Abstract
Background
Intense pulsed light (IPL) has been widely used to improve cutaneous photoaging in recent years. Several studies began to explore the changes of skin barrier function after treatment, but the changes of skin surface lipids (SSL), especially specific lipid content and types are still unclear.
Methods
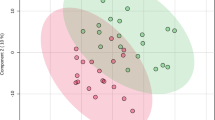
A total of 25 female volunteers were included in our study, and each of them received three full-face treatments with one month apart. Before the first treatment and 1 month after the last treatment, we collected clinical photos and skin stratum corneum samples from individuals. A 5-level scale was used to evaluate the efficacy of IPL treatment, liquid chromatography-mass spectrometry (LC-MS), and Orthogonal Partial Least Squares Discrimination Analysis (OPLS-DA) were used to analyze the changes of SSL.
Results
Two patients got no improvement after treatment, 6 patients had poor improvement and mild improvement was achieved in 9 patients, 5 and 3 patients reported moderate and significant improvement. The overall “effective” rate was 68 % and the “significant effective” rate was 32 %. The results showed 18 lipid subclasses and 487 lipid molecules were identified. The change of total lipid volume was not statistically significant (P = 0.088>0.05), but lipid subclass analysis showed the amount of Triglyceride (TG), Phosphatidic Acid (PA), Phosphatidylglycerol (PG) and Lysophosphatidylglycerol (LPG) were significantly increased (P < 0.05). There were 55 kinds of lipid molecules with significant difference after treatment (P < 0.05), and 51 of them belong to TG. The analysis of chain saturation of TG showed that the quantity of TG with 0, 1 and 2 unsaturated bonds increased significantly (P < 0.05).
Conclusions
IPL treatment does not have a significant effect on the overall amount of lipids while the amount of TG, PA, PG, LPG were significantly increased. These lipid changes may potentially improve the skin barrier function, but more high-quality and comprehensive studies are still needed.
Bullet Point
Lipidomics analysis based on LC-MS; Changes of skin surface lipid after IPL treatment; the relationships between skin surface lipid and skin barrier functions.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.






Similar content being viewed by others
References
Anderson RR, Parrish JA (1983) Selective photothermolysis: precise microsurgery by selective absorption of pulsed radiation. Science 220(4596):524–527
Li D, Lin SB, Cheng B (2016) Intense pulsed light: from the past to the future. Photomed Laser Surg 34(10):435–447
Chang HC, Chang YS (2022) Pulsed dye laser versus intense pulsed light for facial erythema of rosacea: a systematic review and meta-analysis. J Dermatolog Treat 33(4):2394–2396
Fodor L, Carmi N, Fodor A, Ramon Y, Ullmann Y (2009) Intense pulsed light for skin rejuvenation, hair removal, and vascular lesions: a patient satisfaction study and review of the literature. Ann Plast Surg 62(4):345–349
Sales A, Pandolfo IL, de Almeida CM (2022) Intense pulsed light on skin rejuvenation: a systematic review. Arch Dermatol Res 314(9):823–838
Kwan KR, Kolansky Z, Abittan BJ, Farberg AS, Goldenberg G (2020) Skin tightening. Cutis 106(3):134–137
Goldman MP, Weiss RA, Weiss MA (2005) Intense pulsed light as a nonablative approach to photoaging. Dermatol Surg 31(9 Pt 2):1179–1187
Jensen JM, Proksch E (2009) The skin’s barrier. G Ital Dermatol Venereol 144(6):689–700
Brettmann EA, de Guzman SC (2018) Recent evolution of the human skin barrier. Exp Dermatol 27(8):859–866
Zhou M, Gan Y, Yang M, He C, Jia Y (2020) Lipidomics analysis of facial skin surface lipids between forehead and cheek: Association between lipidome, TEWL, and pH. J Cosmet Dermatol 19(10):2752–2758
Kendall AC, Koszyczarek MM, Jones EA (2018) Lipidomics for translational skin research: a primer for the uninitiated. Exp Dermatol 27(7):721–728
Shin JW, Lee DH, Choi SY (2011) Objective and non-invasive evaluation of photorejuvenation effect with intense pulsed light treatment in Asian skin. J Eur Acad Dermatol Venereol 25(5):516–522
Alexiades-Armenakas M (2009) Assessment of the mobile delivery of infrared light (1100–1800 nm) for the treatment of facial and neck skin laxity. J Drugs Dermatol 8(3):221–226
Feingold KR, Elias PM (2014) Role of lipids in the formation and maintenance of the cutaneous permeability barrier. Biochim Biophys Acta 3:280–294
Cajka T, Fiehn O (2014) Comprehensive analysis of lipids in biological systems by liquid chromatography-mass spectrometry. Trends Analyt Chem 61:192–206
Radner FP, Fischer J (2014) The important role of epidermal triacylglycerol metabolism for maintenance of the skin permeability barrier function. Biochim Biophys Acta 3:409–415
Ackerman D, Tumanov S, Qiu B (2018) Triglycerides promote lipid homeostasis during hypoxic stress by balancing fatty acid saturation. Cell Rep 24(10):2596–2605
Esch P, Heiles S (2020) Investigating C[double bond, length as m-dash]C positions and hydroxylation sites in lipids using Paternò-Büchi functionalization mass spectrometry. Analyst 145(6):2256–2266
You L, Fan Y, Liu X (2020) Liquid chromatography-mass spectrometry-based tissue metabolic profiling reveals major metabolic pathway alterations and potential biomarkers of lung cancer. J Proteome Res 19(9):3750–3760
Xie D, Seremwe M, Edwards JG, Podolsky R, Bollag WB (2014) Distinct effects of different phosphatidylglycerol species on mouse keratinocyte proliferation. PLoS ONE 9(9):e107119
Choudhary V, Uaratanawong R, Patel RR (2019) Phosphatidylglycerol inhibits toll-like receptor-mediated inflammation by danger-associated molecular patterns. J Invest Dermatol 139(4):868–877
Xie D, Choudhary V, Seremwe M (2018) Soy phosphatidylglycerol reduces inflammation in a contact irritant ear edema mouse model in vivo. J Pharmacol Exp Ther 366(1):1–8
Monnot GC, Wegrecki M, Cheng TY (2023) Staphylococcal phosphatidylglycerol antigens activate human T cells via CD1a. Nat Immunol 24(1):110–122
Makide K, Kitamura H, Sato Y, Okutani M, Aoki J (2009) Emerging lysophospholipid mediators, lysophosphatidylserine, lysophosphatidylthreonine, lysophosphatidylethanolamine and lysophosphatidylglycerol. Prostaglandins Other Lipid Mediat 89(3–4):135–139
Chen J, Cazenave-Gassiot A, Xu Y (2023) Lysosomal phospholipase A2 contributes to the biosynthesis of the atypical late endosome lipid bis(monoacylglycero)phosphate. Commun Biol 6(1):210
Shim JW, Jo SH, Kim SD, Lee HY, Yun J, Bae YS (2009) Lysophosphatidylglycerol inhibits formyl peptide receptorlike-1-stimulated chemotactic migration and IL-1beta production from human phagocytes. Exp Mol Med 41(8):584–591
Yau A, Fear MW, Gray N (2022) Enhancing the accuracy of surgical wound excision following burns trauma via application of rapid evaporative ionisationmass spectrometry (REIMS). Burns 48(7):1574–1583
Cho S, Kim HH, Lee MJ, Lee S, Park CS, Nam SJ, Han JJ, Kim JW, Chung JH (2008) Phosphatidylserine prevents UV-induced decrease of type I procollagen and increase of MMP-1 in dermal fibroblasts and human skin in vivo. J Lipid Res 49(6):1235–1245
Funding
This study was supported by Hangzhou health science and technology key project (No 20220054).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest to disclose.
Ethical Approval
All procedures performed in studies involving humanparticipants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
All participants have given their informed consent in writing prior to inclusion in the study, any identifying details of the participants will not be published in written descriptions, photographs, and genetic profiles, and the participant has given written informed consent for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cai, Y., Xiang, W. Changes of Facial Lipidomics by Intense Pulsed Light Treatment Based on LC-MS. Aesth Plast Surg 48, 2171–2178 (2024). https://doi.org/10.1007/s00266-023-03842-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-023-03842-w