Abstract
Purpose
To identify features on preoperative MR imaging with diffusion-weighted imaging (DWI) for predicting next-generation sequencing (NGS)-based tumor cellularity and patient outcome after surgical resection of pancreatic ductal adenocarcinoma (PDAC).
Methods
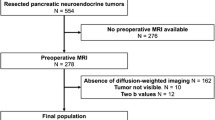
This retrospective study included 105 patients with surgically resected PDAC who underwent preoperative MR imaging with DWI. Tumor cellularity was measured using molecular techniques and bioinformatics methods. Clinico-pathologic findings including tumor T stage for predicting disease-free survival (DFS) and overall survival (OS) were identified using Cox proportional hazards model. Important MR imaging findings including apparent diffusion coefficient (ADC) value of PDAC and modified ADC value (the ratio of the ADC value of PDAC to the ADC value of the spleen) for predicting higher tumor cellularity (≥ 30%) and poor prognosis were also identified.
Results
The median DFS and OS were 12.0 months [95% confidence interval (CI), 8.0–17.0] and 22.0 months (95% CI, 18.0–29.0), respectively. Higher T stage (T3/4) [hazard ratio (HR), 7.720, (95% CI 1.072, 55.612); p = 0.048] and higher tumor cellularity [HR, 1.599 (95% CI, 1.003–2.548); p = 0.048] were significantly associated with worse DFS. Among MR imaging features, the modified ADC value was significantly associated with tumor cellularity [odds ratio, 0.068 (95% CI, 0.012–0.372); p = 0.002], and PDAC with lower modified ADC value [≤ 1.40 (cutoff value)] showed significantly shorter median DFS than PDAC with higher modified ADC value [8 months (95% CI, 4–12) vs. 16 months (95% CI, 10–29); HR, 1.713 (95% CI, 1.073–2.735), log-rank p = 0.024].
Conclusion
Higher NGS-based tumor cellularity may be a negative prognostic factor in pancreatic cancer after resection, and modified ADC value derived from DWI could be helpful in predicting tumor cellularity and patient surgical outcome with regard to recurrence.
Graphic abstract






Similar content being viewed by others
Data availability
We declared that materials described in the manuscript, including all relevant raw data, will be freely available to any scientist wishing to use them for non-commercial purposes, without breaching participant confidentiality.
Code availability
All softwares used during the study appear in the submitted article; No code was generated or used during the study.
Abbreviations
- ADC:
-
Apparent diffusion coefficient
- DFS:
-
Disease-free survival
- DWI:
-
Diffusion-weighted imaging
- NGS:
-
Next-generation sequencing
- OS:
-
Overall survival
- PDAC:
-
Pancreatic ductal adenocarcinoma
References
Siegel RL, Miller KD, Jemal A (2020) Cancer statistics, 2020. CA Cancer J Clin 70:7-30
Jang JY, Kang MJ, Heo JS et al (2014) A prospective randomized controlled study comparing outcomes of standard resection and extended resection, including dissection of the nerve plexus and various lymph nodes, in patients with pancreatic head cancer. Ann Surg 259:656-664
Al-Hawary MM, Francis IR, Chari ST et al (2014) Pancreatic ductal adenocarcinoma radiology reporting template: consensus statement of the Society of Abdominal Radiology and the American Pancreatic Association. Radiology 270:248-260
Hidalgo M (2010) Pancreatic cancer. N Engl J Med 362:1605-1617
Sohn TA, Yeo CJ, Cameron JL et al (2000) Resected adenocarcinoma of the pancreas-616 patients: results, outcomes, and prognostic indicators. J Gastrointest Surg 4:567-579
Strom SP (2016) Current practices and guidelines for clinical next-generation sequencing oncology testing. Cancer Biol Med 13:3-11
Shen GQ, Aleassa EM, Walsh RM, Morris-Stiff G (2019) Next-Generation Sequencing in Pancreatic Cancer. Pancreas 48:739-748
Heid I, Steiger K, Trajkovic-Arsic M et al (2017) Co-clinical Assessment of Tumor Cellularity in Pancreatic Cancer. Clin Cancer Res 23:1461-1470
Cho IK, Kim H, Lee JC et al (2020) Higher Tumor Cellularity in Resected Pancreatic Ductal Adenocarcinoma Is a Negative Prognostic Indicator. Gut Liver 14:521-528
Polyak K, Weinberg RA (2009) Transitions between epithelial and mesenchymal states: acquisition of malignant and stem cell traits. Nat Rev Cancer 9:265-273
Winter JM, Ting AH, Vilardell F et al (2008) Absence of E-cadherin expression distinguishes noncohesive from cohesive pancreatic cancer. Clin Cancer Res 14:412-418
Motosugi U, Ichikawa T, Morisaka H et al (2011) Detection of pancreatic carcinoma and liver metastases with gadoxetic acid-enhanced MR imaging: comparison with contrast-enhanced multi-detector row CT. Radiology 260:446-453
Kim JH, Park SH, Yu ES et al (2010) Visually isoattenuating pancreatic adenocarcinoma at dynamic-enhanced CT: frequency, clinical and pathologic characteristics, and diagnosis at imaging examinations. Radiology 257:87-96
Barral M, Taouli B, Guiu B et al (2015) Diffusion-weighted MR imaging of the pancreas: current status and recommendations. Radiology 274:45-63
Altman DG, McShane LM, Sauerbrei W, Taube SE (2012) Reporting recommendations for tumor marker prognostic studies (REMARK): explanation and elaboration. BMC medicine 10:51
Mahadevan D, Von Hoff DD (2007) Tumor-stroma interactions in pancreatic ductal adenocarcinoma. Mol Cancer Ther 6:1186-1197
Biankin AV, Waddell N, Kassahn KS et al (2012) Pancreatic cancer genomes reveal aberrations in axon guidance pathway genes. Nature 491:399-405
Neesse A, Michl P, Frese KK et al (2011) Stromal biology and therapy in pancreatic cancer. Gut 60:861-868
Michl P, Gress TM (2012) Improving drug delivery to pancreatic cancer: breaching the stromal fortress by targeting hyaluronic acid. Gut 61:1377-1379
Özdemir BC, Pentcheva-Hoang T, Carstens JL et al (2014) Depletion of carcinoma-associated fibroblasts and fibrosis induces immunosuppression and accelerates pancreas cancer with reduced survival. Cancer Cell 25:719-734
Hingorani SR, Zheng L, Bullock AJ et al (2018) HALO 202: Randomized Phase II Study of PEGPH20 Plus Nab-Paclitaxel/Gemcitabine Versus Nab-Paclitaxel/Gemcitabine in Patients With Untreated, Metastatic Pancreatic Ductal Adenocarcinoma. J Clin Oncol 36:359-366
Rhim AD, Oberstein PE, Thomas DH et al (2014) Stromal elements act to restrain, rather than support, pancreatic ductal adenocarcinoma. Cancer Cell 25:735-747
Sasaki M, Yamada K, Watanabe Y et al (2008) Variability in absolute apparent diffusion coefficient values across different platforms may be substantial: a multivendor, multi-institutional comparison study. Radiology 249:624-630
Wang Y, Chen ZE, Nikolaidis P et al (2011) Diffusion-weighted magnetic resonance imaging of pancreatic adenocarcinomas: association with histopathology and tumor grade. J Magn Reson Imaging 33:136-142
Muraoka N, Uematsu H, Kimura H et al (2008) Apparent diffusion coefficient in pancreatic cancer: characterization and histopathological correlations. J Magn Reson Imaging 27:1302-1308
Rosenkrantz AB, Matza BW, Sabach A, Hajdu CH, Hindman N (2013) Pancreatic cancer: lack of association between apparent diffusion coefficient values and adverse pathological features. Clin Radiol 68:e191-197
Legrand L, Duchatelle V, Molinié V, Boulay-Coletta I, Sibileau E, Zins M (2015) Pancreatic adenocarcinoma: MRI conspicuity and pathologic correlations. Abdom Imaging 40:85-94
Cros J, Raffenne J, Couvelard A, Poté N (2018) Tumor Heterogeneity in Pancreatic Adenocarcinoma. Pathobiology 85:64-71
Funding
No funds, grants, or other support was received.
Author information
Authors and Affiliations
Contributions
Conception and design: JHK and JJ; Data acquisition: SKJ, WK, HK, and YH; Data analysis and interpretation: SKJ, DK, and DP; Drafting of the manuscript: SKJ and JHK; Critical revision of the manuscript: JHK.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Ethical approval
This study was approved by Institutional Review Board of Seoul National University Hospital (IRB; No 2005-212-1127) and written informed consent was waived. This study was in accordance with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Written informed consent was waived by Institutional Review Board of Seoul National University Hospital due to retrospective design of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Jeon, S.K., Jang, JY., Kwon, W. et al. Diffusion-weighted MR imaging in pancreatic ductal adenocarcinoma: prediction of next-generation sequencing-based tumor cellularity and prognosis after surgical resection. Abdom Radiol 46, 4787–4799 (2021). https://doi.org/10.1007/s00261-021-03177-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-021-03177-7