Abstract
Background
This study aimed to develop and validate a novel risk stratification model and a web-based survival rate calculator to improve discriminative and predictive accuracy for diffuse large B-cell lymphoma (DLBCL) in the rituximab era.
Methods
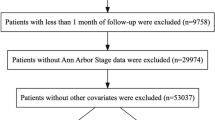
We retrospectively collected pre-treatment data from 873 primary DLBCL patients who received R-CHOP-based immunochemotherapy regimens at the Cancer Hospital, Chinese Academy of Medical Sciences, from January 1, 2005, to December 31, 2018. An independent cohort of 175 DLBCL patients from Fujian Cancer Hospital was used for external validation.
Findings
Age, ECOG PS, number of extranodal sites, Ann Arbor stage, bulky disease, and LDH levels were screened to develop the nomogram and web-based survival rate calculator. The C-index of the nomogram in the training, internal validation, and external validation cohorts was 0.761, 0.758, and 0.768, respectively. The risk stratification model generated based on the nomogram effectively stratified patients into three distinct risk groups. K-M survival curves demonstrated that the novel risk stratification model exhibited a superior level of predictive accuracy compared to IPI, R-IPI, and NCCN-IPI both in training and two validation cohorts. Additionally, the area under the curve (AUC) value of the novel model (0.763) for predicting 5-year overall survival rates was higher than those of IPI (0.749), R-IPI (0.725), and NCCN-IPI (0.727) in the training cohort. Similar results were observed in both internal and external validation cohort.
Conclusions
In conclusion, we have successfully developed and validated a novel risk stratification model and a web-based survival rate calculator that demonstrated superior discriminative and predictive accuracy compared to IPI, R-IPI, and NCCN-IPI in the rituximab era.










Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Abbreviations
- DLBCL :
-
Diffuse large B-cell lymphoma
- NHL :
-
Non-Hodgkin lymphoma
- R-CHOP :
-
Rituximab, cyclophosphamide, doxorubicin, vincristine, prednisone
- IPI :
-
International Prognostic Index
- R-IPI :
-
Revised International Prognostic Index
- NCCN-IPI :
-
National Comprehensive Cancer Network International Prognostic Index
- CBC :
-
Complete blood cell
- CHCAMS :
-
Cancer Hospital, Chinese Academy of Medical Sciences
- FJCH :
-
Fujian Cancer Hospital
- DLBCL-NOS :
-
Diffuse large B-cell lymphoma, not otherwise specified
- ECOG :
-
Eastern Cooperative Oncology
- PS :
-
Performance status
- LDH :
-
Lactate dehydrogenase
- GCB :
-
Germinal center B-cell type
- HBV :
-
Hepatitis B virus
- CI :
-
Confidence interval
- HR :
-
Hazard ratio
- OS :
-
Overall survival
- GCB :
-
Germinal center B-cell-like
- LASSO :
-
Absolute shrinkage and selection operator
- AUC :
-
Area under the curve
- ROC :
-
Receiver operating characteristic curve
- CI :
-
Confidence intervals
- DCA :
-
Decision curve analysis
- ASH :
-
American Society of Hematology
- GELA :
-
Groupe d’Etude des Lymphomes de l’Adulte
- MInT :
-
MabThera International Trial Group
References
Teras L et al (2016) 2016 US lymphoid malignancy statistics by World Health Organization subtypes. CA: Cancer J Clin 66:443–459. https://doi.org/10.3322/caac.21357
Tilly H et al (2022) Polatuzumab vedotin in previously untreated diffuse large B-cell lymphoma. N Engl J Med 386:351–363. https://doi.org/10.1056/NEJMoa2115304
Friedberg J (2011) Relapsed/refractory diffuse large B-cell lymphoma. Hematology 2011:498–505. https://doi.org/10.1182/asheducation-2011.1.498
(1993) A predictive model for aggressive non-Hodgkin’s lymphoma. N Eng J Med 329:987–994. https://doi.org/10.1056/nejm199309303291402
Sehn L et al (2007) The revised International Prognostic Index (R-IPI) is a better predictor of outcome than the standard IPI for patients with diffuse large B-cell lymphoma treated with R-CHOP. Blood 109:1857–1861. https://doi.org/10.1182/blood-2006-08-038257
Zhou Z et al (2014) An enhanced International Prognostic Index (NCCN-IPI) for patients with diffuse large B-cell lymphoma treated in the rituximab era. Blood 123:837–842. https://doi.org/10.1182/blood-2013-09-524108
Alizadeh A et al (2000) Distinct types of diffuse large B-cell lymphoma identified by gene expression profiling. Nature 403:503–511. https://doi.org/10.1038/35000501
Chapuy B et al (2018) Molecular subtypes of diffuse large B cell lymphoma are associated with distinct pathogenic mechanisms and outcomes. Nat Med 24:679–690. https://doi.org/10.1038/s41591-018-0016-8
Malumbres R et al (2008) Paraffin-based 6-gene model predicts outcome in diffuse large B-cell lymphoma patients treated with R-CHOP. Blood 111:5509–5514. https://doi.org/10.1182/blood-2008-02-136374
Alizadeh A et al (2011) Prediction of survival in diffuse large B-cell lymphoma based on the expression of 2 genes reflecting tumor and microenvironment. Blood 118:1350–1358. https://doi.org/10.1182/blood-2011-03-345272
Schmitz R et al (2018) Genetics and pathogenesis of diffuse large B-cell lymphoma. N Engl J Med 378:1396–1407. https://doi.org/10.1056/NEJMoa1801445
Lossos I et al (2004) Prediction of survival in diffuse large-B-cell lymphoma based on the expression of six genes. N Engl J Med 350:1828–1837. https://doi.org/10.1056/NEJMoa032520
Qin Y et al (2021) BCL2Prognostic value of and genetic alterations for diffuse large B-cell lymphoma patients treated with R-CHOP. Cancer Biol Med. https://doi.org/10.20892/j.issn.2095-3941.2021.0193
Adams H, Nievelstein R, Kwee T (2015) Prognostic value of complete remission status at end-of-treatment FDG-PET in R-CHOP-treated diffuse large B-cell lymphoma: systematic review and meta-analysis. Br J Haematol 170:185–191. https://doi.org/10.1111/bjh.13420
Wright G et al (2020) A probabilistic classification tool for genetic subtypes of diffuse large B cell lymphoma with therapeutic implications. Cancer Cell 37:551-568.e514. https://doi.org/10.1016/j.ccell.2020.03.015
Scott D et al (2015) Prognostic significance of diffuse large B-cell lymphoma cell of origin determined by digital gene expression in formalin-fixed paraffin-embedded tissue biopsies. J Clin Oncol 33:2848–2856. https://doi.org/10.1200/jco.2014.60.2383
Johnson N et al (2012) Concurrent expression of MYC and BCL2 in diffuse large B-cell lymphoma treated with rituximab plus cyclophosphamide, doxorubicin, vincristine, and prednisone. J Clin Oncol 30:3452–3459. https://doi.org/10.1200/jco.2011.41.0985
Wilcox R et al (2011) The absolute monocyte and lymphocyte prognostic score predicts survival and identifies high-risk patients in diffuse large-B-cell lymphoma. Leukemia 25:1502–1509. https://doi.org/10.1038/leu.2011.112
Bento L et al (2020) New prognosis score including absolute lymphocyte/monocyte ratio, red blood cell distribution width and beta-2 microglobulin in patients with diffuse large B-cell lymphoma treated with R-CHOP: Spanish Lymphoma Group Experience (GELTAMO). Br J Haematol 188:888–897. https://doi.org/10.1111/bjh.16263
Cheng C et al (2020) Hepatitis B surface antigen positivity is an independent unfavorable prognostic factor in diffuse large B-cell lymphoma in the rituximab era. Oncologist 25:793–802. https://doi.org/10.1634/theoncologist.2019-0756
Wei Y et al (2020) Albumin improves stratification in the low IPI risk patients with diffuse large B-cell lymphoma. Int J Hematol 111:681–685. https://doi.org/10.1007/s12185-020-02818-9
Luan C, Wang F, Wei N, Chen B (2020) Prognostic nutritional index and the prognosis of diffuse large b-cell lymphoma: a meta-analysis. Cancer Cell Int 20:455. https://doi.org/10.1186/s12935-020-01535-x
Cai J et al (2021) A nomogram prognostic index for risk-stratification in diffuse large B-cell lymphoma in the rituximab era: a multi-institutional cohort study. Br J Cancer 125:402–412. https://doi.org/10.1038/s41416-021-01434-6
Wang J, Zhou M, Zhou R, Xu J, Chen B (2020) Nomogram for predicting the overall survival of adult patients with primary gastrointestinal diffuse large B cell lymphoma: a SEER-based study. Front Oncol 10:1093. https://doi.org/10.3389/fonc.2020.01093
Wight J, Chong G, Grigg A, Hawkes E (2018) Prognostication of diffuse large B-cell lymphoma in the molecular era: moving beyond the IPI. Blood Rev 32:400–415. https://doi.org/10.1016/j.blre.2018.03.005
Wu G, Keating A (2006) Biomarkers of potential prognostic significance in diffuse large B-cell lymphoma. Cancer 106:247–257. https://doi.org/10.1002/cncr.21586
Touijer K, Scardino P (2009) Nomograms for staging, prognosis, and predicting treatment outcomes. Cancer 115:3107–3111. https://doi.org/10.1002/cncr.24352
De Paepe P, De Wolf-Peeters C (2007) Diffuse large B-cell lymphoma: a heterogeneous group of non-Hodgkin lymphomas comprising several distinct clinicopathological entities. Leukemia 21:37–43. https://doi.org/10.1038/sj.leu.2404449
Hong F, Kahl B, Gray R (2013) Incremental value in outcome prediction with gene expression-based signatures in diffuse large B-cell lymphoma. Blood 121:156–158. https://doi.org/10.1182/blood-2012-08-450106
Jelicic J, Larsen T, Maksimovic M, Trajkovic G (2019) Available prognostic models for risk stratification of diffuse large B cell lymphoma patients: a systematic review. Crit Rev Oncol Hematol 133:1–16. https://doi.org/10.1016/j.critrevonc.2018.10.006
Rodríguez J et al (1992) A proposal for a simple staging system for intermediate grade lymphoma and immunoblastic lymphoma based on the ‘tumor score’. Ann Oncol 3:711–717. https://doi.org/10.1093/oxfordjournals.annonc.a058324
Danieu L, Wong G, Koziner B, Clarkson B (1986) Predictive model for prognosis in advanced diffuse histiocytic lymphoma. Can Res 46:5372–5379
Hoskins P, Ng V, Spinelli J, Klimo P, Connors J (1991) Prognostic variables in patients with diffuse large-cell lymphoma treated with MACOP-B. J Clin Oncol 9:220–226. https://doi.org/10.1200/jco.1991.9.2.220
Savage K et al (2006) Favorable outcome of primary mediastinal large B-cell lymphoma in a single institution: the British Columbia experience. Ann Oncol 17:123–130. https://doi.org/10.1093/annonc/mdj030
Tomita N et al (2008) Adjuvant radiotherapy to an initial bulky mass in diffuse large B-cell lymphoma: lack of survival benefit. Int J Lab Hematol 30:53–57. https://doi.org/10.1111/j.1751-553X.2007.00900.x
Pfreundschuh M et al (2008) Prognostic significance of maximum tumour (bulk) diameter in young patients with good-prognosis diffuse large-B-cell lymphoma treated with CHOP-like chemotherapy with or without rituximab: an exploratory analysis of the MabThera International Trial Group (MInT) study. Lancet Oncol 9:435–444. https://doi.org/10.1016/s1470-2045(08)70078-0
Habermann T et al (2006) Rituximab-CHOP versus CHOP alone or with maintenance rituximab in older patients with diffuse large B-cell lymphoma. J Clin Oncol 24:3121–3127. https://doi.org/10.1200/jco.2005.05.1003
Coiffier B et al (2002) CHOP chemotherapy plus rituximab compared with CHOP alone in elderly patients with diffuse large-B-cell lymphoma. N Engl J Med 346:235–242. https://doi.org/10.1056/NEJMoa011795
Takasaki H et al (2015) Post-treatment PET-CT Findings may predict the prognosis of DLBCL with a bulky mass. Indian J Hematol Blood Transfus 31:346–351. https://doi.org/10.1007/s12288-014-0479-9
Ribera J (2008) Adverse prognosis of bulky disease in good-risk DLBCL. Lancet Oncol 9:406–407. https://doi.org/10.1016/s1470-2045(08)70111-6
Tokola S, Kuitunen H, Turpeenniemi-Hujanen T, Kuittinen O (2020) Significance of bulky mass and residual tumor-treated with or without consolidative radiotherapy-To the risk of relapse in DLBCL patients. Cancer Med 9:1966–1977. https://doi.org/10.1002/cam4.2798
Gutierrez A et al (2020) Evaluation of the MD Anderson tumor score for diffuse large B-cell lymphoma in the rituximab era. Eur J Haematol 104:400–408. https://doi.org/10.1111/ejh.13364
Bari A et al (2010) Prognostic models for diffuse large B-cell lymphoma in the rituximab era: a never-ending story. Ann Oncol 21:1486–1491. https://doi.org/10.1093/annonc/mdp531
Acknowledgements
The authors would like to thank all the doctors, nurses, and patients as well as their families for their contribution to this study.
Funding
This work was financially supported by the Scientific Research Foundation of Fujian Cancer Hospital (grant numbers 2021YNY02); Natural Science Foundation of Fujian Province (grant numbers 2023J05241); China Postdoctoral Science Foundation (grant numbers 2023M734015); and China National Major Project for New Drug Innovation (grant numbers 2017ZX09304015).
Author information
Authors and Affiliations
Contributions
Yuankai Shi: conceptualization, methodology, resources, writing—review and editing, supervision, funding acquisition; Chuanben Chen: conceptualization, methodology, resources, writing—review and editing, project administration; Qiaofeng Zhong: methodology, software, formal analysis, investigation, data curation, writing—original draft, writing—review and editing, visualization, project administration, funding acquisition; Haizhu Chen: formal analysis, investigation, data curation, writing—original draft, writing—review and editing, visualization; Daoguang Chen: validation, investigation, resources, data curation, visualization, project administration; Yan Qin: investigation, resources, data curation; Xiaohui He: investigation, resources, data curation; Yu Yang: resources, data curation; Jianliang Yang: resources, data curation; Peng Liu: resources, data curation; Shengyu Zhou: resources, data curation; Sheng Yang: resources, data curation; Yu Zhou: investigation, data curation; Le Tang: investigation, data curation.
Corresponding authors
Ethics declarations
Ethics approval
This study was performed in accordance with the Declaration of Helsinki and approved by the Institutional Review Board of Cancer Hospital, Chinese Academy of Medical Sciences (No. NCC2018JJJ-004) and Fujian Cancer Hospital (No. SQ2022-090–01).
Competing interests
The authors declare no competing interests.
Informed consent
Informed consent was waived due to the retrospective nature of the present study, and data of the participants have been anonymized.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Qiaofeng Zhong, Haizhu Chen, and Daoguang Chen contributed equally to this work as co-first authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhong, Q., Chen, H., Chen, D. et al. Development and validation of a novel risk stratification model and a survival rate calculator for diffuse large B-cell lymphoma in the rituximab era: a multi-institutional cohort study. Ann Hematol 103, 211–226 (2024). https://doi.org/10.1007/s00277-023-05491-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-023-05491-0