Abstract
Purpose
Ferroptosis is a form of regulated cell death that has the potential to be targeted as a cancer therapeutic strategy. But cancer cells have a wide range of sensitivities to ferroptosis, which limits its therapeutic potential. Accumulation of lipid peroxides determines the occurrence of ferroptosis. However, the type of lipid involved in peroxidation and the mechanism of lipid peroxide accumulation are less studied.
Methods
The effects of fatty acids (10 μM) with different carbon chain length and unsaturation on ferroptosis were evaluated by MTT and LDH release assay in cell lines derived from prostate cancer (PC3, 22RV1, DU145 and LNCaP), colorectal cancer (HT-29), cervical cancer (HeLa) and liver cancer (HepG2). Inhibitors of apoptosis, necroptosis, autophagy and ferroptosis were used to determine the type of cell death. Then the regulation of reactive oxygen species (ROS) and lipid peroxidation by docosahexaenoic acid (DHA) was measured by HPLC–MS and flow cytometry. The avtive form of DHA was determined by siRNA mediated gene silencing. The role of lipoxygenases was checked by inhibitors and gene silencing. Finally, the effect of DHA on ferroptosis-mediated tumor killing was verified in xenografts.
Results
The sensitivity of ferroptosis was positively correlated with the unsaturation of exogenously added fatty acid. DHA (22:6 n-3) sensitized cancer cells to ferroptosis-inducing reagents (FINs) at the highest level in vitro and in vivo. In this process, DHA increased ROS accumulation, lipid peroxidation and protein oxidation independent of its membrane receptor, GPR120. Inhibition of long chain fatty acid-CoA ligases and lysophosphatidylcholine acyltransferases didn't affect the role of DHA. DHA-involved ferroptosis can be induced in both arachidonate lipoxygenase 5 (ALOX5) negative and positive cells. Down regulation of ALOX5 inhibited ferroptosis, while overexpression of ALOX5 promoted ferroptosis.
Conclusion
DHA can effectively promote ferroptosis-mediated tumor killing by increasing intracellular lipid peroxidation. Both ALOX5 dependent and independent pathways are involved in DHA-FIN induced ferroptosis. And during this process, free DHA plays an important role.






Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this manuscript.
Abbreviations
- PUFA:
-
Polyunsaturated fatty acid
- DHA:
-
Docosahexaenoic acid
- FIN:
-
Ferroptosis-inducing reagent
- ROS:
-
Reactive oxygen species
- LPO:
-
Lipid peroxide
- GPX4:
-
Glutathione peroxidase 4
- ALOX:
-
Arachidonate lipoxygenase
References
Stockwell BR, Friedmann Angeli JP, Bayir H, Bush AI, Conrad M, Dixon SJ, Fulda S, Gascon S, Hatzios SK, Kagan VE, Noel K, Jiang X, Linkermann A, Murphy ME, Overholtzer M, Oyagi A, Pagnussat GC, Park J, Ran Q, Rosenfeld CS, Salnikow K, Tang D, Torti FM, Torti SV, Toyokuni S, Woerpel KA, Zhang DD (2017) Ferroptosis: a regulated cell death nexus linking metabolism, redox biology, and disease. Cell 171(2):273–285. https://doi.org/10.1016/j.cell.2017.09.021
Dixon SJ, Lemberg KM, Lamprecht MR, Skouta R, Zaitsev EM, Gleason CE, Patel DN, Bauer AJ, Cantley AM, Yang WS, Morrison B 3rd, Stockwell BR (2012) Ferroptosis: an iron-dependent form of nonapoptotic cell death. Cell 149(5):1060–1072. https://doi.org/10.1016/j.cell.2012.03.042
Palacin M, Nunes V, Font-Llitjos M, Jimenez-Vidal M, Fort J, Gasol E, Pineda M, Feliubadalo L, Chillaron J, Zorzano A (2005) The genetics of heteromeric amino acid transporters. Physiology (Bethesda) 20:112–124. https://doi.org/10.1152/physiol.00051.2004
Dixon SJ, Patel DN, Welsch M, Skouta R, Lee ED, Hayano M, Thomas AG, Gleason CE, Tatonetti NP, Slusher BS, Stockwell BR (2014) Pharmacological inhibition of cystine-glutamate exchange induces endoplasmic reticulum stress and ferroptosis. Elife 3:e02523. https://doi.org/10.7554/eLife.02523
Brigelius-Flohe R, Maiorino M (2013) Glutathione peroxidases. Biochim Biophys Acta 1830(5):3289–3303. https://doi.org/10.1016/j.bbagen.2012.11.020
Imai H, Matsuoka M, Kumagai T, Sakamoto T, Koumura T (2017) Lipid peroxidation-dependent cell death regulated by GPx4 and ferroptosis. Curr Top Microbiol Immunol 403:143–170. https://doi.org/10.1007/82_2016_508
Yang WS, SriRamaratnam R, Welsch ME, Shimada K, Skouta R, Viswanathan VS, Cheah JH, Clemons PA, Shamji AF, Clish CB, Brown LM, Girotti AW, Cornish VW, Schreiber SL, Stockwell BR (2014) Regulation of ferroptotic cancer cell death by GPX4. Cell 156(1–2):317–331. https://doi.org/10.1016/j.cell.2013.12.010
Yang WS, Stockwell BR (2015) Ferroptosis: death by lipid peroxidation. Trends Cell Biol. https://doi.org/10.1016/j.tcb.2015.10.014
Cramer SL, Saha A, Liu J, Tadi S, Tiziani S, Yan W, Triplett K, Lamb C, Alters SE, Rowlinson S, Zhang YJ, Keating MJ, Huang P, DiGiovanni J, Georgiou G, Stone E (2017) Systemic depletion of L-cyst(e)ine with cyst(e)inase increases reactive oxygen species and suppresses tumor growth. Nat Med 23(1):120–127. https://doi.org/10.1038/nm.4232
Liu DS, Duong CP, Haupt S, Montgomery KG, House CM, Azar WJ, Pearson HB, Fisher OM, Read M, Guerra GR, Haupt Y, Cullinane C, Wiman KG, Abrahmsen L, Phillips WA, Clemons NJ (2017) Inhibiting the system xC(-)/glutathione axis selectively targets cancers with mutant-p53 accumulation. Nat Commun 8:14844. https://doi.org/10.1038/ncomms14844
Dolma S, Lessnick SL, Hahn WC, Stockwell BR (2003) Identification of genotype-selective antitumor agents using synthetic lethal chemical screening in engineered human tumor cells. Cancer Cell 3(3):285–296
Yang WS, Stockwell BR (2008) Synthetic lethal screening identifies compounds activating iron-dependent, nonapoptotic cell death in oncogenic-RAS-harboring cancer cells. Chem Biol 15(3):234–245. https://doi.org/10.1016/j.chembiol.2008.02.010
Sun X, Ou Z, Chen R, Niu X, Chen D, Kang R, Tang D (2016) Activation of the p62-Keap1-NRF2 pathway protects against ferroptosis in hepatocellular carcinoma cells. Hepatology 63(1):173–184. https://doi.org/10.1002/hep.28251
Eling N, Reuter L, Hazin J, Hamacher-Brady A, Brady NR (2015) Identification of artesunate as a specific activator of ferroptosis in pancreatic cancer cells. Oncoscience 2(5):517–532. https://doi.org/10.18632/oncoscience.160
Tesfay L, Paul BT, Konstorum A, Deng Z, Cox AO, Lee J, Furdui CM, Hegde P, Torti FM, Torti SV (2019) Steroyl-CoA desaturase 1 (SCD1) protects ovarian cancer cells from ferroptotic cell death. Cancer Res. https://doi.org/10.1158/0008-5472.CAN-19-0369
Alvarez SW, Sviderskiy VO, Terzi EM, Papagiannakopoulos T, Moreira AL, Adams S, Sabatini DM, Birsoy K, Possemato R (2017) NFS1 undergoes positive selection in lung tumours and protects cells from ferroptosis. Nature 551(7682):639–643. https://doi.org/10.1038/nature24637
Sporn MB, Liby KT (2012) NRF2 and cancer: the good, the bad and the importance of context. Nat Rev Cancer 12(8):564–571. https://doi.org/10.1038/nrc3278
Zhu S, Zhang Q, Sun X, Zeh HJ 3rd, Lotze MT, Kang R, Tang D (2017) HSPA5 regulates ferroptotic cell death in cancer cells. Cancer Res 77(8):2064–2077. https://doi.org/10.1158/0008-5472.CAN-16-1979
Berquin IM, Edwards IJ, Kridel SJ, Chen YQ (2011) Polyunsaturated fatty acid metabolism in prostate cancer. Cancer Metastasis Rev 30(3–4):295–309. https://doi.org/10.1007/s10555-011-9299-7
Rogers KR, Kikawa KD, Mouradian M, Hernandez K, McKinnon KM, Ahwah SM, Pardini RS (2010) Docosahexaenoic acid alters epidermal growth factor receptor-related signaling by disrupting its lipid raft association. Carcinogenesis 31(9):1523–1530. https://doi.org/10.1093/carcin/bgq111
So WW, Liu WN, Leung KN (2015) Omega-3 polyunsaturated fatty acids trigger cell cycle arrest and induce apoptosis in human neuroblastoma LA-N-1 cells. Nutrients 7(8):6956–6973. https://doi.org/10.3390/nu7085319
Pettersen K, Monsen VT, Hakvag Pettersen CH, Overland HB, Pettersen G, Samdal H, Tesfahun AN, Lundemo AG, Bjorkoy G, Schonberg SA (2016) DHA-induced stress response in human colon cancer cells—focus on oxidative stress and autophagy. Free Radic Biol Med 90:158–172. https://doi.org/10.1016/j.freeradbiomed.2015.11.018
Murphy RA, Mourtzakis M, Chu QS, Baracos VE, Reiman T, Mazurak VC (2011) Supplementation with fish oil increases first-line chemotherapy efficacy in patients with advanced nonsmall cell lung cancer. Cancer 117(16):3774–3780. https://doi.org/10.1002/cncr.25933
Chen YQ, Edwards IJ, Kridel SJ, Thornburg T, Berquin IM (2007) Dietary fat-gene interactions in cancer. Cancer Metastasis Rev 26(3–4):535–551. https://doi.org/10.1007/s10555-007-9075-x
Yang WS, Kim KJ, Gaschler MM, Patel M, Shchepinov MS, Stockwell BR (2016) Peroxidation of polyunsaturated fatty acids by lipoxygenases drives ferroptosis. Proc Natl Acad Sci USA 113(34):E4966-4975. https://doi.org/10.1073/pnas.1603244113
Magtanong L, Ko PJ, Dixon SJ (2016) Emerging roles for lipids in non-apoptotic cell death. Cell Death Differ 23(7):1099–1109. https://doi.org/10.1038/cdd.2016.25
Kagan VE, Mao G, Qu F, Angeli JP, Doll S, Croix CS, Dar HH, Liu B, Tyurin VA, Ritov VB, Kapralov AA, Amoscato AA, Jiang J, Anthonymuthu T, Mohammadyani D, Yang Q, Proneth B, Klein-Seetharaman J, Watkins S, Bahar I, Greenberger J, Mallampalli RK, Stockwell BR, Tyurina YY, Conrad M, Bayir H (2017) Oxidized arachidonic and adrenic PEs navigate cells to ferroptosis. Nat Chem Biol 13(1):81–90. https://doi.org/10.1038/nchembio.2238
Yoo SE, Chen L, Na R, Liu Y, Rios C, Van Remmen H, Richardson A, Ran Q (2012) Gpx4 ablation in adult mice results in a lethal phenotype accompanied by neuronal loss in brain. Free Radic Biol Med 52(9):1820–1827. https://doi.org/10.1016/j.freeradbiomed.2012.02.043
Ueta T, Inoue T, Furukawa T, Tamaki Y, Nakagawa Y, Imai H, Yanagi Y (2012) Glutathione peroxidase 4 is required for maturation of photoreceptor cells. J Biol Chem 287(10):7675–7682. https://doi.org/10.1074/jbc.M111.335174
Haeggstrom JZ, Funk CD (2011) Lipoxygenase and leukotriene pathways: biochemistry, biology, and roles in disease. Chem Rev 111(10):5866–5898. https://doi.org/10.1021/cr200246d
Doll S, Proneth B, Tyurina YY, Panzilius E, Kobayashi S, Ingold I, Irmler M, Beckers J, Aichler M, Walch A, Prokisch H, Trumbach D, Mao G, Qu F, Bayir H, Fullekrug J, Scheel CH, Wurst W, Schick JA, Kagan VE, Angeli JP, Conrad M (2017) ACSL4 dictates ferroptosis sensitivity by shaping cellular lipid composition. Nat Chem Biol 13(1):91–98. https://doi.org/10.1038/nchembio.2239
Basavarajappa D, Wan M, Lukic A, Steinhilber D, Samuelsson B, Radmark O (2014) Roles of coactosin-like protein (CLP) and 5-lipoxygenase-activating protein (FLAP) in cellular leukotriene biosynthesis. Proc Natl Acad Sci U S A 111(31):11371–11376. https://doi.org/10.1073/pnas.1410983111
Ruan Q, Chen Y, Kong X, Hua Y (2013) Comparative studies on sulfhydryl determination of soy protein using two aromatic disulfide reagents and two fluorescent reagents. J Agric Food Chem 61(11):2661–2668. https://doi.org/10.1021/jf303005y
Soglia F, Petracci M, Ertbjerg P (2016) Novel DNPH-based method for determination of protein carbonylation in muscle and meat. Food Chem 197(Pt A):670–675. https://doi.org/10.1016/j.foodchem.2015.11.038
Lu H, Chen H, Tang X, Yang Q, Zhang H, Chen YQ, Chen W (2019) Ultra performance liquid chromatography-Q exactive Orbitrap/mass spectrometry-based lipidomics reveals the influence of nitrogen sources on lipid biosynthesis of Mortierella alpina. J Agric Food Chem 67(39):10984–10993. https://doi.org/10.1021/acs.jafc.9b04455
Arienti G, Carlini E, Polci A, Cosmi EV, Palmerini CA (1998) Fatty acid pattern of human prostasome lipid. Arch Biochem Biophys 358(2):391–395. https://doi.org/10.1006/abbi.1998.0876
Faas FH, Dang AQ, Pollard M, Hong XM, Fan K, Luckert PH, Schutz M (1996) Increased phospholipid fatty acid remodeling in human and rat prostatic adenocarcinoma tissues. J Urol 156(1):243–248
Weisser H, Krieg M (1998) Fatty acid composition of phospholipids in epithelium and stroma of human benign prostatic hyperplasia. Prostate 36(4):235–243. https://doi.org/10.1002/(sici)1097-0045(19980901)36:4%3c235::aid-pros4%3e3.0.co;2-e
Andersson A, Nalsen C, Tengblad S, Vessby B (2002) Fatty acid composition of skeletal muscle reflects dietary fat composition in humans. Am J Clin Nutr 76(6):1222–1229. https://doi.org/10.1093/ajcn/76.6.1222
Martinez M, Mougan I (1998) Fatty acid composition of human brain phospholipids during normal development. J Neurochem 71(6):2528–2533. https://doi.org/10.1046/j.1471-4159.1998.71062528.x
Cunnane SC, Schneider JA, Tangney C, Tremblay-Mercier J, Fortier M, Bennett DA, Morris MC (2012) Plasma and brain fatty acid profiles in mild cognitive impairment and Alzheimer’s disease. J Alzheimers Dis 29(3):691–697. https://doi.org/10.3233/JAD-2012-110629
Fraser T, Tayler H, Love S (2010) Fatty acid composition of frontal, temporal and parietal neocortex in the normal human brain and in Alzheimer’s disease. Neurochem Res 35(3):503–513. https://doi.org/10.1007/s11064-009-0087-5
Hamazaki K, Hamazaki T, Inadera H (2013) Abnormalities in the fatty acid composition of the postmortem entorhinal cortex of patients with schizophrenia, bipolar disorder, and major depressive disorder. Psychiatry Res 210(1):346–350. https://doi.org/10.1016/j.psychres.2013.05.006
Abbott SK, Jenner AM, Spiro AS, Batterham M, Halliday GM, Garner B (2015) Fatty acid composition of the anterior cingulate cortex indicates a high susceptibility to lipid peroxidation in Parkinson’s disease. J Parkinsons Dis 5(1):175–185. https://doi.org/10.3233/JPD-140479
Zhang L, Han L, He J, Lv J, Pan R, Lv T (2020) A high serum-free fatty acid level is associated with cancer. J Cancer Res Clin Oncol 146(3):705–710. https://doi.org/10.1007/s00432-019-03095-8
Das M, Das S (2016) Identification of cytotoxic mediators and their putative role in the signaling pathways during docosahexaenoic acid (DHA)-induced apoptosis of cancer cells. Apoptosis 21(12):1408–1421. https://doi.org/10.1007/s10495-016-1298-2
Johansson I, Monsen VT, Pettersen K, Mildenberger J, Misund K, Kaarniranta K, Schonberg S, Bjorkoy G (2015) The marine n-3 PUFA DHA evokes cytoprotection against oxidative stress and protein misfolding by inducing autophagy and NFE2L2 in human retinal pigment epithelial cells. Autophagy 11(9):1636–1651. https://doi.org/10.1080/15548627.2015.1061170
Valencak TG, Ruf T (2007) N-3 polyunsaturated fatty acids impair lifespan but have no role for metabolism. Aging Cell 6(1):15–25. https://doi.org/10.1111/j.1474-9726.2006.00257.x
Marullo R, Werner E, Degtyareva N, Moore B, Altavilla G, Ramalingam SS, Doetsch PW (2013) Cisplatin induces a mitochondrial-ROS response that contributes to cytotoxicity depending on mitochondrial redox status and bioenergetic functions. PLoS ONE 8(11):e81162. https://doi.org/10.1371/journal.pone.0081162
Ichikawa Y, Ghanefar M, Bayeva M, Wu R, Khechaduri A, Naga Prasad SV, Mutharasan RK, Naik TJ, Ardehali H (2014) Cardiotoxicity of doxorubicin is mediated through mitochondrial iron accumulation. J Clin Investig 124(2):617–630. https://doi.org/10.1172/JCI72931
Gutierrez-Uzquiza A, Arechederra M, Bragado P, Aguirre-Ghiso JA, Porras A (2012) p38alpha mediates cell survival in response to oxidative stress via induction of antioxidant genes: effect on the p70S6K pathway. J Biol Chem 287(4):2632–2642. https://doi.org/10.1074/jbc.M111.323709
Shin S, Jing K, Jeong S, Kim N, Song KS, Heo JY, Park JH, Seo KS, Han J, Park JI, Kweon GR, Park SK, Wu T, Hwang BD, Lim K (2013) The omega-3 polyunsaturated fatty acid DHA induces simultaneous apoptosis and autophagy via mitochondrial ROS-mediated Akt-mTOR signaling in prostate cancer cells expressing mutant p53. Biomed Res Int 2013:568671. https://doi.org/10.1155/2013/568671
Dixon SJ, Winter GE, Musavi LS, Lee ED, Snijder B, Rebsamen M, Superti-Furga G, Stockwell BR (2015) Human haploid cell genetics reveals roles for lipid metabolism genes in nonapoptotic cell death. ACS Chem Biol 10(7):1604–1609. https://doi.org/10.1021/acschembio.5b00245
Tan S, Schubert D, Maher P (2001) Oxytosis: a novel form of programmed cell death. Curr Top Med Chem 1(6):497–506
Vanden Berghe T, Linkermann A, Jouan-Lanhouet S, Walczak H, Vandenabeele P (2014) Regulated necrosis: the expanding network of non-apoptotic cell death pathways. Nat Rev Mol Cell Biol 15(2):135–147. https://doi.org/10.1038/nrm3737
Zhang J, Song F, Zhao X, Jiang H, Wu X, Wang B, Zhou M, Tian M, Shi B, Wang H, Jia Y, Wang H, Pan X, Li Z (2017) EGFR modulates monounsaturated fatty acid synthesis through phosphorylation of SCD1 in lung cancer. Mol Cancer 16(1):127. https://doi.org/10.1186/s12943-017-0704-x
Radmark O, Samuelsson B (2009) 5-Lipoxygenase: mechanisms of regulation. J Lipid Res 50(Suppl):S40-45. https://doi.org/10.1194/jlr.R800062-JLR200
Ivanov I, Kuhn H, Heydeck D (2015) Structural and functional biology of arachidonic acid 15-lipoxygenase-1 (ALOX15). Gene 573(1):1–32. https://doi.org/10.1016/j.gene.2015.07.073
Matsushita M, Freigang S, Schneider C, Conrad M, Bornkamm GW, Kopf M (2015) T cell lipid peroxidation induces ferroptosis and prevents immunity to infection. J Exp Med 212(4):555–568. https://doi.org/10.1084/jem.20140857
Asaoka Y, Oka M, Yoshida K, Sasaki Y, Nishizuka Y (1992) Role of lysophosphatidylcholine in T-lymphocyte activation: involvement of phospholipase A2 in signal transduction through protein kinase C. Proc Natl Acad Sci U S A 89(14):6447–6451. https://doi.org/10.1073/pnas.89.14.6447
Shah R, Shchepinov MS, Pratt DA (2018) Resolving the role of lipoxygenases in the initiation and execution of ferroptosis. ACS Cent Sci 4(3):387–396. https://doi.org/10.1021/acscentsci.7b00589
Viswanathan VS, Ryan MJ, Dhruv HD, Gill S, Eichhoff OM, Seashore-Ludlow B, Kaffenberger SD, Eaton JK, Shimada K, Aguirre AJ, Viswanathan SR, Chattopadhyay S, Tamayo P, Yang WS, Rees MG, Chen S, Boskovic ZV, Javaid S, Huang C, Wu X, Tseng YY, Roider EM, Gao D, Cleary JM, Wolpin BM, Mesirov JP, Haber DA, Engelman JA, Boehm JS, Kotz JD, Hon CS, Chen Y, Hahn WC, Levesque MP, Doench JG, Berens ME, Shamji AF, Clemons PA, Stockwell BR, Schreiber SL (2017) Dependency of a therapy-resistant state of cancer cells on a lipid peroxidase pathway. Nature 547(7664):453–457. https://doi.org/10.1038/nature23007
Hangauer MJ, Viswanathan VS, Ryan MJ, Bole D, Eaton JK, Matov A, Galeas J, Dhruv HD, Berens ME, Schreiber SL, McCormick F, McManus MT (2017) Drug-tolerant persister cancer cells are vulnerable to GPX4 inhibition. Nature 551(7679):247–250. https://doi.org/10.1038/nature24297
Acknowledgements
This research was supported by the National Key Research and Development Program of China (2017YFD0400200), the National Natural Science Foundation of China Grants No. 31471128 and 31771539, Key Research and Development Program of Jiangsu Province (BE2018624), and the National First-class Discipline Program of Food Science and Technology (JUFSTR20180101).
Funding
This research was supported by the National Key Research and Development Program of China (2017YFD0400200), the National Natural Science Foundation of China Grants No. 31471128 and 31771539, Key Research and Development Program of Jiangsu Province (BE2018624), and the National First-class Discipline Program of Food Science and Technology (JUFSTR20180101).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflicts of interest to this work.
Ethical approval
All animals were cared for and sacrificed according to the protocol approved by the ACUC of Jiangnan University.
Consent for publication
All authors agree to publish this article in the European Journal of Nutrition.
Supplementary Information
Below is the link to the electronic supplementary material.
394_2022_2940_MOESM1_ESM.tif
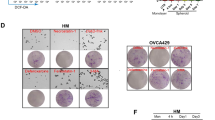
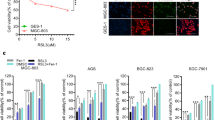
Supplementary file1 (TIF 25311 kb) A. Cell viability, as determined by MTT assays, after treatment of cells with erastin, RSL3, or glutamate and fatty acids for 48 h. The results are expressed as percentages relative to the control cells (untreated with either erastin or fatty acid) and correspond to the means ± S.D.(n=3). ANOVA (Tukey test) was performed. Asterisks marked the statistical difference between the addition group and the non-addition group of Fer-1 under the same treatment. *, P<0.05; **, P<0.01; ***, P<0.001. B. Cell viability of non-cancer cells, as determined by MTT assays, after treatment of six cells with erastin, RSL3, or glutamate and fatty acids for 48 h. Results are expressed as percentages relative to the control cells (untreated with either erastin or fatty acid) and correspond to the means ± S.D. of three independent experiments. C. Viability of cells treated with fish oil, erastin and RSL3 was measured using MTT assay. Results are expressed as percentages relative to the control and correspond to the means ± S.D. of three independent experiments. D. PC3 survival rate with different DHA concentration was determined by the MTT assay (n=3). ANOVA (Tukey test) was performed. Compared with the group without DHA addition, the statistical difference was marked with asterisks. ***, P<0.001.
394_2022_2940_MOESM2_ESM.tif
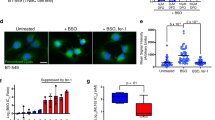
Supplementary file2 (TIF 14616 kb) A. Activation of caspase 3 was checked in ferroptosis and apoptosis. B. PC3 was treated with indicated conditions for 10 h, then flow cytometry was performed. FSC and SSC were used to evaluate cell survival. Gate R1 marked dead cells. C. Intracellular ROS in PC3 cells with different treatments for 2h and 6h. Fluorescence intensity are measured by a flow cytometry and shown as mean±S.D. D. Rols of different ROS inducers on cell viability. Data were shown as the means ± S.D. of three independent experiments. ANOVA with Tukey test was performed, and P < 0.05 was considered significant. Groups with significant differences were shown with different characters.
394_2022_2940_MOESM3_ESM.docx
Supplementary file3 (DOCX 23418 kb) A. HPLC-MS based free AA and DHA analysis was performed in PC3 upon indicated treatment. Fatty acids were determined by high resolution mass spectrometry. B. HPLC-MS based analysis of peroxidized AA and DHA was performed in PC3 upon indicated treatment. Peroxidized fatty acids were determined by high resolution mass spectrometry. C. HPLC-MS based lipidomics analysis was performed in PC3 upon indicated treatment. Target phospholipids were shown. The chromatogram showed the target lipids in different groups. Mass spectrometry was used for qualitative analysis. D. Peroxidized PE (18:0/22:6) and PE (18:0/20:4) were detected by HPLC-MS. Peroxidized PE (18:0/22:6) and PE (18:0/20:4) were determined by high resolution mass spectrometry. E. Western blot was performed to check the expression of ALOX5 in indicated cell lines (THP-1 was primed with PMA for 24h). Role of siALOX5 and zileuton were explored in different cell lines by MTT assay (n=3). F. Viability of cells treated with ALOX5 or FLAP inhibitor during ferroptosis was measured by the MTT assay (n=3). The T-test was performed and asterisks marked the statistical difference. *, P<0.05.
Rights and permissions
About this article
Cite this article
Shan, K., Feng, N., Zhu, D. et al. Free docosahexaenoic acid promotes ferroptotic cell death via lipoxygenase dependent and independent pathways in cancer cells. Eur J Nutr 61, 4059–4075 (2022). https://doi.org/10.1007/s00394-022-02940-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-022-02940-w