrome.
Material and methods
Retrospective consecutive case series attending the Birmingham and Midlands Eye Centre.
Results
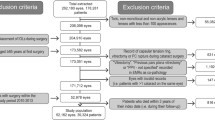
A total of 141 eyes were included (YAGAC: 108 and surgical AC: 33). The surgical AC group had a higher proportion of uveitis than the YAGAC group (eight [24.2%] and two [1.9%] respectively, p < 0.001). In the YAGAC group seven eyes (6.5%) required further laser and one eye (0.9%) needed surgical AC. No patients from the surgical group required further treatment. Median logMAR pre-operative VA was worse in the surgical AC: 0.45 (IQR 0.00–1.19) than in the YAGAC group: 0.12 (interquartile range [IQR] 0.00–0.38, p < 0.001). Both groups had no difference in final VA as the surgical group had a greater VA gain (p = 0.004).
Although the cystoid macular oedema rate was higher in the surgical group (three [9.1%]) than the YAGAC group (one [0.9%], p = 0.040), there was no significant difference in number of complications between the two groups (p = 0.074). No instances of intraocular lens subluxation were recorded in the YAGAC group, while two cases (6.1%) occurred in the surgical group (p = 0.053).
Conclusion
YAGAC and surgical AC lead to good visual outcomes with no differences in final VA between the two groups. The authors also showed low complication rates in both groups. This study will help surgeons in appropriately consenting patients presenting with ACCS when discussing both the YAG and the surgical AC treatment option.
Zusammenfassung
Hintergrund
Die erreichte Sehschärfe, die Ausgangscharakteristika vor und die Komplikationsraten nach Behandlung eines anterioren Kapselkontraktionssyndrom (ACCS) mittels anteriorer YAG-Kapsulotomie (YAGAC [YAG: Yttrium-Aluminium-Granat]) bzw. operativer anteriorer Kapsulektomie (OP) sollten verglichen werden.
Material und Methoden
Es handelt sich um eine retrospektive konsekutive Fallserie am „Birmingham and Midlands Eye Centre“.
Ergebnisse
Insgesamt wurden 141 Augen eingeschlossen (YAGAC: 108, OP: 33). In der Gruppe mit operativer Versorgung war die Uveitisrate höher als in der YAGAC-Gruppe (8 [24,2 %] bzw. 2 [1,9 %], p < 0,001). Nach YAGAC war bei 7 Augen (6,5 %) eine weitere Laserbehandlung und bei 1 Auge (0,9 %) eine operative anteriore Kapsulektomie erforderlich, während kein Patient der OP-Gruppe eine weitere Behandlung benötigte. Der mittlere präoperative logtex MAR (Logarithmus des minimalen Auflösungswinkels) der Sehschärfe der OP-Gruppe war schlechter (0,45, IQR [Interquartilenabstand]: 0,00–1,19) als der der YAGAC-Gruppe (0,12, IQR: 0,00–0,38, p < 0,001). Bei der letztlich erreichten Sehschärfe bestand kein Unterschied zwischen beiden Gruppen, wobei der Zugewinn an Sehschärfe nach OP höher war (p = 0,004).
Obwohl zystoide Makulaödeme nach OP häufiger auftraten (3 [9,1 %] vs.1 [0,9 %], p = 0,040), war die Komplikationsrate zwischen beiden Gruppen nicht signifikant verschieden (p = 0,074). In der YAGAC-Gruppe wurden keine, in der OP-Gruppe 2 Fälle einer Intraokularlinsensubluxation verzeichnet (6,1 %, p = 0,053).
Schlussfolgerung
Das visuelle Outcome ist sowohl nach OP als auch nach YAGAC gut, bei niedrigen Komplikationsraten in und ohne Unterschiede in der endgültig erreichten Sehschärfe zwischen beiden Gruppen. Diese Studie wird Chirurgen helfen, die Einwilligung eines adäquat bezüglich einer Laser- vs. operativen Behandlung aufgeklärten ACCS-Patienten zu erhalten.

Similar content being viewed by others
References
Davison JA. Capsule contraction syndrome. J Cataract Refract Surg. 1993;19:582–9.
Elmohamady MN, Elhabbak A, Gad EA. Circular YAG laser anterior capsulotomy for anterior capsule contraction syndrome. Int Ophthalmol. 2019;39(11):2497–503.
Kurosaka D, et al. Fibrous membrane formation at the capsular margin in capsule contraction syndrome. J Cataract Refract Surg. 1999;25(7):930–5.
Singh VK, Rai G, Agarwal SS. Role of cytokines in experimental and clinical uveitis. Indian J Ophthalmol. 2001;49(2):81–90.
Miyake K. The significance of inflammatory reactions following cataract extraction and intraocular lens implantation. J Cataract Refract Surg. 1996;22:759–63.
Nishi O, Nishi K. Preventive effect of a second-generation silicone intraocular lens on posterior capsule opacification. J Cataract Refract Surg. 2002;28(7):1236–40.
Toldos JJM, Roig AA, Benabent EC. Total anterior capsule closure after silicone intraocular lens implantation. J Cataract Refract Surg. 1996;22:269–71.
Reeves PD, Yung C‑W. Silicone intraocular lens encapsulation by shrinkage of the capsulorhexis opening. J Cataract Refract Surg. 1998;24:1275–6.
Gallagher SP, Pavilack MA. Risk factors for anterior capsule contraction syndrome with polypropylene or polymethylmethacrylate haptics. J Cataract Refract Surg. 1999;25:1356–61.
Lüke C, et al. Massive anterior capsule shrinkage after plate-haptic silicone lens implantation in uveitis. J Cataract Refract Surg. 2001;27(2):333–6.
Hayashi H, Hayashi K, Nakao F, Hayashi F. Area reduction in the anterior capsule opening in eyes of diabetes mellitus patients. J Cataract Refract Surg. 1998;24:1105–10.
Hayashi K, Hayashi H, Matsuo K, et al. Anterior capsule contraction and intraocular lens dislocation after implant surgery in eyes with retinitis pigmentosa. Ophthalmology. 1998;105:1239–43.
Hayashi K, Hayashi H. Effect of anterior capsule contraction on visual function after cataract surgery. J Cataract Refract Surg. 2007;33(11):1936–40.
Ye H, Zhang J, Qian Y. Long-term follow-up of neodymium:YAG laser anterior capsulotomy for the treatment of anterior capsular phimosis. J Int Med Res. 2018;46(9):3692–7.
Reyntjens B, Tassignon MJ, Van Marck E. Capsular peeling in anterior capsule contraction syndrome: surgical approach and histopathological aspects. J Cataract Refract Surg. 2004;30(4):908–12.
Koizumi K, Watanabe A, Koizumi N, Kinoshita S. Peeling the fibrous membrane from the anterior capsule for capsulorhexis contraction after phacoemulsification in aphakic patients. J Cataract Refract Surg. 2002;28:1728–32.
Day AC, Donachie PHJ, Sparrow JM, Johnston RL (2015) The Royal College of Ophthalmologists’ National Ophthalmology Database study of cataract surgery: report 1 visual outcomes and complications. Eye 29(4):552–560. https://doi.org/10.1038/eye.2015.3.
Moussa G, Bassilious K, Mathews N. A novel excel sheet conversion tool from Snellen fraction to LogMAR including ‘counting fingers’, ‘hand movement’, ‘light perception’ and ‘no light perception’ and focused review of literature of low visual acuity reference values. Acta Ophthalmologica [Internet]. 2020;aos.14659. Available from: https://onlinelibrary.wiley.com/doi/10.1111/aos.14659.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
G. Moussa, K. Katsikatsos, S.W. Ch’ng, D. Kalogeropoulos, J. Panthagani, K.S. Lett, S. Sreekantam, I. Masood, V.C. T. Sung and W. Andreatta declare that they have no conflict of interest in the production of this manuscript. There are no external funders that have played a role in study design, data collection and analysis, decision to publish or preparation of the manuscript.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Author roles: All authors have made substantial contributions to the following: (1) the conception and design of the study, or acquisition of data, or analysis and interpretation of data, (2) drafting the article or revising it critically for important intellectual content, (3) final approval of the version to be submitted.
Rights and permissions
About this article
Cite this article
Moussa, G., Katsikatsos, K., Ch’ng, S.W. et al. Outcomes of YAG anterior capsulotomy and surgical capsulectomy in the management of anterior capsular contraction syndrome. Spektrum Augenheilkd. 36, 117–122 (2022). https://doi.org/10.1007/s00717-021-00502-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00717-021-00502-9