Abstract
Introduction
Postoperative cognitive dysfunction (POCD) occurs in up to 26% of patients older than 60 years 1 week after non-cardiac surgery. Intraoperative beach chair positioning (BCP) is advantageous for some types of shoulder surgery. However, this kind of positioning leads to a downward bound redistribution of blood volume, with possible hypoperfusion of the brain. We hypothesized that patients > 60 years undergoing orthopaedic shoulder surgery in a BCP might experience more POCD than patients operated in the supine position (SP).
Material and methods
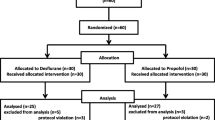
A single-centre, prospective observational trial of 114 orthopaedic patients was performed. Study groups were established according to the type of intraoperative positioning. Anaesthesiological management was carried out similarly in both groups, including types of anaesthetics and blood pressure levels. POCD was evaluated using the Trail Making Test, the Letter–Number Span and the Regensburger Word Fluency Test. The frequency of POCD 1 week after surgery was considered primary outcome.
Results
Baseline characteristics, including duration of surgery, were comparable in both groups. POCD after 1 week occurred in 10.5% of SP patients and in 21.1% of BCP patients (p = 0.123; hazard ratio 2.0 (CI 95% 0.794–5.038)). After 4 weeks, the incidence of POCD decreased (SP: 8.8% vs. BCP: 5.3%; p = 0.463). 12/18 patients with POCD showed changes in their Word Fluency Tests. Near-infrared spectroscopy (NIRS) values were not lower in patients with POCD compared to those without POCD (54% (50/61) vs. 57% (51/61); p = 0.671).
Conclusion
POCD at 1 week after surgery tended to occur more often in patients operated in beach chair position compared to patients in supine position without being statistically significant.
Similar content being viewed by others
Data availability
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
References
Peruto CM, Ciccotti MG, Cohen SB (2009) Shoulder arthroscopy positioning: lateral decubitus versus beach chair. Arthroscopy 25:891–896. https://doi.org/10.1016/j.arthro.2008.10.003
Buget MI, Atalar AC, Edipoglu IS et al (2016) Patient state index and cerebral blood flow changes during shoulder arthroscopy in beach chair position. Braz J Anesthesiol (Elsevier) 66:470–474
Hanouz J-L, Fiant A-L, Gérard J-L (2016) Middle cerebral artery blood flow velocity during beach chair position for shoulder surgery under general anesthesia. J Clin Anesth 33:31–36
Moerman AT, De Hert SG (2012) Utility of near-infrared spectroscopy for assessing cerebral oxygen saturation during beach chair position. Anesthesiology 117:1395 (author reply 1396)
Goettel N, Patet C, Rossi A et al (2016) Monitoring of cerebral blood flow autoregulation in adults undergoing sevoflurane anesthesia: a prospective cohort study of two age groups. J Clin Monit Comput 30:255–264. https://doi.org/10.1007/s10877-015-9754-z
Slupe AM, Kirsch JR (2018) Effects of anesthesia on cerebral blood flow, metabolism, and neuroprotection. J Cereb Blood Flow Metab 38:2192–2208. https://doi.org/10.1177/0271678X18789273
Murphy GS, Greenberg SB, Szokol JW (2019) Safety of beach chair position shoulder surgery: a review of the current literature. Anesth Analg 129:101–118. https://doi.org/10.1213/ANE.0000000000004133
Gillespie R, Shishani Y, Streit J et al (2012) The safety of controlled hypotension for shoulder arthroscopy in the beach-chair position. J Bone Joint Surg Am 94:1284–1290. https://doi.org/10.2106/JBJS.J.01550
Pohl A, Cullen DJ (2005) Cerebral ischemia during shoulder surgery in the upright position: a case series. J Clin Anesth 17:463–469
Friedman DJ, Parnes NZ, Zimmer Z et al (2009) Prevalence of cerebrovascular events during shoulder surgery and association with patient position. Orthopedics. https://doi.org/10.3928/01477447-20090401-23
Pin-on P, Schroeder D, Munis J (2013) The hemodynamic management of 5177 neurosurgical and orthopedic patients who underwent surgery in the sitting or “beach chair” position without incidence of adverse neurologic events. Anesth Analg 116:1317–1324. https://doi.org/10.1213/ANE.0b013e31828446bb
Laflam A, Joshi B, Brady K et al (2015) Shoulder surgery in the beach chair position is associated with diminished cerebral autoregulation but no differences in postoperative cognition or brain injury biomarker levels compared with supine positioning: the anesthesia patient safety foundation beach chair study. Anesth Analg 120:176–185
Larsen JR, Kobborg T, Shahim P et al (2021) Serum-neuroproteins, near-infrared spectroscopy, and cognitive outcome after beach-chair shoulder surgery: observational cohort study analyses. Acta Anaesthesiol Scand 65:26–33. https://doi.org/10.1111/aas.13691
Aguirre JA, Märzendorfer O, Brada M et al (2016) Cerebral oxygenation in the beach chair position for shoulder surgery in regional anesthesia: impact on cerebral blood flow and neurobehavioral outcome. J Clin Anesth 35:456–464
Aguirre J, Borgeat A, Trachsel T et al (2014) Cerebral oxygenation in patients undergoing shoulder surgery in beach chair position: comparing general to regional anesthesia and the impact on neurobehavioral outcome. Rev Esp Anestesiol Reanim 61:64–72
Salazar D, Sears BW, Aghdasi B et al (2013) Cerebral desaturation events during shoulder arthroscopy in the beach chair position: patient risk factors and neurocognitive effects. J Shoulder Elbow Surg 22:1228–1235
Golz AG, Davis WJ, Perry MW et al (2020) Improving the safety of shoulder arthroscopy in the beach chair position: a prospective randomized trial investigating the effect of compression stockings on cerebral desaturation events in obese patients. J Shoulder Elbow Surg 29:2027–2035. https://doi.org/10.1016/j.jse.2020.05.037
Schmidt K-H, Metzler P (1992) Wortschatztest. Beltz Test, Weinheim
Reitan RM (1994) Ward Halstead’s contributions to neuropsychology and the Halstead-Reitan neuropsychological test battery. J Clin Psychol 50(1):47–70
Dumont R, Willis JO, Veizel K, Zibulsky J (2014) Wechsler adult intelligence scale–fourth edition. encyclopedia of special education. In: Reynolds CR, Vannest KJ, Fletcher‐Janzen E (eds) Encyclopedia of special education: a reference for the education of children, adolescents, and adults with disabilities and other exceptional individuals. Wiley, Hoboken
Aschenbrenner S, Tucha O, Lange K, Harth S (2004) Regensburger Wortflüssigkeitstest. Z Neuropsychol 15:315–321
Moller JT, Cluitmans P, Rasmussen LS et al (1998) Long-term postoperative cognitive dysfunction in the elderly ISPOCD1 study. ISPOCD investigators. international study of post-operative cognitive dysfunction. Lancet 351:857–861
Canet J, Raeder J, Rasmussen LS et al (2003) Cognitive dysfunction after minor surgery in the elderly. Acta Anaesthesiol Scand 47:1204–1210
Cox RM, Jamgochian GC, Nicholson K et al (2018) The effectiveness of cerebral oxygenation monitoring during arthroscopic shoulder surgery in the beach chair position: a randomized blinded study. J Shoulder Elbow Surg 27:692–700. https://doi.org/10.1016/j.jse.2017.11.004
Salazar D, Hazel A, Tauchen AJ et al (2016) Neurocognitive deficits and cerebral desaturation during shoulder arthroscopy with patient in beach-chair position: a review of the current literature. Am J Orthop 45:E63–E68
Gilotra MN, Klein A, Elkassabany N et al (2019) Risk factors for cerebral desaturation events during shoulder surgery in the beach chair position. Arthroscopy 35:725–730. https://doi.org/10.1016/j.arthro.2018.10.123
Murphy GS, Szokol JW, Marymont JH et al (2010) Cerebral oxygen desaturation events assessed by near-infrared spectroscopy during shoulder arthroscopy in the beach chair and lateral decubitus positions. Anesth Analg 111:496–505
Rasmussen LS, Johnson T, Kuipers HM et al (2003) Does anaesthesia cause postoperative cognitive dysfunction? a randomised study of regional versus general anaesthesia in 438 elderly patients. Acta Anaesthesiol Scand 47:260–266. https://doi.org/10.1034/j.1399-6576.2003.00057.x
Liu J, Huang K, Zhu B et al (2021) Neuropsychological tests in post-operative cognitive dysfunction: methods and applications. Front Psychol 12:684307. https://doi.org/10.3389/fpsyg.2021.684307
Aguirre JA, Etzensperger F, Brada M et al (2019) The beach chair position for shoulder surgery in intravenous general anesthesia and controlled hypotension: Impact on cerebral oxygenation, cerebral blood flow and neurobehavioral outcome. J Clin Anesth 53:40–48. https://doi.org/10.1016/j.jclinane.2018.09.035
Frey K, Rehm M, Chappell D et al (2018) Preemptive volume therapy to prevent hemodynamic changes caused by the beach chair position: hydroxyethyl starch 130/0.4 versus Ringer’s acetate-a controlled randomized trial. J Shoulder Elbow Surg 27:2129–2138
Rains DD, Rooke GA, Wahl CJ (2011) Pathomechanisms and complications related to patient positioning and anesthesia during shoulder arthroscopy. Arthroscopy 27:532–541. https://doi.org/10.1016/j.arthro.2010.09.008
Nakano M, Nomura Y, Whitman G et al (2021) Cerebral autoregulation in the operating room and intensive care unit after cardiac surgery. Br J Anaesth 126:967–974. https://doi.org/10.1016/j.bja.2020.12.043
Kahl U, Rademacher C, Harler U et al (2021) Intraoperative impaired cerebrovascular autoregulation and delayed neurocognitive recovery after major oncologic surgery: a secondary analysis of pooled data. J Clin Monit Comput. https://doi.org/10.1007/s10877-021-00706-z
Greene NH, Lee LA (2012) Modern and evolving understanding of cerebral perfusion and autoregulation. Adv Anesth 30:97–129
Dippmann C, Winge S, Nielsen HB (2010) Severe cerebral desaturation during shoulder arthroscopy in the beach-chair position. Arthroscopy 26:S148–S150
Salazar DH, Davis WJ, Ziroğlu N, Garbis NG (2019) Cerebral desaturation events during shoulder arthroscopy in the beach chair position. J Am Acad Orthop Surg Glob Res Rev 3:e007. https://doi.org/10.5435/JAAOSGlobal-D-19-00007
Punjasawadwong Y, Chau-In W, Laopaiboon M et al (2018) Processed electroencephalogram and evoked potential techniques for amelioration of postoperative delirium and cognitive dysfunction following non-cardiac and non-neurosurgical procedures in adults. Cochrane Database Syst Rev 5:11283. https://doi.org/10.1002/14651858.CD011283.pub2
Evered LA, Chan MTV, Han R et al (2021) Anaesthetic depth and delirium after major surgery: a randomised clinical trial. Br J Anaesth. https://doi.org/10.1016/j.bja.2021.07.021
Xu N, Li L-X, Wang T-L et al (2021) Processed multiparameter electroencephalogram-guided general anesthesia management can reduce postoperative delirium following carotid endarterectomy: a randomized clinical trial. Front Neurol 12:666814. https://doi.org/10.3389/fneur.2021.666814
Ling L, Yang TX, Lee SWK (2022) Effect of anaesthesia depth on postoperative delirium and postoperative cognitive dysfunction in high-risk patients: a systematic review and meta-analysis. Cureus 14:e30120. https://doi.org/10.7759/cureus.30120
Acknowledgements
The authors thank PD Dr. Karch for helping us select psychometric testing methods and we would like to thank all staff of the operating theatre and the wards who supported the team.
Funding
This study was funded in part by an internal grant from the Ludwig-Maximilians-University to Philipp Groene. Förderung Forschung und Lehre (FöFoLe).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests to declare that are relevant to the content of this article.
Ethical approval
This study was registered at the German clinical trials database (ID: DRKS00015271), and the study protocol was approved by the Ludwig-Maximilians-University’s ethics committee (No 18-558). This study was performed in accordance with the Declaration of Helsinki, with written informed consent being obtained from all participants before they undertook any of the study procedures.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Groene, P., Schaller, T., Zeuzem-Lampert, C. et al. Postoperative cognitive dysfunction after beach chair positioning compared to supine position in orthopaedic surgery in the elderly. Arch Orthop Trauma Surg 144, 575–581 (2024). https://doi.org/10.1007/s00402-023-05109-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-05109-0