Abstract
Objectives
To assess the feasibility and technical outcomes of pelvic bone cementoplasty using an electromagnetic navigation system (EMNS) in standard practice.
Materials and methods
Monocentric retrospective study of all consecutive patients treated with cementoplasty or reinforced cementoplasty of the pelvic bone with EMNS-assisted procedures. The endpoints were periprocedural adverse events, needle repositioning rates, procedure duration, and radiation exposure.
Results
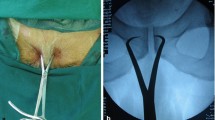
A detailed description of the technical steps is provided. Thirty-three patients (68 years ± 10) were treated between February 2016 and February 2020. Needle repositioning was required for 1/33 patients (3%). The main minor technical adverse event was soft tissue PMMA cement leaks. No major adverse event was noted. The median number of CT acquisitions throughout the procedures was 4 (range: 2 to 8). Radiation exposure and mean procedure duration are provided.
Conclusion
Electromagnetic navigation system–assisted percutaneous interventions for the pelvic bone are feasible and lead to low rates of minor technical adverse events and needle repositioning. Procedure duration and radiation exposure were low.
Key Points
• Initial experience for 33 patients treated with an electromagnetic navigation assistance for pelvic cementoplasty shows feasibility and safety.
• The use of an electromagnetic navigation system does not expose to high procedure duration or radiation exposure.
• The system is efficient in assisting the radiologist for extra-axial planes in challenging approaches.




Similar content being viewed by others
Abbreviations
- CBCT:
-
Cone-beam CT
- CT:
-
Computed tomography
- DAP:
-
Dose-area product
- DLP:
-
Dose-length product
- ED:
-
Effective dose
- EMNS:
-
Electromagnetic navigation system
- FICS:
-
Fixation by internal cemented screw
- MBD:
-
Metastatic bone disease
- MRI:
-
Magnetic resonance imaging
- PC:
-
Percutaneous cementoplasty
- PMMA:
-
Poly-methyl-methacrylate
- RC:
-
Reinforced cementoplasty
References
Müller DA, Capanna R (2015) The surgical treatment of pelvic bone metastases. Adv Orthop 2015:525363–525363
Rich SE, Chow R, Raman S et al (2018) Update of the systematic review of palliative radiation therapy fractionation for bone metastases. Radiother Oncol 126:547–557
Krishnan CK, Han I, Kim HS (2017) Outcome after surgery for metastases to the pelvic bone: a single institutional experience. Clin Orthop Surg 9:116–125
Garnon J, Jennings JW, Meylheuc L et al (2020) Biomechanics of the osseous pelvis and its implication for consolidative treatments in interventional oncology. Cardiovasc Intervent Radiol 43:1589–1599
Deschamps F, de Baere T, Hakime A et al (2016) Percutaneous osteosynthesis in the pelvis in cancer patients. Eur Radiol 26:1631–1639
Premat K, Clarençon F, Bonaccorsi R, Degos V, Cormier É, Chiras J (2017) Reinforced cementoplasty using dedicated spindles in the management of unstable malignant lesions of the cervicotrochanteric region. Eur Radiol 27:3973–3982
Reuther G, Röhner U, Will T, Dehne I, Petereit U (2014) CT-guided screw fixation of vertical sacral fractures in local anaesthesia using a standard CT. Rofo 186:1134–1139
Roux C, Tselikas L, Yevich S et al (2019) Fluoroscopy and Cone-Beam CT-guided Fixation by Internal Cemented Screw for Pathologic Pelvic Fractures. Radiology 290:418–425
Durand P, Moreau-Gaudry A, Silvent AS et al (2017) Computer assisted electromagnetic navigation improves accuracy in computed tomography guided interventions: a prospective randomized clinical trial. PLoS One 12:e0173751
Moulin B, Tselikas L, De Baere T et al (2020) CT guidance assisted by electromagnetic navigation system for percutaneous fixation by internal cemented screws (FICS). Eur Radiol 30:943–949
Teriitehau C, Rabeh H, Pessis E, Sénéchal Q, Besse F, Bravetti M (2020) Reduction of patient radiation dose during percutaneous CT vertebroplasty: impact of a new computer-assisted navigation (CAN) system. Radioprotection 55:11–16
Pereira LP, Clarençon F, Cormier E et al (2013) Safety and effectiveness of percutaneous sacroplasty: a single-centre experience in 58 consecutive patients with tumours or osteoporotic insufficient fractures treated under fluoroscopic guidance. Eur Radiol 23:2764–2772
Binaghi S, Guntern D, Schnyder P, Theumann N (2006) A new, easy, fast, and safe method for CT-guided sacroplasty. Eur Radiol 16:2875–2878
Wong JSY, Lau JCK, Chui KH, Tiu KL, Lee KB, Li W (2019) Three-dimensional-guided navigation percutaneous screw fixation of fragility fractures of the pelvis. J Orthop Surg 27:2309499019833897
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Pr Frederic Clarencon.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was not required for this study because of the type of study.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• observational
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Boeken, T., Pouliquen, G., Premat, K. et al. Initial experience, feasibility, and technical development with an electromagnetic navigation assistance in percutaneous pelvic bone cementoplasty: retrospective analysis. Eur Radiol 33, 2605–2611 (2023). https://doi.org/10.1007/s00330-022-09252-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-09252-x