Abstract
Background
Middle cerebral artery (MCA) M1 bifurcation aneurysms are common because of hemodynamic. For regular-shaped and small aneurysms, direct clipping is optimal. Aneurysmoraphy or bypass blood flow reconstruction are most commonly used in large aneurysm clipping. Based on preoperative vessel wall high-resolution magnetic resonance imaging (VW-HRMRI) and intraoperative angiography, an appropriate surgery strategy could be decided.
Method
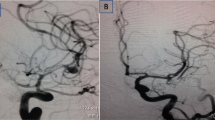
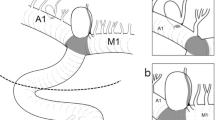
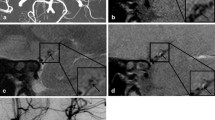
We report a case of large MCA M1 bifurcation aneurysm aneurysmoraphy according to preoperative VW-HRMRI. Intraoperative digital subtraction angiography (DSA) showed an aneurysm neck remnant, and we adjusted clips according to intraoperative DSA. This patient recovered well with a modified Rankin scale of 0 at discharge.
Conclusion
This case demonstrates that preoperative VWHRMRI could supply more aneurysm characteristics for direct aneurysmoraphy. Intraoperative DSA effectively reduces the possibility of aneurysm remnant.




Similar content being viewed by others
Data availability
Not applicable.
References
Catapano JS, Frisoli FA, Cadigan MS, Farhadi DS, Nguyen CL, Lawton MT (2020) Double-barrel superficial temporal artery-M2 middle cerebral artery bypass and creation of a middle communicating artery via M2-M2 end-to-end reimplantation for trapping of a dolichoectatic middle cerebral artery aneurysm: 2-dimensional operative video. Oper Neurosurg (Hagerstown) 19:E521–E522. https://doi.org/10.1093/ons/opaa159
Frisoli FA, Catapano JS, Baranoski JF, Lawton MT (2020) The middle communicating artery: a novel fourth-generation bypass for revascularizing trapped middle cerebral artery bifurcation aneurysms in 2 cases. J Neurosurg 134:1879–1886. https://doi.org/10.3171/2020.4.JNS193412
Labib MA, Gandhi S, Cavallo C, Nisson PL, Mooney MA, Catapano JS, Lang MJ, Chen T, Lawton MT (2020) Anterior cerebral artery bypass for complex aneurysms: advances in intracranial-intracranial bypass techniques. World Neurosurg 141:e42–e54. https://doi.org/10.1016/j.wneu.2020.04.124
Liu P, Shi Y, An Q, Zhu W (2022) Left middle cerebral artery M1-2 segment dissecting aneurysm resection and reanastomosis under double-barrel STA-MCA bypass protection. Acta Neurochir (Wien) 164:3209–3213. https://doi.org/10.1007/s00701-022-05386-5
Liu P, Shi Y, Li P, Zhu W (2023) Reconstruction of both M2 blood flow with a “Y” fashion anastomosis after excision of a large M1 bifurcation aneurysm: advantages and challenges. Acta Neurochir (Wien) 165:483–488. https://doi.org/10.1007/s00701-022-05484-4
Liu P, Shi Y, Li Z, Liu Y, Quan K, Liu Y, An Q, Zhu W (2023) Interposition intracranial-intracranial bypass based on anterior cerebral artery A1 donor anastomosis: technical advances, outcomes, and literature review. Oper Neurosurg (Hagerstown) 24:322–329. https://doi.org/10.1227/ons.0000000000000585
Funding
This study was supported by the Clinical Research Plan of SHDC (No. SHDC2020CR2034B to WZ) and Special Clinical Research Project in Health Industry of Shanghai Municipal Health Commission (No. 20224Y0072 to PL).
Author information
Authors and Affiliations
Contributions
Peixi Liu: participants in surgery, conception and design of study, provision of study material, collection and/or assembly of data, manuscript writing, and final approval of manuscript.
Hongfei Zhang: literature collection and collation.
Peiliang Li: participants in surgery, conception, and design of study.
Wei Zhu: conception and design of the study and revision and final approval of the manuscript.
The authors thank Zongze Li for surgery participants, Yingtao Liu for imaging processing, and Yang Xiao for intraoperative electrophysiological monitoring support.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Research involving human participants
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the Huashan Hospital Institutional Review Board (HIRB), Fudan University, Shanghai, China.
Consent to participate
The patient gave approval for this publication.
Consent for publication
All authors declare that they have no competing financial interest.
Conflict of interest
The authors declare no competing interests.
Additional information
Key points
1. Preoperative VW-HRMRI helps operators assess aneurysm neck and sac atherosclerosis.
2. A high intrasac signal in VW-HRMRI indicates the feasibility of direct clipping or aneurysmoraphy.
3. Bypass should always be prepared in large complex MCA bifurcation aneurysm.
4. STA blood volume needs to be assessed before surgery.
5. Intracranial-intracranial bypass shows more advantages than extracranial-intracranial bypass, especially in young patients.
6. SEP and MEP monitoring are quick measures to determine temporary occlusion tolerance and blood flow changes.
7. ICG provides basic assessment for branch patency, but it cannot show aneurysm remnant.
8. Endoscopy detection is an alternative method after aneurysmoraphy.
9. DSA and three-dimensional rotation construction were the gold standards for complete clipping.
10. At least one DSA long-term follow-up is required after discharge.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The first two authors, PL and HZ, contributed to this article equally.
Supplementary information
(MP4 145025 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, P., Zhang, H., Li, P. et al. Aneurysmoraphy or bypass? Surgical strategy for large M1 bifurcation aneurysm involving two branches based on vessel wall high-resolution MRI and intraoperative angiography. Acta Neurochir 165, 3717–3721 (2023). https://doi.org/10.1007/s00701-023-05846-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-023-05846-6