Abstract
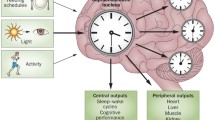
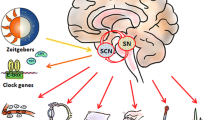
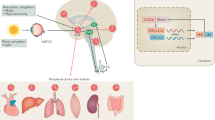
Ambient light is a crucial environmental factor that influences physiology and behavior in all organisms including human beings. A fair understanding of the importance of circadian rhythms and timekeeping would enable us to develop strategies for the management of disrupted circadian rhythm-associated disorders such as depression, Alzheimer’s, and Parkinson’s diseases. Circadian manipulation protocols such as bright light exposure, acute sleep deprivation and photoperiod manipulation have been reported to be beneficial in humans and animal models. This chapter briefly summarizes the current knowledge on the efficacious role of circadian rhythm manipulation strategies in facilitating behavioral recovery and the possible underlying mechanisms. We have also tried to highlight the limitations and implications of futuristic combinatorial circadian rhythm manipulation and pharmacological approaches in the management of chronodisruption-related disorders.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Alessi CA, Martin JL, Webber AP, Kim EC, Harker JO, Josephson KR (2005) Randomized, controlled trial of a nonpharmacological intervention to improve abnormal sleep/wake patterns in nursing home residents. J Am Geriatr Soc 53(5):803–810. https://doi.org/10.1111/j.1532-5415.2005.53251.x
Ancoli-Israel S, Gehrman P, Martin JL, Shochat T, Marler M, Corey-Bloom J, Levi L (2003) Increased light exposure consolidates sleep and strengthens circadian rhythms in severe Alzheimer’s disease patients. Behav Sleep Med 1(1):22–36. https://doi.org/10.1207/S15402010BSM0101_4
Andrews RV, Belknap RW (1993) Seasonal acclimation of prairie deer mice. Int J Biometeorol 37(4):190–193. https://doi.org/10.1007/BF01387521
Archer ZA, Findlay PA, Rhind SM, Mercer JG, Adam CL (2002) Orexin gene expression and regulation by photoperiod in the sheep hypothalamus. Regul Pept 104(1–3):41–45. https://doi.org/10.1016/S0167-0115(01)00347-0
Ashkenazy T, Einat H, Kronfeld-schor N (2009a) Effects of bright light treatment on depression- and anxiety-like behaviors of diurnal rodents maintained on a short daylight schedule. Behav Brain Res 201:343–346. https://doi.org/10.1016/j.bbr.2009.03.005
Ashkenazy T, Einat H, Kronfeld-Schor N (2009b) We are in the dark here: induction of depression- and anxiety-like behaviours in the diurnal fat sand rat, by short daylight or melatonin injections. Int J Neuropsychopharmacol 12(01):83–93. https://doi.org/10.1017/S1461145708009115
Avery DH, Khan A, Dager SR, Cox GB, Dunner DL (1990) Bright light treatment of winter depression: morning versus evening light. Acta Psychiatr Scand 82(5):335–338. https://doi.org/10.1111/j.1600-0447.1990.tb01397.x
Beecher ME, Eggett D, Erekson D, Rees LB, Bingham J, Klundt J, Bailey RJ, Ripplinger C, Kirchhoefer J, Gibson R, Griner D, Cox JC, Boardman RD (2016) Sunshine on my shoulders: weather, pollution, and emotional distress. J Affect Disord 205:234–238. https://doi.org/10.1016/j.jad.2016.07.021
Beery AK, Loo TJ, Zucker I (2008) Day length and estradiol affect same-sex affiliative behavior in the female meadow vole. Horm Behav 54(1):153–159. https://doi.org/10.1016/j.yhbeh.2008.02.007
Benedetti F, Colombo C, Barbini B, Campori E, Smeraldi E (2001) Morning sunlight reduces length of hospitalization in bipolar depression. J Affect Disord 62(3):221–223. https://doi.org/10.1016/S0165-0327(00)00149-X
Benedetti F, Barbini B, Fulgosi MC, Colombo C, Dallaspezia S, Pontiggia A, Smeraldi E (2005) Combined total sleep deprivation and light therapy in the treatment of drug-resistant bipolar depression: acute response and long-term remission rates. J Clin Psychiatry 66(12):1535–1540. https://doi.org/10.4088/jcp.v66n1207
Bilu C, Einat H, Zimmet P, Vishnevskia-Dai V, Schwartz WJ, Kronfeld-Schor N (2022) Beneficial effects of voluntary wheel running on activity rhythms, metabolic state, and affect in a diurnal model of circadian disruption. Scientific reports. Nature Publishing Group, UK, vol 12(1), pp 1–12. https://doi.org/10.1038/s41598-022-06408-z
Bowrey HE, James MH, Aston-Jones G (2017) New directions for the treatment of depression: targeting the photic regulation of arousal and mood (PRAM) pathway. Depress Anxiety 34(7):588–595. https://doi.org/10.1002/da.22635
Campbell PD, Miller AM, Woesner ME (2017) Bright light therapy: seasonal affective disorder and beyond. Einstein J Biol Med : EJBM 32:E13–E25. Available at: http://www.ncbi.nlm.nih.gov/pubmed/31528147
Challet E (2007) Minireview: entrainment of the suprachiasmatic clockwork in diurnal and nocturnal mammals. Endocrinology 148(12):5648–5655. https://doi.org/10.1210/en.2007-0804
Cuesta M, Aungier J, Morton AJ (2014) Behavioral therapy reverses circadian deficits in a transgenic mouse model of Huntington’s disease. Neurobiol Dis 63:85–91. https://doi.org/10.1016/j.nbd.2013.11.008
Daan S, Aschoff J (2001) The entrainment of circadian systems. In: Takahashi JS, Turek FW, Moore RY (eds) Handbook of behavioral neurobiology, pp 7–43. https://doi.org/10.1007/978-1-4615-1201-1_2
Dallaspezia S, Benedetti F (2015) Sleep deprivation therapy for depression. In: Current topics in behavioral neurosciences, vol 25(November 2011), pp 483–502. https://doi.org/10.1007/7854_2014_363
Dowling GA, Mastick J, Hubbard EM, Luxenberg JS, Burr RL (2005) Effect of timed bright light treatment for rest-activity disruption in institutionalized patients with Alzheimer’s disease. Int J Geriatr Psychiatry 20(8):738–43. https://doi.org/10.1002/gps.1352
Dulcis D, Jamshidi P, Leutgeb S, Spitzer NC (2013) Neurotransmitter switching in the adult brain regulates behavior. Science 340(April):449–453
Evans JA, Leise TL, Castanon-Cervantes O, Davidson AJ (2013) Dynamic interactions mediated by nonredundant signaling mechanisms couple circadian clock neurons. Neuron 80(4):973–983. https://doi.org/10.1016/j.neuron.2013.08.022
Farajnia S, Meijer JH, Michel S (2015) Age-related changes in large-conductance calcium-activated potassium channels in mammalian circadian clock neurons. Neurobiol Aging 36(6):2176–2183. https://doi.org/10.1016/j.neurobiolaging.2014.12.040
Ferris CF (2005) Vasopressin/oxytocin and aggression. In: Novartis foundation symposium. Novartis Foundation, pp 190–198. https://doi.org/10.1002/0470010703.ch13
Fetveit A, Skjerve A, Bjorvatn B (2003) Bright light treatment improves sleep in institutionalised elderly—an open trial. Int J Geriatr Psychiatry 18(6):520–526. https://doi.org/10.1002/gps.852
Fu Y, Zhong H, Wang MH, Luo D, Liao H, Maeda H, Hattar S, Frishman LJ, Yau K (2005) Intrinsically photosensitive retinal ganglion cells detect light with a vitamin A-based photopigment, melanopsin. Proc Natl Acad Sci USA 102(29):10339–10344. https://doi.org/10.1073/pnas.0501866102
Fuchs E, Simon M, Schmelting B (2006) Pharmacology of a new antidepressant: benefit of the implication of the melatonergic system. Int Clin Psychopharmacol 21(SUPPL.1):17–20. https://doi.org/10.1097/01.yic.0000199456.39552.c7
Giedke H, Schwärzler F (2002) Therapeutic use of sleep deprivation in depression. Sleep Med Rev 6(5):361–377. https://doi.org/10.1053/smrv.2002.0235
Golden RN, Gaynes BN, Ekstrom RD, Hamer RM, Jacobsen FM, Suppes T, Wisner KL, Nemeroff CB (2005) The efficacy of light therapy in the treatment of mood disorders: a review and meta-analysis of the evidence. Am J Psychiatry 162(April):656–662
GomesJI, Miguel Farinha-Ferreira M, Rei N, Gonçalves-Ribeiro J, Ribeiro JA, Sebastiã AM, Vaz SH (2021) Of adenosine and the blues: the adenosinergic system in the pathophysiology and treatment of major depressive disorder. Pharmacol Res163. https://doi.org/10.1016/j.phrs.2020.105363
Gorgulu Y, Caliyurt O (2009) Rapid antidepressant effects of sleep deprivation therapy correlates with serum BDNF changes in major depression. Brain Res Bull 80(3):158–162. https://doi.org/10.1016/j.brainresbull.2009.06.016
Hale A, Corral R-M, Mencacci C, Saiz Ruiz J, Severo CA, Gentil V (2010) Superior antidepressant efficacy results of agomelatine versus fluoxetine in severe MDD patients: a randomized, double-blind study. Int Clin Psychopharmacol 25(6):305–314. https://doi.org/10.1097/YIC.0b013e32833a86aa
Hastings MH, Reddy AB, Maywood ES (2003) A clockwork web: circadian timing in brain and periphery, in health and disease. Nat Rev Neurosci 4(8):649–661. https://doi.org/10.1038/nrn1177
Hines DJ, Schmitt LI, Hines RM, Moss SJ, Haydon PG (2013) Antidepressant effects of sleep deprivation require astrocyte- dependent adenosine mediated signaling. Trans Psychiatry 3(August 2012). https://doi.org/10.1038/tp.2012.136
Huang LY, Devries GJ, Bittman EL (1998) Bromodeoxyuridine labeling in the brain of a seasonally breeding mammal. J Neurobiol 36:410–420
Hurley SW, Johnson AK (2014) The role of the lateral hypothalamus and orexin in ingestive behavior: a model for the translation of past experience and sensed deficits into motivated behaviors. Front Syst Neurosci 8(November):1–10. https://doi.org/10.3389/fnsys.2014.00216
Johnstone DM, Moro C, Stone J, Benabid AL, Mitrofanis J (2016) Turning on lights to stop neurodegeneration: the potential of near infrared light therapy in Alzheimer’s and Parkinson’s Disease. Front Neurosci 9:1–15. https://doi.org/10.3389/fnins.2015.00500
Kapgal V, Prem N, Hegde P, Laxmi TR, Kutty BM (2016) Long term exposure to combination paradigm of environmental enrichment, physical exercise and diet reverses the spatial memory deficits and restores hippocampal neurogenesis in ventral subicular lesioned rats. Neurobiol Learn Memory 130:61–70. https://doi.org/10.1016/j.nlm.2016.01.013
Kent ST, McClure LA, Crosson WL, Arnett DK, Wadley VG, Sathiakumar N (2009) Effect of sunlight exposure on cognitive function among depressed and non-depressed participants: a REGARDS cross-sectional study. Environ Health: Glob Access Sci Source 8(1). https://doi.org/10.1186/1476-069X-8-34
Kumar U (2007) Colocalization of somatostatin receptor subtypes (SSTR1–5) with somatostatin, NADPH-diaphorase (NADPH-d), and tyrosine hydroxylase in the rat hypothalamus. J Comp Neurol 504(2):185–205. https://doi.org/10.1002/cne.21444
Lee HJ, Macbeth AH, Pagani J, Young WS (2009) Oxytocin: the great facilitator of life. Prog Neurobiol 88(2):127–151. https://doi.org/10.1016/j.pneurobio.2009.04.001
Lee Y, Field JM, Sehgal A (2021) Circadian rhythms, disease and chronotherapy. J Biol Rhythms 36(6):503–531. https://doi.org/10.1177/07487304211044301
LeGates TA, Fernandez DC, Hattar S (2014) Light as a central modulator of circadian rhythms, sleep and affect. Nat Rev Neurosci 15(7):443–54. https://doi.org/10.1038/nrn3743
Lemoine P, Guilleminault C, Alvarez E (2007) Improvement in subjective sleep in major depressive disorder with a novel antidepressant, agomelatine: randomized, double- blind comparison with venlafaxine. J Clin Psychiatry 68(11):1723–1732. https://doi.org/10.4088/jcp.v68n1112
Liu RJ, Van Den Pol AN, Aghajanian GK (2002) Hypocretins (orexins) regulate serotonin neurons in the dorsal raphe nucleus by excitatory direct and inhibitory indirect actions. J Neurosci 22(21):9453–9464. https://doi.org/10.1523/jneurosci.22-21-09453.2002
Lopez-Rodriguez F, Wilson CL, Maidment NT, Poland RE, Engel J (2003) Total sleep deprivation increases extracellular serotonin in the rat hippocampus. Neuroscience 121(2):523–530. https://doi.org/10.1016/S0306-4522(03)00335-X
Lopez-Rodriguez F, Kim J, Poland RE (2004) Total sleep deprivation decreases immobility in the forced-swim test. Neuropsychopharmacology 29(6):1105–1111. https://doi.org/10.1038/sj.npp.1300406
Loving RT, Kripke DF, Elliott JA, Knickerbocker NC, Grandner MA (2005) Bright light treatment of depression for older adults. BMC Psychiatry 5(1):1–14. https://doi.org/10.1186/1471-244x-5-41
Lyketsos CG, Lindell VL, Baker A, Steele C (1999) A randomized, controlled trial of bright light therapy for agitated behaviors in dementia patients residing in long-term care. Int J Geriatr Psychiatry 14(7):520–525. https://doi.org/10.1002/(SICI)1099-1166(199907)14:7%3c520:AID-GPS983%3e3.0.CO;2-M
Ouk K, Aungier J, Morton AJ (2017) Prolonged day length exposure improves circadian deficits and survival in a transgenic mouse model of Huntington’s disease. Neurobiol Sleep Circadian Rhythm 2:27–38. https://doi.org/10.1016/j.nbscr.2016.11.004
Paus S, Schmitz-Hübsch T, Wüllner U, Vogel A, Klockgether T, Abele M (2007) Bright light therapy in Parkinson’s disease: a pilot study. Movement Disorders 22(10):1495–1498. https://doi.org/10.1002/mds.21542
Perrin F, Peigneux P, Fuchs S, Verhaeghe S, Laureys S, Middleton B, Degueldre C, Del Fiore G, Vandewalle G, Balteau E, Poirrier R, Moreau V, Luxen A, Maquet P, Dijk D-J (2004) Nonvisual responses to light exposure in the human brain during the circadian night. Curr Biol 14(20):1842–1846. https://doi.org/10.1016/j.cub.2004.09.082
Pritchard R, Chen H, Romoli B, Spitzer NC, Dulcis D (2020) Photoperiod-induced neurotransmitter plasticity declines with aging: an epigenetic regulation? J Comp Neurol 528(2):199–210. https://doi.org/10.1002/cne.24747
Rainer Q, Xia L, Guilloux JP, Gabriel C, Mocaër E, Hen R, Enhamre E, Gardier AM, David DJ (2012) Beneficial behavioural and neurogenic effects of agomelatine in a model of depression/anxiety. Int J Neuropsychopharmacol 15(3):321–335. https://doi.org/10.1017/S1461145711000356
Salgado-Delgado R, Tapia Osorio A, Saderi N, Escobar C (2011) Disruption of circadian rhythms: a crucial factor in the etiology of depression. Depression Res Treatment 1–9. https://doi.org/10.1155/2011/839743
Sasaki N, Gusain P, Hayano M, Sugaya T, Tonegawa N, Hatanaka Y, Tamura R, Okuyama K, Osada H, Ban N, Mitsukura Y, Lang RA, Mimura M, Tsubota K (2021) Violet light modulates the central nervous system to regulate memory and mood. bioRxiv. https://doi.org/10.1101/2021.11.02.466604
Scammell TE (2015) Narcolepsy. In: Campion EW (ed). N Eng J Med 373(27):2654–2662. https://doi.org/10.1056/NEJMra1500587
Sharma R, Sahota P, Thakkar MM (2018) Melatonin promotes sleep in mice byinhibiting orexin neurons in the perifornical lateral hypothalamus. J Pineal Res 65(2):0–1. https://doi.org/10.1111/jpi.12498
Sinclair RC, Mark MM, Clore GL (1994) Mood-related persuasion depends on (mis)attributions. Soc Cogn 12(4):309–326. https://doi.org/10.1521/soco.1994.12.4.309
Sloane PD, Williams CS, Mitchell CM, Preisser JS, Wood W, Barrick AL, Hickman SE, Gill KS, Connell BR, Edinger J, Zimmerman S (2007) High-intensity environmental light in dementia: effect on sleep and activity. J Am Geriatr Soc 55(10):1524–1533. https://doi.org/10.1111/j.1532-5415.2007.01358.x
Subhadeep D, Srikumar BN, Shankaranarayana Rao BS, Kutty BM (2017) Exposure to short photoperiod regime reduces ventral subicular lesion-induced anxiety-like behavior in Wistar rats. Physiol Behav 170:124–132. https://doi.org/10.1016/j.physbeh.2016.11.040
Subhadeep D, Srikumar BN, Shankaranarayana Rao BS, Kutty BM (2020) Short photoperiod restores ventral subicular lesion-induced deficits in affective and socio-cognitive behavior in male Wistar rats. J Neurosci Res 98(6):1114–1136. https://doi.org/10.1002/jnr.24601
Subhadeep D, Srikumar BN, Shankaranarayana Rao BS, Kutty BM (2021) Exposure to short photoperiod regime restores spatial cognition in ventral subicular lesioned rats: potential role of hippocampal plasticity, glucocorticoid receptors, and neurogenesis. Mole Neurobiol 58(9):4437–4459. https://doi.org/10.1007/s12035-021-02409-7
Tal-Krivisky K, Kronfeld-Schor N, Einat H (2015) Voluntary exercise enhances activity rhythms and ameliorates anxiety- and depression-like behaviors in the sand rat model of circadian rhythm-related mood changes. Physiol Behav 151(April 2016):441–447. https://doi.org/10.1016/j.physbeh.2015.08.002
Terman M, Terman JS (2005) Light therapy for seasonal and nonseasonal depression: efficacy, protocol, safety, and side effects. CNS Spectrums 10(8):647–663; quiz 672. https://doi.org/10.1017/S1092852900019611
Tsujino N, Sakurai T (2009) Orexin/hypocretin: a neuropeptide at the interface of sleep, energy homeostasis, and reward system. Pharmacol Rev 61(2):162–176. https://doi.org/10.1124/pr.109.001321
Tuma J, Strubbe JH, Mocaër E, Koolhaas JM (2005) Anxiolytic-like action of the antidepressant agomelatine (S 20098) after a social defeat requires the integrity of the SCN. Eur Neuropsychopharmacol 15(5):545–555. https://doi.org/10.1016/j.euroneuro.2005.02.004
Vandewalle G, Balteau E, Phillips C, Degueldre C, Moreau V, Sterpenich V, Albouy G, Darsaud A, Desseilles M, Dang-Vu TT, Peigneux P, Luxen A, Dijk DJ, Maquet P (2006) Daytime light exposure dynamically enhances brain responses. Curr Biol 16(16):1616–1621. https://doi.org/10.1016/j.cub.2006.06.031
Voderholzer U, Fiebich BL, Dersch R, Feige B, Piosczyk H, Kopasz M, Riemann D, Lieb K (2012) Effects of sleep deprivation on nocturnal cytokine concentrations in depressed patients and healthy control subjects. J Neuropsychiatry Clin Neurosci 24(3):354–366. https://doi.org/10.1176/appi.neuropsych.11060142
Walton JC, Pyter LM, Weil ZM, Nelson RJ (2012a) Photoperiod mediated changes in olfactory bulb neurogenesis and olfactory behavior in male white-footed mice (Peromyscus leucopus). PLoS ONE 7(8). https://doi.org/10.1371/journal.pone.0042743
Walton JC, Haim A, Spieldenner JM, Nelson RJ (2012b) Photoperiod alters fear responses and basolateral amygdala neuronal spine density in white-footed mice (Peromyscus leucopus). Behav Brain Res 233(2):345–350. https://doi.org/10.1016/j.bbr.2012.05.033
Walton JC, Aubrecht TG, Weil ZM, Leuner B, Nelson RJ (2014) Photoperiodic regulation of hippocampal neurogenesis in adult male white-footed mice (Peromyscus leucopus). Eur J Neurosci 40(4):2674–2679. https://doi.org/10.1111/ejn.12626
Wang HB, Whittaker DS, Truong D, Mulji AK, Ghiani CA, Loh DH, Colwell CS (2017) Blue light therapy improves circadian dysfunction as well as motor symptoms in two mouse models of Huntington’s disease. Neurobiol Sleep Circadian Rhythm 2:39–52. https://doi.org/10.1016/j.nbscr.2016.12.002
Willis GL, Turner EJD (2007) Primary and secondary features of Parkinson’s disease improve with strategic exposure to bright light: a case series study. Chronobiol Int 24(3):521–537. https://doi.org/10.1080/07420520701420717
Yamadera H, Ito T, Suzuki H, Asayama K, Ito R, Endo S (2000) Effects of bright light on cognitive and sleep-wake (circadian) rhythm disturbances in Alzheimer-type dementia. Psychiatry Clin Neurosci 54(3):352–353. https://doi.org/10.1046/j.1440-1819.2000.00711.x
Yan L, Smale L, Nunez AA (2018) Circadian and photic modulation of daily rhythms in diurnal mammals. Eur J Neurosci 51(1):551–566. https://doi.org/10.1111/ejn.14172
Yan L, Lonstein JS, Nunez AA (2019) Light as a modulator of emotion and cognition: lessons learned from studying a diurnal rodent. Hormones Behav 111:78–86. https://doi.org/10.1016/j.yhbeh.2018.09.003
Young JW, Cope ZA, Romoli B, Schrurs E, Aniek J, van Enkhuizen J, Sharp RF, Dulcis D (2018) Mice with reduced DAT levels recreate seasonal-induced switching between states in bipolar disorder. Neuropsychopharmacology 43:1721–1731. https://doi.org/10.1038/s41386-018-0031-y
Zhu H, Wang N, Yao L, Chen Q, Zhang R, Qian J, Hou Y, Guo W, Fan S, Liu S, Zhao Q, Du F, Zuo X, Guo Y, Xu Y, Li J, Xue T, Zhong K, Song X, Huang G, Xiong W (2018) Moderate UV exposure enhances learning and memory by promoting a novel glutamate biosynthetic pathway in the brain. Cell 173(7):1716-1727.e17. https://doi.org/10.1016/j.cell.2018.04.014
Acknowledgments
The study was funded by Science and Engineering Research Board (SERB), New Delhi (EMR/2017/001237).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Ethics declarations
All experimental protocols were approved by the Institute Animal Ethics Committee (AEC/66/403/N.P.) following the guidelines of the Committee for the Purpose of Control and Supervision of Experiments on Animals (CPCSEA), Government of India, at the National Institute of Mental Health and Neuro Sciences (NIMHANS), Bengaluru.
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Subhadeep, D., Srikumar, B.N., Shankaranarayana Rao, B.S., Kutty, B.M. (2023). Circadian Rhythm Manipulations: Implications on Behavioral Restoration in Central Nervous System Insults. In: Jagota, A. (eds) Sleep and Clocks in Aging and Longevity. Healthy Ageing and Longevity, vol 18. Springer, Cham. https://doi.org/10.1007/978-3-031-22468-3_16
Download citation
DOI: https://doi.org/10.1007/978-3-031-22468-3_16
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-22467-6
Online ISBN: 978-3-031-22468-3
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)