Abstract
Objectives
This review aimed to synthesize the available evidence on the effectiveness of telemedicine-based psychosocial interventions among breast cancer (BC) patients regarding quality of life (QOL), depression, anxiety, distress, fatigue, sleep disorders, sexual function, and fear of cancer recurrence (FCR).
Methods
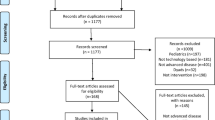
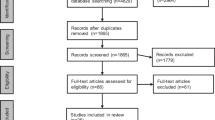
A search of 10 databases was conducted to identify RCTs of the effects of telemedicine-based psychosocial interventions on outcomes. Selection of studies, quality appraisal, and data extraction were performed by two reviewers independently. GRADE and Cochrane risk of bias assessment tools were used for quality appraisal. Heterogeneity was determined by I2, standardized mean differences (SMD) were used to determine intervention effects, and meta-analyses, subgroup analysis, and sensitivity analysis were performed.
Results
In total, 29 RCTs were included. Telemedicine-based psychosocial interventions improved the primary outcomes of QOL (SMD = 0.32), distress (SMD = − 0.22), and anxiety (SMD = − 0.16) in BC patients with moderate effect size. There were some improvements in the secondary outcomes of sleep disorders (SMD = − 056), sexual function (SMD = 0.19), and FCR (SMD = − 0.41). After sensitivity analysis, the effect size of fatigue was moderate (SMD = − 0.24).
Conclusion
Telemedicine-based psychosocial interventions are superior to usual care in BC patients with improved QOL, sexual function, and less distress, anxiety, fatigue, sleep disorders, and FCR. Due to the heterogeneity of the results for QOL, anxiety, fatigue, sleep disturbance, and FCR, these results should be interpreted cautiously. In the future, more rigorous RCTs need to be designed to identify better delivery models and intervention times to further test their effectiveness.
















Similar content being viewed by others
Data availability
Full disclosure, as seen in the supplementary material in the appendix.
References
Sung H, Ferlay J, Siegel RL et al (2021) Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
Li H, Liu Z, Yuan L et al (2021) Radionuclide-based imaging of breast cancer: state of the art. Cancers 13(21):5459. https://doi.org/10.3390/cancers13215459
Jewett PI, Vogel RI, Galchutt P et al (2022) Associations between a sense of connection and existential and psychosocial outcomes in gynecologic and breast cancer survivors. Support Care Cancer 30(4):3329–3336. https://doi.org/10.1007/s00520-021-06784-8
Coles CE, Anderson BO, Cameron D et al (2022) The Lancet Breast Cancer Commission: tackling a global health, gender, and equity challenge. Lancet (London, England) 399(10330):1101–1103. https://doi.org/10.1016/s0140-6736(22)00184-2
Kohrt BA, Song SJ (2018) Who benefits from psychosocial support interventions in humanitarian settings? Lancet Glob Health 6(4):e354–e356. https://doi.org/10.1016/S2214-109X(18)30102-5
Gudenkauf LM, Ehlers SL (2018) Psychosocial interventions in breast cancer survivorship care. Breast (Edinburgh, Scotland) 38:1–6. https://doi.org/10.1016/j.breast.2017.11.005
Treanor CJ, Santin O, Prue G et al (2019) Psychosocial interventions for informal caregivers of people living with cancer. Cochrane Database Syst Rev 6(6):Cd009912. https://doi.org/10.1002/14651858.CD009912.pub2
Boghosian T, McCuaig JM, Carlsson L, Metcalfe KA (2021) Psychosocial interventions for women with a BRCA1 or BRCA2 mutation: a scoping review. Cancers 13(7):1486. https://doi.org/10.3390/cancers13071486
Warmoth K, Yeung NCY, Xie J et al (2020) Benefits of a psychosocial intervention on positive affect and posttraumatic growth for Chinese American breast cancer survivors: a pilot study. Behav Med 46(1):34–42. https://doi.org/10.1080/08964289.2018.1541862
Piroth MD, Draia S, Jawad JA, Piefke M (2022) Anxiety and depression in patients with breast cancer undergoing radiotherapy: the role of intelligence, life history, and social support-preliminary results from a monocentric analysis. Strahlenther Onkol 198(4):388–396. https://doi.org/10.1007/s00066-022-01904-7
Lukas H, Xu C, Yu Y, Gao W (2020) Emerging telemedicine tools for remote COVID-19 diagnosis, monitoring, and management. ACS Nano 14(12):16180–16193. https://doi.org/10.1021/acsnano.0c08494
Nizeyimana E, Joseph C, Louw QA (2022) A scoping review of feasibility, cost-effectiveness, access to quality rehabilitation services and impact of telerehabilitation: a review protocol. Digit Health 8:20552076211066708. https://doi.org/10.1177/20552076211066708
Lee J, Lee EH, Chae D (2021) eHealth literacy instruments: systematic review of measurement properties. J Med Internet Res 23(11):e30644. https://doi.org/10.2196/30644
Jacobs JM, Walsh EA, Rapoport CS et al (2021) Development and refinement of a telehealth intervention for symptom management, distress, and adherence to adjuvant endocrine therapy after breast cancer. J Clin Psychol Med Settings 28(3):603–618. https://doi.org/10.1007/s10880-020-09750-4
Bunnell BE, Barrera JF, Paige SR, Turner D, Welch BM (2020) Acceptability of telemedicine features to promote its uptake in practice: a survey of community telemental health providers. Int J Environ Res Public Health 17(22):8525. https://doi.org/10.3390/ijerph17228525
Ma Y, Cheng HY, Cheng L, Sit JWH (2019) The effectiveness of electronic health interventions on blood pressure control, self-care behavioural outcomes and psychosocial well-being in patients with hypertension: a systematic review and meta-analysis. Int J Nurs Stud 92:27–46. https://doi.org/10.1016/j.ijnurstu.2018.11.007
Lai LL, Player H, Hite S et al (2021) Feasibility of remote occupational therapy services via telemedicine in a breast cancer recovery program. Am J Occup Ther 75(2):7502205030p7502205031–7502205030p7502205039. https://doi.org/10.5014/ajot.2021.042119
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ (Clin Res Ed) 372:n71. https://doi.org/10.1136/bmj.n71
Chen Y, Yang K, Marušic A et al (2017) A reporting tool for practice guidelines in health care: the RIGHT statement. Ann Intern Med 166(2):128–132. https://doi.org/10.7326/m16-1565
Sawilowsky SS (2009) New effect size rules of thumb. J Mod Appl Stat Methods 8(2):26. http://digitalcommons.wayne.edu/jmasm/vol8/iss2/26. Accessed 1 Nov 2009
Hedges LV, Pigott TD (2001) The power of statistical tests in meta-analysis. Psychol Methods 6(3):203–217. https://doi.org/10.1037/1082-989x.6.3.203
Varadhan R, Segal JB, Boyd CM, Wu AW, Weiss CO (2013) A framework for the analysis of heterogeneity of treatment effect in patient-centered outcomes research. J Clin Epidemiol 66(8):818–825. https://doi.org/10.1016/j.jclinepi.2013.02.009
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ (Clin Res Ed) 315(7109):629–634. https://doi.org/10.1136/bmj.315.7109.629
Abrahams HJG, Gielissen MFM, Donders RRT et al (2017) The efficacy of Internet-based cognitive behavioral therapy for severely fatigued survivors of breast cancer compared with care as usual: a randomized controlled trial. Cancer 123(19):3825–3834. https://doi.org/10.1002/cncr.30815
Admiraal JM, van der Velden AWG, Geerling JI et al (2017) Web-based tailored psychoeducation for breast cancer patients at the onset of the survivorship phase: a multicenter randomized controlled trial. J Pain Symptom Manage 54(4):466–475. https://doi.org/10.1016/j.jpainsymman.2017.07.009
Amidi A, Buskbjerg CR, Damholdt MF et al (2022) Changes in sleep following internet-delivered cognitive-behavioral therapy for insomnia in women treated for breast cancer: a 3-year follow-up assessment. Sleep Med 96:35–41. https://doi.org/10.1016/j.sleep.2022.04.020
Akechi T, Yamaguchi T, Uchida M et al (2023) Smartphone psychotherapy reduces fear of cancer recurrence among breast cancer survivors: a fully decentralized randomized controlled clinical trial (J-SUPPORT 1703 Study). J Clin Oncol 41(5):1069–1078. https://doi.org/10.1200/JCO.22.00699
Akkol-Solakoglu S, Hevey D (2023) Internet-delivered cognitive behavioural therapy for depression and anxiety in breast cancer survivors: results from a randomised controlled trial. Psychooncology 32(3):446–456. https://doi.org/10.1002/pon.6097
Ashing K, Rosales M (2014) A telephonic-based trial to reduce depressive symptoms among Latina breast cancer survivors. Psychooncology 23(5):507–515. https://doi.org/10.1002/pon.3441
Atema V, van Leeuwen M, Kieffer JM et al (2019) Efficacy of internet-based cognitive behavioral therapy for treatment-induced menopausal symptoms in breast cancer survivors: results of a randomized controlled trial. J Clin Oncol 37(10):809–822. https://doi.org/10.1200/jco.18.00655
Badger T, Segrin C, Meek P, Lopez AM, Bonham E, Sieger A (2005) Telephone interpersonal counseling with women with breast cancer: symptom management and quality of life. Oncol Nurs Forum 32(2):273–279. https://doi.org/10.1188/05.Onf.273-279
Carpenter KM, Stoner SA, Schmitz K, McGregor BA, Doorenbos AZ (2014) An online stress management workbook for breast cancer. J Behav Med 37(3):458–468. https://doi.org/10.1007/s10865-012-9481-6
David N, Schlenker P, Prudlo U, Larbig W (2011) Online counseling via e-mail for breast cancer patients on the German internet: preliminary results of a psychoeducational intervention. Psycho-Soc Med 8:Doc05. https://doi.org/10.3205/psm000074
Freeman LW, White R, Ratcliff CG et al (2015) A randomized trial comparing live and telemedicine deliveries of an imagery-based behavioral intervention for breast cancer survivors: reducing symptoms and barriers to care. Psychooncology 24(8):910–918. https://doi.org/10.1002/pon.3656
Ghanbari E, Yektatalab S, Mehrabi M (2021) Effects of psychoeducational interventions using mobile apps and mobile-based online group discussions on anxiety and self-esteem in women with breast cancer: randomized controlled trial. JMIR Mhealth Uhealth 9(5):e19262. https://doi.org/10.2196/19262
Holtdirk F, Mehnert A, Weiss M et al (2021) Results of the Optimune trial: a randomized controlled trial evaluating a novel Internet intervention for breast cancer survivors. PLoS ONE 16(5):e0251276. https://doi.org/10.1371/journal.pone.0251276
Hou IC, Lin HY, Shen SH et al (2020) Quality of life of women after a first diagnosis of breast cancer using a self-management support mHealth app in Taiwan: randomized controlled trial. JMIR Mhealth Uhealth 8(3):e17084. https://doi.org/10.2196/17084
Hummel SB, van Lankveld J, Oldenburg HSA et al (2017) Efficacy of internet-based cognitive behavioral therapy in improving sexual functioning of breast cancer survivors: results of a randomized controlled trial. J Clin Oncol 35(12):1328–1340. https://doi.org/10.1200/jco.2016.69.6021
Wang L, Chen X, Peng Y et al (2022) Effect of a 4-week internet-delivered mindfulness-based cancer recovery intervention on the symptom burden and quality of life of patients with breast cancer: randomized controlled trial. J Med Internet Res 24(11):e40059. https://doi.org/10.2196/40059
Peng L, Yang Y, Chen M et al (2022) Effects of an online mindfulness-based intervention on Fear of Cancer Recurrence and quality of life among Chinese breast cancer survivors. Complement Ther Clin Pract 49:101686. https://doi.org/10.1016/j.ctcp.2022.101686
Merckaert I, Waroquier P, Caillier M et al (2023) Improving emotion regulation in breast cancer patients in the early survivorship period: efficacy of a brief ecologically boosted group intervention. Psychooncology 32(4):597–609. https://doi.org/10.1002/pon.6105
Rosen KD, Paniagua SM, Kazanis W, Jones S, Potter JS (2018) Quality of life among women diagnosed with breast cancer: a randomized waitlist controlled trial of commercially available mobile app-delivered mindfulness training. Psychooncology 27(8):2023–2030. https://doi.org/10.1002/pon.4764
Sandgren AK, McCaul KD (2003) Short-term effects of telephone therapy for breast cancer patients. Health Psychol 22(3):310–315. https://doi.org/10.1037/0278-6133.22.3.310
Shen et al, Wanmin Qiang, Qing Wang, Zihan Zhao, Shurui Wang (2021) The effect of internet mindfulness-based cancer recovery on perceived stress, fatigue and anxiety of breast cancer survivors during transitional period. J Nurs Train [in Chinese] 36(23):2113–2116,2123
Van den Berg SW, Gielissen MF, Custers JA, van der Graaf WT, Ottevanger PB, Prins JB (2015) BREATH: web-based self-management for psychological adjustment after primary breast cancer–results of a multicenter randomized controlled trial. J Clin Oncol 33(25):2763–2771. https://doi.org/10.1200/jco.2013.54.9386
Owen JE, Klapow JC, Roth DL et al (2005) Randomized pilot of a self-guided internet coping group for women with early-stage breast cancer. Ann Behav Med 30(1):54–64. https://doi.org/10.1207/s15324796abm3001_7
Stanton AL, Ganz PA, Kwan L et al (2005) Outcomes from the moving beyond cancer psychoeducational, randomized, controlled trial with breast cancer patients. J Clin Oncol 23(25):6009–6018. https://doi.org/10.1200/jco.2005.09.101
Villani D, Cognetta C, Repetto C et al (2018) Promoting emotional well-being in older breast cancer patients: results from an eHealth intervention. Front Psychol 9:2279. https://doi.org/10.3389/fpsyg.2018.02279
Winzelberg AJ, Classen C, Alpers GW et al (2003) Evaluation of an internet support group for women with primary breast cancer. Cancer 97(5):1164–1173. https://doi.org/10.1002/cncr.11174
White V, Farrelly A, Pitcher M, Hill D (2018) Does access to an information-based, breast cancer specific website help to reduce distress in young women with breast cancer? Results from a randomised trial. Eur J Cancer Care 27(6):e12897. https://doi.org/10.1111/ecc.12897
Zachariae R, Amidi A, Damholdt MF et al (2018) Internet-delivered cognitive-behavioral therapy for insomnia in breast cancer survivors: a randomized controlled trial. J Natl Cancer Inst 110(8):880–887. https://doi.org/10.1093/jnci/djx293
Zhu J, Ebert L, Liu X, Wei D, Chan SW (2018) Mobile breast cancer e-support program for Chinese women with breast cancer undergoing chemotherapy (part 2): multicenter randomized controlled trial. JMIR Mhealth Uhealth 6(4):e104. https://doi.org/10.2196/mhealth.9438
Getu MA, Chen C, Panpan W, Mboineki JF, Dhakal K, Du R (2021) The effect of cognitive behavioral therapy on the quality of life of breast cancer patients: a systematic review and meta-analysis of randomized controlled trials. Qual Life Res 30(2):367–384. https://doi.org/10.1007/s11136-020-02665-5
Sacks D, Baxter B, Campbell BCV et al (2018) Multisociety consensus quality improvement revised consensus statement for endovascular therapy of acute ischemic stroke. Int J Stroke 13(6):612–632. https://doi.org/10.1177/1747493018778713
Saffari M, Ghanizadeh G, Koenig HG (2014) Health education via mobile text messaging for glycemic control in adults with type 2 diabetes: a systematic review and meta-analysis. Prim Care Diabetes 8(4):275–285. https://doi.org/10.1016/j.pcd.2014.03.004
Okuyama S, Jones W, Ricklefs C, Tran ZV (2015) Psychosocial telephone interventions for patients with cancer and survivors: a systematic review. Psychooncology 24(8):857–870. https://doi.org/10.1002/pon.3704
Luo X, Chen Y, Chen J et al (2022) Effectiveness of mobile health-based self-management interventions in breast cancer patients: a meta-analysis. Support Care Cancer 30(3):2853–2876. https://doi.org/10.1007/s00520-021-06568-0
Ream E, Hughes AE, Cox A et al (2020) Telephone interventions for symptom management in adults with cancer. Cochrane Database Syst Rev 6(6):Cd007568. https://doi.org/10.1002/14651858.CD007568.pub2
Fridriksdottir N, Gunnarsdottir S, Zoëga S, Ingadottir B, Hafsteinsdottir EJG (2018) Effects of web-based interventions on cancer patients’ symptoms: review of randomized trials. Support Care Cancer 26(2):337–351. https://doi.org/10.1007/s00520-017-3882-6
Lai CH, Kim YK, Radua J (2021) Editorial: neuroimaging biomarkers in mood and anxiety disorders. Front Psych 12:773034. https://doi.org/10.3389/fpsyt.2021.773034
Martin EI, Ressler KJ, Binder E, Nemeroff CB (2009) The neurobiology of anxiety disorders: brain imaging, genetics, and psychoneuroendocrinology. Psychiatr Clin North Am 32(3):549–575. https://doi.org/10.1016/j.psc.2009.05.004
Ratanasiripong P, Ratanasiripong N, Kathalae D (2012) Biofeedback intervention for stress and anxiety among nursing students: a randomized controlled trial. ISRN Nurs 2012:827972. https://doi.org/10.5402/2012/827972
Wang Y, Lin Y, Chen J, Wang C, Hu R, Wu Y (2020) Effects of Internet-based psycho-educational interventions on mental health and quality of life among cancer patients: a systematic review and meta-analysis. Support Care Cancer 28(6):2541–2552. https://doi.org/10.1007/s00520-020-05383-3
Lee JZJ, Chen HC, Lee JX, Klainin-Yobas P (2021) Effects of psychosocial interventions on psychological outcomes among caregivers of advanced cancer patients: a systematic review and meta-analysis. Support Care Cancer 29(12):7237–7248. https://doi.org/10.1007/s00520-021-06102-2
Berner M, Günzler C (2012) Efficacy of psychosocial interventions in men and women with sexual dysfunctions–a systematic review of controlled clinical trials: part 1-the efficacy of psychosocial interventions for male sexual dysfunction. J Sex Med 9(12):3089–3107. https://doi.org/10.1111/j.1743-6109.2012.02970.x
Jannati N, Mazhari S, Ahmadian L, Mirzaee M (2020) Effectiveness of an app-based cognitive behavioral therapy program for postpartum depression in primary care: a randomized controlled trial. Int J Med Informatics 141:104145. https://doi.org/10.1016/j.ijmedinf.2020.104145
Skrabal Ross X, Gunn KM, Olver I et al (2020) Online psychosocial interventions for posttreatment cancer survivors: an international evidence review and update. Curr Opin Support Palliat Care 14(1):40–50. https://doi.org/10.1097/spc.0000000000000478
Rosenman R, Tennekoon V, Hill LG (2011) Measuring bias in self-reported data. Int J Behav Healthc Res 2(4):320–332. https://doi.org/10.1504/ijbhr.2011.043414
Lee I, Kovarik C, Tejasvi T, Pizarro M, Lipoff JB (2020) Telehealth: helping your patients and practice survive and thrive during the COVID-19 crisis with rapid quality implementation. J Am Acad Dermatol 82(5):1213–1214. https://doi.org/10.1016/j.jaad.2020.03.052
Medina JC, Flix-Valle A, Rodríguez-Ortega A, Hernández-Ribas R, Lleras de Frutos M, Ochoa-Arnedo C (2022) ICOnnecta’t: development and initial results of a stepped psychosocial ehealth ecosystem to facilitate risk assessment and prevention of early emotional distress in breast cancer survivors’ journey. Cancers 14(4). https://doi.org/10.3390/cancers14040974
Funding
This work was supported by the Nursing Project of Superior Discipline Construction in Jiangsu Universities (szbf [2018] No. 87), and Nursing Science, a Key Discipline Project of Jiangsu Province during the 13th Five-Year Plan period (sjy [2016] No. 9).
Author information
Authors and Affiliations
Contributions
ZM and YS contributed equally to this work. ZM and YS have made substantial contributions to conception and design, or acquisition of data, or analysis and interpretation of data; SY and NL have critically drafted the important intellectual content of the article; FC approved the version to be published and all subsequent versions.
Corresponding author
Ethics declarations
Ethics approval
This study is a systematic review and does not involve ethical issues such as consent and participation.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ma, Z., Shi, Y., Yao, S. et al. Effectiveness of telemedicine-based psychosocial intervention for breast cancer patients: a systematic review and meta-analysis. Support Care Cancer 31, 595 (2023). https://doi.org/10.1007/s00520-023-08052-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-023-08052-3