Abstract
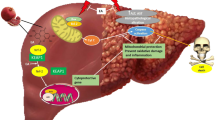
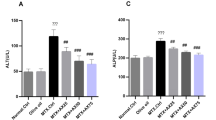
Methotrexate (MTX) is a widely used drug for treatment of many malignant, rheumatic, and autoimmune diseases. However, hepatotoxicity remains one of the most serious side effects of MTX. The extrinsic coagulation pathway is activated after tissue injury through the release of tissue factor (TF) which activates a cascade of clotting factors including prothrombin and fibrinogen. Liver sinusoidal endothelial cells express endothelial nitric oxide synthase (eNOS) as a source for nitric oxide (NO) that serves as vasodilator and antithrombotic factor. In the current study, we tested the possible role of coagulation system activation in MTX-induced hepatotoxicity. Our results showed that single-dose administration of MTX significantly altered rat liver functions with concurrent turbulence in redox status. Immunofluorescence staining showed accumulation of fibrin in the periportal hepatocytes and downregulation of eNOS expression in hepatic endothelial and sinusoidal cells following MTX treatment. Moreover, MTX administration increased the expression of inducible nitric oxide synthase (iNOS) and NOSTRIN (eNOS traffic inducer) in the hepatic sinusoids. On the other hand, pre-treatment with enoxaparin rescued against MTX-induced liver injury with subsequent amelioration of liver redox status. Furthermore, it significantly prevented the effect of MTX on the expression of fibrin, iNOS, eNOS, and NOSTRIN. We concluded that liver tissue aggregation of the coagulation product, fibrin, may play a crucial role in the pathogenesis of MTX-induced liver injury.






Similar content being viewed by others
Change history
29 April 2020
The authors found a mistake in Figure 2 and would like to correct the manuscript.
References
Abdel-Bakky MS, Hammad MA, Walker LA, Ashfaq MK (2011) Tissue factor dependent liver injury causes release of retinoid receptors (RXR-alpha and RAR-alpha) as lipid droplets. Biochem Biophys Res Commun 410:146–151
Abdel-Salam OM, Baiuomy AR, Ameen A, Hassan NS (2005) A study of unfractionated and low molecular weight heparins in a model of cholestatic liver injury in the rat. Pharmacol Res 51:59–67
Bannwarth B, Schaeverbeke T, Labat L, Marce S, Demotes-Mainard F, Dehais J (1994) Side-effects during treatment of rheumatoid arthritis with methotrexate. Rev Rhum Ed Fr 61:337–342
Belfield A, Goldberg DM (1971) Revised assay for serum phenyl phosphatase activity using 4-amino-antipyrine. Enzyme 12:561–573
Beutler E, Duron O, Kelly BM (1963) Improved method for the determination of blood glutathione. J Lab Clin Med 61:882–888
Bishnoi P, Kumari R, Thappa DM (2011) Monitoring methotrexate hepatotoxicity in psoriasis. Indian J Dermatol Venereol Leprol 77:545–548
Claiborne A (1985) Handbook of methods for oxygen radical research, Catalase activity, Boca Raton, Florida 283–284
DeLeve LD, Wang X, Kanel GC, Ito Y, Bethea NW, McCuskey MK, Tokes ZA, Tsai J, McCuskey RS (2003) Decreased hepatic nitric oxide production contributes to the development of rat sinusoidal obstruction syndrome. Hepatology 38:900–908
Ewees MG, Abdelghany TM, Abdel-Aziz AA, Abdel-Bakky MS (2015) All-trans retinoic acid mitigates methotrexate-induced liver injury in rats; relevance of retinoic acid signaling pathway. Naunyn Schmiedeberg's Arch Pharmacol 388:931–938
Fareed J, Hoppensteadt D, Walenga J, Iqbal O, Ma Q, Jeske W, Sheikh T (2003) Pharmacodynamic and pharmacokinetic properties of enoxaparin : implications for clinical practice. Clin Pharmacokinet 42:1043–1057
Hammad MA, Abdel-Bakky MS, Walker LA, Ashfaq MK (2011) Oxidized low-density lipoprotein and tissue factor are involved in monocrotaline/lipopolysaccharide-induced hepatotoxicity. Arch Toxicol 85:1079–1089
Huang L, Si XM, Feng JX (2010) NF-kappaB related abnormal hyper-expression of iNOS and NO correlates with the inflammation procedure in biliary atresia livers. Pediatr Surg Int 26:899–905
Jih DM, Werth VP (1998) Thrombocytopenia after a single test dose of methotrexate. J Am Acad Dermatol 39:349–351
Johnston JA, Johnson ES, Waller PR, Varshavsky A (1995) Methotrexate inhibits proteolysis of dihydrofolate reductase by the N-end rule pathway. J Biol Chem 270:8172–8178
Kukner A, Tore F, Firat T, Terzi EH, Oner H, Balaban YH, Ozogul C (2010) The preventive effect of low molecular weight heparin on CCL(4)-induced necrosis and apoptosis in rat liver. Ann Hepatol 9:445–454
Lapadula G, De BC, Acquista CA, Dell’Accio F, Covelli M, Iannone F (1997) Isolated thrombocytopenia associated with low dose methotrexate therapy. Clin Rheumatol 16:429–430
Longo-Sorbello GS, Bertino JR (2001) Current understanding of methotrexate pharmacology and efficacy in acute leukemias. Use of newer antifolates in clinical trials. Haematologica 86:121–127
Luyendyk JP, Maddox JF, Green CD, Ganey PE, Roth RA (2004) Role of hepatic fibrin in idiosyncrasy-like liver injury from lipopolysaccharide-ranitidine coexposure in rats. Hepatology 40:1342–1351
Luyendyk JP, Mackman N, Sullivan BP (2011) Role of fibrinogen and protease-activated receptors in acute xenobiotic-induced cholestatic liver injury. Toxicol Sci 119:233–243
Mookerjee RP, Wiesenthal A, Icking A, Hodges SJ, Davies NA, Schilling K, Sen S, Williams R, Novelli M, Muller-Esterl W, Jalan R (2007) Increased gene and protein expression of the novel eNOS regulatory protein NOSTRIN and a variant in alcoholic hepatitis. Gastroenterology 132:2533–2541
Neubauer K, Knittel T, Armbrust T, Ramadori G (1995) Accumulation and cellular localization of fibrinogen/fibrin during short-term and long-term rat liver injury. Gastroenterology 108:1124–1135
Nishikimi M, Appaji N, Yagi K (1972) The occurrence of superoxide anion in the reaction of reduced phenazine methosulfate and molecular oxygen. Biochem Biophys Res Commun 46:849–854
Oda M, Yokomori H, Han JY (2003) Regulatory mechanisms of hepatic microcirculation. Clin Hemorheol Microcirc 29:167–182
Park SK, Park SJ, Park SM, Cho IJ, Park CI, Kim YW, Kim SC (2013) Inhibition of acute phase inflammation by Laminaria japonica through regulation of iNOS-NF-kappa B pathway. Evid Based Complement Alternat Med 2013:439498
Pasarin M, La M, Gracia-Sancho VJ, Garcia-Caldero H, Rodriguez-Vilarrupla A, Garcia-Pagan JC, Bosch J, Abraldes JG (2012) Sinusoidal endothelial dysfunction precedes inflammation and fibrosis in a model of NAFLD. PLoS One 7:e32785
Reitman S, Frankel S (1957) A colorimetric method for the determination of serum glutamic oxalacetic and glutamic pyruvic transaminases. Am J Clin Pathol 28:56–63
Sass G, Koerber K, Bang R, Guehring H, Tiegs G (2001) Inducible nitric oxide synthase is critical for immune-mediated liver injury in mice. J Clin Invest 107:439–447
Satoh K (1978) Serum lipid peroxide in cerebrovascular disorders determined by a new colorimetric method. Clin Chim Acta 90:37–43
Sotoudehmanesh R, Anvari B, Akhlaghi M, Shahraeeni S, Kolahdoozan S (2010) Methotrexate hepatotoxicity in patients with rheumatoid arthritis. Middle East J Dig Dis 2:104–109
Steffel J, Luscher TF, Tanner FC (2006) Tissue factor in cardiovascular diseases: molecular mechanisms and clinical implications. Circulation 113:722–731
Van De Casteele M, Van Pelt JF, Nevens F, Fevery J, Reichen J (2003) Low NO bioavailability in CCl4 cirrhotic rat livers might result from low NO synthesis combined with decreased superoxide dismutase activity allowing superoxide-mediated NO breakdown: a comparison of two portal hypertensive rat models with healthy controls. Comp Hepatol 2:2
Vekemans K, Braet F, Muyllaert D, Wisse E (2004) Nitric oxide from rat liver sinusoidal endothelial cells induces apoptosis in IFN gamma-sensitized CC531s colon carcinoma cells. J Hepatol 41:11–18
Wisse E, De Zanger RB, Jacobs R, McCuskey RS (1983) Scanning electron microscope observations on the structure of portal veins, sinusoids and central veins in rat liver. Scan Electron Microsc (Pt 3):1441–1452
Zachariae H (1990) Methotrexate side-effects. Br J Dermatol 122(Suppl 36):127–133
Zimmermann K, Opitz N, Dedio J, Renne C, Muller-Esterl W, Oess S (2002) NOSTRIN: a protein modulating nitric oxide release and subcellular distribution of endothelial nitric oxide synthase. Proc Natl Acad Sci U S A 99:17167–17172
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All animal procedures were approved by the ethical committee in Al-Azhar University and performed in accordance with the regulations of the international guide for the care and use of laboratory animals.
Conflict of interest
The authors declare that there is no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ewees, M.G., Abdelghany, T.M., Abdel-Aziz, AA.H. et al. Enoxaparin prevents fibrin accumulation in liver tissues and attenuates methotrexate-induced liver injury in rats. Naunyn-Schmiedeberg's Arch Pharmacol 392, 623–631 (2019). https://doi.org/10.1007/s00210-019-01618-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-019-01618-1