Abstract
Objectives
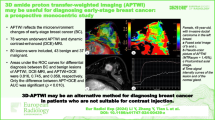
To evaluate the potential of molecular amide proton transfer (APT) MRI for predicting the risk group of abdominal tumors in children, and compare it with quantitative T1 and T2 mapping.
Methods
This prospective study enrolled 133 untreated pediatric patients with suspected abdominal tumors from February 2019 to September 2020. APT-weighted (APTw) imaging and quantitative relaxation time mapping sequences were executed for each subject. The region of interest (ROI) was generated with automatic artifact detection and ROI-shrinking algorithms, within which the APTw, T1, and T2 indices were calculated and compared between different risk groups. The prediction performance of different imaging parameters was assessed with the receiver operating characteristics (ROC) analysis and Student’s t-test.
Results
Fifty-seven patients were included in the final analysis, including 24 neuroblastomas (NB), 18 Wilms’ tumors (WT), and 15 hepatoblastomas (HB). The APTw signal was significantly (p < .001) higher in patients with high-risk NB than those with low-risk NB, while the difference between patients with low-risk and high-risk WT (p = .69) or HB (p = .35) was not statistically significant. The associated areas under the curve (AUC) for APT to differentiate low-risk and high-risk NB, WT, and HB were 0.93, 0.58, and 0.71, respectively. The quantitative T1 and T2 values generated AUCs of 0.61–0.70 for the risk stratification of abdominal tumors.
Conclusions
APT MRI is a potential imaging biomarker for stratifying the risk group of pediatric neuroblastoma in the abdomen preoperatively and provides added value to structural MRI.
Key Points
• Amide proton transfer (APT) imaging showed significantly (p < .001) higher values in pediatric patients with high-risk neuroblastoma than those with low-risk neuroblastoma, but did not demonstrate a significant difference in patients with Wilms’ tumor (p = .69) or hepatoblastoma (p = .35).
• The associated areas under the curve (AUC) for APT to differentiate low-risk and high-risk neuroblastoma, Wilms’ tumor, and hepatoblastoma were 0.93, 0.58, and 0.71, respectively.
• The quantitative T1 and T2 indices generated AUCs of 0.61–0.70 for dichotomizing the risk group of abdominal tumors.






Similar content being viewed by others
Abbreviations
- APT:
-
Amide proton transfer
- APTw:
-
Amide proton transfer-weighted
- CEST:
-
Chemical exchange saturation transfer
- HB:
-
Hepatoblastoma
- MIX:
-
Interleaved T1 and T2 mapping sequence
- NB:
-
Neuroblastoma
- T1w:
-
T1-weighted
- T2w:
-
T2-weighted
- WT:
-
Wilms’ tumor
References
Steliarova-Foucher E, Colombet M, Ries LAG et al (2017) International incidence of childhood cancer, 2001–10: a population-based registry study. Lancet Oncol 18:719–731
Maris JM, Hogarty MD, Bagatell R, Cohn SL (2007) Neuroblastoma. Lancet 369:2106–2120
Hiorns M, Owens C (2001) Radiology of neuroblastoma in children. Eur Radiol 11:2071–2081
Davidoff AM (2012) Wilms tumor. Adv Pediatr 59:247–267
Herzog CE, Andrassy RJ, Eftekhari F (2000) Childhood cancers: hepatoblastoma. Oncologist 5:445–453
Cohn SL, Pearson ADJ, London WB et al (2009) The International Neuroblastoma Risk Group (INRG) Classification System: an INRG Task Force report. J Clin Oncol 27:289–297
Vujanic GM, Sandstedt B, Harms D et al (2002) Revised International Society of Paediatric Oncology (SIOP) working classification of renal tumors of childhood. Med Pediatr Oncol 38:79–82
Meyers RL, Maibach R, Hiyama E et al (2017) Risk-stratified staging in paediatric hepatoblastoma: a unified analysis from the Children’s Hepatic tumors International Collaboration. Lancet Oncol 18:122–131
Van Zijl PCM, Yadav NN (2011) Chemical exchange saturation transfer (CEST): What is in a name and what isn’t? Magn Reson Med 65:927–948
Zhou J, Payen J-F, Wilson DA, Traystman RJ, van Zijl PC (2003) Using the amide proton signals of intracellular proteins and peptides to detect pH effects in MRI. Nat Med 9:1085–1090
Zhou JY, Tryggestad E, Wen ZB et al (2011) Differentiation between glioma and radiation necrosis using molecular magnetic resonance imaging of endogenous proteins and peptides. Nat Med 17:130-U308
Togao O, Yoshiura T, Keupp J et al (2014) Amide proton transfer imaging of adult diffuse gliomas: correlation with histopathological grades. Neuro Oncol 16:441–448
Kamitani T, Sagiyama K, Togao O et al (2020) Amide proton transfer (APT) imaging of parotid tumors: differentiation of malignant and benign tumors. Eur J Radiol 129:109047
Ohno Y, Yui M, Koyama H et al (2016) Chemical exchange saturation transfer MR imaging: preliminary results for differentiation of malignant and benign thoracic lesions. Radiology 279:578–589
Liu R, Zhang H, Niu W et al (2019) Improved chemical exchange saturation transfer imaging with real-time frequency drift correction. Magn Reson Med 81:2915–2923
Pruessmann KP, Weiger M, Scheidegger MB, Boesiger P (1999) SENSE: sensitivity encoding for fast MRI. Magn Reson Med 42:952–962
Zhou J, Zhu H, Lim M et al (2013) Three-dimensional amide proton transfer MR imaging of gliomas: initial experience and comparison with gadolinium enhancement. J Magn Reson Imaging 38:1119–1128
Zhu H, Jones CK, Van Zijl PCM, Barker PB, Zhou J (2010) Fast 3D chemical exchange saturation transfer (CEST) imaging of the human brain. Magn Reson Med 64:638–644
Heo HY, Zhang Y, Jiang S, Lee DH, Zhou J (2016) Quantitative assessment of amide proton transfer (APT) and nuclear overhauser enhancement (NOE) imaging with extrapolated semisolid magnetization transfer reference (EMR) signals: II. Comparison of three EMR models and application to human brain glioma at 3 Tesla. Magn Reson Med 75:1630–1639
In Den Kleef JJE, Cuppen JJM (1987) RLSQ:T1, T2, and ρ calculations, combining ratios and least squares. Magn Reson Med 5:513–524
Zhang H, Lai C, Liu R et al (2019) Age-specific optimization of T1-weighted brain MRI throughout infancy. Neuroimage 199:387–395
Zhang Y, Heo HY, Lee DH et al (2016) Selecting the reference image for registration of CEST series. J Magn Reson Imaging 43:756–761
Jenkinson M (2002) Improved optimization for the robust and accurate linear registration and motion correction of brain images. Neuroimage 17:825–841
Kim M, Gillen J, Landman BA, Zhou J, van Zijl P (2009) Water saturation shift referencing (WASSR) for chemical exchange saturation transfer (CEST) experiments. Magn Reson Med 61:1441–1450
Hanley JA, McNeil BJ (1982) The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology 143:29–36
Hanley JA, McNeil BJ (1983) A method of comparing the areas under receiver operating characteristic curves derived from the same cases. Radiology 148:839–843
Pinto NR, Applebaum MA, Volchenboum SL et al (2015) Advances in risk classification and treatment strategies for neuroblastoma. J Clin Oncol 33:3008–3017
von Schweinitz D (2012) Hepatoblastoma: recent developments in research and treatment. Semin Pediatr Surg 21:21–30
D’Angio GJ, Breslow N, Beckwith JB et al (1989) Treatment of Wilms’ tumor. Results of the third national Wilms’ tumor study. Cancer 64:349–360
Zaiss M, Windschuh J, Paech D et al (2015) Relaxation-compensated CEST-MRI of the human brain at 7 T: unbiased insight into NOE and amide signal changes in human glioblastoma. Neuroimage 112:180–188
Park JE, Kim HS, Park KJ, Choi CG, Kim SJ (2015) Histogram analysis of amide proton transfer imaging to identify contrast-enhancing low-grade brain tumor that mimics high-grade tumor: increased accuracy of MR perfusion. Radiology 277:151–161
Wen Z, Hu S, Huang F et al (2010) MR imaging of high-grade brain tumors using endogenous protein and peptide-based contrast. Neuroimage 51:616–622
Sagiyama K, Mashimo T, Togao O et al (2014) In vivo chemical exchange saturation transfer imaging allows early detection of a therapeutic response in glioblastoma. Proc Natl Acad Sci U S A 111:4542–4547
Park JR, Eggert A, Caron H (2008) Neuroblastoma: biology, prognosis, and treatment. Pediatr Clin North Am 55:97–120
Aherne W, Buck P (1971) The potential cell population doubling time in neuroblastoma and nephroblastoma. Br J Cancer 25:691–696
Liu CJ, Lu MY, Liu YL et al (2017) Risk stratification of pediatric patients with neuroblastoma using volumetric parameters of 18F-FDG and 18F-DOPA PET/CT. Clin Nucl Med 42:e142–e148
Zhang Y, Yong X, Liu R et al (2020) Whole-brain chemical exchange saturation transfer imaging with optimized turbo spin echo readout. Magn Reson Med 84:1161–1172
Funding
This study has received funding by National Natural Science Foundation of China (grant number: 81971605, 61801421, 61801424, and 91859201) and Ministry of Science and Technology of the People’s Republic of China (grant number: 2018YFE0114600). Leading Innovation and Entrepreneurship Team of Zhejiang Province: 2020R01003. This work was supported by the MOE Frontier Science Center for Brain Science & Brain-Machine Integration, Zhejiang University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Yi Zhang.
Conflict of interest
The authors of this manuscript declare relationships with the following companies: Philips Healthcare (employee: Weibo Chen).
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• prospective
• diagnostic or prognostic study
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Jia, X., Wang, W., Liang, J. et al. Risk stratification of abdominal tumors in children with amide proton transfer imaging. Eur Radiol 32, 2158–2167 (2022). https://doi.org/10.1007/s00330-021-08376-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-021-08376-w