Abstract
Critical roles of stem cell-extracellular vesicles (EVs) in the management of osteoporosis have been documented. Here, this study was designed to enlarge the research of the specific effects and underlying mechanism of urine-derived stem cells-EVs (USCs-EVs) on osteoporosis in diabetes rats. Firstly, miR-26a-5p and histone deacetylase 4 (HDAC4) expression in USCs of rats after diabetic osteoporosis (DOP) modeling induced by streptozotocin injection was determined, followed by study of their interaction. Then, USCs-EVs were co-cultured with osteogenic precursor cells, the effects of miRNA-26a-5p (miR-26a-5p) on osteoblasts, osteoclasts, bone mineralization deposition rate were evaluated. Meanwhile, the effect of USCs-EVs carrying miR-26a-5p on DOP rats was assessed. Elevated miR-26a-5p was seen in USCs-EVs which limited HDAC4 expression. Moreover, USCs-EVs delivered miR-26a-5p to osteogenic precursor cells, thereby promoting their differentiation, enhancing the activity of osteoblasts, and inhibiting the activity of osteoclasts, thereby preventing DOP through the activation of hypoxia inducible factor 1 subunit alpha (HIF-1α)/vascular endothelial growth factor A (VEGFA) pathway by repressing HDAC4. In a word, USCs-EVs-miR-26a-5p is a promising therapy for DOP by activating HIF-1α/VEGFA pathway through HDAC4 inhibition.
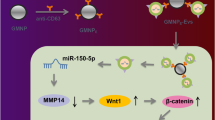
Graphical abstract
1. USCs-EVs-miR-26a-5p targeted HDAC4 and limited HDAC4 expression. 2. miR-26a-5p was delivered by USCs-EVs into osteoblast precursor cells. 3. USCs-EVs-miR-26a-5p promoted the differentiation of osteoblast precursor cells into osteoblasts. 4. miR-26a-5p delivered by USCs-EVs could inhibit HDAC4. 5. USCs-EVs-miR-26a-5p could prevent the pathogenesis of DOP via HIF-1α/VEGFA aix.










Similar content being viewed by others
Data availability
The data and materials of the study can be obtained from the corresponding author upon request.
Code availability
Not applicable.
References
Aspray TJ, Hill TR. Osteoporosis and the Ageing Skeleton. Subcell Biochem. 2019;91:453–76. https://doi.org/10.1007/978-981-13-3681-2_16.
Burdeyron P, Giraud S, Hauet T, Steichen C. Urine-derived stem/progenitor cells: A focus on their characterization and potential. World J Stem Cells. 2020;12(10):1080–96. https://doi.org/10.4252/wjsc.v12.i10.1080.
Bustin SA, Benes V, Garson JA, Hellemans J, Huggett J, Kubista M, et al. The MIQE guidelines: minimum information for publication of quantitative real-time PCR experiments. Clin Chem. 2009;55(4):611–22. https://doi.org/10.1373/clinchem.2008.112797.
Chen CY, Rao SS, Tan YJ, Luo MJ, Hu XK, Yin H, et al. Extracellular vesicles from human urine-derived stem cells prevent osteoporosis by transferring CTHRC1 and OPG. Bone Res. 2019a;7:18. https://doi.org/10.1038/s41413-019-0056-9.
Chen R, Qiu H, Tong Y, Liao F, Hu X, Qiu Y, et al. MiRNA-19a-3p alleviates the progression of osteoporosis by targeting HDAC4 to promote the osteogenic differentiation of hMSCs. Biochem Biophys Res Commun. 2019b;516(3):666–72. https://doi.org/10.1016/j.bbrc.2019.06.083.
Chen CY, Du W, Rao SS, Tan YJ, Hu XK, Luo MJ, et al. Extracellular vesicles from human urine-derived stem cells inhibit glucocorticoid-induced osteonecrosis of the femoral head by transporting and releasing pro-angiogenic DMBT1 and anti-apoptotic TIMP1. Acta Biomater. 2020;111:208–20. https://doi.org/10.1016/j.actbio.2020.05.020.
Choi C, Lee H, Lim H, Park S, Lee J, Do S. Effect of Rubus coreanus extracts on diabetic osteoporosis by simultaneous regulation of osteoblasts and osteoclasts. Menopause. 2012;19(9):1043–51. https://doi.org/10.1097/gme.0b013e31824b1cc5.
Cotts KG, Cifu AS. Treatment of Osteoporosis. JAMA. 2018;319(10):1040–1. https://doi.org/10.1001/jama.2017.21995.
DeShields SC, Cunningham TD. Comparison of osteoporosis in US adults with type 1 and type 2 diabetes mellitus. J Endocrinol Invest. 2018;41(9):1051–60. https://doi.org/10.1007/s40618-018-0828-x.
Duan YR, Chen BP, Chen F, Yang SX, Zhu CY, Ma YL, et al. Exosomal microRNA-16-5p from human urine-derived stem cells ameliorates diabetic nephropathy through protection of podocyte. J Cell Mol Med. 2019. https://doi.org/10.1111/jcmm.14558.
Ensrud KE, Crandall CJ. Osteoporosis. Ann Intern Med. 2017;167(3):ITC17–32. https://doi.org/10.7326/AITC201708010.
Faulkner B, Astleford K, Mansky KC. Regulation of Osteoclast Differentiation and Skeletal Maintenance by Histone Deacetylases. Molecules. 2019;24(7). https://doi.org/10.3390/molecules24071355.
Guan H, Peng R, Mao L, Fang F, Xu B, Chen M. Injured tubular epithelial cells activate fibroblasts to promote kidney fibrosis through miR-150-containing exosomes. Exp Cell Res. 2020;392(2): 112007. https://doi.org/10.1016/j.yexcr.2020.112007.
Ji X, Wang M, Chen F, Zhou J. Urine-Derived Stem Cells: The Present and the Future. Stem Cells Int. 2017;2017:4378947. https://doi.org/10.1155/2017/4378947.
Khosla S, Hofbauer LC. Osteoporosis treatment: recent developments and ongoing challenges. Lancet Diabetes Endocrinol. 2017;5(11):898–907. https://doi.org/10.1016/S2213-8587(17)30188-2.
Kilkenny C, Browne WJ, Cuthill IC, Emerson M, Altman DG. Improving bioscience research reporting: the ARRIVE guidelines for reporting animal research. Osteoarthritis Cartilage. 2012;20(4):256–60. https://doi.org/10.1016/j.joca.2012.02.010.
Leidig-Bruckner G, Grobholz S, Bruckner T, Scheidt-Nave C, Nawroth P, Schneider JG. Prevalence and determinants of osteoporosis in patients with type 1 and type 2 diabetes mellitus. BMC Endocr Disord. 2014;14:33. https://doi.org/10.1186/1472-6823-14-33.
Li Y, Fan L, Hu J, Zhang L, Liao L, Liu S, et al. MiR-26a Rescues Bone Regeneration Deficiency of Mesenchymal Stem Cells Derived From Osteoporotic Mice. Mol Ther. 2015;23(8):1349–57. https://doi.org/10.1038/mt.2015.101.
Li J, Li X, Liu D, Hamamura K, Wan Q, Na S, et al. eIF2alpha signaling regulates autophagy of osteoblasts and the development of osteoclasts in OVX mice. Cell Death Dis. 2019;10(12):921. https://doi.org/10.1038/s41419-019-2159-z.
Li X, Liao J, Su X, Li W, Bi Z, Wang J, et al. Human urine-derived stem cells protect against renal ischemia/reperfusion injury in a rat model via exosomal miR-146a-5p which targets IRAK1. Theranostics. 2020;10(21):9561–78. https://doi.org/10.7150/thno.42153.
Ling X, Zhang G, Xia Y, Zhu Q, Zhang J, Li Q, et al. Exosomes from human urine-derived stem cells enhanced neurogenesis via miR-26a/HDAC6 axis after ischaemic stroke. J Cell Mol Med. 2020;24(1):640–54. https://doi.org/10.1111/jcmm.14774.
Liu XD, Cai F, Liu L, Zhang Y, Yang AL. MicroRNA-210 is involved in the regulation of postmenopausal osteoporosis through promotion of VEGF expression and osteoblast differentiation. Biol Chem. 2015;396(4):339–47. https://doi.org/10.1515/hsz-2014-0268.
Liu SG, Zhang D, He Y, Gao W, Shi X. A split aptamer sensing platform for highly sensitive detection of theophylline based on dual-color fluorescence colocalization and single molecule photobleaching. Biosens Bioelectron. 2020;166: 112461. https://doi.org/10.1016/j.bios.2020.112461.
Ma H, Wang X, Zhang W, Li H, Zhao W, Sun J, et al. Melatonin Suppresses Ferroptosis Induced by High Glucose via Activation of the Nrf2/HO-1 Signaling Pathway in Type 2 Diabetic Osteoporosis. Oxid Med Cell Longev. 2020;2020:9067610. https://doi.org/10.1155/2020/9067610.
Malavika D, Shreya S, Raj Priya V, Rohini M, He Z, Partridge NC, et al. miR-873-3p targets HDAC4 to stimulate matrix metalloproteinase-13 expression upon parathyroid hormone exposure in rat osteoblasts. J Cell Physiol. 2020;235(11):7996–8009. https://doi.org/10.1002/jcp.29454.
Mohsin S, Baniyas MM, AlDarmaki RS, Tekes K, Kalasz H, Adeghate EA. An update on therapies for the treatment of diabetes-induced osteoporosis. Expert Opin Biol Ther. 2019;19(9):937–48. https://doi.org/10.1080/14712598.2019.1618266.
Muraca M, Cappariello A. The Role of Extracellular Vesicles (EVs) in the Epigenetic Regulation of Bone Metabolism and Osteoporosis. Int J Mol Sci. 2020;21(22). https://doi.org/10.3390/ijms21228682.
Ouyang B, Xie Y, Zhang C, Deng C, Lv L, Yao J, et al. Extracellular Vesicles From Human Urine-Derived Stem Cells Ameliorate Erectile Dysfunction in a Diabetic Rat Model by Delivering Proangiogenic MicroRNA. Sex Med. 2019;7(2):241–50. https://doi.org/10.1016/j.esxm.2019.02.001.
Quinlan E, Partap S, Azevedo MM, Jell G, Stevens MM, O’Brien FJ. Hypoxia-mimicking bioactive glass/collagen glycosaminoglycan composite scaffolds to enhance angiogenesis and bone repair. Biomaterials. 2015;52:358–66. https://doi.org/10.1016/j.biomaterials.2015.02.006.
Schoepflin ZR, Shapiro IM, Risbud MV. Class I and IIa HDACs Mediate HIF-1alpha Stability Through PHD2-Dependent Mechanism, While HDAC6, a Class IIb Member, Promotes HIF-1alpha Transcriptional Activity in Nucleus Pulposus Cells of the Intervertebral Disc. J Bone Miner Res. 2016;31(6):1287–99. https://doi.org/10.1002/jbmr.2787.
Trompeter HI, Dreesen J, Hermann E, Iwaniuk KM, Hafner M, Renwick N, et al. MicroRNAs miR-26a, miR-26b, and miR-29b accelerate osteogenic differentiation of unrestricted somatic stem cells from human cord blood. BMC Genomics. 2013;14:111. https://doi.org/10.1186/1471-2164-14-111.
Wang CG, Hu YH, Su SL, Zhong D. LncRNA DANCR and miR-320a suppressed osteogenic differentiation in osteoporosis by directly inhibiting the Wnt/beta-catenin signaling pathway. Exp Mol Med. 2020a;52(8):1310–25. https://doi.org/10.1038/s12276-020-0475-0.
Wang Y, Yao J, Cai L, Liu T, Wang X, Zhang Y, et al. Bone-Targeted Extracellular Vesicles from Mesenchymal Stem Cells for Osteoporosis Therapy. Int J Nanomedicine. 2020b;15:7967–77. https://doi.org/10.2147/IJN.S263756.
Wang JS, Yoon SH, Wein MN. Role of histone deacetylases in bone development and skeletal disorders. Bone. 2021;143:115606. https://doi.org/10.1016/j.bone.2020.115606.
Wei H, Cao C, Wei X, Meng M, Wu B, Meng L, et al. Circular RNA circVEGFC accelerates high glucose-induced vascular endothelial cells apoptosis through miR-338–3p/HIF-1alpha/VEGFA axis. Aging (Albany NY). 2020;12(14):14365–75. https://doi.org/10.18632/aging.103478.
Xu D, Gao Y, Hu N, Wu L, Chen Q. miR-365 Ameliorates Dexamethasone-Induced Suppression of Osteogenesis in MC3T3-E1 Cells by Targeting HDAC4. Int J Mol Sci. 2017;18(5). https://doi.org/10.3390/ijms18050977.
Yu L, Xie M, Zhang F, Wan C, Yao X. TM9SF4 is a novel regulator in lineage commitment of bone marrow mesenchymal stem cells to either osteoblasts or adipocytes. Stem Cell Res Ther. 2021;12(1):573. https://doi.org/10.1186/s13287-021-02636-8.
Zhang J, Chen C, Hu B, Niu X, Liu X, Zhang G, et al. Exosomes Derived from Human Endothelial Progenitor Cells Accelerate Cutaneous Wound Healing by Promoting Angiogenesis Through Erk1/2 Signaling. Int J Biol Sci. 2016;12(12):1472–87. https://doi.org/10.7150/ijbs.15514.
Zhang Y, Ren YJ, Guo LC, Ji C, Hu J, Zhang HH, et al. Nucleus accumbens-associated protein-1 promotes glycolysis and survival of hypoxic tumor cells via the HDAC4-HIF-1alpha axis. Oncogene. 2017;36(29):4171–81. https://doi.org/10.1038/onc.2017.51.
Zhong F, Geng G, Chen B, Pan T, Li Q, Zhang H, et al. Identification of benzenesulfonamide quinoline derivatives as potent HIV-1 replication inhibitors targeting Rev protein. Org Biomol Chem. 2015;13(6):1792–9. https://doi.org/10.1039/c4ob02247e.
Zhou T, Benda C, Duzinger S, Huang Y, Li X, Li Y, et al. Generation of induced pluripotent stem cells from urine. J Am Soc Nephrol. 2011;22(7):1221–8. https://doi.org/10.1681/ASN.2011010106.
Author information
Authors and Affiliations
Contributions
Dan Zhang conceived and together with Linna Suo designed the study. Dan Zhang, Min Yu, and Linna Suo were involved in data collection. Dan Zhang and Jian Du performed the statistical analysis and preparation of Figs. Dan Zhang and Linna Suo drafted the paper. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was implemented under the ratification of the Research Ethics Committee of The Fourth Affiliated Hospital of China Medical University (approval number: EC-2019-KS-072(YJ)). We tried our best to limit animals’ pain. Informed consent form was signed prior to participation by all participants.
Consent to participate
All participants signed informed consent documentation.
Consent for publication
Not Applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhang, D., Du, J., Yu, M. et al. Urine-derived stem cells-extracellular vesicles ameliorate diabetic osteoporosis through HDAC4/HIF-1α/VEGFA axis by delivering microRNA-26a-5p. Cell Biol Toxicol 39, 2243–2257 (2023). https://doi.org/10.1007/s10565-022-09713-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10565-022-09713-5