Abstract
Purpose
To determine the impact of the healthy worker effect (HWE) as a bias for the external and internal validity of the follow-up assessment in prospective survey research. Specifically, the study examined (1) whether the health status of respondents at the baseline measurement influenced response at the follow-up survey (external validity) and (2) whether HWE is a threat to internal validity by differential attrition, i.e., whether associations between work and health at baseline differ between stayers and dropouts.
Methods
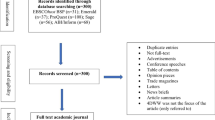
In a two-wave questionnaire survey with a 2-year time lag comprising 6283 persons, 4392 responded at both time points (response rate 70 %). Mental distress and somatic symptoms served as indicators of health. Role conflict and role clarity were indicators of work factors.
Results
There were few differences in response rate at follow-up between persons with and without health complaints at the baseline measurement. As response rate increased incrementally with educational level, there seems to be a socio-educational bias, rather than a HWE bias on survey participation. Baseline relationships between work factors and health indicators were equal in magnitude among stayers and dropouts.
Conclusion
The health status of participants at baseline seems to have little impact on the external and internal validity of the follow-up assessment in prospective survey research. Hence, the findings provide little support to the HWE as a potential bias in prospective studies within occupational health research. A limitation of the study is that the findings do not inform about the impact of the HWE on participation in the baseline assessment.
Similar content being viewed by others
References
Baruch Y, Holtom BC (2008) Survey response rate levels and trends in organizational research. Hum Relat 61(8):1139–1160
Bentler PM, Chou CP (1987) Practical issues in structural modeling. Sociol Methods Res 16(1):78–117
Burns CJ, Bodner KM, Jammer BL, Collins JJ, Swaen GM (2011) The healthy worker effect in US chemical industry workers. Occup Med (Lond) 61(1):40–44. doi:10.1093/occmed/kqq168
Christensen JO, Knardahl S (2010) Work and neck pain: a prospective study of psychological, social, and mechanical risk factors. Pain 151(1):162–173. doi:10.1016/j.pain.2010.07.001
Christensen JO, Knardahl S (2012a) Work and back pain: a prospective study of psychological, social and mechanical predictors of back pain severity. Eur J Pain 16(6):921–933. doi:10.1002/j.1532-2149.2011.00091.x
Christensen JO, Knardahl S (2012b) Work and headache: a prospective study of psychological, social, and mechanical predictors of headache severity. Pain 153(10):2119–2132. doi:10.1016/j.pain.2012.07.009
Christensen JO, Knardahl S (2014) Time-course of occupational psychological and social factors as predictors of new-onset and persistent neck pain: a three-wave prospective study over 4 years. Pain 155(7):1262–1271. doi:10.1016/j.pain.2014.03.021
Dallner M et al (2000) Validation of the General Nordic Questionnaire (QPSNordic) for psychological and social factors at work. Nordic Council of Ministers, Copenhagen
Derogatis LR, Lipman RS, Rickels K, Uhlenhuth EH, Covi L (1974) The Hopkins Symptom Checklist (HSCL): a self report symptom inventory. Behav Sci 19(1):1–15
Dumas O et al (2013) Work related asthma. A causal analysis controlling the healthy worker effect. Occup Environ Med 70(9):603–610. doi:10.1136/oemed-2013-101362
Ford MT, Matthews RA, Wooldridge JD, Mishra V, Kakar UM, Strahan SR (2014) How do occupational stressor-strain effects vary with time? A review and meta-analysis of the relevance of time lags in longitudinal studies. Work Stress 28(1):9–30
Hu LT, Bentler PM (1999) Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Struct Equ Model Multidiscip J 6(1):1–55. doi:10.1080/10705519909540118
IBM Corp. Released (2013) IBM SPSS statistics for windows, version 22.0. IBM Corp, Armonk, NY
Ilies R, Hauserman N, Schwochau S, Stibal J (2003) Reported incidence rates of work-related sexual harassment in the United States: using meta-analysis to explain reported rate disparities. Pers Psychol 56:607–631
Li CY, Sung FC (1999) A review of the healthy worker effect in occupational epidemiology. Occup Med (Lond) 49(4):225–229
McMichael AJ (1976) Standardized mortality ratios and the “healthy worker effect”: scratching beneath the surface. J Occup Med 18(3):165–168
Nettelbladt P, Hansson L, Stefansson C-G, Borgquist L, Nordström G (1993) Test characteristics of the Hopkins Symptom Check List-25 (HSCL-25) in Sweden, using the Present State Examination (PSE-9) as a caseness criterion. Soc Psychiatry Psychiatr Epidemiol 28:130–133
Nielsen MB, Einarsen S (2008) Sampling in research on interpersonal aggression. Aggress Behav 34(3):265–272
Nielsen MB, Einarsen S (2012) Outcomes of workplace bullying: a meta-analytic review. Work Stress 26(4):309–332
Nielsen MB, Knardahl S (2014) Coping strategies: a prospective study of patterns, stability, and relationships with psychological distress. Scand J Psychol 55(2):142–150
Powell DA et al (1990) Some determinants of attrition in prospective studies on aging. Exp Aging Res 16(1–2):17–24
Rogelberg SG, Stanton JM (2007) Understanding and dealing with organizational survey nonresponse—introduction. Organ Res Methods 10(2):195–209. doi:10.1177/1094428106294693
Sonne-Holm S, Sorensen TI, Jensen G, Schnohr P (1989) Influence of fatness, intelligence, education and sociodemographic factors on response rate in a health survey. J Epidemiol Community Health 43(4):369–374
Steingrimsdottir OA, Vollestad NK, Roe C, Knardahl S (2004) Variation in reporting of pain and other subjective health complaints in a working population and limitations of single sample measurements. Pain 110(1–2):130–139. doi:10.1016/j.pain.2004.03.016
Thygesen LC, Hvidtfeldt UA, Mikkelsen S, Bronnum-Hansen H (2011) Quantification of the healthy worker effect: a nationwide cohort study among electricians in Denmark. BMC Public Health 11:571. doi:10.1186/1471-2458-11-571
Acknowledgments
This study was funded by the Norwegian Research Council. The authors thank the participating companies for their willingness to participate, and Bjørn Lau, Anne Lene Andersen, Shahrooz Elka, Margrethe Schøning, Elisabeth Petersen, and Jan S. Emberland for their assistance in the survey administration.
Conflict of interest
The authors have no conflicts of interest related to the work described in this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nielsen, M.B., Knardahl, S. The healthy worker effect: Do health problems predict participation rates in, and the results of, a follow-up survey?. Int Arch Occup Environ Health 89, 231–238 (2016). https://doi.org/10.1007/s00420-015-1066-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00420-015-1066-6