Abstract
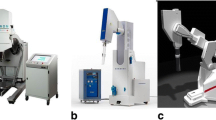
Mobile radiotherapy systems offer a versatility desirable for certain cancer treatments where the patient requires some form of surgical intervention. These systems can be taken into operating rooms and used to irradiate the tumour or tumour bed as part of a surgical procedure. Mobile techniques include brachytherapy treatments using sealed sources (i.e. HDR), electron units (Mobetron, Novac-7) and photon units (INTRABEAM®).
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Carl Zeiss Surgical (2007) INTRABEAM® system PRS 500 with XRS 4. Carl Zeiss Surgical, Oberkochen
Biggs DS, Thomson ES (1996) Radiation properties of a miniature X-ray device for radiosurgery. Br J Radiol 69:544–547
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Appendices
Appendices
3.1.1 Appendix A: Treatment Calculation Time
3.1.1.1 Depth Dose Curve in Water
During production or recalibration, Zeiss determines the depth dose curve of a given XRS in a specially designed water phantom that allows the mounting and positioning of the XRS without the stand, as well as the insertion of the ion chamber (IC) inside a purpose-made holder within the phantom. The current obtained from the IC measured at different depths (z) will allow calculation of the depth dose curve from the following equation:
where D w,z = absorbed dose to water at depth z; ICTP,z = ion chamber current reading in water phantom at depth z, temperature and pressure corrected; N s = calibration factor for the ion chamber used during the water phantom measurements taken from the PTW calibration certificate; f = conversion factor from roentgens to grays with a value of 8.81 mGy/R, as extracted from ICRU Report 17; and k q = beam quality correction factor – this takes the value of 1 for beam qualities in the (PTW) T30 to T50 range (accelerating voltage of 30 to 50 kV with effective energies of approx. 17–20 kV).
A fit function of the depth dose curve is generated mathematically to account for the impossibility of measuring directly on the surface of the XRS tip.
Similarly, depth dose curves are obtained with applicator, for each of the clinical applicators. The ratio between the depth curves with and without applicator provides the transfer function (Y z) for each applicator. Again, a fit function of these depth dose curves will be generated to account for the impossibility of directly measuring from the surface of the applicator.
Both calibration files, bare probe depth dose curve and applicator transfer functions, will be loaded onto the user terminal. The information is securely linked via the serial numbers of XRS and each individual applicator.
3.1.1.2 Original PAICH Output and IRM
Baseline values for dose rates and IRM rates are also loaded onto the system via calibration files obtained from measurements taken with the Zeiss factory PAICH and IC.
Thus, the original PAICH output at factory will be given as:
where ICTP = ion chamber current reading inside the PAICH, temperature and pressure corrected; N k,factory = calibration factor for the ion chamber used during the PAICHfactory measurements and taken from its PTW Air Kerma calibration certificate; and k q = beam quality correction factor as above.
3.1.1.3 Customer’s PAICH Output and IRM
The PAICH output measurement performed during the pre-treatment quality control determines the output of the XRS before the actual treatment session:
where N k,customer = calibration factor for the ion chamber used during the PAICHcustomer measurements taken from its PTW Air Kerma calibration certificate.
The software will compare the PAICH output value calculated during pre-treatment QA with that given in the stored calibration file. The software will not permit delivery of treatment when the deviation revealed by the comparison exceeds 10 %. If the deviation is between 5 and 10 %, the software will require the customer to acknowledge a warning message.
The actual absolute dose output in water (depth dose curve to be used for treatment) is calculated from the fitted depth dose curve in water and the factory and customer’s PAICH outputs:
Finally, the total depth dose curve for the XRS plus applicator chosen will be:
The calculated treatment time given by the INTRABEAM for a prescribed dose D w,z (Gy) will be:
This time and the actual IRM rate [count/s] measured during the pre-treatment QA procedure are used to calculate the total number of IRM counts that correspond to the treatment dose prescribed, D w,z [Gy].
where I actual = IRM rate during pre-treatment QA procedure.
The actual treatment time, i.e. time during which radiation is being emitted, may increase or decrease depending on whether the dose rate of the XRS changes during treatment. The radiation will stop once the total IRM counts have been reached. However, if the calculated counts are not reached during 110 % of the calculated treatment time, then the system will stop the treatment. The delivered dose, up until the system stops the radiation, is recorded at all times.
3.1.2 Appendix B: Troubleshooting
The following flowcharts aim to provide a quick guide to the essential steps to follow when a problem or interlock with the INTRABEAM system is encountered. Any problem beyond the common faults/interlocks given here will require consultation with the manufacturer before an attempt is made to resolve it.


Rights and permissions
Copyright information
© 2014 Springer-Verlag Berlin Heidelberg
About this chapter
Cite this chapter
Gonzalez, R., Reynolds, C. (2014). How to Use the INTRABEAM System. In: Keshtgar, M., Pigott, K., Wenz, F. (eds) Targeted Intraoperative Radiotherapy in Oncology. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-642-39821-6_3
Download citation
DOI: https://doi.org/10.1007/978-3-642-39821-6_3
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-642-39820-9
Online ISBN: 978-3-642-39821-6
eBook Packages: MedicineMedicine (R0)