Abstract
Purpose
The current investigation evaluated the relationship between the synovial fluid cytokine microenvironment at the time of isolated anterior cruciate ligament (ACL) reconstruction and the presence of subsequent chondral wear and radiologic evidence of osteoarthritis (OA) on cartilage-specific MRI sequences at a minimum of 5-year follow-up.
Methods
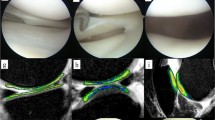
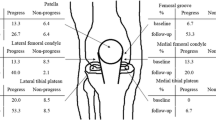
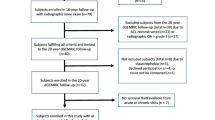
Patients who underwent primary ACL reconstruction with no baseline concomitant cartilage or meniscal defects and had synovial fluid samples obtained at the time of surgery were retrospectively identified. Patients with a minimum of 5 years of postoperative follow-up were contacted and asked to complete patient-reported outcome (PRO) measures including Visual Analog Scale (VAS) for pain, Lysholm Scale, Knee Injury and Osteoarthritis Outcome Score (KOOS), and Tegner Activity Scale, along with postoperative magnetic resonance imaging (MRI). The concentration of ten biomarkers that have previously been suggested to play a role in cartilage degradation and inflammation in the joint space was measured. Linear regression controlling for age, sex, and body mass index (BMI) was performed to create a model using the synovial fluid concentrations at the time of surgery to predict postoperative semiquantitative cartilage lesion size and depth on MRI at a minimum of 5 years follow up.
Results
The patients were comprised of eight males (44.4%) and ten females (55.6%) with a mean age at the time of surgery of 30.8 ± 8.7 years (range 18.2–44.5 years). The mean follow-up time was 7.8 ± 1.5 years post-operatively (range 5.7–9.7 years). MCP-1, VEGF, and IL-1Ra were found to have significant associations with the presence of postoperative cartilage wear (p < 0.05). No correlations were demonstrated among the biomarker concentrations at the time of injury with PRO scores at final follow-up (NS).
Conclusion
Synovial fluid inflammatory biomarker concentrations at the time of injury can predict progression of early-stage post-traumatic osteoarthritis at a mean of almost 8 years post-operatively. Findings from this study may help identify treatment targets to alter the natural history of cartilage loss following anterior cruciate ligament injury.
Level of evidence
Level III, retrospective cohort study.

Similar content being viewed by others
References
Ajuied A, Wong F, Smith C, Norris M, Earnshaw P, Back D et al (2014) Anterior cruciate ligament injury and radiologic progression of knee osteoarthritis: a systematic review and meta-analysis. Am J Sports Med 42:2242–2252
Appleton CT, Usmani SE, Pest MA, Pitelka V, Mort JS, Beier F (2015) Reduction in disease progression by inhibition of transforming growth factor alpha-CCL2 signaling in experimental posttraumatic osteoarthritis. Arthritis Rheum 67:2691–2701
Bodkin SG, Werner BC, Slater LV, Hart JM (2020) Post-traumatic osteoarthritis diagnosed within 5 years following ACL reconstruction. Knee Surg Sports Traumatol Arthrosc ESSKA 28:790–796
Briggs KK, Lysholm J, Tegner Y, Rodkey WG, Kocher MS, Steadman JR (2009) The reliability, validity, and responsiveness of the Lysholm score and Tegner activity scale for anterior cruciate ligament injuries of the knee: 25 years later. Am J Sports Med 37:890–897
Brophy RH, Wright RW, Matava MJ (2009) Cost analysis of converting from single-bundle to double-bundle anterior cruciate ligament reconstruction. Am J Sports Med 37:683–687
Brown TD, Johnston RC, Saltzman CL, Marsh JL, Buckwalter JA (2006) Posttraumatic osteoarthritis: a first estimate of incidence, prevalence, and burden of disease. J Orthop Trauma 20:739–744
Carlevaro MF, Cermelli S, Cancedda R, Descalzi Cancedda F (2000) Vascular endothelial growth factor (VEGF) in cartilage neovascularization and chondrocyte differentiation: auto-paracrine role during endochondral bone formation. J Cell Sci 113(Pt 1):59–69
Chou CH, Lee MT, Song IW, Lu LS, Shen HC, Lee CH et al (2015) Insights into osteoarthritis progression revealed by analyses of both knee tibiofemoral compartments. Osteoarthr Cartil 23:571–580
Clair AJ, Kingery MT, Anil U, Kenny L, Kirsch T, Strauss EJ (2019) Alterations in synovial fluid biomarker levels in knees with meniscal injury as compared with asymptomatic contralateral knees. Am J Sports Med 47:847–856
Cohen J (2013) Statistical power analysis for the behavioral sciences. Routledge, New York
Colak C, Polster JM, Obuchowski NA, Jones MH, Strnad G, Gyftopoulos S et al (2020) Comparison of clinical and semiquantitative cartilage grading systems in predicting outcomes after arthroscopic partial meniscectomy. Am J Roentgenol 215:441–447
Corrado A, Neve A, Cantatore FP (2013) Expression of vascular endothelial growth factor in normal, osteoarthritic and osteoporotic osteoblasts. Clin Exp Med 13:81–84
Cuellar VG, Cuellar JM, Golish SR, Yeomans DC, Scuderi GJ (2010) Cytokine profiling in acute anterior cruciate ligament injury. Arthroscopy 26:1296–1301
Cuellar VG, Cuellar JM, Kirsch T, Strauss EJ (2016) Correlation of synovial fluid biomarkers with cartilage pathology and associated outcomes in knee arthroscopy. Arthroscopy 32:475–485
Daniel DM, Stone ML, Dobson BE, Fithian DC, Rossman DJ, Kaufman KR (1994) Fate of the ACL-injured patient. A prospective outcome study. Am J Sports Med 22:632–644
Deshmane SL, Kremlev S, Amini S, Sawaya BE (2009) Monocyte chemoattractant protein-1 (MCP-1): an overview. J Interferon Cytokine Res 29:313–326
Ding J, Niu X, Su Y, Li X (2017) Expression of synovial fluid biomarkers in patients with knee osteoarthritis and meniscus injury. Exp Ther Med 14:1609–1613
Ellman MB, An HS, Muddasani P, Im HJ (2008) Biological impact of the fibroblast growth factor family on articular cartilage and intervertebral disc homeostasis. Gene 420:82–89
Faul F, Erdfelder E, Lang AG, Buchner A (2007) G*Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods 39:175–191
Goldring MB, Tsuchimochi K, Ijiri K (2006) The control of chondrogenesis. J Cell Biochem 97:33–44
Hamilton JL, Nagao M, Levine BR, Chen D, Olsen BR, Im H-J (2016) Targeting VEGF and its receptors for the treatment of osteoarthritis and associated pain. J Bone Miner Res 31:911–924
Hoff P, Buttgereit F, Burmester G-R, Jakstadt M, Gaber T, Andreas K et al (2013) Osteoarthritis synovial fluid activates pro-inflammatory cytokines in primary human chondrocytes. Int Orthop 37:145–151
Höher J, Münster A, Klein J, Eypasch E, Tiling T (1995) Validation and application of a subjective knee questionnaire. Knee Surg Sports Traumatol Arthrosc 3:26–33
Kaplan DJ, Cuellar VG, Jazrawi LM, Strauss EJ (2017) Biomarker changes in anterior cruciate ligament-deficient knees compared with healthy controls. Arthroscopy 33:1053–1061
Kessler MA, Behrend H, Henz S, Stutz G, Rukavina A, Kuster MS (2008) Function, osteoarthritis and activity after ACL-rupture: 11 years follow-up results of conservative versus reconstructive treatment. Knee Surg Sports Traumatol Arthrosc 16:442–448
Lohmander LS, Ostenberg A, Englund M, Roos H (2004) High prevalence of knee osteoarthritis, pain, and functional limitations in female soccer players twelve years after anterior cruciate ligament injury. Arthritis Rheum 50:3145–3152
Mabey T, Honsawek S, Saetan N, Poovorawan Y, Tanavalee A, Yuktanandana P (2014) Angiogenic cytokine expression profiles in plasma and synovial fluid of primary knee osteoarthritis. Int Orthop 38:1885–1892
Marks PH, Donaldson ML (2005) Inflammatory cytokine profiles associated with chondral damage in the anterior cruciate ligament-deficient knee. Arthroscopy 21:1342–1347
Markus DH, Berlinberg EJ, Strauss EJ (2021) Current state of synovial fluid biomarkers in sports medicine. JBJS Rev 9:12–14
Meulenbelt I (2012) Osteoarthritis year 2011 in review: genetics. Osteoarthr Cartil 20:218–222
Nagao M, Hamilton JL, Kc R, Berendsen AD, Duan X, Cheong CW et al (2017) Vascular endothelial growth factor in cartilage development and osteoarthritis. Sci Rep 7:13027
Øiestad BE, Engebretsen L, Storheim K, Risberg MA (2009) Knee osteoarthritis after anterior cruciate ligament injury: a systematic review. Am J Sports Med 37:1434–1443
Pfander D, Kortje D, Zimmermann R, Weseloh G, Kirsch T, Gesslein M et al (2001) Vascular endothelial growth factor in articular cartilage of healthy and osteoarthritic human knee joints. Ann Rheum Dis 60:1070–1073
Raghu H, Lepus CM, Wang Q, Wong HH, Lingampalli N, Oliviero F et al (2017) CCL2/CCR2, but not CCL5/CCR5, mediates monocyte recruitment, inflammation and cartilage destruction in osteoarthritis. Ann Rheum Dis 76:914–922
Ries C (2014) Cytokine functions of TIMP-1. Cell Mol Life Sci 71:659–672
Roos EM, Roos HP, Lohmander LS, Ekdahl C, Beynnon BD (1998) Knee injury and osteoarthritis outcome score (KOOS)—development of a self-administered outcome measure. J Orthop Sports Phys Ther 28:88–96
Roos H, Adalberth T, Dahlberg L, Lohmander LS (1995) Osteoarthritis of the knee after injury to the anterior cruciate ligament or meniscus: the influence of time and age. Osteoarthr Cartil 3:261–267
Rothrauff BB, Jorge A, de Sa D, Kay J, Fu FH, Musahl V (2020) Anatomic ACL reconstruction reduces risk of post-traumatic osteoarthritis: a systematic review with minimum 10-year follow-up. Knee Surg Sports Traumatol Arthrosc 28:1072–1084
Saetan N, Honsawek S, Tanavalee A, Yuktanandana P, Meknavin S, Ngarmukos S et al (2014) Relationship of plasma and synovial fluid vascular endothelial growth factor with radiographic severity in primary knee osteoarthritis. Int Orthop 38:1099–1104
Sandell LJ, Aigner T (2001) Articular cartilage and changes in arthritis. An introduction: cell biology of osteoarthritis. Arthritis Res 3:107–113
Schmal H, Mehlhorn A, Stoffel F, Kostler W, Sudkamp NP, Niemeyer P (2009) In vivo quantification of intraarticular cytokines in knees during natural and surgically induced cartilage repair. Cytotherapy 11:1065–1075
Sun JH, Yang B, Donnelly DF, Ma C, LaMotte RH (2006) MCP-1 enhances excitability of nociceptive neurons in chronically compressed dorsal root ganglia. J Neurophysiol 96:2189–2199
Svoboda SJ, Harvey TM, Owens BD, Brechue WF, Tarwater PM, Cameron KL (2013) Changes in serum biomarkers of cartilage turnover after anterior cruciate ligament injury. Am J Sports Med 41:2108–2116
Takano S, Uchida K, Inoue G, Matsumoto T, Aikawa J, Iwase D et al (2018) Vascular endothelial growth factor expression and their action in the synovial membranes of patients with painful knee osteoarthritis. BMC Musculoskelet Disord 19:204
Walsh DA, McWilliams DF, Turley MJ, Dixon MR, Franses RE, Mapp PI et al (2010) Angiogenesis and nerve growth factor at the osteochondral junction in rheumatoid arthritis and osteoarthritis. Rheumatology 49:1852–1861
White FA, Sun J, Waters SM, Ma C, Ren D, Ripsch M et al (2005) Excitatory monocyte chemoattractant protein-1 signaling is up-regulated in sensory neurons after chronic compression of the dorsal root ganglion. Proc Natl Acad Sci U S A 102:14092
Wu JJ, Lark MW, Chun LE, Eyre DR (1991) Sites of stromelysin cleavage in collagen types II, IX, X, and XI of cartilage. J Biol Chem 266:5625–5628
Xu Y-k, Ke Y, Wang B, Lin J-h (2015) The role of MCP-1-CCR2 ligand-receptor axis in chondrocyte degradation and disease progress in knee osteoarthritis. Biol Res 48:64–64
Yoshihara Y, Nakamura H, Obata K, Yamada H, Hayakawa T, Fujikawa K et al (2000) Matrix metalloproteinases and tissue inhibitors of metalloproteinases in synovial fluids from patients with rheumatoid arthritis or osteoarthritis. Ann Rheum Dis 59:455–461
Funding
Funding for this study was received from Arthroscopy Association of North America, Rosemont, IL, USA (Grant no. SOM01-15-C-39000-NYUPG-115854).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declare that they have no competing interests.
Ethical approval
IRB Protocol # 19-01449.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Markus, D.H., Hurley, E.T., Mojica, E.S. et al. Concentration of synovial fluid biomarkers on the day of anterior cruciate ligament (ACL)-reconstruction predict size and depth of cartilage lesions on 5-year follow-up. Knee Surg Sports Traumatol Arthrosc 31, 1753–1760 (2023). https://doi.org/10.1007/s00167-022-07045-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-022-07045-9