Abstract
Objectives
To conduct a scoping review of the literature on psychological interventions directed to identify primary prevention strategies for depression among adult head and neck cancer (HNC) patients.
Methods
Systematic searches were conducted following Preferred Reporting Items for Systematic Reviews and Meta-Analysis Extension for Scoping Review including relevant studies within the PubMed, PsycINFO, and EMBASE databases. Two authors independently screened the searches and reviewed the included articles according to the predetermined eligibility criteria based on the PICOS format. Studies included subjects with previous or current diagnosis of depression were excluded. The risk of bias assessment of these trials was conducted following the Cochrane tool for assessing the risk of bias in randomized trials. The search was repeated prior to submission to ensure all current articles meeting criteria were included.
Results
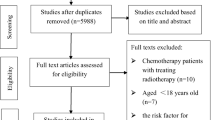
The search yielded 875 studies. The title and abstract screen, followed by the review of full texts identified five articles that met inclusion criteria. Four were randomized controlled trials (RCT) and the fifth was a non-randomized but controlled study. Different psychosocial interventions were used, including psycho-educational interventions, psychosocial counseling, and pharmacotherapy. All studies established the diagnosis of depression or screened for the diagnosis using standardized psychiatric assessment tools, either Diagnostic and Statistical Manual of Mental Disorders criteria or validated patient reported outcome measures. The average follow-up periods after intervention was 9.8 months. There was a significant decrease in the incidence of depression or depressive symptoms favoring the intervention group in three out of the five studies that were included.
Conclusion
Psychological interventions identified thus far studying primary prevention of depression in HNC patients show promising results. However, the paucity of data and heterogeneity of the interventions challenges the ability to compare the prevention modalities and outcomes. Future well-designed RCTs with large sample sizes are recommended to better conclude a result of effectiveness.


Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249
Howren MB, Christensen AJ, Karnell LH, Funk GF (2013) Psychological factors associated with head and neck cancer treatment and survivorship: evidence and opportunities for behavioral medicine. J Consult Clin Psychol 81(2):299–317
Sehlen S, Lenk M, Herschbach P, Aydemir U, Dellian M, Schymura B, Hollenhorst H, Dühmke E (2003) Depressive symptoms during and after radiotherapy for head and neck cancer. Head Neck 25(12):1004–1018
Lue BH, Huang TS, Chen HJ (2008) Physical distress, emotional status, and quality of life in patients with nasopharyngeal cancer complicated by post-radiotherapy endocrinopathy. Int J Radiat Oncol Biol Phys 70(1):28–34
Wagner KD, Robb AS, Findling RL, Jin J, Gutierrez MM, Heydorn WE (2004) A randomized, placebo-controlled trial of citalopram for the treatment of major depression in children and adolescents. Am J Psychiatry 161(6):1079–1083
Barber B, Dergousoff J, Slater L, Harris J, O’Connell D, El-Hakim H, Biron VL, Mitchell N, Seikaly H (2016) Depression and survival in patients with head and neck cancer: a systematic review. JAMA Otolaryngol Head Neck Surg 142(3):284–288
Ehlers SL (2002) Effects of depression and substance use on head and neck cancer mortality. The University of Iowa, Iowa
Lazure KE, Lydiatt WM, Denman D, Burke WJ (2009) Association between depression and survival or disease recurrence in patients with head and neck cancer enrolled in a depression prevention trial. Head Neck 31(7):888–892
Rieke K, Schmid KK, Lydiatt W, Houfek J, Boilesen E, Watanabe-Galloway S (2017) Depression and survival in head and neck cancer patients. Oral Oncol 65:76–82
Kam D, Salib A, Gorgy G, Patel TD, Carniol ET, Eloy JA, Baredes S, Park RC (2015) Incidence of suicide in patients with head and neck cancer. JAMA Otolaryngol Head Neck Surg 141(12):1075–1081
Osazuwa-Peters N, Simpson MC, Zhao L, Boakye EA, Olomukoro SI, Deshields T, Loux TM, Varvares MA, Schootman M (2018) Suicide risk among cancer survivors: head and neck versus other cancers. Cancer 124(20):4072–4079
Semple C, Parahoo K, Norman A, McCaughan E, Humphris G, Mills M (2013) Psychosocial interventions for patients with head and neck cancer. Cochrane Database Syst Rev 7:CD009441
Fawzy FIFN, Arndt LA, Pasnau RO (1995) Critical review of psychosocial interventions in cancer care. Arch Gen Psychiatry 52(2):100–113
Duffy SA, Ronis DL, Valenstein M, Lambert MT, Fowler KE, Gregory L, Bishop C, Myers LL, Blow FC, Terrell JE (2006) A tailored smoking, alcohol, and depression intervention for head and neck cancer patients. Cancer Epidemiol Biomark Prev 15(11):2203–2208
Kisling LA, MD J (2022) Prevention strategies. In: StatPearls. StatPearls Publishing LLC, Treasure Island
Lydiatt WM, Denman D, McNeilly DP, Puumula SE, Burke WJ (2008) A randomized, placebo-controlled trial of citalopram for the prevention of major depression during treatment for head and neck cancer. Arch Otolaryngol Head Neck Surg 134(5):528–535
McLaughlin KA (2011) The public health impact of major depression: a call for interdisciplinary prevention efforts. Prev Sci 12(4):361–371
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, Cates CJ, Cheng HY, Corbett MS, Eldridge SM et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Methods guide for effectiveness and comparative effectiveness reviews. https://effectivehealthcare.ahrq.gov/products/collections/cer-methods-guide
Lydiatt WM, Bessette D, Schmid KK, Sayles H, Burke WJ (2013) Prevention of depression with escitalopram in patients undergoing treatment for head and neck cancer: randomized, double-blind, placebo-controlled clinical trial. JAMA Otolaryngol Head Neck Surg 139(7):678–686
Katz MR, Irish JC, Devins GM (2004) Development and pilot testing of a psychoeducational intervention for oral cancer patients. Psychooncology 13(9):642–653
D’Souza V, Blouin E, Zeitouni A, Muller K, Allison PJ (2013) An investigation of the effect of tailored information on symptoms of anxiety and depression in head and neck cancer patients. Oral Oncol 49(5):431–437
Zigmond AS, Snaith RP (1983) The hospital anxiety and depression scale. Acta Psychiatr Scand 67(6):361–370
Snaith RP, Zigmond AS (1986) The hospital anxiety and depression scale. Br Med J (Clin Res Ed) 292(6516):344
van der Meulen IC, May AM, de Leeuw JR, Koole R, Oosterom M, Hordijk GJ, Ros WJ (2014) Long-term effect of a nurse-led psychosocial intervention on health-related quality of life in patients with head and neck cancer: a randomised controlled trial. Br J Cancer 110(3):593–601
Yadav P, Karkal R, Kakunje A, Mahatme N, Akhilesh M (2019) Prevalence of depressive disorders among head-and-neck cancer patients: a hospital-based, cross-sectional study. Indian J Psychiatry 61(4):409–414
Robinson RG, Jorge RE, Long J (2017) Prevention of poststroke mortality using problem-solving therapy or escitalopram. Am J Geriatr Psychiatry 25(5):512–519
Lewinsohn PM, Seeley JR, Roberts RE, Allen NB (1997) Center for Epidemiologic Studies Depression Scale (CES-D) as a screening instrument for depression among community-residing older adults. Psychol Aging 12(2):277–287
Radloff LS (1977) The CES-D Scale: a self-report depression scale for research in the general population. Appl Psychol Meas 1(3):385–401
Amster WW, Love RJ, Menzel OJ, Sandler J, Sculthorpe WB, Gross FM (1972) Psychosocial factors and speech after laryngectomy. J Commun Disord 5(1):1–18
Blanchard SL (1982) Current practices in the counseling of the laryngectomy patient. J Commun Disord 15(3):233–241
Carroll-Alfano MA (2019) Education, counseling, support groups, and provider knowledge of total laryngectomy: the patient’s perspective. J Commun Disord 82:105938
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Arif, R., Marzouki, H.Z., Silver, J.A. et al. Primary prevention of depression in head and neck cancer patients: a scoping review. Eur Arch Otorhinolaryngol 280, 1547–1554 (2023). https://doi.org/10.1007/s00405-022-07783-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-022-07783-z