Abstract
Purpose
Our study was to determine whether immediate androgen deprivation therapy (ADT) plus radiotherapy (RT) extends survival in men with node-positive prostate cancer (PCa) after radical prostatectomy (RP) compared with those who received ADT alone.
Methods
A total of 99 consecutive patients with pathological positive lymph nodes (pN1) PCa were included in this study to receive immediate ADT plus RT (n = 70) or to receive immediate ADT alone (n = 29). The primary endpoint was castration-resistant prostate cancer (CRPC) free survival; the secondary endpoints were distant metastasis-free survival. Cox regression was used to assess the independent risk factors for CRPC.
Results
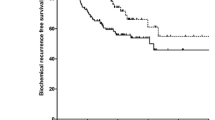
The median follow-up time was 34.0 (24.8, 47.8) months and 34.25 (23.0, 49.0) months, respectively, in the ADT + RT group and ADT-alone group. The 5-year CRPC-free survival rate was 79.5% and 58.3%, respectively, in the ADT + RT group and ADT-alone group (p = 0.308). The 5-year distant metastasis-free survival rate was 71.4% and 38.8, respectively, in the ADT + RT group and ADT-alone group (p = 0.478). Compared with ADT-alone group, we saw a modest, but no significant improvement in CRPC-free survival and distant metastasis-free survival in ADT + RT group. The results of Cox regression showed that positive lymph nodes ≥ 4 was an independent risk factor for CRPC (p = 0.041).
Conclusions
We found that immediate ADT plus RT compared to ADT alone did not improve CRPC-free and metastasis-free survival. Multivariate Cox regression analyses also indicated that patients with positive lymph nodes < 4 may benefits from ADT plus RT.


Similar content being viewed by others
Data availability
All data generated or analyzed during the current study are included in this published article.
Abbreviations
- PCa:
-
Prostate cancer
- pN1:
-
Pathological positive lymph nodes
- RP:
-
Radical prostatectomy
- ADT:
-
Androgen deprivation therapy
- RT:
-
Radiotherapy
- CRPC:
-
Castration-resistant prostate cancer
- ePLND:
-
Extended pelvic lymph node dissection
- LAPC:
-
Locally advanced prostate cancer
- RT + ADT:
-
Adjuvant radiotherapy plus androgen deprivation therapy
- PSA:
-
Prostate specific antigen
- GS:
-
Gleason score
- BMI:
-
Body mass index
References
Abdollah F et al (2013) Extended pelvic lymph node dissection in prostate cancer: a 20-year audit in a single center. Ann Oncol 24:1459–1466. https://doi.org/10.1093/annonc/mdt120
Abdollah F et al (2014) Impact of adjuvant radiotherapy on survival of patients with node-positive prostate cancer. J Clin Oncol 32:3939–3947. https://doi.org/10.1200/JCO.2013.54.7893
Bastian PJ et al (2006) Clinical and pathologic outcome after radical prostatectomy for prostate cancer patients with a preoperative Gleason sum of 8 to 10. Cancer 107:1265–1272. https://doi.org/10.1002/cncr.22116
Bernstein AN et al (2018) Contemporary incidence and outcomes of prostate cancer lymph node metastases. J Urol 199:1510–1517. https://doi.org/10.1016/j.juro.2017.12.048
Boorjian SA et al (2007) Long-term outcome after radical prostatectomy for patients with lymph node positive prostate cancer in the prostate specific antigen era. J Urol 178:864–870. https://doi.org/10.1016/j.juro.2007.05.048 (Discussion 870–871)
Chen R et al (2014) Prostate cancer in Asia: a collaborative report. Asian J Urol 1:15–29. https://doi.org/10.1016/j.ajur.2014.08.007
Chen W et al (2018) Cancer incidence and mortality in China, 2014. Chin J Cancer Res 30:1–12. https://doi.org/10.21147/j.issn.1000-9604.2018.01.01
Dalela D et al (2017) Genomic classifier augments the role of pathological features in identifying optimal candidates for adjuvant radiation therapy in patients with prostate cancer: development and internal validation of a multivariable prognostic model. J Clin Oncol 35:1982–1990. https://doi.org/10.1200/JCO.2016.69.9918
Donohue JF et al (2006) Poorly differentiated prostate cancer treated with radical prostatectomy: long-term outcome and incidence of pathological downgrading. J Urol 176:991–995. https://doi.org/10.1016/j.juro.2006.04.048
Eggener SE et al (2011) Predicting 15-year prostate cancer specific mortality after radical prostatectomy. J Urol 185:869–875. https://doi.org/10.1016/j.juro.2010.10.057
Ghavamian R, Bergstralh EJ, Blute ML, Slezak J, Zincke H (1999) Radical retropubic prostatectomy plus orchiectomy versus orchiectomy alone for pTxN+ prostate cancer: a matched comparison. J Urol 161:1223–1227 (Discussion 1227–1228)
Gore JL et al (2017) Decipher test impacts decision making among patients considering adjuvant and salvage treatment after radical prostatectomy: interim results from the multicenter prospective PRO-IMPACT study. Cancer 123:2850–2859. https://doi.org/10.1002/cncr.30665
Gözen AS, Akin Y, Ates M, Hruza M, Rassweiler J (2015) Impact of laparoscopic radical prostatectomy on clinical T3 prostate cancer: experience of a single centre with long-term follow-up. BJU Int 116:102–108. https://doi.org/10.1111/bju.12710
Hofman MS et al (2020) Prostate-specific membrane antigen PET-CT in patients with high-risk prostate cancer before curative-intent surgery or radiotherapy (proPSMA): a prospective, randomised, multicentre study. Lancet 395:1208–1216. https://doi.org/10.1016/S0140-6736(20)30314-7
Lancee M, Tikkinen K, de Reijke TM, Kataja VV, Aben K, Vernooij R (2018) Guideline of guidelines: primary monotherapies for localised or locally advanced prostate cancer. BJU Int 122:535–548. https://doi.org/10.1111/bju.14237
Marvaso G et al (2021) Adjuvant radiotherapy in node positive prostate cancer patients: a debate still on, when, for whom. BJU Int 127:454–462. https://doi.org/10.1111/bju.15228
Messing EM et al (2006) Immediate versus deferred androgen deprivation treatment in patients with node-positive prostate cancer after radical prostatectomy and pelvic lymphadenectomy. Lancet Oncol 7:472–479. https://doi.org/10.1016/S1470-2045(06)70700-8
Moris L et al (2020) Benefits and risks of primary treatments for high-risk localized and locally advanced prostate cancer: an international multidisciplinary systematic review. Eur Urol 77:614–627. https://doi.org/10.1016/j.eururo.2020.01.033
Mottet N et al (2022) EAU guidelines. Presented at the EAU annual congress Amsterdam. ISBN 978-94-92671-16-5. https://uroweb.org.guidelinesprostate-cancerchaptercitation-information
Preisser F et al (2019) Persistent prostate-specific antigen after radical prostatectomy and its impact on oncologic outcomes. Eur Urol 76:106–114. https://doi.org/10.1016/j.eururo.2019.01.048
Schumacher MC, Burkhard FC, Thalmann GN, Fleischmann A, Studer UE (2008) Good outcome for patients with few lymph node metastases after radical retropubic prostatectomy. Eur Urol 54:344–352. https://doi.org/10.1016/j.eururo.2008.05.023
Shin TY, Lee YS (2022) Robot-assisted radical prostatectomy in the treatment of patients with clinically high-risk localized and locally advanced prostate cancer: single surgeons functional and oncologic outcomes. BMC Urol 22:49. https://doi.org/10.1186/s12894-022-00998-6
Siegel RL, Miller KD, Fuchs HE, Jemal A (2022) Cancer statistics, 2022. CA Cancer J Clin 72:7–33. https://doi.org/10.3322/caac.21708
Tilki D et al (2017) Adjuvant radiation therapy is associated with better oncological outcome compared with salvage radiation therapy in patients with pN1 prostate cancer treated with radical prostatectomy. BJU Int 119:717–723. https://doi.org/10.1111/bju.13679
Ventimiglia E et al (2019) A systematic review of the role of definitive local treatment in patients with clinically lymph node-positive prostate cancer. Eur Urol Oncol 2:294–301. https://doi.org/10.1016/j.euo.2019.02.001
Ward JF, Blute ML, Slezak J, Bergstralh EJ, Zincke H (2003) The long-term clinical impact of biochemical recurrence of prostate cancer 5 or more years after radical prostatectomy. J Urol 170:1872–1876. https://doi.org/10.1097/01.ju.0000091876.13656.2e
Yossepowitch O, Eggener SE, Bianco FJ Jr, Carver BS, Serio A, Scardino PT, Eastham JA (2007) Radical prostatectomy for clinically localized, high risk prostate cancer: critical analysis of risk assessment methods. J Urol 178:493–499. https://doi.org/10.1016/j.juro.2007.03.105 (Discussion 499)
Acknowledgements
I wish to thank Xu Gao, Yan Wang for advice on experimental design, Zhenyang Dong for data acquisition. The authors received no funding for this study.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
XG and YW contributed to the study conception and design. Material preparation, data collection and analysis were performed by HC, MQ, ZD and YW. The first draft of the manuscript was written by HC, MQ. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Conflict of interest
The authors have no conflict of interest relevant to the present paper to disclose.
Consent to participate
Study purpose and procedures were explained to all patients and written informed consent was obtained from all individual participants included in the study.
Consent to publish
Not applicable.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the 1964 Declaration of Helsinki and its later amendments. As a retrospective study and data analysis were performed anonymously, this study was exempt from the ethical approval. Written informed consent was obtained from all participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, H., Qu, M., Shi, H. et al. Adjuvant radiotherapy in patients with node-positive prostate cancer after radical prostatectomy. J Cancer Res Clin Oncol 149, 4925–4932 (2023). https://doi.org/10.1007/s00432-022-04409-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-022-04409-z