Abstract
Background
This study is aimed to compare the occurrence of postoperative infections between patients with hepatocellular carcinoma (HCC) undergoing laparoscopic liver resection (LLR) and those undergoing open liver resection (OLR).
Methods
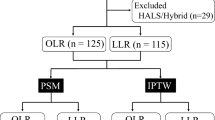
This study included 446 patients who underwent initial curative liver resection for HCC 5 cm or less in size without macroscopic vascular invasion. To adjust for confounding factors between the LLR and OLR groups, propensity score matching and inverse probability weighting (IPW) analysis were performed. The incidence rates of postoperative infection, including incisional surgical site infection (SSI), organ/space SSI, and remote infection (RI), were compared between the two groups.
Results
An imbalance in several confounding variables, including period of surgery, extent of liver resection, difficult location, proximity to a major vessel, tumor size ≥ 3 cm, and multiple tumors, was observed between the two groups in the original cohort. After matching and weighting, the imbalance between the two groups significantly decreased. Compared with OLR, LLR was associated with a lower volume of intraoperative blood loss (140 vs. 350 mL, P < 0.001 in the matched cohort; 120 vs. 320 mL, P < 0.001 in the weighted cohort) and reduced risk of postoperative infection (2.0% vs. 12%, P = 0.015 in the matched cohort; 2.9% vs. 14%, P = 0.005 in the weighted cohort). Of the types of postoperative infections, organ/space SSI and RI were less frequently observed in the LLR group than in the OLR group in the matched cohort (1.0% vs. 6.0%, P = 0.091 for organ/space SSI; 0% vs. 6.0%, P < 0.001 for RI) and in the weighted cohort (1.2% vs. 7.8%, P < 0.001 for organ/space SSI; 0.3% vs. 5.1%, P = 0.009 for RI).
Conclusions
Compared with OLR, LLR for HCC might reduce postoperative infections, including organ/space SSI and RI.


Similar content being viewed by others
References
Fortner JG, Kim DK, Maclean BJ, Barrett MK, Iwatsuki S, Turnbull AD et al (1978) Major hepatic resection for neoplasia: personal experience in 108 patients. Ann Surg 188:363–371
Kenjo A, Miyata H, Gotoh M, Kitagawa Y, Shimada M, Baba H et al (2014) Risk stratification of 7732 hepatectomy cases in 2011 from the National clinical database for Japan. J Am Coll Surg 218:412–422
Kingham TP, Correa-Gallego C, D’Angelica MI, Gönen M, Dematteo RP, Fong Y et al (2015) Hepatic parenchymal preservation surgery: decreasing morbidity and mortality rates in 4152 resections for malignancy. J Am Coll Surg 220:471–479
Gani F, Cerullo M, Amini N, Buettner S, Margonis GA, Sasaki K et al (2017) Frailty as a risk predictor of morbidity and mortality following liver surgery. J Gastrointest Surg 21:822–830
Togo S, Tanaka K, Matsuo K, Nagano Y, Ueda M, Morioka D et al (2007) Duration of antimicrobial prophylaxis in patients undergoing hepatectomy: a prospective randomized controlled trial using flomoxef. J Antimicrob Chemother 59:964–970
Hirokawa F, Hayashi M, Miyamoto Y, Asakuma M, Shimizu T, Komeda K et al (2013) Evaluation of postoperative antibiotic prophylaxis after liver resection: a randomized controlled trial. Am J Surg 206:8–15
Zhou Y-M, Chen Z-Y, Li X-D, Xu D-H, Su X, Li B (2016) Preoperative antibiotic prophylaxis does not reduce the risk of postoperative infectious complications in patients undergoing elective hepatectomy. Dig Dis Sci 61:1707–1713
Sadamori H, Yagi T, Shinoura S, Umeda Y, Yoshida R, Satoh D et al (2013) Risk factors for organ/space surgical site infection after hepatectomy for hepatocellular carcinoma in 359 recent cases. J Hepatobiliary Pancreat Sci 20:186–196
Nanashima A, Arai J, Oyama S, Ishii M, Abo T, Wada H et al (2014) Associated factors with surgical site infections after hepatectomy: predictions and countermeasures by a retrospective cohort study. Int J Surg 12:310–314
Tang H, Lu W, Yang Z, Jiang K, Chen Y, Lu S et al (2017) Risk factors and long-term outcome for postoperative intra-abdominal infection after hepatectomy for hepatocellular carcinoma. Medicine (Baltimore) 96:e6795
Takahara T, Wakabayashi G, Beppu T, Aihara A, Hasegawa K, Gotohda N et al (2015) Long-term and perioperative outcomes of laparoscopic versus open liver resection for hepatocellular carcinoma with propensity score matching: a multi-institutional Japanese study. J Hepatobiliary Pancreat Sci 22:721–727
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS et al (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261:619–629
Ciria R, Cherqui D, Geller DA, Briceno J, Wakabayashi G (2016) Comparative short-term benefits of laparoscopic liver resection: 9000 cases and climbing. Ann Surg 263:761–777
Shehta A, Han HS, Yoon YS, Cho JY, Choi Y (2016) Laparoscopic liver resection for hepatocellular carcinoma in cirrhotic patients: 10-year single-center experience. Surg Endosc 30:638–648
Martinez-Cecilia D, Cipriani F, Shelat V, Ratti F, Tranchart H, Barkhatov L et al (2017) Laparoscopic versus open liver resection for colorectal metastases in elderly and octogenarian patients: a multicenter propensity score based analysis of short- and long-term outcomes. Ann Surg 265:1192–1200
Scuderi V, Barkhatov L, Montalti R, Ratti F, Cipriani F, Pardo F et al (2017) Outcome after laparoscopic and open resections of posterosuperior segments of the liver. Br J Surg 104:751–759
Miyagi S, Nakanishi C, Hara Y, Kamei T, Kawagishi N, Ohuchi N (2015) An evaluation of the safety of pure laparoscopic hepatectomy in patients with liver cirrhosis: investigations including serum albumin and ascites. Surg Laparosc Endosc Percutan Tech 25:209–211
López-Ben S, Palacios O, Codina-Barreras A, Albiol MT, Falgueras L, Castro E et al (2014) Pure laparoscopic liver resection reduces surgical site infections and hospital stay. Results of a case-matched control study in 50 patients. Langenbeck’s Archives of Surgery. 399:307–314
Matsukuma S, Tokumitsu Y, Nakagami Y, Shindo Y, Matsui H, Nakajima M et al (2021) Laparoscopic resection reduces superficial surgical site infection in liver surgery. Surg Endosc 35:7131–7141
Cheung TT, Han H-S, She WH, Chen K-H, Chow PKH, Yoong BK et al (2018) The Asia Pacific consensus statement on laparoscopic liver resection for hepatocellular carcinoma: a report from the 7th Asia-Pacific primary liver cancer expert meeting held in Hong Kong. Liver Cancer 7:28–39
Makuuchi M, Kosuge T, Takayama T, Yamazaki S, Kakazu T, Miyagawa S et al (1993) Surgery for small liver cancers. Semin Surg Oncol 9:298–304
Tanaka S, Takemura S, Shinkawa H, Nishioka T, Hamano G, Kinoshita M et al (2015) Outcomes of pure laparoscopic versus open hepatic resection for hepatocellular carcinoma in cirrhotic patients: a case-control study with propensity score matching. Eur Surg Res 55:291–301
Kinoshita M, Shinkawa H, Kabata D, Tanaka S, Takemura S, Amano R et al (2021) Impact of advancing age on the status and risk of postoperative infections after liver resection. World J Surg 45:3386–3394
Berríos-Torres SI, Umscheid CA, Bratzler DW, Leas B, Stone EC, Kelz RR et al (2017) Centers for disease control and prevention guideline for the prevention of surgical site infection, 2017. JAMA Surg 152:784
Chan KM, Lee CF, Wu TJ, Chou HS, Yu MC, Lee WC et al (2012) Adverse outcomes in patients with postoperative ascites after liver resection for hepatocellular carcinoma. World J Surg 36:392–400
Koch M, Garden OJ, Padbury R, Rahbari NN, Adam R, Capussotti L et al (2011) Bile leakage after hepatobiliary and pancreatic surgery: a definition and grading of severity by the International Study Group of Liver Surgery. Surgery 149:680–688
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Rosenbaum PR, Rubin DB (1984) Reducing bias in observational studies using subclassification on the propensity score. J Am Stat Assoc 79:516–524
Kabata D, Shintani A (2022) Estimating the treatment effect with propensity score when the effect varies by patient characteristics: A case study and simulation. Communications in Statistics: Case Studies, Data Analysis and Applications 1–13
Cho JY, Han H-S, Yoon Y-S, Shin S-H (2008) Experiences of laparoscopic liver resection including lesions in the posterosuperior segments of the liver. Surg Endosc 22:2344–2349
Stuart EA (2010) Matching methods for causal inference: a review and a look forward. Stat Sci 25:1–21
Imai K, Ratkovic M (2014) Covariate balancing propensity score. J Royal Stat Soc 76:243–263
Austin PC, Stuart EA (2015) Moving towards best practice when using inverse probability of treatment weighting (IPTW) using the propensity score to estimate causal treatment effects in observational studies. Stat Med 34:3661–3679
Takesue Y, Kusachi S, Mikamo H, Sato J, Watanabe A, Kiyota H et al (2018) Antimicrobial susceptibility of common pathogens isolated from postoperative intra-abdominal infections in Japan. J Infect Chemother 24:330–340
Nishizaki T, Matsumata T, Yanaga K, Shimada M, Higashi H, Sugimachi K (1993) Open and closed suction drainage after hepatic resection. Surg Today 23:871–874
Shirata C, Hasegawa K, Kokudo T, Arita J, Akamatsu N, Kaneko J et al (2018) Surgical site infection after hepatectomy for hepatocellular carcinoma. Dig Surg 35:204–211
Jildeh TR, Okoroha KR, Marshall NE, Abdul-Hak A, Zeni F, Moutzouros V (2018) Infection and rerupture after surgical repair of achilles tendons. Orthop J Sports Med 6:232596711877430
Matsuo Y, Nomi T, Hokuto D, Yoshikawa T, Kamitani N, Sho M (2020) Pulmonary complications after laparoscopic liver resection. Surg Endosc 35:1659–1666
Fuks D, Cauchy F, Ftériche S, Nomi T, Schwarz L, Dokmak S et al (2016) Laparoscopy decreases pulmonary complications in patients undergoing major liver resection. Ann Surg 263:353–361
Alkaaki A, Al-Radi OO, Khoja A, Alnawawi A, Alnawawi A, Maghrabi A et al (2019) Surgical site infection following abdominal surgery: a prospective cohort study. Can J Surg 62:111–117
Caroff DA, Chan C, Kleinman K, Calderwood MS, Wolf R, Wick EC et al (2019) Association of open approach vs laparoscopic approach with risk of surgical site infection after colon surgery. JAMA Netw Open 2:e1913570
Acknowledgements
This work was supported by Health, Labour and Welfare Policy Research Grants from the Ministry of Health, Labour, and Welfare of Japan (Policy Research for Hepatitis Measures [H30-Kansei-Shitei-003]).
Funding
This work was supported by Health, Labour and Welfare Policy Research Grants from the Ministry of Health, Labour, and Welfare of Japan (Policy Research for Hepatitis Measures [H30-Kansei-Shitei-003]).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Daisuke Shirai, Hiroji Shinkawa, Daijiro Kabata, Shigekazu Takemura, Shogo Tanaka, Ryosuke Amano, Kenjiro Kimura, Go Ohira, Kohei Nishio, Jun Tauchi, Masahiko Kinoshita, and Shoji Kubo have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Shirai, D., Shinkawa, H., Kabata, D. et al. Laparoscopic liver resection reduces postoperative infection in patients with hepatocellular carcinoma: a propensity score-based analysis. Surg Endosc 36, 9194–9203 (2022). https://doi.org/10.1007/s00464-022-09403-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09403-7