Abstract
Purpose
To evaluate the usefulness of prostate health index (PHI) as an indicator for recommending magnetic resonance imaging (MRI) in patients with prostate-specific antigen (PSA) gray zone level < 10 ng/mL.
Methods
443 patients who underwent prostate biopsy (PB) after serum PHI test and MRI between April 2019 and December 2022 were enrolled. For patients with visible lesion on MRI with Prostate Imaging Reporting and Data System Score (PI-RADS) ≥ 3, MRI-targeted PB was performed in addition to systematic 12-core PB.
Results
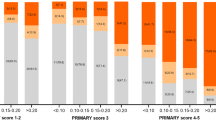
The optimal cutoff value of PHI for predicting PI-RADS ≥ 3 lesions was 39.6, which was significantly associated with overall prostate cancer (OR 3.07, p = 0.018) and clinically significant prostate cancer (csPCa) (OR 4.15, p = 0.006) at MRI-targeted PB cores. When MRI was restricted to patients with PHI ≥ 39.6 alone, 28.7% of unnecessary MRI could be saved at the cost of missing 13.6% of csPCa. When omitting MRI for patients with PHI < 39.6 and PSAD < 0.12 ng/mL2, unnecessary MRI could be reduced by 20.1% with the risk of missing 6.2% of csPCa. With addition of systematic PB, 21.0% of patients with negative MRI-targeted PB were diagnosed as csPCa.
Conclusions
For patients in PSA gray zone, PHI of 39.6 might be an indicator for MRI and further MRI-targeted PB in additional to PSAD of 0.12 ng/mL2, reducing 20.1% of unnecessary MRI with the minimal risk of missing 6.2% of csPCa. To maximize csPCa detection, combining both MRI-targeted and systematic PB should be also considered.

Similar content being viewed by others
Data availability statement
The authors confirm that the data supporting the findings of this study are available within the article and its supplementary materials.
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71:209–249. https://doi.org/10.3322/caac.21660
Boniol M, Boyle P, Autier P, Ruffion A, Perrin P (2012) Critical role of prostate biopsy mortality in the number of years of life gained and lost within a prostate cancer screening programme. BJU Int 110:1648–1652. https://doi.org/10.1111/j.1464-410X.2012.11513.x
Welch HG, Albertsen PC (2020) Reconsidering prostate cancer mortality—the future of PSA screening. N Engl J Med 382:1557–1563. https://doi.org/10.1056/NEJMms1914228
Li X, Li C, Chen M (2023) Patients With “Gray Zone” PSA levels: application of prostate MRI and MRS in the diagnosis of prostate cancer. J Magn Reson Imaging 57:992–1010. https://doi.org/10.1002/jmri.28505
Pedler K, Kitzing YX, Varol C, Arianayagam M (2015) The current status of MRI in prostate cancer. Aust Fam Physician 44:225–230
Ahmed HU, El-Shater Bosaily A, Brown LC, Gabe R, Kaplan R, Parmar MK, Collaco-Moraes Y, Ward K, Hindley RG, Freeman A, Kirkham AP, Oldroyd R, Parker C, Emberton M, PROMIS study group (2017) Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet 389:815–822. https://doi.org/10.1016/S0140-6736(16)32401-1
Ahdoot M, Wilbur AR, Reese SE, Lebastchi AH, Mehralivand S, Gomella PT, Bloom J, Gurram S, Siddiqui M, Pinsky P, Parnes H, Linehan WM, Merino M, Choyke PL, Shih JH, Turkbey B, Wood BJ, Pinto PA (2020) MRI-targeted, systematic, and combined biopsy for prostate cancer diagnosis. N Engl J Med 382:917–928. https://doi.org/10.1056/NEJMoa1910038
Kasivisvanathan V, Rannikko AS, Borghi M, Panebianco V, Mynderse LA, Vaarala MH, Briganti A, Budäus L, Hellawell G, Hindley RG, Roobol MJ, Eggener S, Ghei M, Villers A, Bladou F, Villeirs GM, Virdi J, Boxler S, Robert G, Singh PB, Venderink W, Hadaschik BA, Ruffion A, Hu JC, Margolis D, Crouzet S, Klotz L, Taneja SS, Pinto P, Gill I, Allen C, Giganti F, Freeman A, Morris S, Punwani S, Williams NR, Brew-Graves C, Deeks J, Takwoingi Y, Emberton M, Moore CM, PRECISION Study Group Collaborators (2018) MRI-targeted or standard biopsy for prostate-cancer diagnosis. N Engl J Med 378:1767–1777. https://doi.org/10.1056/NEJMoa1801993
Getaneh AM, Heijnsdijk EAM, de Koning HJ (2021) The comparative effectiveness of mpMRI and MRI-guided biopsy vs regular biopsy in a population-based PSA testing: a modeling study. Sci Rep 11:1801. https://doi.org/10.1038/s41598-021-81459-2
Xu N, Wu YP, Chen DN, Ke ZB, Cai H, Wei Y, Zheng QS, Huang JB, Li XD, Xue XY (2018) Can Prostate Imaging Reporting and Data System Version 2 reduce unnecessary prostate biopsies in men with PSA levels of 4–10 ng/ml? J Cancer Res Clin Oncol 144:987–995. https://doi.org/10.1007/s00432-018-2616-6
Carroll PH, Mohler JL (2018) NCCN guidelines updates: prostate cancer and prostate cancer early detection. J Natl Compr Canc Netw 16:620–623. https://doi.org/10.6004/jnccn.2018.0036
Oerther B, Engel H, Bamberg F, Sigle A, Gratzke C, Benndorf M (2022) Cancer detection rates of the PI-RADSv2.1 assessment categories: systematic review and meta-analysis on lesion level and patient level. Prostate Cancer Prostatic Dis 25:256–263. https://doi.org/10.1038/s41391-021-00417-1
Lu YF, Zhang Q, Chen HY, Chen JY, Pan Y, Xu CC, Xu JX, Yu RS (2019) Improving the detection rate of prostate cancer in the gray zone of PI-RADS v2 and serum tPSA by using prostate-specific antigen-age volume. Medicine (Baltimore) 98:e16289. https://doi.org/10.1097/MD.0000000000016289
Kim S, Vickers AJ, Hu JC (2018) Challenges in adopting level 1 evidence for multiparametric magnetic resonance imaging as a biomarker for prostate cancer screening. JAMA Oncol 4:1663–1664. https://doi.org/10.1001/jamaoncol.2018.4160
Deniffel D, Zhang Y, Salinas E, Satkunasivam R, Khalvati F, Haider MA (2020) Reducing unnecessary prostate multiparametric magnetic resonance imaging by using clinical parameters to predict negative and indeterminate findings. J Urol 203:292–298. https://doi.org/10.1097/JU.0000000000000518
Jeon JH, Koo KC, Chung BH, Lee KS (2021) Usefulness of prostate-specific antigen density as an indicator for recommending prebiopsy magnetic resonance imaging to prevent missed prostate cancer diagnoses. Korean J Urol Oncol 19:155–163. https://doi.org/10.22465/kjuo.2021.19.3.155
Falagario UG, Martini A, Wajswol E, Treacy PJ, Ratnani P, Jambor I, Anastos H, Lewis S, Haines K, Cormio L, Carrieri G, Rastinehad AR, Wiklund P, Tewari A (2020) Avoiding unnecessary Magnetic Resonance Imaging (MRI) and biopsies: negative and positive predictive value of MRI according to prostate-specific antigen density, 4k score and risk calculators. Eur Urol Oncol 3:700–704. https://doi.org/10.1016/j.euo.2019.08.015
Rico L, Contreras P, Vitagliano G, Rios Pita H, Ameri C, Blas L (2020) Value of prostate-specific antigen density in negative or equivocal lesions on multiparametric magnetic resonance imaging. Turk J Urol 46:367–372. https://doi.org/10.5152/tud.2020.20111
Leow JJ, Koh SH, Chow MW, Loke W, Salada R, Hong SK, Yeow Y, Lee CH, Tan CH, Tan TW (2023) Can we omit systematic biopsies in patients undergoing MRI fusion-targeted prostate biopsies? Asian J Androl 25:43–49. https://doi.org/10.4103/aja2021128
Ye C, Ho JN, Kim DH, Song SH, Kim H, Lee H, Jeong SJ, Hong SK, Byun SS, Ahn H, Hwang SI, Lee HJ, Lee S (2022) The Prostate Health Index and multi-parametric MRI improve diagnostic accuracy of detecting prostate cancer in Asian populations. Investig Clin Urol 63:631–638. https://doi.org/10.4111/icu.20220056
Fan YH, Pan PH, Cheng WM, Wang HK, Shen SH, Liu HT, Cheng HM, Chen WR, Huang TH, Wei TC, Huang IS, Lin CC, Huang EYH, Chung HJ, Huang WJS, Lin TP (2021) The Prostate Health Index aids multi-parametric MRI in diagnosing significant prostate cancer. Sci Rep 11:1286. https://doi.org/10.1038/s41598-020-78428-6
Hsieh PF, Li WJ, Lin WC, Chang H, Chang CH, Huang CP, Yang CR, Chen WC, Chang YH, Wu HC (2020) Combining prostate health index and multiparametric magnetic resonance imaging in the diagnosis of clinically significant prostate cancer in an Asian population. World J Urol 38:1207–1214. https://doi.org/10.1007/s00345-019-02889-2
Tan TW, Png KS, Lee CH, Yuwono A, Yeow Y, Chong KT, Lee YM, Tan CH, Tan YK (2017) MRI fusion-targeted transrectal prostate biopsy and the role of prostate-specific antigen density and prostate health index for the detection of clinically significant prostate cancer in Southeast Asian Men. J Endourol 31:1111–1116. https://doi.org/10.1089/end.2017.0485
Chen H, Shi B, Wu Y, Qian Y, Zhou J, Zhang X, Ding J, Yu Y (2022) The modified prostate health index (PHI) outperforms PHI density in the detection of clinical prostate cancer within the PSA grey zone. Int Urol Nephrol 54:749–756. https://doi.org/10.1007/s11255-022-03113-8
Hwang SI, Lee HJ, Lee SE, Hong SK, Byun SS, Lee SC, Choe G (2019) Value of MR-US fusion in guidance of repeated prostate biopsy in men with PSA < 10 ng/mL. Clin Imaging 53:1–5. https://doi.org/10.1016/j.clinimag.2018.09.012
Bazinet M, Meshref AW, Trudel C, Aronson S, Péloquin F, Nachabe M, Bégin LR, Elhilali MM (1994) Prospective evaluation of prostate-specific antigen density and systematic biopsies for early detection of prostatic carcinoma. Urology 43:44–51. https://doi.org/10.1016/s0090-4295(94)80260-2. (discussion 51-2)
Acknowledgements
This work was supported by a grant of Korea Medical Device Development Fund funded by the Korea government (the Ministry of Science and ICT, the Ministry of Trade, Industry and Energy, the Ministry of Health & Welfare, the Ministry of Food and Drug Safety) (Project Number: 1711138269 , RS-2020-KD000141) (NTIS, RS-2020-KD000141).
Author information
Authors and Affiliations
Contributions
BS and SL contributed to protocol/project development; BS analyzed the data; BS and SL contributed to manuscript writing/editing; SHS, SIH and HJL were involved in data collection/analysis/management; HL, SKH and SSB were involved in the critical review; SL supervised the study.
Corresponding author
Ethics declarations
Conflict of interest
Our research was conducted without commercial or financial relationships that could be interpreted as a potential conflict of interest. The authors declare that there is no potential conflict of interest.
Research involving human participants and/or animals
The Seoul National University Bundang Hospital Institutional Review Board (IRB) approved this study (IRB no. B-2304-825-103). Our research does not include animals as subjects. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
The requirement of written informed consent was waived due to the retrospective nature of this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Song, B., Song, S.H., Hwang, S.I. et al. Clinical value of prostate health index as an indicator for recommending magnetic resonance imaging in patients with gray-zone prostate-specific antigen level. World J Urol 41, 3519–3526 (2023). https://doi.org/10.1007/s00345-023-04613-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-023-04613-7