Abstract
Objective
Glycomacropeptide (GMP) is a bioactive peptide derived from milk that has been reported to exhibit a range of anti-inflammatory and immunomodulatory properties. The aim of this study was to analyze the prophylactic effect of GMP administration on airway inflammation and remodeling in an experimental model of asthmatic rat.
Methods
Animals treated orally with or without GMP (500 mg/kg/day) were ovalbumin-sensitized and -nebulized and several indicators of Th2 response, airway structural changes and inflammatory cells recruitment were evaluated.
Results
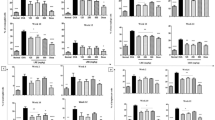
Treatment with GMP prior and during asthma development resulted in reduction of allergen-specific IgE titers in serum and blood eosinophilia. Also, GMP substantially suppressed the recruitment of inflammatory cells to bronchoalveolar compartment. Histological studies demonstrated that GMP markedly inhibits eosinophils infiltration, goblet cells hyperplasia and collagen deposit in lung tissue. The latter effect was related with an inhibition in transforming growth factor-β expression. In addition, expression of interleukin-5 and -13 were substantially inhibited in lung while that of interleukin-10 was increased.
Conclusion
Our results suggest that administration of GMP may prevent the development of an excessive Th2 response in asthma and effectively ameliorates the progression of the disease.






Similar content being viewed by others
References
Agrawal DK, Shao Z. Pathogenesis of allergic airway inflammation. Curr Allergy Asthma Rep. 2012;10:39–48.
Pelaia G, Vatrella A, Busceti MT, Gallelli L, Calabrese C, Terracciano R, Maselli R. Cellular mechanisms underlying eosinophilic and neutrophilic airway inflammation in asthma. Mediators Inflamm. 2015. doi:10.1155/2015/879783.
Broide DH. Molecular and cellular mechanisms of allergic disease. J Allergy Clin Immunol. 2001;108:S65–71.
Bergeron C, Tulic MK, Hamid Q. Airway remodelling in asthma: from benchside to clinical practice. Can Respir J. 2010;17:e85–93.
Doeing DC, Solway J. Airway smooth muscle in the pathophysiology and treatment of asthma. J Appl Physiol. 2013;114:834–43.
Oliphant CJ, Barlow JL, McKenzie AN. Insights into the initiation of type 2 immune responses. Immunology. 2011;134:378–85.
Foster PS, Hogan SP, Ramsay AJ, Matthaei KI, Young IG. Interleukin 5 deficiency abolishes eosinophilia, airways hyperreactivity, and lung damage in a mouse asthma model. J Exp Med. 1996;183:195–201.
Greenfeder S, Umland SP, Cuss FM, Chapman RW, Egan RW. Th2 cytokines and asthma. The role of interleukin-5 in allergic eosinophilic disease. Respir Res. 2001;2:71–9.
Kudo M, Ishigatsubo Y, Aoki I. Pathology of asthma. Front Microbiol. 2013. doi:10.3389/fmicb.2013.00263.
Halwani R, Al-Muhsen S, Al-Jahdali H, Hamid Q. Role of transforming growth factor-β in airway remodeling in asthma. Am J Respir Cell Mol Biol. 2011;44:127–33.
Hall S, Agrawal DK. Key mediators in the immunopathogenesis of allergic asthma. Int Immunopharmacol. 2014;23:316–29.
Chini L, Monteferrario E, Graziani S, Moschese V. Novel treatments of asthma and allergic diseases. Paediatr Respir Rev. 2014;15:355–62.
Romagnani R. T-cell subsets (Th1 versus Th2). Ann Allergy Asthma Immunol. 2000;85:9–18.
Galli SJ, Tsai M, Piliponsky AM. The development of allergic inflammation. Nature. 2008;454:445–54.
Brody EP. Biological activities of bovine glycomacropeptide. Br J Nutr. 2000;84:S39–46.
Mikkelsen TL, Rasmussen E, Olsen A, Barkholt V, Frøkiaer H. Immunogenicity of kappa-casein and glycomacropeptide. J Dairy Sci. 2006;89:824–30.
Abd El-Salam MH. Separation of casein glycomacropeptide from whey: methods of potential industrial applications. Int J Dairy Res. 2006;1:93–9.
Chen Q, Cao J, Jia Y, Liu X, Yan Y, Pang G. Modulation of mice fecal microbiota by administration of casein glycomacropeptide. Microbiol Res. 2012;3:8–12.
Daddaoua A, Puerta V, Zarzuelo A, Suárez MD, de Sánchez Medina F, Martínez-Augustin O. Bovine glycomacropeptide is anti-inflammatory in rats with hapten-induced colitis. J Nutr. 2005;135:1164–70.
Requena P, Daddaoua A, Martínez-Plata E, González M, Zarzuelo A, Suárez MD, de Sánchez Medina F, Martínez-Augustin O. Bovine glycomacropeptide ameliorates experimental rat ileitis by mechanisms involving downregulation of interleukin 17. Br J Pharmacol. 2008;154:825–32.
Requena P, González R, López-Posadas R, Abadía-Molina A, Suárez MD, Zarzuelo A. The intestinal antiinflammatory agent glycomacropeptide has immunomodulatory actions on rat splenocytes. Biochem Pharmacol. 2010;79:1797–804.
Chen QS, Wang JF, Yan YL, Pang GC. Effects of casein glycomacropeptide on dimethyl hydrazine-induced alteration of cytokine network in rats. Food Sci. 2014;35:192–8.
Monnai M, Horimoto Y, Otani H. Immunomodificatory effect of dietary bovine k-caseinoglycopeptide on serum antibody levels and proliferative responses of lymphocytes in mice. Milchwissenschaft. 1998;53:129–32.
Ye L, Chen QS, Li W, Yan YL, Zhao P, Pang GC, Hu ZH. Effect of casein glycomacropeptide on phagocytic cells and intestinal mucosa immune cells in mice. Food Sci. 2014;35:234–40.
Jiménez M, Chávez NA, Salinas E. Pretreatment with glycomacropeptide reduces allergen sensitization, alleviates immediate cutaneous hypersensitivity and protects from anaphylaxis. Clin Exp Immunol. 2012;170:18–27.
Chen YH, Wu R, Geng B, Qi YF, Wang PP, Yao WZ. Endogenous hydrogen sulfide reduces airway inflammation and remodeling in a rat model of asthma. Cytokine. 2009;45:117–23.
Galli SJ, Tsai M. IgE and mast cells in allergic disease. Nat Med. 2012;18:693–704.
Honsinger RW Jr, Silverstein D, Van Arsdel PP Jr. The eosinophil and allergy: Why? J Allergy Clin Immunol. 1972;49:142–55.
Cohn L, Elias JA, Chupp GL. Asthma: mechanisms of disease persistence and progression. Annu Rev Immunol. 2004;22:789–815.
Takanashi S, Hasegawa Y, Kanehira Y, Yamamoto K, Fujimoto K, Satoh K, Okamura K. Interleukin-10 level in sputum is reduced in bronchial asthma, COPD and in smokers. Eur Respir J. 1999;14:309–14.
Sandeep T, Roopakala MS, Silvia CR, Chandrashekara S, Rao M. Evaluation of serum immunoglobulin E levels in bronchial asthma. Lung India. 2010;27:138–40.
Lama M, Chatterjee M, Chaudhuri TK. Total serum immunoglobulin E in children with asthma. Indian J Clin Biochem. 2013;28:197–200.
Van der Pouw Kraan TC, Van der Zee JS, Boeije LC, De Groot ER, Stapel SO, Aarden LA. The role of IL-13 in IgE synthesis by allergic asthma patients. Clin Exp Immunol. 1998;111:129–35.
Scheerens H, Arron JR, Zheng Y, Putnam WS, Erickson RW, Choy DF, Harris JM, Lee J, Jarjour NN, Matthews JG. The effects of lebrikizumab in patients with mild asthma following whole lung allergen challenge. Clin Exp Allergy. 2014;44:38–46.
De Bie JJ, Henricks PA, Cruikshank WW, Hofman G, Jonker EH, Nijkamp FP, Van Oosterhout AJ. Modulation of airway hyperresponsiveness and eosinophilia by selective histamine and 5-HT receptor antagonists in a mouse model of allergic asthma. Br J Pharmacol. 1998;124:857–64.
Mayr SI, Zuberi RI, Zhang M, de Sousa-Hitzler J, Ngo K, Kuwabara Y, Yu L, Fung-Leung WP, Liu FT. IgE-dependent mast cell activation potentiates airway responses in murine asthma models. J Immunol. 2002;169:2061–8.
Venge P. The eosinophil and airway remodelling in asthma. Clin Respir J. 2010;4:15–9.
Cho JY, Miller M, Baek KJ, Han JW, Nayar J, Lee SY, McElwain K, McElwain S, Friedman S, Broide DH. Inhibition of airway remodeling in IL-5-deficient mice. J Clin Invest. 2004;113:551–60.
Al-Alawi M, Hassan T, Chotirmall SH. Transforming growth factor β and severe asthma: a perfect storm. Respir Med. 2014;108:1409–23.
Pégorier S, Wagner LA, Gleich GJ, Pretolani M. Eosinophil-derived cationic proteins activate the synthesis of remodeling factors by airway epithelial cells. J Immunol. 2006;177:4861–9.
Ciepiela O, Ostafin M, Demkow U. Neutrophils in asthma–a review. Respir Physiol Neurobiol. 2015;209:13–6.
Holgate ST, Polosa R. Treatment strategies for allergy and asthma. Nat Rev Immunol. 2008;8:218–30.
Hershey GK. IL-13 receptors and signaling pathways: an evolving web. J Allergy Clin Immunol. 2003;111:677–90.
Palomares O, Martín-Fontecha M, Lauener R, Traidl-Hoffmann C, Cavkaytar O, Akdis M, Akdis CA. Regulatory T cells and immune regulation of allergic diseases: roles of IL-10 and TGF-β. Genes Immun. 2014;15:511–20.
Pacciani V, Gregori S, Chini L, Corrente S, Chianca M, Moschese V, Rossi P, Roncarolo MG, Angelini F. Induction of anergic allergen-specific suppressor T cells using tolerogenic dendritic cells derived from children with allergies to house dust mites. J Allergy Clin Immunol. 2010;125:727–36.
Meiler F, Zumkehr J, Klunker S, Ruckert B, Akdis CA, Akdis M. In vivo switch to IL-10-secreting T regulatory cells in high dose allergen exposure. J Exp Med. 2008;205:2887–98.
van de Veen W, Stanic B, Yaman G, Wawrzyniak M, Sollner S, Akdis DG, Rückert B, Akdis CA, Akdis M. IgG4 production is confined to human IL-10-producing regulatory B cells that suppress antigen-specific immune responses. J Allergy Clin Immunol. 2013;131:1204–12.
Joetham A, Takeda K, Taube C, Miyahara N, Matsubara S, Koya T, Rha YH, Dakhama A, Gelfand EW. Naturally occurring lung CD4(+)CD25(+) T cell regulation of airway allergic responses depends on IL-10 induction of TGF-beta. J Immunol. 2007;178:1433–42.
Fueki N, Sagara H, Akimoto K, Ota M, Okada T, Sugiyama K, Fueki M, Makino S, Fukuda T. Interleukin-10 regulates transforming growth factor-beta signaling in cultured human bronchial epithelial cells. Respiration. 2007;74:454–9.
Forsythe P, Inman MD, Bienenstock J. Oral treatment with live Lactobacillus reuteri inhibits the allergic airway response in mice. Am J Respir Crit Care Med. 2007;175:561–9.
Feleszko W, Jaworska J, Rha RD, Steinhausen S, Avagyan A, Jaudszus A, Ahrens B, Groneberg DA, Wahn U, Hamelmann E. Probiotic-induced suppression of allergic sensitization and airway inflammation is associated with an increase of T regulatory-dependent mechanisms in a murine model of asthma. Clin Exp Allergy. 2007;37:498–505.
Yu J, Jang SO, Kim BJ, Song YH, Kwon J, Kang MJ, Choi WA, Jung HD, Hong SJ. The Effects of Lactobacillus rhamnosus on the Prevention of Asthma in a Murine Model. Allergy Asthma Immunol Res. 2012;2:199–205.
Chabance B, Jollés P, Izquierdo C, Mazoyer E, Francoual C, Drouet L, Fiat AM. Characterization of an antithrombotic peptide from kappa-casein in newborn plasma after milk ingestion. Br J Nutr. 1995;73:583–90.
Chabance B, Marteau P, Rambaud JC, Migliore-Samour D, Boynard M, Perrotin P, Guillet R, Jollès P, Fiat AM. Casein peptide release and passage to the blood in humans during digestion of milk or yogurt. Biochimie. 1998;80:155–65.
Acknowledgments
This work was supported by grants PIBB 14-1 and 240921 from the Autonomous University of Aguascalientes and CONACYT, respectively. Renata Roldán has a master fellowship from CONACYT. The authors wish to thanks Istvan Berczi for reviewing the paper, Berenice Barrón for excellent technical assistance and MVZ José Luis Ponce for providing the animals for the study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible Editor: John Di Battista.
Rights and permissions
About this article
Cite this article
Roldán, N.R., Jiménez, M., Cervantes-García, D. et al. Glycomacropeptide administration attenuates airway inflammation and remodeling associated to allergic asthma in rat. Inflamm. Res. 65, 273–283 (2016). https://doi.org/10.1007/s00011-015-0913-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-015-0913-y