Abstract
Objective
Esophageal cancer (EC) poses a persistent threat to the health of non-elderly adults. This study aims to elucidate the temporal trends of EC-related mortality and investigate the impact of various risk factors on such deaths in the age group of 20–59 years, spanning 3 decades.
Methods
Data on EC deaths were acquired from the Global Burden of Disease, Injuries, and Risk Factors (GBD) study. We employed estimated average percentage change (EAPC) and linear mixed-effects (LME) models to analyze mortality trends and pertinent risk factors for EC.
Results
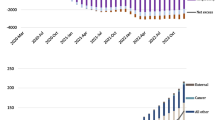
Between 1990 and 2019, EC mortality showed a downward trend, and the global number of deaths from EC among non-elderly adults surged by 24.37%. During this period, mortality rates saw an increase in only two regions—the Caribbean and Western Sub-Saharan Africa (EAPCs > 0). For male deaths, smoking and alcohol use emerged as the primary risk factors, while high body mass index (BMI) stood out as the main risk factor for female deaths. Furthermore, the LME model identified male sex, advancing age, alcohol use, smoking, and chewing tobacco as factors associated with an additional rise in EC deaths.
Conclusion
EC continues to exert a substantial toll on mortality among young and middle-aged adults globally. Implementing targeted interventions are significant in alleviating the burden of this disease within this population.




Similar content being viewed by others
Data availability
The data were obtained through an online query tool from the website of IHME (http://ghdx.healthdata.org/), and no permissions were required to access the data.
Abbreviations
- ASIR:
-
Age-standardized incidence rate;
- ASMR:
-
Age-standardized mortality rate
- BMI:
-
Body-mass index
- CI:
-
Confidence interval
- EAC:
-
Esophageal adenocarcinoma
- EAPC:
-
Estimated average percentage change
- EC:
-
Esophageal cancer
- ESCC:
-
Esophageal squamous cell carcinoma
- GBD:
-
Global Burden of Disease, Injuries, and Risk Factors Study
- LME:
-
Linear mixed effects
- PAF:
-
Population attributable fraction
- RR:
-
Rate ratio
- SDI:
-
Socio-demographic index
- SEV:
-
Summary exposure value
- UI:
-
Uncertainty interval
References
Anandavadivelan P, Lagergren P (2016) Cachexia in patients with oesophageal cancer. Nat Rev Clin Oncol 13:185–198. https://doi.org/10.1038/nrclinonc.2015.200
Arnold M, Soerjomataram I, Ferlay J et al (2015) Global incidence of oesophageal cancer by histological subtype in 2012. Gut 64:381–387. https://doi.org/10.1136/gutjnl-2014-308124
Baba Y, Yoshida N, Kinoshita K et al (2018) Clinical and prognostic features of patients with esophageal cancer and multiple primary cancers: a retrospective single-institution study. Ann Surg 267:478–483. https://doi.org/10.1097/sla.0000000000002118
Bohanes P, Yang D, Chhibar RS et al (2012) Influence of sex on the survival of patients with esophageal cancer. J Clin Oncol 30:2265–2272. https://doi.org/10.1200/jco.2011.38.8751
Chang AY, Skirbekk VF, Tyrovolas S et al (2019) Measuring population ageing: an analysis of the Global Burden of Disease Study 2017. The Lancet Public Health 4:e159–e167. https://doi.org/10.1016/s2468-2667(19)30019-2
Cook MB, Chow WH, Devesa SS (2009) Oesophageal cancer incidence in the United States by race, sex, and histologic type, 1977–2005. Br J Cancer 101:855–859. https://doi.org/10.1038/sj.bjc.6605246
Datta KK, Patil S, Patel K et al (2019) Chronic exposure to chewing tobacco induces metabolic reprogramming and cancer stem cell-like properties in esophageal epithelial cells. Cells. https://doi.org/10.3390/cells8090949
Edgren G, Adami HO, Weiderpass E et al (2013) A global assessment of the oesophageal adenocarcinoma epidemic. Gut 62:1406–1414. https://doi.org/10.1136/gutjnl-2012-302412
Fan J, Liu Z, Mao X et al (2020) Global trends in the incidence and mortality of esophageal cancer from 1990 to 2017. Cancer Med 9:6875–6887. https://doi.org/10.1002/cam4.3338
Fitzmaurice C, Akinyemiju TF, Al Lami FH et al (2018) Global, regional, and national cancer incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life-years for 29 cancer groups, 1990 to 2016: A systematic analysis for the Global Burden of Disease Study. JAMA Oncol 4:1553–1568. https://doi.org/10.1001/jamaoncol.2018.2706
Foreman KJ, Marquez N, Dolgert A et al (2018) Forecasting life expectancy, years of life lost, and all-cause and cause-specific mortality for 250 causes of death: reference and alternative scenarios for 2016–40 for 195 countries and territories. Lancet (london, England) 392:2052–2090. https://doi.org/10.1016/s0140-6736(18)31694-5
Freedman ND, Abnet CC, Leitzmann MF et al (2007) A prospective study of tobacco, alcohol, and the risk of esophageal and gastric cancer subtypes. Am J Epidemiol 165:1424–1433. https://doi.org/10.1093/aje/kwm051
Freedman ND, Murray LJ, Kamangar F et al (2011) Alcohol intake and risk of oesophageal adenocarcinoma: a pooled analysis from the BEACON Consortium. Gut 60:1029–1037. https://doi.org/10.1136/gut.2010.233866
Gao S, Yang WS, Bray F et al (2012) Declining rates of hepatocellular carcinoma in urban Shanghai: incidence trends in 1976–2005. Eur J Epidemiol 27:39–46. https://doi.org/10.1007/s10654-011-9636-8
Gapstur SM, Drope JM, Jacobs EJ et al (2018) A blueprint for the primary prevention of cancer: Targeting established, modifiable risk factors. CA Cancer J Clin 68:446–470. https://doi.org/10.3322/caac.21496
Global Burden of Disease Study (2017) Global, regional, and national age-sex specific mortality for 264 causes of death, 1980–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet (london, England) 390:1151–1210. https://doi.org/10.1016/s0140-6736(17)32152-9
Global Burden of Disease Study (2018) Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet (london, England) 392:1789–1858. https://doi.org/10.1016/s0140-6736(18)32279-7
Global Burden of Disease Study (2020) Global burden of 87 risk factors in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet (london, England) 396:1223–1249. https://doi.org/10.1016/s0140-6736(20)30752-2
Global Burden of Disease Study (2021) Global, regional, and national burden of respiratory tract cancers and associated risk factors from 1990 to 2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet Respir Med 9:1030–1049. https://doi.org/10.1016/s2213-2600(21)00164-8
Guy GP Jr, Yabroff KR, Ekwueme DU et al (2015) Healthcare expenditure burden among non-elderly cancer survivors, 2008–2012. Am J Prev Med 49:S489-497. https://doi.org/10.1016/j.amepre.2015.09.002
He J, Chen WQ, Li ZS et al (2022) China guideline for the screening, early detection and early treatment of esophageal cancer (2022, Beijing). Zhonghua Zhong Liu Za Zhi [chin J Oncol] 44:491–522. https://doi.org/10.3760/cma.j.cn112152-20220517-00348
Hung GY, Horng JL, Yen HJ et al (2015) Changing incidence patterns of hepatocellular carcinoma among age groups in Taiwan. J Hepatol 63:1390–1396. https://doi.org/10.1016/j.jhep.2015.07.032
Jiang Y, Lin Y, Wen Y et al (2023) Global trends in the burden of esophageal cancer, 1990–2019: results from the Global Burden of Disease Study 2019. J Thorac Dis 15:348–364. https://doi.org/10.21037/jtd-22-856
Khan Z (2016) A gaping gap (smokeless tobacco control in Pakistan). Tob Induc Dis 14:36. https://doi.org/10.1186/s12971-016-0102-y
Kocarnik JM, Compton K, Dean FE et al (2022) Cancer incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life years for 29 cancer groups from 2010 to 2019: a systematic analysis for the Global Burden of Disease Study 2019. JAMA Oncol 8:420–444. https://doi.org/10.1001/jamaoncol.2021.6987
La Rosa F, Cresci A, Orpianesi C et al (1988) Esophageal cancer mortality: relationship with alcohol intake and cigarette smoking in Italy. Eur J Epidemiol 4:93–98. https://doi.org/10.1007/bf00152698
Lee YC, Hashibe M (2014) Tobacco, alcohol, and cancer in low and high income countries. Ann Glob Health 80:378–383. https://doi.org/10.1016/j.aogh.2014.09.010
Li C, He WQ (2022) Comparison of primary liver cancer mortality estimates from World Health Organization, global burden disease and global cancer observatory. Liver Int 42:2299–2316. https://doi.org/10.1111/liv.15357
Li N, Deng Y, Zhou L et al (2019) Global burden of breast cancer and attributable risk factors in 195 countries and territories, from 1990 to 2017: results from the Global Burden of Disease Study 2017. J Hematol Oncol 12:140. https://doi.org/10.1186/s13045-019-0828-0
Li N, Zhai Z, Zheng Y et al (2021) Association of 13 occupational carcinogens in patients with cancer, individually and collectively, 1990–2017. JAMA Netw Open 4:e2037530. https://doi.org/10.1001/jamanetworkopen.2020.37530
Lin Y, Totsuka Y, He Y et al (2013) Epidemiology of esophageal cancer in Japan and China. J Epidemiol 23:233–242. https://doi.org/10.2188/jea.je20120162
Martikainen P, Mäkelä P, Peltonen R et al (2014) Income differences in life expectancy: the changing contribution of harmful consumption of alcohol and smoking. Epidemiology 25:182–190. https://doi.org/10.1097/ede.0000000000000064
Miller KD, Fidler-Benaoudia M, Keegan TH et al (2020) Cancer statistics for adolescents and young adults, 2020. CA Cancer J Clin 70:443–459. https://doi.org/10.3322/caac.21637
Molassiotis A, Kwok SWH, Leung AYM et al (2022) Associations between sociodemographic factors, health spending, disease burden, and life expectancy of older adults (70 + years old) in 22 countries in the Western Pacific Region, 1995–2019: estimates from the Global Burden of Disease (GBD) Study 2019. GeroScience 44:925–951. https://doi.org/10.1007/s11357-021-00494-z
Napier KJ, Scheerer M, Misra S (2014) Esophageal cancer: a review of epidemiology, pathogenesis, staging workup and treatment modalities. World J Gastrointest Oncol 6:112–120. https://doi.org/10.4251/wjgo.v6.i5.112
Paik JM, Mir S, Alqahtani SA et al (2022) Dietary risks for liver mortality in NAFLD: global burden of disease data. Hepatol Commun 6:90–100. https://doi.org/10.1002/hep4.1707
Patrick ME, Evans-Polce RJ, Arterberry BJ et al (2023) Initiation of and escalation to high-intensity drinking in young adults. JAMA Pediatr 177:286–293. https://doi.org/10.1001/jamapediatrics.2022.5642
Qumseya B, Sultan S, Bain P et al (2019) ASGE guideline on screening and surveillance of Barrett’s esophagus. Gastrointest Endosc 90:335-359.e332. https://doi.org/10.1016/j.gie.2019.05.012
Rock CL, Thomson C, Gansler T et al (2020) American Cancer Society guideline for diet and physical activity for cancer prevention. CA Cancer J Clin 70:245–271. https://doi.org/10.3322/caac.21591
Rumgay H, Shield K, Charvat H et al (2021) Global burden of cancer in 2020 attributable to alcohol consumption: a population-based study. Lancet Oncol 22:1071–1080. https://doi.org/10.1016/s1470-2045(21)00279-5
Sawas T, Manrique GC, Iyer PG et al (2019) Young adults with esophageal adenocarcinoma present with more advanced stage tumors and have shorter survival times. Clin Gastroenterol Hepatol 17:1756–1762. https://doi.org/10.1016/j.cgh.2018.09.031
Shah MA, Kennedy EB, Catenacci DV et al (2020) Treatment of locally advanced esophageal carcinoma: ASCO guideline. J Clin Oncol 38:2677–2694. https://doi.org/10.1200/jco.20.00866
Siemiatycki J, Krewski D, Franco E et al (1995) Associations between cigarette smoking and each of 21 types of cancer: a multi-site case-control study. Int J Epidemiol 24:504–514. https://doi.org/10.1093/ije/24.3.504
Sung H, Ferlay J, Siegel RL et al (2021) Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. cA Cancer J Cli 71:209–249. https://doi.org/10.3322/caac.21660
Xie W, Yang T, Zuo J et al (2022) Chinese and global burdens of gastrointestinal cancers from 1990 to 2019. Front Public Health 10:941284. https://doi.org/10.3389/fpubh.2022.941284
Zhang D, Liu S, Li Z et al (2022) Global, regional and national burden of gastroesophageal reflux disease, 1990–2019: update from the GBD 2019 study. Ann Med 54:1372–1384. https://doi.org/10.1080/07853890.2022.2074535
Acknowledgements
All authors highly appreciate all members of the Global Burden of Disease Study 2019.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Conception: QML, FL; design of the work: QML, LYZ, TW, ZPZ, XRZ, YJW, RG, YJZ, XTZ, and FL; data analysis: QML, XRZ, YJW, RG, YJZ, and XTZ; statistical analysis: QML, LYZ, TW, and ZPZ; manuscript editing: QML, FL.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, Q., Zhu, L., Wei, T. et al. Secular trends and attributable risk factors of esophageal cancer deaths among non-elderly adults based on Global Burden of Disease Study. J Cancer Res Clin Oncol 149, 16417–16427 (2023). https://doi.org/10.1007/s00432-023-05380-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-05380-z