Abstract
Background
Laparoscopic liver resection (LLR) of high difficulty score is technically challenging. There is a lack of clinical evidence to support its applicability in terms of the long-term survival benefits. This study aims to compare clinical outcomes between LLR and the open liver resection of high difficulty score for hepatocellular carcinoma (HCC).
Materials and Methods
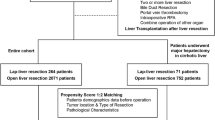
From 2010 to 2020, using Iwate criteria, 424 patients underwent liver resection of high difficulty score by the laparoscopic (n = 65) or open (n = 359) approach. Propensity score (PS) matching was performed between the two groups. Short-term and long-term outcomes were compared between PS-matched groups. Univariate and multivariate analyses were performed to identify prognostic factors affecting survival.
Results
The laparoscopic group had significantly fewer severe complications (3% vs. 10.8%), and shorter median hospital stays (6 days vs. 8 days) than the open group. Meanwhile, the long-term oncological outcomes were comparable between the two groups, in terms of the tumor recurrence rate (40% vs. 46.1%), the 5-year overall survival rate (75.4% vs. 76.2%), and the 5-year recurrence-free survival rate (50.3% vs. 53.5%). The high preoperative serum alpha-fetoprotein level, multiple tumors, and severe postoperative complications were the independent poor prognostic factors associated with worse overall survival. The surgical approach (Laparoscopic vs. Open) did not influence the survival.
Conclusion
LLR of high difficulty score for selected patients with HCC has better short-term outcomes than the open approach. More importantly, it can achieve similar long-term survival outcomes as the open approach.















Similar content being viewed by others
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: Cancer J Clin 68:394–424
Galle Peter R, Forner Alejandro, Llovet Josep M, Mazzaferro Vincenzo, Piscaglia Fabio, Raoul Jean-Luc, Schirmacher Peter, Vilgrain Valérie (2018) EASL clinical practice guidelines: management of hepatocellular carcinoma. J Hepatol 69:182–236
Heimbach JK, Kulik LM, Finn RS, Sirlin CB, Abecassis MM, Roberts LR, Zhu AX, Murad MH, Marrero JA (2018) AASLD guidelines for the treatment of hepatocellular carcinoma. Hepatology 67:358–380
Vogel A, Cervantes A, Chau I, Daniele B, Llovet JM, Meyer T, Nault JC, Neumann U, Ricke J, Sangro B, Schirmacher P, Verslype C, Zech CJ, Arnold D, Martinelli E (2018) Hepatocellular carcinoma: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 29(Suppl 4):iv238–iv255
Yoon YI, Kim KH, Kang SH, Kim WJ, Shin MH, Lee SK, Jung DH, Park GC, Ahn CS, Moon DB, Ha TY, Song GW, Hwang S, Lee SG (2016) Pure laparoscopic versus open right hepatectomy for hepatocellular carcinoma in patients with cirrhosis: a propensity score matched analysis. Ann Surg. https://doi.org/10.1097/SLA.0000000000002072
Morise Z (2019) Developments and perspectives of laparoscopic liver resection in the treatment of hepatocellular carcinoma. Surg Today 49:649–655
Buell JF, Cherqui D, Geller DA, O’Rourke N, Iannitti D, Dagher I, Koffron AJ, Thomas M, Gayet B, Han HS, Wakabayashi G, Belli G, Kaneko H, Ker CG, Scatton O, Laurent A, Abdalla EK, Chaudhury P, Dutson E, Gamblin C, D’Angelica M, Nagorney D, Testa G, Labow D, Manas D, Poon RT, Nelson H, Martin R, Clary B, Pinson WC, Martinie J, Vauthey JN, Goldstein R, Roayaie S, Barlet D, Espat J, Abecassis M, Rees M, Fong Y, McMasters KM, Broelsch C, Busuttil R, Belghiti J, Strasberg S, Chari RS (2009) The international position on laparoscopic liver surgery: the Louisville statement, 2008. Ann Surg 250:825–830
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS, Asbun H, O’Rourke N, Tanabe M, Koffron AJ, Tsung A, Soubrane O, Machado MA, Gayet B, Troisi RI, Pessaux P, Van Dam RM, Scatton O, Abu Hilal M, Belli G, Kwon CH, Edwin B, Choi GH, Aldrighetti LA, Cai X, Cleary S, Chen KH, Schön MR, Sugioka A, Tang CN, Herman P, Pekolj J, Chen XP, Dagher I, Jarnagin W, Yamamoto M, Strong R, Jagannath P, Lo CM, Clavien PA, Kokudo N, Barkun J, Strasberg SM (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261:619–629
Ban D, Tanabe M, Ito H, Otsuka Y, Nitta H, Abe Y, Hasegawa Y, Katagiri T, Takagi C, Itano O, Kaneko H, Wakabayashi G (2014) A novel difficulty scoring system for laparoscopic liver resection. J Hepatobiliary Pancreat Sci 21:745–753
Wakabayashi G (2016) What has changed after the Morioka consensus conference 2014 on laparoscopic liver resection? Hepatobiliary Surg Nutr 5:281–289
Tanaka S, Kubo S, Kanazawa A, Takeda Y, Hirokawa F, Nitta H, Nakajima T, Kaizu T, Kaneko H, Wakabayashi G (2017) Validation of a difficulty scoring system for laparoscopic liver resection: a multicenter analysis by the endoscopic liver surgery study group in Japan. J Am Coll Surg 225(249–258):e241
Chong CCN, Lok HT, Fung AKY, Fong AKW, Cheung YS, Wong J, Lee KF, Lai PBS (2020) Robotic versus laparoscopic hepatectomy: application of the difficulty scoring system. Surg Endosc 34:2000–2006
Cipriani F, Fiorentini G, Magistri P, Fontani A, Menonna F, Annecchiarico M, Lauterio A, De Carlis L, Coratti A, Boggi U, Ceccarelli G, Di Benedetto F, Aldrighetti L (2021) Pure laparoscopic versus robotic liver resections: multicentric propensity score-based analysis with stratification according to difficulty scores. J Hepatobiliary Pancreat Sci. https://doi.org/10.1016/j.hpb.2021.08.123
Ng KK, Vauthey JN, Pawlik TM, Lauwers GY, Regimbeau JM, Belghiti J, Ikai I, Yamaoka Y, Curley SA, Nagorney DM, Ng IO, Fan ST, Poon RT, International Cooperative Study Group on Hepatocellular C (2005) Is hepatic resection for large or multinodular hepatocellular carcinoma justified? Results from a multi-institutional database. Ann Surg Oncol 12:364–373
Lee KF, Cheung YS, Wong J, Chong CC, Wong JS, Lai PB (2012) Randomized clinical trial of open hepatectomy with or without intermittent Pringle manoeuvre. Br J Surg 99:1203–1209
Ng KKC, Chok KSH, Chan ACY, Cheung TT, Wong TCL, Fung JYY, Yuen J, Poon RTP, Fan ST, Lo CM (2017) Randomized clinical trial of hepatic resection versus radiofrequency ablation for early-stage hepatocellular carcinoma. Br J Surg 104:1775–1784
Couinaud C (1999) Liver anatomy: portal (and suprahepatic) or biliary segmentation. Dig Surg 16:459–467
Lang H, de Santibañes E, Schlitt HJ, Malagó M, van Gulik T, Machado MA, Jovine E, Heinrich S, Ettorre GM, Chan A, Hernandez-Alejandro R, Robles Campos R, Sandström P, Linecker M, Clavien PA (2019) 10th anniversary of ALPPS-lessons learned and quo vadis. Ann Surg 269:114–119
Wang X, Teh CSC, Ishizawa T, Aoki T, Cavallucci D, Lee SY, Panganiban KM, Perini MV, Shah SR, Wang H, Xu Y, Suh KS, Kokudo N (2021) Consensus guidelines for the use of fluorescence imaging in hepatobiliary surgery. Ann Surg 274:97–106
Choi SH, Choi GH, Han DH, Choi JS (2015) Laparoscopic liver resection using a rubber band retraction technique: usefulness and perioperative outcome in 100 consecutive cases. Surg Endosc 29:387–397
Liu CL, Fan ST, Cheung ST, Lo CM, Ng IO, Wong J (2006) Anterior approach versus conventional approach right hepatic resection for large hepatocellular carcinoma: a prospective randomized controlled study. Ann Surg 244:194–203
Sugioka A, Kato Y, Tanahashi Y (2017) Systematic extrahepatic Glissonean pedicle isolation for anatomical liver resection based on Laennec’s capsule: proposal of a novel comprehensive surgical anatomy of the liver. J Hepatobiliary Pancreat Sci 24:17–23
Shirata C, Kokudo T, Gillet M, Uldry E, Demartines N, Kokudo N, Hasegawa K, Halkic N (2020) Reappraisal of Laennec’s capsule. Surg Oncol 33:222–223
Ng KKC, Cheng NMY, Huang J, Liao M, Chong CCN, Lee KF, Wong J, Cheung SYS, Lok HT, Fung AKY, Wong GLH, Wong VWS, Lai PBS (2021) Development and validation of a novel nomogram predicting 10-year actual survival after curative hepatectomy for hepatocellular carcinoma. Surgeon 19:329–337
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Rahbari NN, Garden OJ, Padbury R, Brooke-Smith M, Crawford M, Adam R, Koch M, Makuuchi M, Dematteo RP, Christophi C, Banting S, Usatoff V, Nagino M, Maddern G, Hugh TJ, Vauthey JN, Greig P, Rees M, Yokoyama Y, Fan ST, Nimura Y, Figueras J, Capussotti L, Buchler MW, Weitz J (2011) Posthepatectomy liver failure: a definition and grading by the International study group of liver surgery (ISGLS). Surgery 149:713–724
Reich H, McGlynn F, DeCaprio J, Budin R (1991) Laparoscopic excision of benign liver lesions. Obstet Gynecol 78:956–958
Nguyen KT, Gamblin TC, Geller DA (2009) World review of laparoscopic liver resection-2,804 patients. Ann Surg 250:831–841
Berardi G, Van Cleven S, Fretland ÅA, Barkhatov L, Halls M, Cipriani F, Aldrighetti L, Abu Hilal M, Edwin B, Troisi RI (2017) Evolution of laparoscopic liver surgery from innovation to implementation to mastery: perioperative and oncologic outcomes of 2,238 patients from 4 European specialized centers. J Am Coll Surg 225:639–649
Hasegawa Y, Wakabayashi G, Nitta H, Takahara T, Katagiri H, Umemura A, Makabe K, Sasaki A (2017) A novel model for prediction of pure laparoscopic liver resection surgical difficulty. Surg Endosc 31:5356–5363
Halls MC, Berardi G, Cipriani F, Barkhatov L, Lainas P, Harris S, D’Hondt M, Rotellar F, Dagher I, Aldrighetti L, Troisi RI, Edwin B, Abu Hilal M (2018) Development and validation of a difficulty score to predict intraoperative complications during laparoscopic liver resection. Brit J Surg. https://doi.org/10.1002/bjs.10821
Kawaguchi Y, Fuks D, Kokudo N, Gayet B (2018) Difficulty of laparoscopic liver resection: proposal for a new classification. Ann Surg 267:13–17
Lin H, Bai Y, Yin M, Chen Z, Yu S (2022) External validation of different difficulty scoring systems of laparoscopic liver resection for hepatocellular carcinoma. Surg Endosc 36:3732–3749
Barron JO, Orabi D, Moro A, Quintini C, Berber E, Aucejo FN, Sasaki K, Kwon C-HD (2022) Validation of the IWATE criteria as a laparoscopic liver resection difficulty score in a single North American cohort. Surg Endosc 36:3601–3609
Choi SH, Chen KH, Syn NL, Cipriani F, Cheung TT, Chiow AKH, Choi GH, Siow TF, Sucandy I, Marino MV, Gastaca M, Chong CC, Lee JH, Ivanecz A, Mazzaferro V, Lopez-Ben S, Fondevila C, Rotellar F, Campos RR, Efanov M, Kingham TP, Sutcliffe RP, Troisi RI, Pratschke J, Wang X, D’Hondt M, Yong CC, Levi Sandri GB, Tang CN, Ruzzenente A, Cherqui D, Ferrero A, Wakabayashi G, Scatton O, Aghayan D, Edwin B, Coelho FF, Giuliante F, Liu R, Sijberden J, Abu Hilal M, Sugioka A, Long TCD, Fuks D, Aldrighetti L, Han HS, Goh BKP (2022) Utility of the Iwate difficulty scoring system for laparoscopic right posterior sectionectomy: do surgical outcomes differ for tumors in segments VI and VII? Surg Endosc 36:9204–9214
Tanaka S, Kawaguchi Y, Kubo S, Kanazawa A, Takeda Y, Hirokawa F, Nitta H, Nakajima T, Kaizu T, Kaibori M, Kojima T, Otsuka Y, Fuks D, Hasegawa K, Kokudo N, Kaneko H, Gayet B, Wakabayashi G (2019) Validation of index-based IWATE criteria as an improved difficulty scoring system for laparoscopic liver resection. Surgery 165:731–740
Tang Z, Tang Y, Liu T, Liu R, Xie S, Xie D, Yang J, Tang Y (2021) Clinical study on the efficacy of laparoscopic hepatectomy and its influence on the expression of serum VEGF, FGF, and immune function. Evid Based Complement Alternat Med 2021:4432022
Li W, Zhou X, Huang Z, Zhang H, Zhang L, Shang C, Chen Y (2015) Laparoscopic surgery minimizes the release of circulating tumor cells compared to open surgery for hepatocellular carcinoma. Surg Endosc 29:3146–3153
Ibuki S, Hibi T, Tanabe M, Geller DA, Cherqui D, Wakabayashi G (2022) Short-term outcomes of “Difficult” laparoscopic liver resection at specialized centers: report from INSTALL (International survey on technical aspects of laparoscopic liver resection)-2 on 4478 patients. Ann Surg 275:940–946
Lv X, Zhang L, Yu X, Yu H (2023) The difficulty grade of laparoscopic hepatectomy for hepatocellular carcinoma correlates with long-term outcomes. Updates Surg. https://doi.org/10.1007/s13304-023-01452-4
Moris D, Tsilimigras DI, Kostakis ID, Ntanasis-Stathopoulos I, Shah KN, Felekouras E, Pawlik TM (2018) Anatomic versus non-anatomic resection for hepatocellular carcinoma: a systematic review and meta-analysis. Eur J Surg Oncol 44:927–938
Cipriani F, Alzoubi M, Fuks D, Ratti F, Kawai T, Berardi G, Barkhatov L, Lainas P, Van der Poel M, Faoury M, Besselink MG, D’Hondt M, Dagher I, Edwin B, Troisi RI, Scatton O, Gayet B, Aldrighetti L, Abu Hilal M (2020) Pure laparoscopic versus open hemihepatectomy: a critical assessment and realistic expectations—a propensity score-based analysis of right and left hemihepatectomies from nine European tertiary referral centers. J Hepatobiliary Pancreat Sci 27:3–15
Kong J, Li G, Chai J, Yu G, Liu Y, Liu J (2021) Impact of postoperative complications on long-term survival after resection of hepatocellular carcinoma: a systematic review and meta-analysis. Ann Surg Oncol 28:8221–8233
Ng KKC, Chong CCN, Lee KF, Lai PBS, Cheng TKC, Chen HW, Yi B, Huang JW (2023) Asia-Pacific multicentre randomized trial of laparoscopic versus open major hepatectomy for hepatocellular carcinoma (AP-LAPO trial). BJS Open. https://doi.org/10.1093/bjsopen/zrac166
Vigano L, Laurent A, Tayar C, Tomatis M, Ponti A, Cherqui D (2009) The learning curve in laparoscopic liver resection: improved feasibility and reproducibility. Ann Surg 250:772–782
Nomi T, Fuks D, Kawaguchi Y, Mal F, Nakajima Y, Gayet B (2015) Learning curve for laparoscopic major hepatectomy. Br J Surg 102:796–804
Acknowledgements
The authors would gratefully thank Mr. Philip Ip (Department of Surgery, The Chinese University of Hong Kong) for his excellent help with the data collection and analysis.
Funding
The present study receives no funding from any organization.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Prof. Kelvin K.C. Ng, Dr. Kai-Chi Cheng, Dr. Janet W.C. Kung, Dr. Kit-Man Ho, Dr. Hon-Ting Lok, Dr. Andrew K.Y. Fung, Dr. Charing C.N. Chong, Dr. Sunny Y.S. Cheung, Dr. Kit-Fai Lee, Dr. John Wong, and Prof. Paul B.S. Lai have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ng, K.K.C., Cheng, KC., Kung, J.W.C. et al. Comparison of clinical outcome between laparoscopic and open hepatectomy of high difficulty score for hepatocellular carcinoma: a propensity score analysis. Surg Endosc 38, 857–871 (2024). https://doi.org/10.1007/s00464-023-10634-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10634-5