Abstract
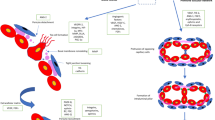
Brain arteriovenous malformation (BAVM) is a rare but serious cerebrovascular disease whose pathogenesis has not been fully elucidated. Studies have found that epigenetic regulation, genetic variation and their signaling pathways, immune inflammation, may be the cause of BAVM the main reason. This review comprehensively analyzes the key pathways and inflammatory factors related to BAVMs, and explores their interplay with epigenetic regulation and genetics. Studies have found that epigenetic regulation such as DNA methylation, non-coding RNAs and m6A RNA modification can regulate endothelial cell proliferation, apoptosis, migration and damage repair of vascular malformations through different target gene pathways. Gene defects such as KRAS, ACVRL1 and EPHB4 lead to a disordered vascular environment, which may promote abnormal proliferation of blood vessels through ERK, NOTCH, mTOR, Wnt and other pathways. PDGF-B and PDGFR-β were responsible for the recruitment of vascular adventitial cells and smooth muscle cells in the extracellular matrix environment of blood vessels, and played an important role in the pathological process of BAVM. Recent single-cell sequencing data revealed the diversity of various cell types within BAVM, as well as the heterogeneous expression of vascular-associated antigens, while neutrophils, macrophages and cytokines such as IL-6, IL-1, TNF-α, and IL-17A in BAVM tissue were significantly increased. Currently, there are no specific drugs targeting BAVMs, and biomarkers for BAVM formation, bleeding, and recurrence are lacking clinically. Therefore, further studies on molecular biological mechanisms will help to gain insight into the pathogenesis of BAVM and develop potential therapeutic strategies.




Similar content being viewed by others
References
Al-Olabi L, Polubothu S, Dowsett K, Andrews KA, Stadnik P, Joseph AP, Knox R, Pittman A, Clark G, Baird W, Bulstrode N, Glover M, Gordon K, Hargrave D, Huson SM, Jacques TS, James G, Kondolf H, Kangesu L, Keppler-Noreuil KM, Khan A, Lindhurst MJ, Lipson M, Mansour S, O’Hara J, Mahon C, Mosica A, Moss C, Murthy A, Ong J, Parker VE, Rivière J-B, Sapp JC, Sebire NJ, Shah R, Sivakumar B, Thomas A, Virasami A, Waelchli R, Zeng Z, Biesecker LG, Barnacle A, Topf M, Semple RK, Patton EE, Kinsler VA (2018) Mosaic RAS/MAPK variants cause sporadic vascular malformations which respond to targeted therapy. J Clin Invest 128(4):1496–1508
Al-Sadi O, Schulze-Tanzil G, Kohl B, Lohan A, Lemke M, Ertel W, John T (2011) Tenocytes, pro-inflammatory cytokines and leukocytes: a relationship? Muscles Ligaments Tendons J 1(3):68–76
Amyere M, Revencu N, Helaers R, Pairet E, Baselga E, Cordisco M, Chung W, Dubois J, Lacour J-P, Martorell L, Mazereeuw-Hautier J, Pyeritz RE, Amor DJ, Bisdorff A, Blei F, Bombei H, Dompmartin A, Brooks D, Dupont J, González-Enseñat MA, Frieden I, Gérard M, Kvarnung M, Hanson-Kahn AK, Hudgins L, Léauté-Labrèze C, McCuaig C, Metry D, Parent P, Paul C, Petit F, Phan A, Quere I, Salhi A, Turner A, Vabres P, Vicente A, Wargon O, Watanabe S, Weibel L, Wilson A, Willing M, Mulliken JB, Boon LM, Vikkula M (2017) Germline loss-of-function mutations in EPHB4 cause a second form of capillary malformation-arteriovenous malformation (CM-AVM2) deregulating RAS-MAPK signaling. Circulation 136(11):1037–1048
Arango D, Sturgill D, Alhusaini N, Dillman AA, Sweet TJ, Hanson G, Hosogane M, Sinclair WR, Nanan KK, Mandler MD, Fox SD, Zengeya TT, Andresson T, Meier JL, Coller J, Oberdoerffer S (2018) Acetylation of cytidine in mRNA promotes translation efficiency. Cell. https://doi.org/10.1016/j.cell.2018.10.030
Ardelt AA, McCullough LD, Korach KS, Wang MM, Munzenmaier DH, Hurn PD (2005) Estradiol regulates angiopoietin-1 mRNA expression through estrogen receptor-alpha in a rodent experimental stroke model. Stroke 36(2):337–341
Barbosa Do Prado L, Han C, Oh SP, Su H (2019) Recent advances in basic research for brain arteriovenous malformation. Int J Mol Sci. https://doi.org/10.3390/ijms20215324
Bendjilali N, Kim H, Weinsheimer S, Guo DE, Kwok P-Y, Zaroff JG, Sidney S, Lawton MT, McCulloch CE, Koeleman BPC, Klijn CJM, Young WL, Pawlikowska L (2013) A genome-wide investigation of copy number variation in patients with sporadic brain arteriovenous malformation. PLoS ONE 8(10):e71434
Bilguvar K, Yasuno K, Niemelä M, Ruigrok YM, von Und Zu Fraunberg M, van Duijn CM, van den Berg LH, Mane S, Mason CE, Choi M, Gaál E, Bayri Y, Kolb L, Arlier Z, Ravuri S, Ronkainen A, Tajima A, Laakso A, Hata A, Kasuya H, Koivisto T, Rinne J, Ohman J, Breteler MMB, Wijmenga C, State MW, Rinkel GJE, Hernesniemi J, Jääskeläinen JE, Palotie A, Inoue I, Lifton RP, Günel M (2008) Susceptibility loci for intracranial aneurysm in European and Japanese populations. Nat Genet 40(12):1472–1477
Bokar JA, Rath-Shambaugh ME, Ludwiczak R, Narayan P, Rottman F (1994) Characterization and partial purification of mRNA N6-adenosine methyltransferase from HeLa cell nuclei. Internal mRNA methylation requires a multisubunit complex. J Biol Chem 269(26):17697–17704
Bokar JA, Shambaugh ME, Polayes D, Matera AG, Rottman FM (1997) Purification and cDNA cloning of the AdoMet-binding subunit of the human mRNA (N6-adenosine)-methyltransferase. RNA 3(11):1233–1247
Briot A, Iruela-Arispe ML (2015) Blockade of specific NOTCH ligands: a new promising approach in cancer therapy. Cancer Discov 5(2):112–114
Chen Y, Pawlikowska L, Yao JS, Shen F, Zhai W, Achrol AS, Lawton MT, Kwok PY, Yang GY, Young WL (2006) Interleukin-6 involvement in brain arteriovenous malformations. Ann Neurol 59(1):72–80
Chen Y, Zhu W, Bollen AW, Lawton MT, Barbaro NM, Dowd CF, Hashimoto T, Yang G-Y, Young WL (2008) Evidence of inflammatory cell involvement in brain arteriovenous malformations. Neurosurgery. https://doi.org/10.1227/01.neu.0000333306.64683.b5
Chen H, Gu Y, Wu W, Chen D, Li P, Fan W, Lu D, Zhao F, Qiao N, Qiu H, Fu C, Mao Y, Zhao Y (2011) Polymorphisms of the vascular endothelial growth factor A gene and susceptibility to sporadic brain arteriovenous malformation in a Chinese population. J Clin Neurosci 18(4):549–553
Chen W, Guo Y, Walker EJ, Shen F, Jun K, Oh SP, Degos V, Lawton MT, Tihan T, Davalos D, Akassoglou K, Nelson J, Pile-Spellman J, Su H, Young WL (2013) Reduced mural cell coverage and impaired vessel integrity after angiogenic stimulation in the Alk1-deficient brain. Arterioscler Thromb Vasc Biol 33(2):305–310
Chen X, Liu Y, Zhou S, Nie S, Lin Z, Zhou C, Sun J, Gao X, Huang Y (2019) Methylation of the CDKN2A gene increases the risk of brain arteriovenous malformations. J Mol Neurosci 69(2):316–323
Chen N, Peng C, Li D (2022) Epigenetic underpinnings of inflammation: a key to unlock the tumor microenvironment in glioblastoma. Front Immunol 13:869307
Choi H, Kim B-G, Kim YH, Lee S-J, Lee YJ, Oh SP (2023) BMP10 functions independently from BMP9 for the development of a proper arteriovenous network. Angiogenesis 26(1):167–186
Claesson-Welsh L, Welsh M (2013) VEGFA and tumour angiogenesis. J Intern Med 273(2):114–127
Conrad DF, Pinto D, Redon R, Feuk L, Gokcumen O, Zhang Y, Aerts J, Andrews TD, Barnes C, Campbell P, Fitzgerald T, Hu M, Ihm CH, Kristiansson K, Macarthur DG, Macdonald JR, Onyiah I, Pang AWC, Robson S, Stirrups K, Valsesia A, Walter K, Wei J, Tyler-Smith C, Carter NP, Lee C, Scherer SW, Hurles ME (2010) Origins and functional impact of copy number variation in the human genome. Nature 464(7289):704–712
Dardiotis E, Aloizou AM, Markoula S, Siokas V, Tsarouhas K, Tzanakakis G, Libra M, Kyritsis AP, Brotis AG, Aschner M, Gozes I, Bogdanos DP, Spandidos DA, Mitsias PD, Tsatsakis A (2019) Cancer-associated stroke: pathophysiology, detection and management (Review). Int J Oncol 54(3):779–796
David L, Feige J-J, Bailly S (2009) Emerging role of bone morphogenetic proteins in angiogenesis. Cytokine Growth Factor Rev 20(3):203–212
Deng Y, Chen D, Gao F, Lv H, Zhang G, Sun X, Liu L, Mo D, Ma N, Song L, Huo X, Yan T, Zhang J, Luo Y, Miao Z (2020) Silencing of long non-coding RNA GAS5 suppresses neuron cell apoptosis and nerve injury in ischemic stroke through inhibiting DNMT3B-dependent MAP4K4 methylation. Transl Stroke Res 11(5):950–966
Dinicola S, Proietti S, Cucina A, Bizzarri M, Fuso A (2017) Alpha-lipoic acid downregulates IL-1β and IL-6 by DNA hypermethylation in SK-N-BE neuroblastoma cells. Antioxidants (basel). https://doi.org/10.3390/antiox6040074
Dock H, Theodorsson A, Theodorsson E (2015) DNA methylation inhibitor zebularine confers stroke protection in ischemic rats. Transl Stroke Res 6(4):296–300
Fan Y, Lv X, Chen Z, Peng Y, Zhang M (2023) m6A methylation: critical roles in aging and neurological diseases. Front Mol Neurosci 16:1102147
Fish JE, Flores Suarez CP, Boudreau E, Herman AM, Gutierrez MC, Gustafson D, DiStefano PV, Cui M, Chen Z, De Ruiz KB, Schexnayder TS, Ward CS, Radovanovic I, Wythe JD (2020) Somatic gain of KRAS function in the endothelium is sufficient to cause vascular malformations that require MEK but not PI3K signaling. Circ Res 127(6):727–743
Florian IA, Timiș TL, Ungureanu G, Florian IS, Bălașa A, Berindan-Neagoe I (2020) Deciphering the vascular labyrinth: role of microRNAs and candidate gene SNPs in brain AVM development—literature review. Neurol Res 42(12):1043–1054
Florian IA, Beni L, Moisoiu V, Timis TL, Florian IS, Balașa A, Berindan-Neagoe I (2021a) “De Novo” brain AVMs-hypotheses for development and a systematic review of reported cases. Medicina (kaunas). https://doi.org/10.3390/medicina57030201
Florian IA, Buruiana A, Timis TL, Susman S, Florian IS, Balasa A, Berindan-Neagoe I (2021b) An insight into the microRNAs associated with arteriovenous and cavernous malformations of the brain. Cells. https://doi.org/10.3390/cells10061373
Folkman J (2007) Angiogenesis: an organizing principle for drug discovery? Nat Rev Drug Discov 6(4):273–286
Fu W, Huo R, Yan Z, Xu H, Li H, Jiao Y, Wang L, Weng J, Wang J, Wang S, Cao Y, Zhao J (2020) Mesenchymal behavior of the endothelium promoted by SMAD6 downregulation is associated with brain arteriovenous malformation microhemorrhage. Stroke 51(7):2197–2207
Fukuda K, Majumdar M, Masoud H, Nguyen T, Honarmand A, Shaibani A, Ansari S, Tan LA, Chen M (2017) Multicenter assessment of morbidity associated with cerebral arteriovenous malformation hemorrhages. J Neurointerv Surg 9(7):664–668
Gale NW, Dominguez MG, Noguera I, Pan L, Hughes V, Valenzuela DM, Murphy AJ, Adams NC, Lin HC, Holash J, Thurston G, Yancopoulos GD (2004) Haploinsufficiency of delta-like 4 ligand results in embryonic lethality due to major defects in arterial and vascular development. Proc Natl Acad Sci U S A 101(45):15949–15954
Gallione CJ, Repetto GM, Legius E, Rustgi AK, Schelley SL, Tejpar S, Mitchell G, Drouin E, Westermann CJJ, Marchuk DA (2004) A combined syndrome of juvenile polyposis and hereditary haemorrhagic telangiectasia associated with mutations in MADH4 (SMAD4). Lancet 363(9412):852–859
Germans MR, Sun W, Sebök M, Keller A, Regli L (2022) Molecular signature of brain arteriovenous malformation hemorrhage: a systematic review. World Neurosurg 157:143–151
Goumans M-J, Liu Z, ten Dijke P (2009) TGF-beta signaling in vascular biology and dysfunction. Cell Res 19(1):116–127
Gross BA, Du R (2013) Natural history of cerebral arteriovenous malformations: a meta-analysis. J Neurosurg 118(2):437–443
Hakki S, Robinson EJ, Robson MG (2022) Circulating Interleukin-6 and CD16 positive monocytes increase following angioplasty of an arteriovenous fistula. Sci Rep 12(1):1427
Heard E, Martienssen RA (2014) Transgenerational epigenetic inheritance: myths and mechanisms. Cell. https://doi.org/10.1016/j.cell.2014.02.045
Hong T, Yan Y, Li J, Radovanovic I, Ma X, Shao YW, Yu J, Ma Y, Zhang P, Ling F, Huang S, Zhang H, Wang Y (2019) High prevalence of KRAS/BRAF somatic mutations in brain and spinal cord arteriovenous malformations. Brain 142(1):23–34
Hong T, Xiao X, Ren J, Cui B, Zong Y, Zou J, Kou Z, Jiang N, Meng G, Zeng G, Shan Y, Wu H, Chen Z, Liang J, Xiao X, Tang J, Wei Y, Ye M, Sun L, Li G, Hu P, Hui R, Zhang H, Wang Y (2021) Somatic MAP3K3 and PIK3CA mutations in sporadic cerebral and spinal cord cavernous malformations. Brain 144(9):2648–2658
Huang J, Song J, Qu M, Wang Y, An Q, Song Y, Yan W, Wang B, Wang X, Zhang S, Chen X, Zhao B, Liu P, Xu T, Zhang Z, Greenberg DA, Wang Y, Gao P, Zhu W, Yang G-Y (2017) MicroRNA-137 and microRNA-195* inhibit vasculogenesis in brain arteriovenous malformations. Ann Neurol 82(3):371–384
Huo R, Fu W, Li H, Jiao Y, Yan Z, Wang L, Wang J, Wang S, Cao Y, Zhao J (2019) RNA sequencing reveals the activation of Wnt signaling in low flow rate brain arteriovenous malformations. J Am Heart Assoc 8(12):e012746
Huo R, Yang Y, Sun Y, Zhou Q, Zhao S, Mo Z, Xu H, Wang J, Weng J, Jiao Y, Zhang J, He Q, Wang S, Zhao J, Wang J, Cao Y (2023) Endothelial hyperactivation of mutant MAP3K3 induces cerebral cavernous malformation enhanced by PIK3CA GOF mutation. Angiogenesis 26(2):295–312
Hwan Kim Y, Vu P-N, Choe S-W, Jeon C-J, Arthur HM, Vary CPH, Lee YJ, Oh SP (2020) Overexpression of activin receptor-like kinase 1 in endothelial cells suppresses development of arteriovenous malformations in mouse models of hereditary hemorrhagic telangiectasia. Circ Res 127(9):1122–1137
Illi B, Nanni S, Scopece A, Farsetti A, Biglioli P, Capogrossi MC, Gaetano C (2003) Shear stress-mediated chromatin remodeling provides molecular basis for flow-dependent regulation of gene expression. Circ Res 93(2):155–161
Jaenisch R, Bird A (2003) Epigenetic regulation of gene expression: how the genome integrates intrinsic and environmental signals. Nat Genet 33(Suppl):245–254
Jain RK (2003) Molecular regulation of vessel maturation. Nat Med 9(6):685–693
Jeltsch M, Leppänen V-M, Saharinen P, Alitalo K (2013) Receptor tyrosine kinase-mediated angiogenesis. Cold Spring Harb Perspect Biol. https://doi.org/10.1101/cshperspect.a009183
Jeong JH, Ojha U, Lee YM (2021) Pathological angiogenesis and inflammation in tissues. Arch Pharm Res 44(1):1–15
Kar S, Bali KK, Baisantry A, Geffers R, Hartmann C, Samii A, Bertalanffy H (2018) Genome-wide sequencing reveals small nucleolar RNAs downregulated in cerebral cavernous malformations. Cell Mol Neurobiol 38(7):1369–1382
Karlsson B, Jokura H, Yang HC, Yamamoto M, Martinez R, Kawagishi J, Guo WY, Beute G, Chung WY, Soderman M, Yeo TT (2020) Clinical outcome following cerebral AVM hemorrhage. Acta Neurochir (wien) 162(7):1759–1766
Kawasaki J, Aegerter S, Fevurly RD, Mammoto A, Mammoto T, Sahin M, Mably JD, Fishman SJ, Chan J (2014) RASA1 functions in EPHB4 signaling pathway to suppress endothelial mTORC1 activity. J Clin Invest 124(6):2774–2784
Kim YH, Hu H, Guevara-Gallardo S, Lam MTY, Fong S-Y, Wang RA (2008) Artery and vein size is balanced by Notch and ephrin B2/EphB4 during angiogenesis. Development 135(22):3755–3764
Kim H, Hysi PG, Pawlikowska L, Poon A, Burchard EG, Zaroff JG, Sidney S, Ko NU, Achrol AS, Lawton MT, McCulloch CE, Kwok P-Y, Young WL (2009) Common variants in interleukin-1-Beta gene are associated with intracranial hemorrhage and susceptibility to brain arteriovenous malformation. Cerebrovasc Dis 27(2):176–182
Kopan R, Ilagan MXG (2009) The canonical Notch signaling pathway: unfolding the activation mechanism. Cell 137(2):216–233
Krebs LT, Shutter JR, Tanigaki K, Honjo T, Stark KL, Gridley T (2004) Haplo insufficient lethality and formation of arteriovenous malformations in Notch pathway mutants. Genes Dev 18(20):2469–2473
Kremer PHC, Koeleman BPC, Pawlikowska L, Weinsheimer S, Bendjilali N, Sidney S, Zaroff JG, Rinkel GJE, van den Berg LH, Ruigrok YM, de Kort GAP, Veldink JH, Kim H, Klijn CJM (2015) Evaluation of genetic risk loci for intracranial aneurysms in sporadic arteriovenous malformations of the brain. J Neurol Neurosurg Psychiatry 86(5):524–529
Krithika S, Sumi S (2021) Neurovascular inflammation in the pathogenesis of brain arteriovenous malformations. J Cell Physiol 236(7):4841–4856
Lawton MT, Rutledge WC, Kim H, Stapf C, Whitehead KJ, Li DY, Krings T, terBrugge K, Kondziolka D, Morgan MK, Moon K, Spetzler RF (2015) Brain arteriovenous malformations. Nat Rev Dis Primers 1:15008
Lee JS, Cho HG, Ryu JY, Oh EJ, Kim HM, Kwak S, Lee S-J, Lee J, Lee SY, Huh S, Kim JY, Chung HY (2022) Hypoxia promotes angiogenic effect in extracranial arteriovenous malformation endothelial cells. Int J Mol Sci. https://doi.org/10.3390/ijms23169109
Li A, Dubey S, Varney ML, Dave BJ, Singh RK (2003) IL-8 directly enhanced endothelial cell survival, proliferation, and matrix metalloproteinases production and regulated angiogenesis. J Immunol 170(6):3369–3376
Li X, Wang R, Wang X, Xue X, Ran D, Wang S (2013) Relevance of IL-6 and MMP-9 to cerebral arteriovenous malformation and hemorrhage. Mol Med Rep 7(4):1261–1266
Li X, Lin F, Wu J, Wang S (2018) LncRNAs expression signatures of human brain arteriovenous malformation revealed by microarray. Medicine (baltimore) 97(30):e11308
Li H, Nam Y, Huo R, Fu W, Jiang B, Zhou Q, Song D, Yang Y, Jiao Y, Weng J, Yan Z, Di L, Li J, Wang J, Xu H, Wang S, Zhao J, Wen Z, Wang J, Cao Y (2021) De Novo germline and somatic variants convergently promote endothelial-to-mesenchymal transition in simplex brain arteriovenous malformation. Circ Res 129(9):825–839
Liu J, Yue Y, Han D, Wang X, Fu Y, Zhang L, Jia G, Yu M, Lu Z, Deng X, Dai Q, Chen W, He C (2014) A METTL3-METTL14 complex mediates mammalian nuclear RNA N6-adenosine methylation. Nat Chem Biol 10(2):93–95
Liu Y, Wu X, Nie S, Zhou S, Xiao S, Gao X, Lin Z, Sun J, Huang Y (2020) Methylation of phospholipase A2 group VII gene is associated with brain arteriovenous malformations in Han Chinese populations. J Mol Neurosci 70(7):1056–1063
Liu C, Wang X, Yang S, Cao S (2023) Research progress of m6A RNA methylation in skin diseases. Biomed Res Int 2023:3091204
Luna-Zurita L, Prados B, Grego-Bessa J, Luxán G, del Monte G, Benguría A, Adams RH, Pérez-Pomares JM, de la Pompa JL (2010) Integration of a Notch-dependent mesenchymal gene program and Bmp2-driven cell invasiveness regulates murine cardiac valve formation. J Clin Invest 120(10):3493–3507
Margariti A, Zampetaki A, Xiao Q, Zhou B, Karamariti E, Martin D, Yin X, Mayr M, Li H, Zhang Z, De Falco E, Hu Y, Cockerill G, Xu Q, Zeng L (2010) Histone deacetylase 7 controls endothelial cell growth through modulation of beta-catenin. Circ Res 106(7):1202–1211
Marín-Ramos NI, Thein TZ, Ghaghada KB, Chen TC, Giannotta SL, Hofman FM (2020) miR-18a inhibits BMP4 and HIF-1α normalizing brain arteriovenous malformations. Circ Res 127(9):e210–e231
Matouk CC, Marsden PA (2008) Epigenetic regulation of vascular endothelial gene expression. Circ Res 102(8):873–887
Morales-Valero SF, Bortolotti C, Sturiale C, Lanzino G (2014) Are parenchymal AVMs congenital lesions? Neurosurg Focus 37(3):2
Mottet D, Bellahcène A, Pirotte S, Waltregny D, Deroanne C, Lamour V, Lidereau R, Castronovo V (2007) Histone deacetylase 7 silencing alters endothelial cell migration, a key step in angiogenesis. Circ Res 101(12):1237–1246
Mouchtouris N, Jabbour PM, Starke RM, Hasan DM, Zanaty M, Theofanis T, Ding D, Tjoumakaris SI, Dumont AS, Ghobrial GM, Kung D, Rosenwasser RH, Chalouhi N (2015) Biology of cerebral arteriovenous malformations with a focus on inflammation. J Cereb Blood Flow Metab 35(2):167–175
Mouillesseaux KP, Wiley DS, Saunders LM, Wylie LA, Kushner EJ, Chong DC, Citrin KM, Barber AT, Park Y, Kim J-D, Samsa LA, Kim J, Liu J, Jin S-W, Bautch VL (2016) Notch regulates BMP responsiveness and lateral branching in vessel networks via SMAD6. Nat Commun 7:13247
Murphy PA, Lu G, Shiah S, Bollen AW, Wang RA (2009) Endothelial Notch signaling is upregulated in human brain arteriovenous malformations and a mouse model of the disease. Lab Invest 89(9):971–982
Murphy PA, Kim TN, Lu G, Bollen AW, Schaffer CB, Wang RA (2012) Notch4 normalization reduces blood vessel size in arteriovenous malformations. Sci Transl Med 4(117):117ra8
Nadeem T, Bogue W, Bigit B, Cuervo H (2020) Deficiency of Notch signaling in pericytes results in arteriovenous malformations. JCI Insight 5(21)
Nagai Y, Anan M, Fujiki M (2020) Cerebral arteriovenous malformations as acquired lesions: case reports and review of the literature. J Stroke Cerebrovasc Dis 29(10):105157
Nakayama I, Shinozaki E, Matsushima T, Wakatsuki T, Ogura M, Ichimura T, Ozaka M, Takahari D, Suenaga M, Chin K, Mizunuma N, Yamaguchi K (2017) Retrospective study of RAS/PIK3CA/BRAF tumor mutations as predictors of response to first-line chemotherapy with bevacizumab in metastatic colorectal cancer patients. BMC Cancer 17(1):38
Niessen K, Karsan A (2008) Notch signaling in cardiac development. Circ Res 102(10):1169–1181
Nikolaev SI, Vetiska S, Bonilla X, Boudreau E, Jauhiainen S, Rezai Jahromi B, Khyzha N, DiStefano PV, Suutarinen S, Kiehl T-R, Mendes Pereira V, Herman AM, Krings T, Andrade-Barazarte H, Tung T, Valiante T, Zadeh G, Tymianski M, Rauramaa T, Ylä-Herttuala S, Wythe JD, Antonarakis SE, Frösen J, Fish JE, Radovanovic I (2018) Somatic activating KRAS mutations in arteriovenous malformations of the brain. N Engl J Med 378(3):250–261
Numata S, Ye T, Herman M, Lipska BK (2014) DNA methylation changes in the postmortem dorsolateral prefrontal cortex of patients with schizophrenia. Front Genet 5:280
Pan P, Weinsheimer S, Cooke D, Winkler E, Abla A, Kim H, Su H (2021) Review of treatment and therapeutic targets in brain arteriovenous malformation. J Cereb Blood Flow Metab 41(12):3141–3156
Pandolfini L, Barbieri I, Bannister AJ, Hendrick A, Andrews B, Webster N, Murat P, Mach P, Brandi R, Robson SC, Migliori V, Alendar A, d’Onofrio M, Balasubramanian S, Kouzarides T (2019) METTL1 promotes let-7 microRNA processing via m7G methylation. Mol Cell. https://doi.org/10.1016/j.molcel.2019.03.040
Pardali E, Ten Dijke P (2012) TGFβ signaling and cardiovascular diseases. Int J Biol Sci 8(2):195–213
Park H, Koh EJ, Lee EJ, Cheon J-E, Kim S-K (2021a) An acquired cerebral arteriovenous malformation after brain abscess treatment: case report and a review of the literature. Childs Nerv Syst 37(9):2923–2926
Park ES, Kim S, Huang S, Yoo JY, Korbelin J, Lee TJ, Kaur B, Dash PK, Chen PR, Kim E (2021b) Selective endothelial hyperactivation of oncogenic KRAS induces brain arteriovenous malformations in mice. Ann Neurol 89(5):926–941
Patan S (2000) Vasculogenesis and angiogenesis as mechanisms of vascular network formation, growth and remodeling. J Neurooncol 50(1–2):1–15.
Pawlikowska L, Tran MN, Achrol AS, McCulloch CE, Ha C, Lind DL, Hashimoto T, Zaroff J, Lawton MT, Marchuk DA, Kwok P-Y, Young WL (2004) Polymorphisms in genes involved in inflammatory and angiogenic pathways and the risk of hemorrhagic presentation of brain arteriovenous malformations. Stroke 35(10):2294–2300
Ping X-L, Sun B-F, Wang L, Xiao W, Yang X, Wang W-J, Adhikari S, Shi Y, Lv Y, Chen Y-S, Zhao X, Li A, Yang Y, Dahal U, Lou X-M, Liu X, Huang J, Yuan W-P, Zhu X-F, Cheng T, Zhao Y-L, Wang X, Rendtlew Danielsen JM, Liu F, Yang Y-G (2014) Mammalian WTAP is a regulatory subunit of the RNA N6-methyladenosine methyltransferase. Cell Res 24(2):177–189
Portela A, Esteller M (2010) Epigenetic modifications and human disease. Nat Biotechnol 28(10):1057–1068
Rawlik K, Rowlatt A, Tenesa A (2016) Imputation of DNA methylation levels in the brain implicates a risk factor for Parkinson’s disease. Genetics 204(2):771–781
Rees E, Kirov G (2021) Copy number variation and neuropsychiatric illness. Curr Opin Genet Dev 68:57–63
Ren J, Huang Y, Ren Y, Tu T, Qiu B, Ai D, Bi Z, Bai X, Li F, Li JL, Chen XJ, Feng Z, Guo Z, Lei J, Tian A, Cui Z, Lindner V, Adams RH, Wang Y, Zhao F, Korbelin J, Sun W, Wang Y, Zhang H, Hong T, Ge WP (2023) Somatic variants of MAP3K3 are sufficient to cause cerebral and spinal cord cavernous malformations. Brain. https://doi.org/10.1093/brain/awad104
Ruiz S, Zhao H, Chandakkar P, Papoin J, Choi H, Nomura-Kitabayashi A, Patel R, Gillen M, Diao L, Chatterjee PK, He M, Al-Abed Y, Wang P, Metz CN, Oh SP, Blanc L, Campagne F, Marambaud P (2020) Correcting Smad1/5/8, mTOR, and VEGFR2 treats pathology in hereditary hemorrhagic telangiectasia models. J Clin Invest 130(2):942–957
Santos R, Aguilar-Salinas P, Entwistle JJ, Aldana PR, Beier AD, Hanel RA (2018) De Novo arteriovenous malformation in a pediatric patient: case report and review of the literature. World Neurosurg 111:341–345
Sati L, Soygur B, Goksu E, Bassorgun CI, McGrath J (2021) CTCFL expression is associated with cerebral vascular abnormalities. Tissue Cell 72:101528
Scimone C, Granata F, Longo M, Mormina E, Turiaco C, Caragliano AA, Donato L, Sidoti A, D’Angelo R (2020) Germline mutation enrichment in pathways controlling endothelial cell homeostasis in patients with brain arteriovenous malformation: implication for molecular diagnosis. Int J Mol Sci. https://doi.org/10.3390/ijms21124321
Shen Q, Zhang Q, Shi Y, Shi Q, Jiang Y, Gu Y, Li Z, Li X, Zhao K, Wang C, Li N, Cao X (2018) Tet2 promotes pathogen infection-induced myelopoiesis through mRNA oxidation. Nature 554(7690):123–127
Singh AK, Kilari S, Cai C, Misra S (2022) Bindarit encapsulated nanoparticles prevent venous neointimal hyperplasia and restenosis in a murine angioplasty model. Transl Res 248:68–86
Sohn SJ, Sarvis BK, Cado D, Winoto A (2002) ERK5 MAPK regulates embryonic angiogenesis and acts as a hypoxia-sensitive repressor of vascular endothelial growth factor expression. J Biol Chem 277(45):43344–43351
Spiegler S, Rath M, Paperlein C, Felbor U (2018) Cerebral cavernous malformations: an update on prevalence, molecular genetic analyses, and genetic counselling. Mol Syndromol 9(2):60–69
Stanzione R, Cotugno M, Bianchi F, Marchitti S, Forte M, Volpe M, Rubattu S (2020) Pathogenesis of ischemic stroke: role of epigenetic mechanisms. Genes (basel). https://doi.org/10.3390/genes11010089
Storer KP, Tu J, Karunanayaka A, Morgan MK, Stoodley MA (2008) Inflammatory molecule expression in cerebral arteriovenous malformations. J Clin Neurosci 15(2):179–184
Sturiale CL, Puca A, Sebastiani P, Gatto I, Albanese A, Di Rocco C, Maira G, Pola R (2013) Single nucleotide polymorphisms associated with sporadic brain arteriovenous malformations: where do we stand? Brain 136(Pt 2):665–681
Su H, Kim H, Pawlikowska L, Kitamura H, Shen F, Cambier S, Markovics J, Lawton MT, Sidney S, Bollen AW, Kwok P-Y, Reichardt L, Young WL, Yang G-Y, Nishimura SL (2010) Reduced expression of integrin alphavbeta8 is associated with brain arteriovenous malformation pathogenesis. Am J Pathol 176(2):1018–1027
Tanaka T, Narazaki M, Kishimoto T (2014) IL-6 in inflammation, immunity, and disease. Cold Spring Harb Perspect Biol 6(10):a016295
Taniguchi R, Ohashi Y, Lee JS, Hu H, Gonzalez L, Zhang W, Langford J, Matsubara Y, Yatsula B, Tellides G, Fahmy TM, Hoshina K, Dardik A (2022) Endothelial cell TGF-β (transforming growth factor-beta) signaling regulates venous adaptive remodeling to improve arteriovenous fistula patency. Arterioscler Thromb Vasc Biol 42(7):868–883
Thomas JM, Surendran S, Abraham M, Rajavelu A, Kartha CC (2016) Genetic and epigenetic mechanisms in the development of arteriovenous malformations in the brain. Clin Epigenet 8:78
Thomas JM, Surendran S, Abraham M, Sasankan D, Bhaadri S, Rajavelu A, Kartha CC (2018) Gene expression analysis of nidus of cerebral arteriovenous malformations reveals vascular structures with deficient differentiation and maturation. PLoS ONE 13(6):e0198617
Thomas JM, Sasankan D, Abraham M, Surendran S, Kartha CC, Rajavelu A (2022) DNA methylation signatures on vascular differentiation genes are aberrant in vessels of human cerebral arteriovenous malformation nidus. Clin Epigenet 14(1):127
Tu J, Li Y, Hu Z (2014) Notch1 and 4 signaling responds to an increasing vascular wall shear stress in a rat model of arteriovenous malformations. Biomed Res Int 2014:368082
Venugopal V, Sumi S (2022) Molecular biomarkers and drug targets in brain arteriovenous and cavernous malformations: where are we? Stroke 53(1):279–289
Walcott BP (2014) BMP signaling modulation attenuates cerebral arteriovenous malformation formation in a vertebrate model. J Cereb Blood Flow Metab 34(10):1688–1694
Walcott BP, Winkler EA, Zhou S, Birk H, Guo D, Koch MJ, Stapleton CJ, Spiegelman D, Dionne-Laporte A, Dion PA, Kahle KT, Rouleau GA, Lawton MT (2018) Identification of a rare BMP pathway mutation in a non-syndromic human brain arteriovenous malformation via exome sequencing. Hum Genome Var 5:18001
Walker EJ, Su H, Shen F, Choi E-J, Oh SP, Chen G, Lawton MT, Kim H, Chen Y, Chen W, Young WL (2011) Arteriovenous malformation in the adult mouse brain resembling the human disease. Ann Neurol 69(6):954–962
Wang L, Guo S, Zhang N, Tao Y, Zhang H, Qi T, Liang F, Huang Z (2015) The role of SDF-1/CXCR4 in the vasculogenesis and remodeling of cerebral arteriovenous malformation. Ther Clin Risk Manag 11:1337–1344
Wang Z, Zhao J, Sun J, Nie S, Li K, Gao F, Zhang T, Duan S, Di Y, Huang Y, Gao X (2016) Sex-dichotomous effects of NOS1AP promoter DNA methylation on intracranial aneurysm and brain arteriovenous malformation. Neurosci Lett 621:47–53
Wang K, Zhao S, Liu B, Zhang Q, Li Y, Liu J, Shen Y, Ding X, Lin J, Wu Y, Yan Z, Chen J, Li X, Song X, Niu Y, Liu J, Chen W, Ming Y, Du R, Chen C, Long B, Zhang Y, Tong X, Zhang S, Posey JE, Zhang B, Wu Z, Wythe JD, Liu P, Lupski JR, Yang X, Wu N (2018) Perturbations of BMP/TGF-β and VEGF/VEGFR signalling pathways in non-syndromic sporadic brain arteriovenous malformations (BAVM). J Med Genet 55(10):675–684
Wang L-J, Xue Y, Huo R, Yan Z, Xu H, Li H, Wang J, Zhang Q, Cao Y, Zhao J-Z (2020a) N6-methyladenosine methyltransferase METTL3 affects the phenotype of cerebral arteriovenous malformation via modulating Notch signaling pathway. J Biomed Sci 27(1):62
Wang L-J, Xue Y, Li H, Huo R, Yan Z, Wang J, Xu H, Wang J, Cao Y, Zhao J-Z (2020b) Wilms’ tumour 1-associating protein inhibits endothelial cell angiogenesis by m6A-dependent epigenetic silencing of desmoplakin in brain arteriovenous malformation. J Cell Mol Med 24(9):4981–4991
Wang S, Zeng Y, Pei P, He X, Liu F, Zhang T (2022) Abnormal transcriptome-wide DNA demethylation induced by folate deficiency causes neural tube defects. Front Genet 13:987210
Wei T, Richter GT, Zhang H, Sun RW, Smith CH, Strub GM (2022) Extracranial arteriovenous malformations demonstrate dysregulated TGF-β/BMP signaling and increased circulating TGF-β1. Sci Rep 12(1):16612
Weng J, Yang Y, Song D, Huo R, Li H, Chen Y, Nam Y, Zhou Q, Jiao Y, Fu W, Yan Z, Wang J, Xu H, Di L, Li J, Wang S, Zhao J, Wang J, Cao Y (2021) Somatic MAP3K3 mutation defines a subclass of cerebral cavernous malformation. Am J Hum Genet 108(5):942–950
Westbroek EM, Pawlikowska L, Lawton MT, McCulloch CE, Young WL, Kim H (2012) Brain-derived neurotrophic factor Val66Met polymorphism predicts worse functional outcome after surgery in patients with unruptured brain arteriovenous malformation. Stroke 43(8):2255–2257
Winkle M, El-Daly SM, Fabbri M, Calin GA (2021) Noncoding RNA therapeutics—challenges and potential solutions. Nat Rev Drug Discov 20(8):629–651
Winkler EA, Birk H, Burkhardt J-K, Chen X, Yue JK, Guo D, Rutledge WC, Lasker GF, Partow C, Tihan T, Chang EF, Su H, Kim H, Walcott BP, Lawton MT (2018) Reductions in brain pericytes are associated with arteriovenous malformation vascular instability. J Neurosurg 129(6):1464–1474
Winkler EA, Kim CN, Ross JM, Garcia JH, Gil E, Oh I, Chen LQ, Wu D, Catapano JS, Raygor K, Narsinh K, Kim H, Weinsheimer S, Cooke DL, Walcott BP, Lawton MT, Gupta N, Zlokovic BV, Chang EF, Abla AA, Lim DA, Nowakowski TJ (2022) A single-cell atlas of the normal and malformed human brain vasculature. Science 375(6584):eabi7377
Xia M, Wang B, Wang Z, Zhang X, Wang X (2021) Epigenetic regulation of NK cell-mediated antitumor immunity. Front Immunol 12:672328
Yan D, Hao Q, Chen Y, Li Z, Zhang H, Yuan K, Li R, Li R, Zhao Y, Wang K, Peng H, Zhang D, Chen X, Zhao Y (2022) mTOR-FABP4 signal is activated in brain arteriovenous malformations in humans. J Mol Med (berl) 100(9):1287–1297
Yao JS, Zhai W, Fan Y, Lawton MT, Barbaro NM, Young WL, Yang GY (2007) Interleukin-6 upregulates expression of KDR and stimulates proliferation of human cerebrovascular smooth muscle cells. J Cereb Blood Flow Metab 27(3):510–520
Yao J, Wu X, Zhang D, Wang L, Zhang L, Reynolds EX, Hernandez C, Boström KI, Yao Y (2019) Elevated endothelial Sox2 causes lumen disruption and cerebral arteriovenous malformations. J Clin Invest 129(8):3121–3133
Yu K, Lin CJ, Hatcher A, Lozzi B, Kong K, Huang-Hobbs E, Cheng YT, Beechar VB, Zhu W, Zhang Y, Chen F, Mills GB, Mohila CA, Creighton CJ, Noebels JL, Scott KL, Deneen B (2020) PIK3CA variants selectively initiate brain hyperactivity during gliomagenesis. Nature 578(7793):166–171
Zhao Y, Li P, Fan W, Chen D, Gu Y, Lu D, Zhao F, Hu J, Fu C, Chen X, Zhou L, Mao Y (2010) The rs522616 polymorphism in the matrix metalloproteinase-3 (MMP-3) gene is associated with sporadic brain arteriovenous malformation in a Chinese population. J Clin Neurosci 17(12):1568–1572
Zhou S, Gao X, Sun J, Lin Z, Huang Y (2017) DNA methylation of the PDGFD gene promoter increases the risk for intracranial aneurysms and brain arteriovenous malformations. DNA Cell Biol 36(6):436–442
Zhu W, Chen W, Zou D, Wang L, Bao C, Zhan L, Saw D, Wang S, Winkler E, Li Z, Zhang M, Shen F, Shaligram S, Lawton M, Su H (2018) Thalidomide reduces hemorrhage of brain arteriovenous malformations in a mouse model. Stroke 49(5):1232–1240
Funding
This study was supported by the grants from the Zhejiang Provincial Natural Science Foundation of China (LY22H090001), Ningbo Health Branding Subject Fund (PPXK2018-04), Ningbo Top Medical and Health Research Program (2022020304), Key Laboratory of Precision Medicine for Atherosclerotic Diseases of Zhejiang Province (2022E10026).
Author information
Authors and Affiliations
Contributions
YH and JY contributed to the conception and design of the study. SW, XD, YW, YW and SZ organized the database. SW and XD wrote the first draft of the manuscript. YH reviewed and edited.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have not disclosed any competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, S., Deng, X., Wu, Y. et al. Understanding the pathogenesis of brain arteriovenous malformation: genetic variations, epigenetics, signaling pathways, and immune inflammation. Hum. Genet. 142, 1633–1649 (2023). https://doi.org/10.1007/s00439-023-02605-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00439-023-02605-6