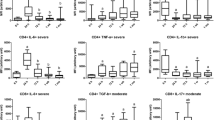
Abstract
Inflammatory mediators produced in response to hypoxic-ischemic (H-I) injury and infection in the newborn, include multi-potent cytokines and chemokines released by a variety of somatic and bone marrow-derived cells both locally, in the brain and systemically, in the circulation. Pro-inflammatory cytokines, such as interleukin (IL)-1, IL-6, IL-18, interferon (IFN)-γ and tumor necrosis factor (TNF)-α, are small polypeptides secreted in response to cellular injury and inflammation. Cytokines trigger somatic and immune cell activation, differentiation and death after signaling through their cognate receptors. Chemokines, such as CCL2 and CXCL8, are chemotactic cytokines that induce cells of the innate and adaptive immune system to leave the blood stream and migrate to sites of injury in the central nervous system (CNS) and in the periphery [1]. Cytokines and chemokines are considered critical mediators of brain damage and clinical indicators of overwhelming sepsis in the newborns. We review the cellular origin and role of cytokines and chemokines in these diseases. We also discuss treatment modalities that may interrupt these inflammatory cascades. A better understanding of the role of cytokines and chemokines in response to H-I injury and infection is likely to improve the outcome and long-term prognosis of these diseases in the newborn period.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Glass HC, Bonifacio SL, Chau V et al (2008). Recurrent postnatal infections are associated with progressive white matter injury in premature infants. Pediatrics 122: 299–305
Hagberg H, Mallard C (2005) Effect of inflammation on central nervous system development and vulnerability. Curr Opin Neurol 18: 117–123
Xanthou M (2006) Proinflammatory cytokines and chemokines in neonatal brain damage. Curr Ped Rev 2: 3–15
Diaz-Alvarez A, Hilario E, de Cerio FG et al (2007) Hypoxic-Ischemic injury in the immature brain-key vascular and cellular players. Neonatology 92: 227–235
Laing, KJ, Secombes CJ (2004). Chemokines. Dev Comp Immunol 28: 443–460
Dammann O, O’Shea MT (2008) Cytokines and perinatal brain damage. In: Spitzer AR, White RD (eds) Neuroprotection in the newborn. Elsevier Saunders, Philadelphia, pp 643–663
Vanucci RC, Perlman JM (1997) Interventions for perinatal hypoxic-ischemic encephalopathy. Pediatrics 100: 1004–1014
Okazaki K, Nishida A, Kato M et al (2006) Elevation of cytokine concentrations in asphyxiated neonates. Biol Neonate 89: 183–189
Florio P, Perrone S, Luisi S et al (2003) Activin-A plasma levels at birth: an index of fetal hypoxia in preterm newborn. Pediatr Res 54: 696–700
Petrakou E, Mouchtouri A, Levi A et al (2007) Interleukin-8 and monocyte chemotactic protein-1 mRNA expression in perinatally infected and asphyxiated preterm neonates. Neonatology 91: 107–113
Adams-Chapman I, Stoll BJ (2006) Neonatal infection and longterm neurodevelopmental outcome in the preterm infant. Curr Opin Infect Dis 19: 290–297
Levy O (2007) Innate Immunity of the newborn: basic mechanisms and clinical correlates. Nat Rev Immunol 7: 379–389
Medzhitov R (2007) Recognition of microorganisms and activation of the immune response. Nature 18: 819–826
Maxwell NC, Davies PL, Kotecha S (2006) Antenatal infection and inflammation: what’s new? Curr Opin Infect Dis 19: 253–258
Dammann O, Leviton A (1997) Maternal intrauterine infection, cytokines, and brain damage in the preterm newborn. Pediatr Res 42: 1–8
Ganz T (2004) Antimicrobial polypeptides. J Leukoc Biol 75: 34–38
Ouellette AJ (2006). Paneth cell alpha-defensin synthesis and function. Curr Top Microbiol Immunol 306: 1–25
Ayabe T, Satchell D, Wilson CL et al (2000). Secretion of microbicidal alpha-defensins by intestinal Paneth cells in response to bacteria. Nat Immunol 1: 113–118
Salzman NH, Polin RA, Harris MC et al (1998) Enteric defensin expression in necrotizing enterocolitis. Pediatr Res 44: 20–26
Haeney M (1994) Infection determinants at extremes of age. J Antimicrob Chemother 34: 1–9
Adkins B (1999) T-cell function in newborn mice and humans. Immunol Today 20: 330–335
Mayer L (2003) Mucosal immunity. Pediatrics 111: 1595–1600
Arnon S, Litmanovitz I (2008) Diagnostic tests in neonatal sepsis. Curr Opin Infect Dis 21: 223–227
Yerkovich J, Wikstrom ME, Suriyaarachchi D et al (2007) Postnatal development of monocyte cytokine response to bacterial lipopolysaccharide. Ped Res 62: 547–552
Tatad AMF, Nesin M, Peoples J et al (2008) Cytokine Expression in Response to Bacterial Antigens in Preterm and Term Infant Cord Blood Monocytes. Neonatology 94: 8–15
Zhao J, Kim KD, Yang X et al (2008) Hyper-innate responses in neonates lead to increased morbidity and mortality after infection. PNAS USA 21: 7528–7533
Levy E, Xanthou G, Petrakou E et al (2009) Distinct roles of TLR4 and CD14 in LPS-induced inflammatory responses of neonates. Pediatr Res 66: 179–184
Ramaswamy, V, Horton J, Vandermeer B et al (2009) Systematic review of biomarkers of brain injury in term neonatal encephalopathy. Pediatr Neurol 40: 215–226
Feldman M, Maini RN (2001) Anti-TNF alpha therapy of rheumatoid arthritis: what have we learned? Annu Rev Immunol 19: 163–196
Schnitzler F, Fidder H, Ferrante M et al (2009). Long-term outcome of treatment with infliximab in 614 patients with Crohn’s disease: results from a single centre cohort. Gut 58: 492–500
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2012 Springer-Verlag Italia
About this chapter
Cite this chapter
Xanthou, M., Niklas, V. (2012). Inflammatory Mediators in Neonatal Asphyxia and Infection. In: Buonocore, G., Bracci, R., Weindling, M. (eds) Neonatology. Springer, Milano. https://doi.org/10.1007/978-88-470-1405-3_110
Download citation
DOI: https://doi.org/10.1007/978-88-470-1405-3_110
Publisher Name: Springer, Milano
Print ISBN: 978-88-470-1404-6
Online ISBN: 978-88-470-1405-3
eBook Packages: MedicineMedicine (R0)