Abstract
Purpose
To assess the incidence of pigment epithelial detachment (PED) in age-related macular degeneration (AMD) with submacular hemorrhage (SMH) and its response to treatment with pars plana vitrectomy (ppV), subretinal co-application of recombinant tissue plasminogen activator (rtPA) and anti-VEGF, and an intravitreal gas tamponade.
Methods
Consecutive interventional case series of 132 eyes of 129 patients with neovascular AMD with SMH. All eyes underwent ppV with subretinal co-application of rtPA and bevacizumab followed by a gas tamponade. Postoperatively, two additional intravitreal anti-VEGF injections were applied monthly, followed by intravitreal anti-VEGF injections applied PRN thereafter. PEDs and SMHs were evaluated with SD-OCT pre- and postoperatively.
Results
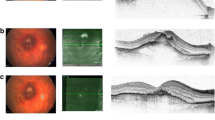
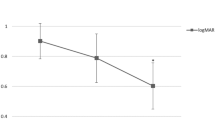
Preoperatively, 88 of 132 (67%) eyes were examined by OCT, and in 81 of these eyes the RPE could be visualised. A PED was found in 74 (91%) eyes, and no PED was found in five (6%) eyes. Median height of preoperative PED was 503 μm (range 150–1242, n = 65) and reduced to 344 (n = 62) and 306 μm (n = 27) after 3 and 12 months respectively. Two eyes showed a pre-existing rip of the RPE. Postoperatively, a rip was documented in 12 of 128 (9%) eyes. Median height of SMH was 762 μm (range 217–1840), median diameter was 4.3 (1.5-15) disc diameter. A complete displacement of the SMH from the fovea was achieved in 112 of 129 (87%) eyes. Overall, median best-corrected logMAR visual acuity (BCVA) improved significantly from preoperative 1.6 (0.5–2.0, n = 132) to 1.0 (0.2–2.0) 3 (n = 132) and 12 months (n = 74) postoperatively. Excluding eyes with pre-existing macular scars (n = 22), BCVA 3 months postoperatively was 0.8. Height of PED or SMH did not correlate with postoperatively BCVA, while size of SMH showed a mild correlation (rho = 0.25, p = 0.005).
Conclusion
PpV with subretinal co-application of rtPA and bevacizumab and an intravitreal gas tamponade effectively displaces SMH and improves BCVA. Preoperatively, PED is found in the majority of eyes. Height of PED or SMH did not correlate with postoperatively BCVA. Tears of the RPE occur as frequently as in exudative AMD without SMH.





Similar content being viewed by others
References
Pauleikhoff D, Löffert D, Spital G et al (2002) Pigment epithelial detachment in the elderly. Clinical differentiation, natural course and pathogenetic implications. Graefes Arch Clin Exp Ophthalmol 240:533–538
Baba T, Kitahashi M, Kubota-Taniai M et al (2012) Two-year course of subfoveal pigment epithelial detachment in eyes with age-related macular degeneration and visual acuity better than 20/40. Ophthalmologica 228:102–109
Dirani A, Ambresin A, Marchionno L et al (2015) Factors influencing the treatment response of pigment epithelium detachment in age-related macular degeneration. Am J Ophthalmol 160:732–738
Clemens CR, Eter N (2016) Retinal pigment epithelium tears: risk factors, mechanism and therapeutic monitoring. Ophthalmologica 235:1–9
Treumer F, Klatt C, Roider J, Hillenkamp J (2010) Subretinal coapplication of recombinant tissue plasminogen activator and bevacizumab for neovascular age-related macular degeneration with submacular haemorrhage. Br J Ophthalmol 94:48–53
Treumer F, Roider J, Hillenkamp J (2012) Long-term outcome of subretinal coapplication of rtPA and bevacizumab followed by repeated intravitreal anti-VEGF injections for neovascular AMD with submacular haemorrhage. Br J Ophthalmol 96:708–713
González-López JJ, McGowan G, Chapman E, Yorston D (2016) Vitrectomy with subretinal tissue plasminogen activator and ranibizumab for submacular haemorrhages secondary to age-related macular degeneration: retrospective case series of 45 consecutive cases. Eye (Lond Engl). doi:10.1038/eye.2016.65
Bach M, Kommerell G (1998) Determining visual acuity using European normal values: scientific principles and possibilities for automatic measurement. Klin Monatsbl Augenheilkd 212:190–195
Joussen AM, Heussen FMA, Joeres S et al (2006) Autologous translocation of the choroid and retinal pigment epithelium in age-related macular degeneration. Am J Ophthalmol 142:17–30
Heimes B, Lommatzsch A, Zeimer M et al (2011) Long-term visual course after anti-VEGF therapy for exudative AMD in clinical practice evaluation of the German reinjection scheme. Graefes Arch Clin Exp Ophthalmol 249:639–644
Stanescu-Segall D, Balta F, Jackson TL (2016) Submacular hemorrhage in neovascular age-related macular degeneration: a synthesis of the literature. Surv Ophthalmol 61:18–32
Sandhu SS, Manvikar S, Steel DHW (2010) Displacement of submacular hemorrhage associated with age-related macular degeneration using vitrectomy and submacular tPA injection followed by intravitreal ranibizumab. Clin Ophthalmol 4:637–642
Hillenkamp J, Surguch V, Framme C et al (2010) Management of submacular hemorrhage with intravitreal versus subretinal injection of recombinant tissue plasminogen activator. Graefes Arch Clin Exp Ophthalmol 248:5–11
Casswell AG, Kohen D, Bird AC (1985) Retinal pigment epithelial detachments in the elderly: classification and outcome. Br J Ophthalmol 69:397–403
Shah CP, Hsu J, Garg SJ et al (2006) Retinal pigment epithelial tear after intravitreal bevacizumab injection. Am J Ophthalmol 142:1070–1072
Singh RP, Sears JE (2006) Retinal pigment epithelial tears after pegaptanib injection for exudative age-related macular degeneration. Am J Ophthalmol 142:160–162
Saito M, Kano M, Itagaki K et al (2013) Retinal pigment epithelium tear after intravitreal aflibercept injection. Clin Ophthalmol Auckl NZ 7:1287–1289
Carvounis PE, Kopel AC, Benz MS (2007) Retinal pigment epithelium tears following ranibizumab for exudative age-related macular degeneration. Am J Ophthalmol 143:504–505
Chang LK, Flaxel CJ, Lauer AK, Sarraf D (2007) RPE tears after pegaptanib treatment in age-related macular degeneration. Retina Phila Pa 27:857–863
Sarraf D, Chan C, Rahimy E, Abraham P (2013) Prospective evaluation of the incidence and risk factors for the development of RPE tears after high- and low-dose ranibizumab therapy. Retina Phila Pa 33:1551–1557
Chan CK, Abraham P, Meyer CH et al (2010) Optical coherence tomography-measured pigment epithelial detachment height as a predictor for retinal pigment epithelial tears associated with intravitreal bevacizumab injections. Retina Phila Pa 30:203–211
Doguizi S, Ozdek S (2014) Pigment epithelial tears associated with anti-VEGF therapy: incidence, long-term visual outcome, and relationship with pigment epithelial detachment in age-related macular degeneration. Retina Phila Pa 34:1156–1162
Clemens CR, Bastian N, Alten F et al (2014) Prediction of retinal pigment epithelial tear in serous vascularized pigment epithelium detachment. Acta Ophthalmol (Copenh) 92:e50–56
Clemens CR, Alten F, Eter N (2015) Reading the signs: Microrips as a prognostic sign for impending RPE tear development. Acta Ophthalmol (Copenh) 93:e600–602
Mukai R, Sato T, Kishi S (2014) Precursor stage of retinal pigment epithelial tear in age-related macular degeneration. Acta Ophthalmol (Copenh) 92:e407–408
Lehmann B, Heimes B, Gutfleisch M et al (2015) Serous vascularized pigment epithelial detachment in exudative AMD. Morphological typing and risk of tears in the RPE. Ophthalmologe 112:49–56
Kim JH, Chang YS, Kim JW et al (2014) Intravitreal anti-vascular endothelial growth factor for submacular hemorrhage from choroidal neovascularization. Ophthalmology 121:926–935
CATT Research Group, Martin DF, Maguire MG (2011) Ranibizumab and bevacizumab for neovascular age-related macular degeneration. N Engl J Med 364:1897–1908
Acknowledgements
We thank Jürgen Hedderich from the Institute of Medical Informatics and Statistics, University Medical Center Schleswig-Holstein, Kiel, Germany for his help with the statistical calculations.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Funding
No funding was received for this research.
Ethical approval
The analysis have been approved by the institutional research ethics committee. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Treumer, F., Wienand, S., Purtskhvanidze, K. et al. The role of pigment epithelial detachment in AMD with submacular hemorrhage treated with vitrectomy and subretinal co-application of rtPA and anti-VEGF. Graefes Arch Clin Exp Ophthalmol 255, 1115–1123 (2017). https://doi.org/10.1007/s00417-017-3620-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-017-3620-2