Abstract
Background
We identified trends of inpatient therapeutic endoscopic retrograde cholangiopancreatography (ERCP) in the United States (US), focusing on outcomes related to specific patient demographics.
Methods
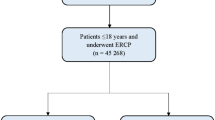
The National Inpatient Sample was utilized to identify all adult inpatient ERCP in the US between 2007–2018. Trends of utilization and adverse outcomes were highlighted. P-values ≤ 0.05 were considered statistically significant.
Results
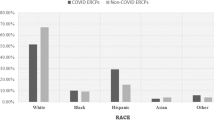
We noted a rising trend for total inpatient ERCP in the US from 126,921 in 2007 to 165,555 in 2018 (p = 0.0004), with a significant increase in utilization for Blacks, Hispanics, and Asians. Despite an increasing comorbidity burden [Charlson Comorbidity Index (CCI) score ≥ 2], the overall inpatient mortality declined from 1.56% [2007] to 1.46% [2018] without a statistically significant trend (p = 0.14). Moreover, there was a rising trend of inpatient mortality for Black and Hispanic populations, while a decline was noted for Asians. After a comparative analysis, we noted higher rates of inpatient mortality for Blacks (2.4% vs 1.82%, p = 0.0112) and Hispanics (1.17% vs 0.83%, p = 0.0052) at urban teaching hospitals between July toand September compared to the October to June study period; however, we did not find a statistically significant difference for the Asian cohort (1.9% vs 2.10%, p = 0.56). The mean length of stay (LOS) decreased from 7 days in 2007 to 6 days in 2018 (p < 0.0001), while the mean total hospital charge (THC) increased from $48,883 in 2007 to $85,909 in 2018 (p < 0.0001) for inpatient ERCPs. Compared to the 2015–2018 study period, we noted higher rates of post-ERCP pancreatitis (27.76% vs 17.25%, p < 0.0001) from 2007–2014.
Conclusion
Therapeutic ERCP utilization and inpatient mortality were on the rise for a subset of the American minority population, including Black and Hispanics.


Similar content being viewed by others
Data availability
The NIS is a large, publicly available database accessed at https://www.hcup-us.ahrq.gov. Due to the large sample size provided by the NIS, it is ideal for estimating national trends and outcomes.
References
Kozarek RA (2017) The past, present, and future of endoscopic retrograde cholangiopancreatography. Gastroenterol Hepatol (N Y) 13:620–622
Kröner PT, Bilal M, Samuel R et al (2020) Use of ERCP in the United States over the past decade. Endosc Int Open 8:E761–E769
Szary NM, Al-Kawas FH (2013) Complications of endoscopic retrograde cholangiopancreatography: how to avoid and manage them. Gastroenterol Hepatol (N Y) 9:496–504
Solanki S, Kichloo A, Dahiya DS et al (2021) Endoscopic Retrograde Cholangiopancreatography (ERCP) in patients with liver cirrhosis: analysis of trends and outcomes from the national inpatient sample database. J Clin Gastroenterol. https://doi.org/10.1097/MCG.0000000000001573,June9,2021
Moffatt DC, Yu BN, Yie W et al (2014) Trends in utilization of diagnostic and therapeutic ERCP and cholecystectomy over the past 25 years: a population-based study. Gastrointest Endosc 79:615–622
Schutz SM (2011) Grading the degree of difficulty of ERCP procedures. Gastroenterol Hepatol (N Y) 7:674–676
Cao J, Peng C, Ding X et al (2018) Risk factors for post-ERCP cholecystitis: a single-center retrospective study. BMC Gastroenterol 18:128
Sharma A, Mossad D, Markert R (2017) ERCP is associated with greater morbidity and mortality when compared to laparoscopic cholecystectomy. Am J Gastroenterol 112:S18–S19
Williams EJ, Taylor S, Fairclough P et al (2007) Risk factors for complication following ERCP; results of a large-scale, prospective multicenter study. Endoscopy 39:793–801
Kwak N, Yeoun D, Arroyo-Mercado F et al (2020) Outcomes and risk factors for ERCP-related complications in a predominantly black urban population. BMJ Open Gastroenterol 7:e000462
Tavakkoli A, Singal AG, Waljee AK et al (2019) Regional and racial variations in the utilization of endoscopic retrograde cholangiopancreatography among pancreatic cancer patients in the United States. Cancer Med 8:3420–3427
Chiang AL, Banks PA, McNabb-Baltar J (2015) Racial and insurance status disparities in ERCP utilization in acute pancreatitis. Am J Gastroenterol 110:S35
Kanotra R, Ahmed M, Khan HM et al (2015) Median household, racial, and insurance disparities in endoscopic retrograde cholangiopancreatography (ERCP). Am J Gastroenterol 110:S972
Rustgi SD, Amin SP, Kim MK et al (2019) Age, socioeconomic features, and clinical factors predict receipt of endoscopic retrograde cholangiopancreatography in pancreatic cancer. World J Gastrointest Endosc 11:133–144
Fogel EL, Shahda S, Sandrasegaran K et al (2016) A multidisciplinary approach to pancreas cancer in 2016: A Review. Am J Gastroenterol 112:537–554
ASGE Standards of Practice Committee, Chandrasekhara V, Khashab MA et al (2017) Adverse events associated with ERCP. Gastrointest Endosc 85:32–47
Healthcare Cost and Utilization Project (2018) Introduction to the HCUP National Inpatient Sample (NIS). Available at: https://www.hcup-us.ahrq.gov/db/nation/nis/NIS_Introduction_2018.jsp and https://www.hcup-us.ahrq.gov/db/nation/nis/NIS_Introduction_2018.jsp. November 2020; Accessed 1 Oct 2021
Houchens R, Ross, D, Elixhauser A, et al (2014) Nationwide Inpatient Sample (NIS) Redesign Final Report. Available: http://www.hcup-us.ahrq.gov/reports/methods/methods.jsp. November 2014; Accessed 1 Oct 2021
Galeazzi M, Mazzola P, Valcarcel B et al (2018) Endoscopic retrograde cholangiopancreatography in the elderly: results of a retrospective study and a geriatricians’ point of view. BMC Gastroenterol 18:38
Finkelmeier F, Tal A, Ajouaou M et al (2015) ERCP in elderly patients: increased risk of sedation adverse events but low frequency of post-ERCP pancreatitis. Gastrointest Endosc 82:1051–1059
Ukkonen M, Siiki A, Antila A et al (2016) Safety and efficacy of acute endoscopic retrograde cholangiopancreatography in the elderly. Dig Dis Sci 61:3302–3308
Elta GH, Jorgensen J, Coyle WJ (2015) Training in interventional endoscopy: current and future state. Gastroenterology 148:488–490
Lee DW, Kim HG (2018) Age is important, but patient status is also important in endoscopic retrograde cholangiopancreatography. Clin Endosc 51:315–316
Ho VP, Schiltz NK, Reimer AP et al (2019) High-risk comorbidity combinations in older patients undergoing emergency general surgery. J Am Geriatr Soc 67:503–510
Sherman SK, Poli EC, Kapadia MR et al (2018) Estimating surgical risk for patients with severe comorbidities. JAMA Surg 153:778–780
Bai Y, Li F, Wang SL et al (2019) Chinese expert consensus on perioperative medications for endoscopic retrograde cholangiopancreatography (ERCP). J Dig Dis 20:103–113
Hu LH, Xin L, Liao Z et al (2016) Endoscopy audit of the Chinese Society of Digestive Endoscopy. ERCP development in the largest developing country: a national survey from China in 2013. Gastrointest Endosc 84:659–666
Noonan AS, Velasco-Mondragon HE, Wagner FA (2016) Improving the health of African Americans in the USA: an overdue opportunity for social justice. Public Health Rev 37:12
Wechkunanukul K, Grantham H, Damarell R et al (2016) The association between ethnicity and delay in seeking medical care for chest pain: a systematic review. JBI Database Syst Rev Implement Rep 14:208–235
Lee F, Ohanian E, Rheem J et al (2015) Delayed endoscopic retrograde cholangiopancreatography is associated with persistent organ failure in hospitalised patients with acute cholangitis. Aliment Pharmacol Ther 42:212–220
Chong VH, Yim HB, Lim CC (2005) Endoscopic retrograde cholangiopancreatography in the elderly: outcomes, safety and complications. Singapore Med J 46:621–626
Rotundo L, Afridi F, Feurdean M et al (2021) Effect of hospital teaching status on endoscopic retrograde cholangiopancreatography mortality and complications in the USA. Surg Endosc 35:326–332
Changoor NR, Ortega G, Ekladios M et al (2015) Racial disparities in surgical outcomes: does the level of resident surgeon play a role? Surgery 158:547–555
Fiscella K, Sanders MR (2016) Racial and ethnic disparities in the quality of health care. Annu Rev Public Health 37:375–394
Burke LG, Frakt AB, Khullar D et al (2017) Association between teaching status and mortality in US hospitals. JAMA 23:2105–2113
Fiscella K, Franks P, Gold MR et al (2000) Inequality in quality: addressing socioeconomic, racial, and ethnic disparities in health care. JAMA 283:2579–2584
Dotson E, Nuru-Jeter A (2012) Setting the stage for a business case for leadership diversity in healthcare: history, research, and leverage. J Healthc Manag 57:35–44
Henderson VA, Barr KL, An LC et al (2013) Community-based participatory research and user-centered design in a diabetes medication information and decision tool. Prog Community Health Partnersh 7:171–184
Murray E, Treweek S, Pope C et al (2010) Normalisation process theory: a framework for developing, evaluating and implementing complex interventions. BMC Med 8:63
Johnson KD, Perisetti A, Tharian B et al (2020) Endoscopic retrograde cholangiopancreatography-related complications and their management strategies: a “Scoping” literature review. Dig Dis Sci 65:361–375
Lee TH, Jung YK, Park SH (2014) Preparation of high-risk patients and the choice of guidewire for a successful endoscopic retrograde cholangiopancreatography procedure. Clin Endosc 47:334–340
Sobani ZA, Yunina D, Abbasi A et al (2018) Endoscopic retrograde cholangiopancreatography in nonagenarian patients: is it really safe? Clin Endosc 51:375–380
Mehta HB, Dimou F, Adhikari D et al (2016) Comparison of comorbidity scores in predicting surgical outcomes. Med Care 54:180–187
Flynn DE, Mao D, Yerkovich ST et al (2020) The impact of comorbidities on post-operative complications following colorectal cancer surgery. PLoS ONE 15:e0243995
Heitman SJ (2014) ERCP and mortality. Gastroenterol Hepatol (N Y) 10:752–754
Yu LM, Zhao KJ, Lu B (2018) Use of NSAIDs via the rectal route for the prevention of pancreatitis after ERCP in all-risk patients: an updated meta-analysis. Gastroenterol Res Pract 2018:1027530
Wong LL, Tsai HH (2014) Prevention of post-ERCP pancreatitis. World J Gastrointest Pathophysiol 5:1–10
Dumonceau JM, Andriulli A, Elmunzer BJ (2014) Prophylaxis of post-ERCP pancreatitis: European Society of Gastrointestinal Endoscopy (ESGE) Guideline - updated June 2014. Endoscopy 46:799–815
Acknowledgements
None.
Funding
No funding was received for this study, and the authors have no financial disclosures.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dushyant Singh Dahiya, Abhilash Perisetti, Neil Sharma, Sumant Inamdar, Hemant Goyal, Amandeep Singh, Laura Rotundo, Rajat Garg, Chin-I Cheng, Sailaja Pisipati, Mohammad Al-Haddad, and Madhusudhan Sanaka have no conflict or financial interest to declare.
Ethical approval
The NIS database does not contain any information which can be used to identify patient identity. Hence, our study was exempt from Institutional Review Board (IRB) approval per our institutional guidelines.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dahiya, D.S., Perisetti, A., Sharma, N. et al. Racial disparities in endoscopic retrograde cholangiopancreatography (ERCP) utilization in the United States: are we getting better?. Surg Endosc 37, 421–433 (2023). https://doi.org/10.1007/s00464-022-09535-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09535-w