Abstract
Objective
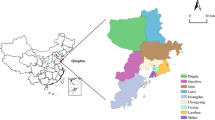
The aim of this study was to examine the impacts of short-term exposure to air pollutants on hospitalizations for mental disorders (MDs) in Qingdao, a Chinese coastal city, and to assess the corresponding hospitalization risk and economic cost.
Methods
Daily data on MD hospitalizations and environmental variables were collected from January 1, 2015, to December 31, 2019. An overdispersed generalized additive model was used to estimate the association between air pollution and MD hospitalizations. The cost of illness method was applied to calculate the corresponding economic burden.
Results
With each 10 μg/m3 increase in the concentration of fine particulate matter (PM2.5) at lag05, inhalable particulate matter (PM10) at lag0, sulfur dioxide (SO2) at lag06 and ozone (O3) at lag0, the corresponding relative risks (RRs) and 95% confidence intervals (CIs) were 1.0182 (1.0035–1.0332), 1.0063 (1.0001–1.0126), 1.0997 (1.0200–1.1885) and 1.0099 (1.0005–1.0194), respectively. However, no significant effects of nitrogen dioxide (NO2) or carbon monoxide (CO) were found. Stratified analysis showed that males were susceptible to SO2 and O3, while females were susceptible to PM2.5. Older individuals (≥ 45 years) were more vulnerable to air pollutants (PM2.5, PM10, SO2 and O3) than younger individuals (< 45 years). Taking the Global Air Quality Guidelines 2021 as a reference, 8.71% (2,168 cases) of MD hospitalizations were attributable to air pollutant exposure, with a total economic burden of 154.36 million RMB.
Conclusion
Short-term exposure to air pollution was associated with an increased risk of hospitalization for MDs. The economic advantages of further reducing air pollution are enormous.


Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author upon reasonable request.
References
Altman DG, Bland JM (2003) Interaction revisited: the difference between two estimates. BMJ 326(7382):219. https://doi.org/10.1136/bmj.326.7382.219
Attademo L, Bernardini F (2020) Air pollution as risk factor for mental disorders: in search for a possible link with Alzheimer’s disease and schizophrenia. J Alzheimers Dis 76(3):825–830. https://doi.org/10.3233/JAD-200289
Attademo L, Bernardini F, Garinella R et al (2017) Environmental pollution and risk of psychotic disorders: a review of the science to date. Schizophr Res 181:55–59
Bernardini F, Attademo L, Trezzi R et al (2019) Air pollutants and daily number of admissions to psychiatric emergency services: evidence for detrimental mental health effects of ozone. Epidemiol Psychiatr Sci 29:e66. https://doi.org/10.1017/S2045796019000623
Brokamp C, Strawn JR, Beck AF et al (2019) Pediatric psychiatric emergency department utilization and fine particulate matter: a case-crossover study. Environ Health Perspect 127(9):97006. https://doi.org/10.1289/EHP4815
Buoli M, Grassi S, Caldiroli A et al (2018) Is there a link between air pollution and mental disorders? Environ Int 118:154–168. https://doi.org/10.1016/j.envint.2018.05.044
Calderón-Garcidueñas L, Mora-Tiscareño A, Styner M et al (2012) White matter hyperintensities, systemic inflammation, brain growth, and cognitive functions in children exposed to air pollution. J Alzheimers Dis 31(1):183–191
Cao X, You X, Wang D et al (2023) Short-term effects of ambient ozone exposure on daily hospitalizations for circulatory diseases in Ganzhou, China: a time-series study. Chemosphere 327:138513. https://doi.org/10.1016/j.chemosphere.2023.138513
Chen C, Liu C, Chen R et al (2018) Ambient air pollution and daily hospital admissions for mental disorders in Shanghai, China. Sci Total Environ 613–614:324–330. https://doi.org/10.1016/j.scitotenv.2017.09.098
Chen R, Yin P, Meng X et al (2019) Associations between coarse particulate matter air pollution and cause-specific mortality: a nationwide analysis in 272 Chinese cities. Environ Health Perspect 127(1):17008. https://doi.org/10.1289/EHP2711
Chen J, Lv M, Yao W et al (2020) Association between fine particulate matter air pollution and acute aortic dissections: a time-series study in Shanghai, China. Chemosphere 243:125357. https://doi.org/10.1016/j.chemosphere.2019.125357
Fan YS, Xu Y, Bayrak Ş et al (2023) Macroscale thalamic functional organization disturbances and underlying core cytoarchitecture in early-onset schizophrenia. Schizophr Bull. https://doi.org/10.1093/schbul/sbad048
Gao Q, Xu Q, Guo X et al (2017) Particulate matter air pollution associated with hospital admissions for mental disorders: a time-series study in Beijing, China. Eur Psychiatry 44:68–75. https://doi.org/10.1016/j.eurpsy.2017.02.492
GBD (2018) Global, regional, and national disability-adjusted life-years (DALYs) for 359 diseases and injuries and healthy life expectancy (HALE) for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 392(10159):1859–1922. https://doi.org/10.1016/S0140-6736(18)32335-3
Hahad O, Lelieveld J, Birklein F et al (2020) Ambient air pollution increases the risk of cerebrovascular and neuropsychiatric disorders through induction of inflammation and oxidative stress. Int J Mol Sci 21(12):4306. https://doi.org/10.3390/ijms21124306
Hao G, Zuo L, Xiong P et al (2022) Associations of PM2.5 and road traffic noise with mental health: evidence from UK Biobank. Environ Res 207:112221. https://doi.org/10.1016/j.envres.2021.112221
Ji Y, Liu B, Song J et al (2021) Particulate matter pollution associated with schizophrenia hospital re-admissions: a time-series study in a coastal Chinese city. Environ Sci Pollut Res Int 28(41):58355–58363. https://doi.org/10.1007/s11356-021-14816-3
Ji Y, Liu B, Song J et al (2022a) Association between traffic-related air pollution and anxiety hospitalizations in a coastal Chinese city: are there potentially susceptible groups? Environ Res 209:112832. https://doi.org/10.1016/j.envres.2022.112832
Ji Y, Liu B, Song J et al (2022b) Short-term effects and economic burden assessment of ambient air pollution on hospitalizations for schizophrenia. Environ Sci Pollut Res Int 29(30):45449–45460. https://doi.org/10.1007/s11356-022-19026-z
Ji Y, Xiong J, Yuan Z et al (2023) Risk assessment and disease burden of extreme precipitation on hospitalizations for acute aortic dissection in a subtropical coastal Chinese city. Front Public Health 11:1216847. https://doi.org/10.3389/fpubh.2023.1216847
Kennelly B (2017) How should cost-of-illness studies be interpreted? Lancet Psychiatry 4(10):735–736. https://doi.org/10.1016/S2215-0366(17)30364-4
Kim SH, Shin SD, Song KJ et al (2019) Association between ambient PM2.5 and emergency department visits for psychiatric emergency diseases. Am J Emerg Med 37(9):1649–1656. https://doi.org/10.1016/j.ajem.2018.11.034
Laskaris LE, Di Biase MA, Everall I et al (2016) Microglial activation and progressive brain changes in schizophrenia. Br J Pharmacol 173(4):666–680. https://doi.org/10.1111/bph.13364
Lee S, Lee W, Kim D et al (2019) Short-term PM2.5 exposure and emergency hospital admissions for mental disease. Environ Res 171:313–320. https://doi.org/10.1016/j.envres.2019.01.036
Li W, Wilker EH, Dorans KS et al (2016) Short-term exposure to air pollution and biomarkers of oxidative stress: the framingham heart study. J Am Heart Assoc 5(5):e002742
Li H, Zhang S, Qian ZM et al (2020) Short-term effects of air pollution on cause-specific mental disorders in three subtropical Chinese cities. Environ Res 191:110214. https://doi.org/10.1016/j.envres.2020.110214
Li F, Cui Y, Li Y et al (2022) Prevalence of mental disorders in school children and adolescents in China: diagnostic data from detailed clinical assessments of 17,524 individuals. J Child Psychol Psychiatry 63(1):34–46. https://doi.org/10.1111/jcpp.13445
Lu P, Zhang Y, Xia G et al (2020) Attributable risks associated with hospital outpatient visits for mental disorders due to air pollution: a multi-city study in China. Environ Int 143:105906. https://doi.org/10.1016/j.envint.2020.105906
Marshall M (2020) The hidden links between mental disorders. Nature 581(7806):19–21. https://doi.org/10.1038/d41586-020-00922-8
Min JY, Kim HJ, Min KB (2018) Long-term exposure to air pollution and the risk of suicide death: a population-based cohort study. Sci Total Environ 628–629:573–579. https://doi.org/10.1016/j.scitotenv.2018.02.011
Muhsin HA, Steingrimsson S, Oudin A et al (2022) Air pollution and increased number of psychiatric emergency room visits: a case-crossover study for identifying susceptible groups. Environ Res 204(Pt A):112001. https://doi.org/10.1016/j.envres.2021.112001
Nakazawa T (2023) Modeling mental disorders in a dish. Psychiatry Clin Neurosci 77(6):307. https://doi.org/10.1111/pcn.13552
Nguyen AM, Malig BJ, Basu R (2021) The association between ozone and fine particles and mental health-related emergency department visits in California, 2005–2013. PLoS ONE 16(4):e0249675. https://doi.org/10.1371/journal.pone.0249675
Oppenheim HA, Lucero J, Guyot AC et al (2013) Exposure to vehicle emissions results in altered blood brain barrier permeability and expression of matrix metalloproteinases and tight junction proteins in mice. Part Fibre Toxicol 10:62
Oudin A, Åström DO, Asplund P et al (2018) The association between daily concentrations of air pollution and visits to a psychiatric emergency unit: a case-crossover study. Environ Health 17(1):4. https://doi.org/10.1186/s12940-017-0348-8
Paksarian D, Trabjerg BB, Merikangas KR et al (2020) Adolescent residential mobility, genetic liability and risk of schizophrenia, bipolar disorder and major depression. Br J Psychiatry 217(1):390–396. https://doi.org/10.1192/bjp.2020.8
Phillips C (2017) Lifestyle modulators of neuroplasticity: how physical activity, mental engagement, and diet promote cognitive health during aging. Neural Plast 2017:3589271. https://doi.org/10.1155/2017/3589271
Qiu H, Zhu X, Wang L et al (2019) Attributable risk of hospital admissions for overall and specific mental disorders due to particulate matter pollution: a time-series study in Chengdu, China. Environ Res 170:230–237. https://doi.org/10.1016/j.envres.2018.12.019
Qiu H, Wang L, Luo L et al (2022) Gaseous air pollutants and hospitalizations for mental disorders in 17 Chinese cities: association, morbidity burden and economic costs. Environ Res 204(Pt A):111928. https://doi.org/10.1016/j.envres.2021.111928
Song J, Zheng L, Lu M et al (2018) Acute effects of ambient particulate matter pollution on hospital admissions for mental and behavioral disorders: a time-series study in Shijiazhuang, China. Sci Total Environ 636:205–211. https://doi.org/10.1016/j.scitotenv.2018.04.187
Szyszkowicz M, Zemek R, Colman I et al (2020) Air pollution and emergency department visits for mental disorders among youth. Int J Environ Res Public Health 17(12):4190. https://doi.org/10.3390/ijerph17124190
Tong L, Li K, Zhou Q (2016) Season, sex and age as modifiers in the association of psychosis morbidity with air pollutants: a rising problem in a Chinese metropolis. Sci Total Environ 541:928–933. https://doi.org/10.1016/j.scitotenv.2015.09.066
Wang Y, Xiong L, Tang M (2017) Toxicity of inhaled particulate matter on the central nervous system: neuroinflammation, neuropsychological effects and neurodegenerative disease. J Appl Toxicol 37(6):644–667. https://doi.org/10.1002/jat.3451
Wang L, Gao X, Wang R et al (2023) (2023) Ecological correlation between short term exposure to particulate matter and hospitalization for mental disorders in Shijiazhuang, China. Sci Rep 13(1):11412. https://doi.org/10.1038/s41598-023-37279-7
Wu Z, Chen X, Li G et al (2020) Attributable risk and economic cost of hospital admissions for mental disorders due to PM2.5 in Beijing. Sci Total Environ 718:137274. https://doi.org/10.1016/j.scitotenv.2020.137274
Xu X, Ha SU, Basnet R (2016) A review of epidemiological research on adverse neurological effects of exposure to ambient air pollution. Front Public Health 4:157. https://doi.org/10.3389/fpubh.2016.00157
Yan W, Ji X, Shi J et al (2015) Acute nitrogen dioxide inhalation induces mitochondrial dysfunction in rat brain. Environ Res 138:416–424. https://doi.org/10.1016/j.envres.2015.02.022
You X, Cao X, Guo Y et al (2023) Associations between short-term PM25 exposure and daily hospital admissions for circulatory system diseases in Ganzhou, China: a time series study. Front Public Health 11:1134516. https://doi.org/10.3389/fpubh.2023.1134516
Zhang P, Zhou X (2020) Health and economic impacts of particulate matter pollution on hospital admissions for mental disorders in Chengdu, Southwestern China. Sci Total Environ 733:139114. https://doi.org/10.1016/j.scitotenv.2020.139114
Zhang X, Yu S, Zhang F et al (2023) Association between traffic-related air pollution and osteoporotic fracture hospitalizations in inland and coastal areas: evidences from the central areas of two cities in Shandong Province, China. Arch Osteoporos 18(1):96. https://doi.org/10.1007/s11657-023-01308-9
Zhou YM, Fan YN, Yao CY et al (2021) Association between short-term ambient air pollution and outpatient visits of anxiety: a hospital-based study in northwestern China. Environ Res 197:111071. https://doi.org/10.1016/j.envres.2021.111071
Acknowledgements
Not applicable.
Funding
No funding was received to assist with the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
YC and YM wrote the manuscript and analysed the data. XL collected the data. YM, XL and JY reviewed the results and provided guidelines for presentation and interpretation. All of the authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This was a retrospective study, and there was no direct contact with the patients. Consequently, informed consent was not necessary. Our protocol was approved by the Ethics Committee of Qingdao Mental Health Center and complied with the Declaration of Helsinki.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cheng, Y., Meng, Y., Li, X. et al. Effects of ambient air pollution on the hospitalization risk and economic burden of mental disorders in Qingdao, China. Int Arch Occup Environ Health 97, 109–120 (2024). https://doi.org/10.1007/s00420-023-02030-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00420-023-02030-2