Abstract
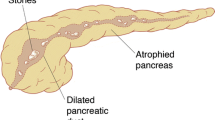
For chronic pancreatitics who have a glandular morphology characterized by a dilated main pancreatic duct, pain is thought to be due to ductal hypertension and glandular/capsular stretch. Decompression of the pancreatic duct by either endoscopic transampullary stenting or surgical drainage is the principle method of treating symptoms in these patients. Surgical intervention is commonly thought to carry increased risk of perioperative morbidity, thus current practice involves an intervention sequence starting with endoscopic stenting and falling back to surgery in cases of recalcitrant pain. There is, however, little evidence to argue that an “endoscopy first” approach is better than early surgical intervention. Few studies prospectively examine outcomes of endoscopy compared to surgery in terms of pain relief, morbidity and mortality, number of repeated interventions, and preservation of pancreatic function. The evidence that is available suggests surgical management of large duct chronic pancreatitis results in better long term outcomes when compared to endoscopic therapy without incurring prohibitive risk of significant perioperative morbidity. In our view, surgical drainage of the pancreas should be considered as a primary method of managing patients with chronic pancreatitis and a dilated main pancreatic duct.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
D’Haese JG, Ceyham GO, Demir IE, et al. Treatment options in painful chronic pancreatitis: a systematic review. HPB (Oxf). 2014;16:512–21.
Issa Y, van Santvoort HC, van Goor H, et al. Surgical and endoscopic treatment of pain in chronic pancreatitis: a multidisciplinary update. Dig Surg. 2013;30:35–50.
Issa Y, Bruno MJ, Bakker OJ, et al. Treatment options for chronic pancreatitis. Nat Rev Gastroenterol Hepatol. 2014;11:556–64. doi:10.1038/nrgastro.2014.74.
Ali Ahmed UA, Issa Y, Bruno M, et al. Early surgery versus optimal current step-up practice for chronic pancreatitis (ESCAPE): design and rational of a randomized trial. BMC Gastroenterol. 2013;13:49.
Glass LM, Whitcomb DC, Yadav D, et al. Spectrum of use and effectiveness of endoscopic and surgical therapies for chronic pancreatitis in the United States. Pancreas. 2014;43:539–43.
Clarke B, Silvka A, Tomizawa Y, et al. Endoscopic therapy is effect for patients with chronic pancreatitis. Clin Gastroenterol Hepatol. 2012;10:795–802.
Hong J, Wang J, Keleman AM, et al. Endoscopic versus surgical treatment of downstream pancreatic duct stones in chronic pancreatitis. Am Surg. 2011;77(11):1531–8.
Nealon WH, Thomson JC. Progressive loss of pancreatic function in chronic pancreatitis is delayed by main pancreatic duct decompression. A longitudinal prospective analysis of the modified Puestow procedure. Ann Surg. 1993;217:458–66.
Ali Ahmed UA, Pahlplatz JM, Nealon WH, et al. Endoscopic or surgical intervention for painful obstructive chronic pancreatitis (review). Cochrane Libr. 2012;(1):CD007884. doi:10.1002/14651858.CD007884.pub2.
Dite P, Ruzicka M, Zboril V, Novotny I. A prospective, randomized trial comparing endoscopic and surgical therapy for chronic pancreatitis. Endoscopy. 2003;35(7):553–8.
Cahen DL, Gouma DJ, Nio Y, et al. Endoscopic versus surgical drainage of the pancreatic duct in chronic pancreatitis. N Eng J Med. 2007;356(7):676–84.
Cahen DL, Gouma DJ, Laramee P, et al. Long-term outcomes of endoscopic vs surgical drainage of the pancreatic duct in patients with chronic pancreatitis. Gastroenterology. 2011;141:1690–5.
Rutter K, Ferlitsch A, Sautner T, et al. Hospitalization, frequency of interventions and quality of life after endoscopic, surgical, or conservative treatment in patients with chronic pancreatitis. World J Surg. 2010;34:2642–7.
Hirota M, Asakura T, Kanno A, et al. Long-period pancreatic stenting for painful chronic calcified pancreatitis required high medical costs and frequent hospitalizations compared with surgery. Pancreas. 2011;40:946–50.
Ahmed Ali UA, Nieuwenhuijs VB, van Eijck CH, et al. Clinical outcome in relation to timing of surgery in chronic pancreatitis: a nomogram to predict pain relief. Arch Surg. 2012;147:825–32.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Liu, J.B., Baker, M.S. (2016). Surgery or Endotherapy for Large Duct Chronic Pancreatitis. In: Millis, J., Matthews, J. (eds) Difficult Decisions in Hepatobiliary and Pancreatic Surgery. Difficult Decisions in Surgery: An Evidence-Based Approach. Springer, Cham. https://doi.org/10.1007/978-3-319-27365-5_42
Download citation
DOI: https://doi.org/10.1007/978-3-319-27365-5_42
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-27363-1
Online ISBN: 978-3-319-27365-5
eBook Packages: MedicineMedicine (R0)