Abstract
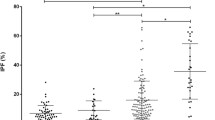
The bleeding risk in immune thrombocytopenia (ITP) is related not only to low platelet count but also to the presence of platelet dysfunction. However, diagnosing a concomitant platelet dysfunction is challenging as most of the available platelet function assays (PFAs) require a platelet count of greater than 100,000/μL. Sonoclot coagulation and platelet function analyzer works on the principle of viscoelastometry, and results remain unaffected by the platelet counts. To assess the platelet function in adult acute ITP patients with the help of sonoclot coagulation and platelet function analyzer and correlate it with the risk of bleeding. Newly diagnosed acute ITP patients with a platelet count less than 20,000/μL were divided into two groups based on WHO bleeding grade: ITP non-bleeder (ITP-NB) group (WHO bleeding grade ≤1) and ITP bleeder (ITP-B) group (WHO bleeding grade ≥2). Platelet function was assessed by sonoclot in both groups. The patients without significant bleeding (ITP-NB) were followed up monthly for six months with the assessment of platelet function during each contact. Eighty patients (30 ITP-B and 50 ITP-NB) were prospectively included in this study. The median age of patients in the two groups was 37 years and 30 years, respectively. The female-to-male ratio was 4:1 and 1:1 in ITP-B and ITP-NB groups. The median platelet count in ITP-B and ITP-NB was 12000/μL (range 1000–19000/μL) and 8000/μL (range 1000–19000/μL), respectively. Mean platelet functions by sonoclot in both groups were lower than the normal cut-off (>1.6). However, the mean platelet function in the ITP-B group (0.2 + 0.17) was significantly lower than the ITP-NB group (1.2 ± 0.52) (p = 0.01). During the follow-up period of 6 months, patients in ITP-NB with a normal platelet function (>1.6) on sonoclot had lesser episodes (one episode) of clinically significant bleeding than patients with a low platelet function (4 episodes). Patients with acute severe thrombocytopenia and bleeding phenotype have a greater abnormality on platelet function by sonoclot than patients with non-bleeding phenotype. This information may help in taking therapeutic decisions in patients with acute ITP.




Similar content being viewed by others
References
Sandal R, Mishra K, Jandial A, Sahu KK, Siddiqui AD (2021) Update on diagnosis and treatment of immune thrombocytopenia. Expert Rev Clin Pharmacol 14(5):553–568
Psaila B, Bussel JB, Frelinger AL, Babula B, Linden MD, Li Y et al (2011) Differences in platelet function in patients with acute myeloid leukemia and myelodysplasia compared to equally thrombocytopenic patients with immune thrombocytopenia. J Thromb Haemost 9(11):2302–2310
Mishra K, Sahu KK (2022) Re: risk factors and predictors of treatment responses and complications in immune thrombocytopenia. Ann Hematol 101(2):447–448
Mishra K, Jandial A, Malhotra P, Varma N (2017) Wet purpura: a sinister sign in thrombocytopenia. BMJ Case Rep 2017:1–2
Malhotra P, Prasad H, Jain A, Gupta V, Varma N (2021) Variables affecting the presence of occult cerebral microbleeds and subsequent spontaneous intracranial haemorrhage in adult patients with severe thrombocytopenia. Br J Haematol 194(3):e67–e70
Neunert C, Terrell DR, Arnold DM, Buchanan G, Cines DB, Cooper N et al (2019) American Society of Hematology 2019 guidelines for immune thrombocytopenia. Blood Adv 3(23):3829–3866
Khera S, Pramanik SK, Yanamandra U, Mishra K, Kapoor R, Das S (2020) Dapsone: an old but effective therapy in pediatric refractory immune thrombocytopenia. Indian J Hematol Blood Transfus 36:690–694
Slichter SJ (2004) Relationship between platelet count and bleeding risk in thrombocytopenic patients. Transfus Med Rev 18(3):153–167
Frelinger AL 3rd, Grace RF, Gerrits AJ, Berny-Lang MA, Brown T, Carmichael SL et al (2015) Platelet function tests, independent of platelet count, are associated with bleeding severity in ITP. Blood 126(7):873–879
Mishra K, Jandial A, Sandal R, Porchezhian P, Charan S, Kumar LDP et al (2018) Poor platelet function on sonoclot signature is associated with high incidence of bleeding in severe immune thrombocytopenia. Blood 132(Supplement 1):4991
Bhoria P, Varma N, Malhotra P, Varma S, Luthra-Guptasarma M. Immunodiagnosis of platelet activation in immune thrombocytopenia through scFv antibodies cognate to activated IIb3 integrins. MAbs 2015;7(6):1212-1220 Taylor & Francis.
Picker SM (2011) In-vitro assessment of platelet function. Transfus Apher Sci 44(3):305–319
Liszka-Hackzell JJ, Ekback G (2002) Analysis of the information content in sonoclot data and reconstruction of coagulation test variables. J Med Syst 26(1):1–8
Sienco® I. Sonoclot® coagulation & platelet function analyzer with graphics printer for in vitro diagnostic use operator’s manual for firmware version 4. 2004 https://www.sienco.com/sonoclot-usa/sonoclot-usa/user-manuals/020-1001-user-manual-r401.pdf.
Ganter MT, Hofer CK (2008) Coagulation monitoring: current techniques and clinical use of viscoelastic point-of-care coagulation devices. Anesth Analg 106(5):1366–1375
Gunduz E, Akay OM, Bal C, Gulbas Z (2011) Can thrombelastography be a new tool to assess bleeding risk in patients with idiopathic thrombocytopenic purpura? Platelets 22(7):516–520
Neunert C, Lim W, Crowther M, Cohen A, Solberg L Jr, Crowther MA (2011) The American Society of Hematology 2011 evidence-based practice guideline for immune thrombocytopenia. Blood 117(16):4190–4207
Varma S, Kumar S, Garg A, Malhotra P, Das A, Sharma A et al (2011) Hepatitis C virus infection among patients with chronic immune thrombocytopenic purpura in northern India. J Clin Exp Hepatol 1(2):68–72
Webert K, Cook RJ, Sigouin CS, Rebulla P, Heddle NM (2006) The risk of bleeding in thrombocytopenic patients with acute myeloid leukemia. Haematologica 91(11):1530–1537
Saxena P, Bihari C, Rastogi A, Agarwal S, Anand L, Sarin SK (2013) Sonoclot signature analysis in patients with liver disease and its correlation with conventional coagulation studies. Adv Hematol 2013:237351
Provan D, Arnold DM, Bussel JB, Chong BH, Cooper N, Gernsheimer T et al (2019) Updated international consensus report on the investigation and management of primary immune thrombocytopenia. Blood Adv 3(22):3780–3817
Rodeghiero F, Stasi R, Gernsheimer T, Michel M, Provan D, Arnold DM et al (2009) Standardization of terminology, definitions and outcome criteria in immune thrombocytopenic purpura of adults and children: report from an international working group. Blood 113(11):2386–2393
van Bladel ER, Laarhoven AG, van der Heijden LB, Heitink-Pollé KM, Porcelijn L, van der Schoot CE et al (2014) Functional platelet defects in children with severe chronic ITP as tested with 2 novel assays applicable for low platelet counts. Blood 123(10):1556–1563
Middelburg RA, Carbaat-Ham JC, Hesam H, Ragusi MA, Zwaginga JJ (2016) Platelet function in adult ITP patients can be either increased or decreased, compared to healthy controls, and is associated with bleeding risk. Hematology 21(9):549–551
Panzer S, Rieger M, Vormittag R, Eichelberger B, Dunkler D, Pabinger I (2007) Platelet function to estimate the bleeding risk in autoimmune thrombocytopenia. Eur J Clin Invest 37(10):814–819
Eldor A, Avitzour M, Or R, Hanna R, Penchas S (1982) Prediction of haemorrhagic diathesis in thrombocytopenia by mean platelet volume. Br Med J (Clin Res Ed) 285(6339):397–400
Kenet G, Lubetsky A, Shenkman B, Tamarin I, Dardik R, Rechavi G et al (1998) Cone and platelet analyser (CPA): a new test for the prediction of bleeding among thrombocytopenic patients. Br J Haematol 101(2):255–259
Mishra K, Kumar S, Singh K, Jandial A, Sandal R, Sahu KK et al (2022) Real-world experience of anti-D immunoglobulin in immune thrombocytopenia. Ann Hematol 101(6):1173–1179
Mishra K, Kumar S, Jandial A, Sahu KK, Sandal R, Ahuja A et al (2021) Real-world experience of rituximab in immune thrombocytopenia. Indian J Hematol Blood Transfus 37(3):404–413
Mishra K, Pramanik S, Sandal R, Jandial A, Sahu KK, Singh K et al (2021) Safety and efficacy of azathioprine in immune thrombocytopenia. Am J Blood Res 11(3):217–226
Stern MP, DeVos-Doyle K, Viguera MG, Lajos TZ (1989) Evaluation of post-cardiopulmonary bypass sonoclot signatures in patients taking nonsteroidal anti-inflammatory drugs. J Cardiothorac Anesth 3(6):730–733
Miyashita T, Kuro M (1998) Evaluation of platelet function by sonoclot analysis compared with other hemostatic variables in cardiac surgery. Anesth Analg 87(6):1228–1233
Mishra K, Malhotra P, Jandial A, Kumar LDP, Varma N, Dhiman R et al (2017) Bleeding risk assessment by sonoclot in severe immune thrombocytopenia. Blood 130(Supplement 1):2320
Hett DA, Walker D, Pilkington SN, Smith DC (1995) Sonoclot analysis. Br J Anaesth 75(6):771–776
Tuman KJ, Spiess BD, McCarthy RJ, Ivankovich AD (1989) Comparison of viscoelastic measures of coagulation after cardiopulmonary bypass. Anesth Analg 69(1):69–75
Furuhashi M, Ura N, Hasegawa K, Yoshida H, Tsuchihashi K, Miura T et al (2002) Sonoclot coagulation analysis: new bedside monitoring for determination of the appropriate heparin dose during haemodialysis. Nephrol Dial Transplant 17(8):1457–1462
Yang WX, Lai CL, Chen FH, Wang JR, Ji YR, Wang DX (2017) The value of sonoclot detection technology to guide the clinical medication of the perioperative anticoagulation and antiplatelet therapy in patients with acute myocardial infarction undergoing emergent PCI. Exp Ther Med 13(6):2917–2921
Haas T, Spielmann N, Mauch J, Madjdpour C, Speer O, Schmugge M et al (2012) Comparison of thromboelastometry (ROTEM®) with standard plasmatic coagulation testing in paediatric surgery. Br J Anaesth 108(1):36–41
De Caterina R, Lanza M, Manca G, Strata GB, Maffei S, Salvatore L (1994) Bleeding time and bleeding: an analysis of the relationship of the bleeding time test with parameters of surgical bleeding. Blood 84(10):3363–3370
Uhl L, Assmann SF, Hamza TH, Harrison RW, Gernsheimer T, Slichter SJ (2017) Laboratory predictors of bleeding and the effect of platelet and RBC transfusions on bleeding outcomes in the PLADO trial. Blood 130(10):1247–1258
Carson JL, Stanworth SJ (2017) Anemia and bleeding in thrombocytopenic patients. Blood 130(10):1178–1179
Valeri CR, Cassidy G, Pivacek LE, Ragno G, Lieberthal W, Crowley JP et al (2001) Anemia-induced increase in the bleeding time: implications for treatment of nonsurgical blood loss. Transfusion 41(8):977–983
Friedmann AM, Sengul H, Lehmann H, Schwartz C, Goodman S (2002) Do basic laboratory tests or clinical observations predict bleeding in thrombocytopenic oncology patients? A reevaluation of prophylactic platelet transfusions. Transfus Med Rev 16(1):34–45
Acknowledgements
We thank Mrs. Lalita for her untiring support. We also thank Mrs. Kusum for her help in data analysis. We thank all our patients for their unconditional support.
Author information
Authors and Affiliations
Contributions
K Mishra, A Jandial, D Lad, G Prakash, A Khadwal, R Kapoor, S Varma, and P Malhotra designed the study. K Mishra, A Jandial, R Sandal, and A Meshram performed the research. RK Dhiman, J Ahluwalia, Neelam Varma, and P Malhotra contributed essential reagents. K Mishra, A Jandial, D Lad, R Kapoor, and P Malhotra analyzed the data. K Mishra, A Jandial, and R Sandal wrote the paper. The manuscript was critically reviewed by all the authors. The final manuscript was vetted by all authors prior to submission.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed signed written consent was taken from the patient involved.
Human and animal rights
No animals were involved in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mishra, K., Jandial, A., Sandal, R. et al. Bleeding risk assessment in immune thrombocytopenia. Ann Hematol 102, 3007–3014 (2023). https://doi.org/10.1007/s00277-023-05466-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-023-05466-1