Abstract
This chapter describes in detail how a CBCR course can be organized. All roles of students, peer teachers, and consultants are discussed, as well as the materials, required facilities, and coordinator tasks. A variation, using senior medical students acting as consultant, is described. A brief section on effectiveness concludes the chapter.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Following the summary description of CBCR education in Chap. 1, this chapter elaborates on a CBCR course in practice. This is to provide teachers and curriculum developers as much as possible with a detailed picture of a CBCR course as it unfolds. The description is derived from many years of experience at UMC Utrecht, which can be at some variance with other sites using CBCR, but readers should read this with their own local constraints in mind and adapt as far as necessary to meet local needs.
The Course Conditions
Scheduling Groups
CBCR takes place in small groups consisting of 10–13 students. If the class consists of 300 students (as is the case in Utrecht), 24 groups operate in parallel with 12 or 13 students each, which is a convenient number of groups to schedule from a logistical point of view. If all groups must meet within a week, 1 or 2 days can be allocated to schedule four sets of six groups for a CBCR session (e.g., groups 1–6 and 7–12 from 9:00-11:00 and 11:00–13:00, respectively, and groups 13–18 and 19–24 in the afternoon or at the same time the next day). This way the same rooms and consultants can be scheduled for multiple groups, and at the same time the exchange of information can be avoided by preventing too much spreading in between groups. Avoidance of exchange of information is to maximize the freshness of the case for the students. During the session follow-up information about the patient is provided that should not be known before the session.
Spread of Sessions Over the Year
Ten CBCR meetings in a year is a convenient number, but it could be twice as many. This can be scheduled, with at least 2 weeks in between sessions, to allow for enough time for students, consultants, and particularly peer teachers (see participant roles ) to prepare for sessions.
Curriculum planners should be mindful of conflicting obligations of the students for other courses and avoid planning sessions just before examinations. Another important consideration in planning sessions is that CBCR tries to apply and rehearse previously acquired knowledge. A case of a patient with shortness of breath should, for all groups, be scheduled after student had education about physiology and anatomy, and preferably pathology of relevant organ systems, in this case the respiratory system.
Rooms , Arrangement and Facilities
Rooms are suitable for CBCR session if students face each other and their peer teachers. A recommended arrangement is a square placement of tables with 2–4 chairs on each side. Peer teachers best sit next to each other and the consultant at a corner, to stress their more aloof role during the session. There should either be a blackboard (or whiteboard) or a flip-over chart if there is no board. A board is necessary to build clinical reasoning when filling tables of diagnostic hypotheses and history, signs and symptoms, test results, etc. in an interactive dialogue with the group.
Increasingly, computer projection screens are used, for instance , to depict the text of a “handout ” about new patient information at requested moments during the session. The table filling during group dialogues can also be done starting with an empty table on a projection screen . But an old-fashioned blackboard is at least as convenient.
Consultants
Consultants, the teachers present, should be clinicians and can be recruited from various clinical departments. They do not necessarily have to be very experienced clinicians. Indeed, that may even be a drawback. An experienced subspecialist may have less fresh knowledge about cases outside their specialty than a recent graduate. Our experiences with educationally interested residents or even interns around graduation, serving preclinical student groups, are excellent (Zijdenbos et al. 2010, 2011). Sometimes CBCR sessions are held with more advanced medical student groups; then a more experienced clinician may be advisable as a consultant.
It can be recommended, for reasons of group dynamics , to have a similar consultant facilitate a group throughout a year. The detailed consultant version of case descriptions includes answers to all questions and will support any physician to guide a CBCR session with junior medical students in cases that are not their specialty.
Materials
The written materials of a CBCR case include three versions: (a) a student version with the objectives , the requirements, a case introduction, and questions; (b) a peer teacher version , including all information of the student version and with additional information, hints, and all hand-out texts about additional patient information that needs to be provided at the right time during the session; and (c) a consultant version, consisting of the peer teacher version supplemented with background information and all model answers.
All students receive all student cases, usually together at the beginning of the course. Downloadable texts are convenient. At each session, the consultant provides the upcoming peer teachers with the peer teacher version of the case of the next session.
A CBCR Session
A CBCR session has a minimum duration of 1′45″ h and a maximum of 2′30″ h. During a session usually one but sometimes two patient cases are being discussed. The session is preferably led by three peer teachers . Having two peer teachers doing this is not impossible, but one peer teacher is not recommended as that makes sessions too vulnerable, and more than three is not practical. Before a meeting, all students should have read the assigned literature about the topic of the case described in a student version of the case that they have received at the beginning of the year or at least sufficiently long before the session. Clinical practice guidelines and a handbook for general practice could be suitable as preparatory materials for this purpose. All students must have read the recommended literature—which should be doable in a few hours—and the introduction of the patient case and have prepared the first few questions for that case, until the stage where new patient information must be provided to proceed with the case.
Across the course, at each session three different students serve as a peer teacher, so all students have turns in this role. These peer teachers are provided with more information about the patient case and are therefore able to guide the group through the case. Although a consultant (clinician teacher) is present, his or her role is really that of a true consultant: remaining at the background, responding to questions, and only interrupting to clarify things and help the group process.
The meeting starts by having one of the peer teachers read the initial patient vignette out loud, introducing the patient and his or her complaint. After this, the first question is introduced. Students are randomly asked by peer teachers to give and substantiate answers. The peer teachers collect all answers. They monitor that all answers are given in a way that stimulates the group discussion . If necessary, they can provide hints based on their thorough preparation.
During the sessions, the peer teachers guide these discussions, as they provide handouts containing additional information about the patient. Usually one mini lecture (5 to maximum 10 min) is given by one of the peer teachers, summarizing an essential feature of the case, often a pathophysiological mechanism or background information about diagnostic tests.
At the end of the session, one of the non-peer teaching students, usually randomly chosen, is asked to summarize the case in 2–3 min, in a way that resembles case summaries for handovers in the clinical setting.
Participant Roles
All students should be made familiar with the rules before the start of the first CBCR session . An introductory session to set the stage is useful for that purpose.
The Student Role
It is essential that the students have read about the topic in advance and have prepared the first few general questions of the case. They do not know how the case will unfold, as they have limited information about the patient. They must therefore read about the major complaint of the patient to have enough background information.
Students should realize that this education requires verbally active participation. Verbalization of thoughts is essential in the acquisition of clinical reasoning skill, even if those thoughts later become more routine, encapsulated, and tacit (Schmidt and Boshuizen 1993).
The Peer Teacher Role
Peer teachers perform an essential role in CBCR sessions since they act as teachers. Students have this role 2–3 times in a year and must prepare well for it.
The peer teachers must figure out in advance what pathology the patient has, guided by hints provided in their version of the case description. During the session, they should provide similar hints to students if needed and lead them through the case.
During the session the peer teachers are responsible for the active participation of all students in an equal manner. So they might give turns to students and proactively address the more silent students. They collect answers to case questions by summarizing items on a flip chart or board and letting students explain why they think the way they do. They are instructed to use tables to create a clear overview of answers given. See Table 6.1 for an example.
The three peer teacher students may distribute preparatory tasks among themselves before the session and during the session. One peer teacher can act as a chairperson for a series of questions, while one other can provide extra information or hints, and the third peer teacher summarizes after each question or discussion if needed. During the session, the peer teachers should regularly switch these sub-roles. All should be prepared to take all roles.
The Consultant Role
The consultant oversees the CBCR session , keeps a record of attendance, globally assesses the students’ active participation, and provides feedback to students and peer teachers. He or she distributes peer teacher versions of written materials for a next session and completes evaluation forms.
Their most important role is guiding the CBCR sessions in an adaptive way, depending on the quality of the guidance already provided by peer teachers. This is very different from what many teachers are familiar with in traditional curricula, in which they are the primary source of information and have strong instructional tasks. It also differs from many other tutorial teaching formats where the teacher remains a central instructor deciding how to proceed. Problem-based learning arrangements come closest to demanding a similar teacher role (Barrows and Tamblyn 1980), but that role is not particularly clinically focused and does not require clinical experience as in CBCR education. CBCR is different. Peer teachers lead sessions and discussions, and the consultant only supports and helps when things are unclear, by asking clarifying questions or by offering perspectives when students think of rare and exotic diseases and forget or are unaware of the predominant epidemiology. Consultants usually stimulate peer teachers best to lead the group when they remain aside and only interfere when really necessary. This gives students a great responsibility and stimulates clinical thinking. If necessary of course, they can be consulted and give answers to questions from the group.
In most CBCR courses, the consultant keeps an attendance list for each session to register when students are present or absent. The course director receives these lists regularly and will have an overview of the attendance of every student.
Students should be evaluated on their preparation and active participation during the session in the clinical thinking of the group. The marks together can be part of the final grade. Consultants learning the dynamics of their group can develop a balanced impression of the participation of its members over sessions, which helps both the decision when to interrupt discussions to redirect the group if needed and how to score the students’ participation.
After each session three new peer teachers receive the peer teachers’ version of the next case to prepare for the next class. With a class of 12, nine sessions and three peer teachers per session, every student has this role once in four sessions. This way every student fulfills at least twice the role of peer teacher. The consultant coordinates this and ensures that each student regularly fulfills peer teacher tasks and he or she controls the distribution of peer teacher versions of the materials. The first peer teachers receive their version in or after the introductory session, at which meeting also the procedures of CBCR are explained.
As part of a continuous quality assurance of the course, it is very useful if consultants write down feedback about cases during or directly after sessions, such as linguistic errors, medical inadequacies or pedagogical improvements, and provide these comments to the CBCR course director .
CBCR Course Management
To organize a CBCR course in the curriculum, a course director or course manager needs to be appointed, as should be the case for any course. Tasks of the course director are planning sessions, preparing and delivering materials to consultants and students, collecting records of attendance and case evaluations, instructing students and faculty (consultants), serving as a contact person for students and consultants, evaluating and updating materials annually, and preparing and administering exams. At UMC Utrecht, the course management is carried out by a team of three and, in total, requires about a 0.2 full-time equivalent for 24 groups, i.e., 300 students, to be served.
The course director should make sure that there are no scheduling conflicts with other courses or exams. It is recommended to randomly assign students to groups. This improves group dynamics , allows struggling students to learn from others, and also challenges clever students to improve their argumentation by explaining their thoughts to their peers. During the course, the group should keep the same composition.
The course director should ensure that all consultants and students receive their respective versions of the course materials and should avoid that consultant versions are seen by students, as that may interfere with the desired reasoning process during the class. Consultants receive, in addition, peer teacher materials, forms for registration of attendance and for marking of students, and program evaluation forms. At UMC Utrecht a photograph of the students of each group is taken during the first session with students holding their names on a piece of paper. This helps consultants to know their students by face from the very start. The consultant keeps an overview of which students have been peer teachers and makes sure that all students perform their respective roles.
A general CBCR study guide should also be included in the folder for consultants. It contains the description of the course for the students and explains the rules and regulations of the course (see Chap. 10). For some CBCR cases, as a service for the consultant, additional literature can be included as well.
Recruiting and instructing consultants should be one of the course director’s tasks. New consultants must become familiar with the course requirements and procedures. An annual faculty development workshop for new consultants is an excellent opportunity to supplement with oral instructions and discussions. More elaborate faculty development, as explained in Chap. 9, may include a volunteer student CBCR group meeting during such a workshop, with new consultants practicing or observing.
As is the case with new consultants, students are usually not familiar with CBCR before the course either. An annual information session, such as a lecture, is useful before the CBCR course starts and should elaborate on what the purposes and practice of CBCR are. Most practical aspects should be discussed, e.g., what is expected of students in their roles of regular students or peer teachers, what students should prepare for sessions, how sessions proceed, and what the end-of-term examination will look like. Tasks of students and peer teachers should be explained, but also the task of the consultant and the different setup of CBCR compared to other courses. It should be made clear that students are largely responsible for the CBCR sessions and that a good preparation of their part is essential to make sessions a success.
The CBCR course director oversees the cases written. All cases and case revisions should however be written or at least thoroughly checked by a specialist on the topic and preferably by someone who checks language, following instructions as elaborated in Chap. 8.
The course director should also be the responsible examiner, who designs and administers exams and analyzes and communicates results, if needed assisted by content experts. We refer for details to Chap. 7.
A CBCR Course Version Using Senior Medical Students as Consultants
In the most recent years at UMC Utrecht, the CBCR course uses final year medical students as consultants for second year medical students. This near-peer consultant role, with a 4-year difference in education, has proven to be a successful adaptation. All final year medical students at Utrecht have a 1-week mandatory teacher training course with different components (Zijdenbos et al. 2011). One component is a true teaching experience with second year medical students in at least one CBCR session . These near-peer consultants receive a thorough pedagogical instruction and receive the consultant version of the case materials for their session (Zijdenbos et al. 2010). The teacher training course is delivered in groups of 15 students who are prepared and debriefed before and after the CBCR session. Their role as a consultant includes facilitating, evaluating, and scoring students and peer teachers for active participation. Across the year all ±300 final year students must practice this teaching, usually in a team of two, once or twice with one of the 24 groups in one of their nine sessions. The schedules are organized in a way to provide all second year groups with near-peer consultants . Both the sixth year students and the second year students show consistent favorable evaluations of their experiences as receivers and providers of clinical reasoning training, since the start of this model in 2006 (Zijdenbos et al. 2010).
Evidence of Effectiveness
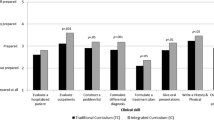
As said, CBCR courses have been well received across decades of implementation. Student ratings are usually high. There is no doubt that students and schools consider the courses valuable. A comparative study to objectify this impression has not been carried out however. The reason is that this curriculum model has been applied across complete cohorts and because the course did not replace a different course with similar objectives , which excludes a suitable comparison group. In other words, there is no treatment comparison with the same or similar students possible. Comparing the effects of curricula with and without the CBCR course is difficult because of methodological and confounding problems. However, one interesting curriculum comparison study has been reported in the literature. In 1996 Schmidt et al. reported superior performance of an Amsterdam cohort of students that compared two other universities in the preclinical years 2 and 3 (Schmidt et al. 1996). The Amsterdam curriculum had recently introduced a CBCR course that later stood model for the Utrecht CBCR course (ten Cate 1994). The effect that Schmidt et al. found may have been caused by the CBCR course in that curriculum. While this is speculation, no other explanation has been offered for the superiority of the Amsterdam curriculum in the preclinical years of a measure of clinical reasoning.
Finally, the development of illness scripts , an objective of the CBCR course by students, was recently studied and found to be better in preclinical students for cases discussed in the CBCR course than other common cases not studied in the CBCR course (Keemink et al. n.d.).
References
Barrows, H. S., & Tamblyn, R. M. (1980). Problem-based learning. An approach to medical education. New York: Springer.
Keemink, Y. et al. (n.d.) Illness script development through Case-Based Clinical Reasoning training. Submitted.
Schmidt, H. G., & Boshuizen, H. P. A. (1993). On acquiring expertise in medicine. Educational Psychology Review, 5(3), 205–221.
Schmidt, H., et al. (1996). The development of diagnostic competence: Comparison of a problem-based, and integrated and a conventional medical curriculum. Academic Medicine, 71(6), 658–664.
ten Cate, O. (1994). Training case-based clinical reasoning in small groups [Dutch]. Nederlands Tijdschrift voor Geneeskunde, 138, 1238–1243.
Zijdenbos, I. L., et al. (2010). A student-led course in clinical reasoning in the core curriculum. International Journal of Medical Education, 1, 42–46.
Zijdenbos, I., Fick, T., & ten Cate, O. (2011). How we offer all medical students training in basic teaching skills. Medical Teacher, 33(1), 24–26.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2018 The Author(s)
About this chapter
Cite this chapter
van Zijl, A., van Loon, M., ten Cate, O. (2018). Case-Based Clinical Reasoning in Practice. In: ten Cate, O., Custers, E., Durning, S. (eds) Principles and Practice of Case-based Clinical Reasoning Education . Innovation and Change in Professional Education, vol 15. Springer, Cham. https://doi.org/10.1007/978-3-319-64828-6_6
Download citation
DOI: https://doi.org/10.1007/978-3-319-64828-6_6
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-64827-9
Online ISBN: 978-3-319-64828-6
eBook Packages: EducationEducation (R0)