Abstract
Objective
To construct a scoring model based on MRI signs to predict massive hemorrhage during dilatation and curettage in cesarean scar pregnancy (CSP) patients.
Materials and methods
The MRIs of CSP patients admitted to a tertiary referral hospital between February 2020 and July 2022 were retrospectively reviewed. The included patients were randomly assigned to the training and validation cohorts. The univariate and multivariate logistic regression analyses were adopted to identify the independent risk factors for massive hemorrhage (the amount of bleeding ≥ 200 ml) during the dilatation and curettage. A scoring model predicting intraoperative massive hemorrhage was established where each positive independent risk factor was assigned 1 point, and the predictive power of this model was evaluated both in the training and validation cohorts via the receiver operating characteristic curve.
Results
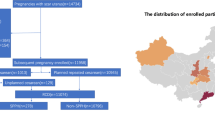
A total of 187 CSP patients were enrolled, who were divided into the training cohort (31 in 131 patients had massive hemorrhage) and validation cohort (10 in 56 patients had massive hemorrhage). The independent risk factors for intraoperative massive hemorrhage included cesarean section diverticulum area (OR = 6.957, 95% CI 1.993–21.887; P = 0.001), uterine scar thickness (OR = 5.113, 95% CI 2.086–23.829; P = 0.025) and gestational sac diameter (OR = 3.853, 95% CI 1.103–13.530; P = 0.025). A scoring model with a total point of 3 was developed and the CSP patients were divided into low-risk (Total points < 2) and high-risk groups (Total points ≥ 2) for intraoperative massive hemorrhage accordingly. This model possessed high prediction performance both in the training cohort (area under the curve [AUC] = 0.896, 95% CI 0.830–0.942) and validation cohort (AUC = 0.915, 95% CI 0.785–1.000).
Conclusion
We first constructed a MRI-based scoring model for predicting intraoperative massive hemorrhage in CSP patients, which could help the decision-making of the patients’ therapy strategies. Low-risk patients can be cured by D&C alone to reduce the financial burden, while high-risk patients require more adequate preoperative preparation or consideration of changing surgical approaches to reduce bleeding risk.
Graphical abstract







Similar content being viewed by others
Abbreviations
- CSP:
-
Cesarean scar pregnancy
- D&C:
-
Dilatation and curettage
- MRI:
-
Magnetic resonance imaging
- β-hCG:
-
β-Human chorionic gonatropin
- TR:
-
Repetition time
- TE:
-
Echo time
- FOV:
-
Field of view
- CSD:
-
Cesarean section diverticulum
- ICC:
-
Interclass correlation coefficient
- ROC:
-
Receiver operating characteristic curve
- AUC:
-
Area under the curve
- CI:
-
Confidence interval
References
Grechukhina O, Deshmukh U, Fan L, et al. Cesarean Scar Pregnancy, Incidence, and Recurrence: Five-Year Experience at a Single Tertiary Care Referral Center [J]. Obstet Gynecol, 2018,132(5): 1285-1295.
Shah JS, Nasab S. Management and reproductive counseling in cervical, caesarean scar and interstitial ectopic pregnancies over 11 years: identifying the need for a modern management algorithm [J]. Hum Reprod Open, 2019,2019(4): hoz028.
Family Planning Subgroup CSoOaG, Chinese Medical Association. [Expert opinion of diagnosis and treatment of cesarean scar pregnancy (2016)] [J]. Zhonghua Fu Chan Ke Za Zhi, 2016,51(8): 568-572.
Le A, Li M, Xu Y, et al. Different Surgical Approaches to 313 Cesarean Scar Pregnancies [J]. J Minim Invasive Gynecol, 2019,26(1): 148-152.
Sun QL, Luo L, Gao CY, et al. Scoring system for the prediction of the successful treatment modality in women with cesarean scar pregnancy [J]. Int J Gynaecol Obstet, 2019,146(3): 289-295.
Wang Q, Ma H, Peng H, et al. Risk factors for intra-operative haemorrhage and bleeding risk scoring system for caesarean scar pregnancy: a case-control study [J]. Eur J Obstet Gynecol Reprod Biol, 2015,195: 141-145.
Ma Y, Shao M, Shao X. Analysis of risk factors for intraoperative hemorrhage of cesarean scar pregnancy [J]. Medicine (Baltimore), 2017,96(25): e7327.
Chiang YC, Tu YA, Yang JH, et al. Risk factors associated with failure of treatment for cesarean scar pregnancy [J]. Int J Gynaecol Obstet, 2017,138(1): 28-36.
Zhang Y, Chen L, Zhou M, et al. Risk factors of persistent cesarean scar pregnancy after dilation and curettage: a matched case-control study [J]. Taiwan J Obstet Gynecol, 2020,59(2): 237-242.
Lin Y, Xiong C, Dong C, et al. Approaches in the Treatment of Cesarean Scar Pregnancy and Risk Factors for Intraoperative Hemorrhage: A Retrospective Study [J]. Front Med (Lausanne), 2021,8: 682368.
Liu D, Yang M, Wu Q. Application of ultrasonography in the diagnosis and treatment of cesarean scar pregnancy [J]. Clin Chim Acta, 2018,486: 291-297.
Peng KW, Lei Z, Xiao TH, et al. First trimester caesarean scar ectopic pregnancy evaluation using MRI [J]. Clin Radiol, 2014,69(2): 123-129.
Xiao X, Ding R, Peng L, et al. Diagnostic performance of magnetic resonance imaging and ultrasonography on the detection of cesarean scar pregnancy: A meta-analysis [J]. Medicine (Baltimore), 2021,100(48): e27532.
Guo S, Wang H, Yu X, et al. The diagnostic value of 3.0T MRI in cesarean scar pregnancy [J]. Am J Transl Res, 2021,13(6): 6229-6235.
Hoffmann J, Exner M, Bremicker K, et al. Cesarean section scar in 3 T magnetic resonance imaging and ultrasound: image characteristics and comparison of the methods [J]. Arch Gynecol Obstet, 2019,299(2): 439-449.
Du Q, Liu G, Zhao W. A novel method for typing of cesarean scar pregnancy based on size of cesarean scar diverticulum and its significance in clinical decision-making [J]. J Obstet Gynaecol Res, 2020,46(5): 707-714.
Du Q, Zhao W. Exploring the value of cesarean section diverticulum area to predict the safety of hysteroscopic management for cesarean scar pregnancy patients [J]. Int J Gynaecol Obstet, 2022,156(3): 488-493.
Wang X, Yang B, Chen W, et al. Clinical efficacy and re-pregnancy outcomes of patients with previous cesarean scar pregnancy treated with either high-intensity focused ultrasound or uterine artery embolization before ultrasound-guided dilatation and curettage: a retrospective cohort study [J]. BMC Pregnancy Childbirth, 2023,23(1): 85.
Wang J, Zhao R, Qian H, et al. Pituitrin local injection versus uterine artery embolization in the management of cesarean scar pregnancy: A retrospective cohort study [J]. J Obstet Gynaecol Res, 2021,47(5): 1711-1718.
Soares DM, Junior HW, Bittencourt LK, et al. The role of cine MR imaging in the assessment of uterine function [J]. Arch Gynecol Obstet, 2019,300(3): 545-553.
Fang Q, Sun L, Tang Y, et al. Quantitative risk assessment to guide the treatment of cesarean scar pregnancy [J]. Int J Gynaecol Obstet, 2017,139(1): 78-83.
Tang M, Zhou Q, Huang M, et al. Nomogram development and validation to predict hepatocellular carcinoma tumor behavior by preoperative gadoxetic acid-enhanced MRI [J]. Eur Radiol, 2021,31(11): 8615-8627.
Mu L, Weng H, Wang X. Evaluation of the treatment of high intensity focused ultrasound combined with suction curettage for exogenous cesarean scar pregnancy [J]. Arch Gynecol Obstet, 2022,306(3): 769-777.
Sun QL, Wu XH, Luo L, et al. Characteristics of women with mixed mass formation after evacuation following uterine artery chemoembolization for cesarean scar pregnancy [J]. Arch Gynecol Obstet, 2018,297(4): 1059-1066.
Bourgioti C, Konstantinidou A, Zafeiropoulou K, et al. Intraplacental Fetal Vessel Diameter May Help Predict for Placental Invasiveness in Pregnant Women at High Risk for Placenta Accreta Spectrum Disorders [J]. Radiology, 2020,298(2): 403-412.
Ueno Y, Maeda T, Tanaka U, et al. Evaluation of interobserver variability and diagnostic performance of developed MRI-based radiological scoring system for invasive placenta previa [J]. J Magn Reson Imaging, 2016,44(3): 573-583.
Wang Y, Zhu Q, Lin F, et al. Development and internal validation of a Nomogram for preoperative prediction of surgical treatment effect on cesarean section diverticulum [J]. BMC Womens Health, 2019,19(1): 136.
Gui T, Peng P, Liu X, et al. Clinical and ultrasound parameters in prediction of excessive hemorrhage during management of cesarean scar pregnancy [J]. Ther Clin Risk Manag, 2017,13: 807-812.
Ying X, Zheng W, Zhao L, et al. Clinical characteristics and salvage management of persistent cesarean scar pregnancy [J]. J Obstet Gynaecol Res, 2017,43(8): 1293-1298.
Liu J, Chai Y, Yu Y, et al. The value of 3-dimensional color Doppler in predicting intraoperative hemorrhage for cesarean scar pregnancy [J]. Medicine(Baltimore), 2018,97(33): e11969.
Zhang Y, Zhang C, He J, et al. The impact of gestational sac size on the effectiveness and safety of high intensity focused ultrasound combined with ultrasound-guided suction curettage treatment for caesarean scar pregnancy [J]. Int J Hyperthermia, 2018,35(1): 291-297.
Acknowledgements
The authors want to thank the Chengdu Municipal Health Commission for the financial support. The authors would like to dedicate the paper as a memorial for the wedding of Dr. Fengleng Yang and Miss Fanyu Lin on 18 June 2023.
Funding
This study has received funding by the Chengdu Medical Research Projects (Grant No. 2021030).
Author information
Authors and Affiliations
Contributions
FLY and ZGW participated in the conception/design. HBJ and XDW participated in the provision of study material or patients. YZS, XDW, and CD participated in the collection and/or assembly of data. FLY and YZS participated in the data analysis and interpretation. FLY and XLY participated in the manuscript writing. HL and ZGW participated in the manuscript revision. All authors contributed to final approval of manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
This study was approved by the medical ethics committee of Chengdu women’s and children’s Central Hospital [Approval number: 2021 (107)], and the written informed consent of the research subjects was also obtained.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, F., Yang, X., Jing, H. et al. MRI-based scoring model to predict massive hemorrhage during dilatation and curettage in patients with cesarean scar pregnancy. Abdom Radiol 48, 3195–3206 (2023). https://doi.org/10.1007/s00261-023-03968-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-023-03968-0