Abstract
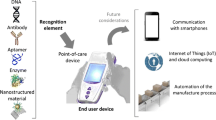
Point-of-Care (POC) devices enable medical interventions, such as testing, to be performed near the patient and often by the patient. It has been suggested that the use of POC devices will change medicine from a symptom/diagnosis/treatment endeavor to a monitoring/prediction/prevention exercise. The rate at which this area introduces innovation and discovery is high, although a majority of such devices are currently utilized for screening purposes. This article discusses the public health benefits of POC devices in terms of patient engagement, health inequality, health promotion and their impact on healthcare system. Low-cost screening clinics that use POC devices ultimately help reduce health inequality in developing countries and remote areas. The article also outlines the issues hindering the benefits of using POC such as connectivity, integration and data management, and calibration. Further, it suggests a framework to present and evaluate POC devices used in the healthcare industry. We argue that having such a framework provides a set of measures to evaluate and select POC for various tasks. The scope of this study is limited to medical-grade devices used at home or in clinics, aged care facilities, and hospital settings.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
R. Abdolkhani, A. Borda, K. Gray, Quality management of patient generated health data in remote patient monitoring using medical wearables—a systematic review. Stud. Health Technol. Inform. 252, 1–7 (2018)
W.T. Abraham, L.W. Stevenson, R.C. Bourge, J.A. Lindenfeld, J.G. Bauman, P.B. Adamson, C.T.S. Group, Sustained efficacy of pulmonary artery pressure to guide adjustment of chronic heart failure therapy: complete follow-up results from the champion randomised trial. Lancet 387, 453–641 (2016). https://doi.org/10.1016/S0140-6736(15)00723-0
P. Adhikari, S. Pemminati, R. Pathak, M.S. Kotian, S. Ullal, Prevalence of hypertension in Boloor diabetes study (BDS-II) and its risk factors. J. Clin. Diagnos. Res. JCDR 9, IC01–IC04 (2015). https://doi.org/10.7860/JCDR/2015/16509.6781
P. Aggarwal, S. Galwankar, J. Nayer, Utility of point-of-care testing of natriuretic peptides (brain natriuretic peptide and n-terminal pro-brain natriuretic peptide) in the emergency department. Int. J. Crit. Illn. Inj. Sci. 4, 209 (2014). https://doi.org/10.4103/2229-5151.141406
A. Alanazi, Using machine learning for healthcare challenges and opportunities (2022). https://doi.org/10.1016/j.imu.2022.100924
A. Alshaer, B.A. Badgheish, Z.H. Alsadah, K. Sewify, S. Alghazal, S. Alzahrani, A. Qadi, R. Alqahtani, G.A. Farsani, A. Shilash, Comparing the accuracy of point-of-care with laboratory (capillary, venous, and arterial) blood glucose levels in critically ill patients with and without shock. BMC Res. Notes 15(1), 372 (2022)
C. American Pathologists, Point-of-care-testing checklist CAP accreditation program (2021), www.cap.org. Accessed 09.22.2021
R. Anchala, N.K. Kannuri, H. Pant, H. Khan, O.H. Franco, E.D. Angelantonio, D. Prabhakaran, Hypertension in india: a systematic review and meta-analysis of prevalence, awareness, and control of hypertension (2014). https://doi.org/10.1097/HJH.0000000000000146
E. Andrès, L. Meyer, A.A. Zulfiqar, M. Hajjam, S. Talha, T. Bahougne, S. Ervé, J. Hajjam, J. Doucet, N. Jeandidier, A.H.E. Hassani, Telemonitoring in diabetes: evolution of concepts and technologies, with a focus on results of the more recent studies (2019). https://doi.org/10.25122/jml-2019-0006
E. Archibong, K.R. Konnaiyan, H. Kaplan, A. Pyayt, A mobile phone-based approach to detection of hemolysis. Biosens. Bioelectron. 88, 204–209 (2017). https://doi.org/10.1016/j.bios.2016.08.030
E. Bakker, Can calibration-free sensors be realized? ACS Sensors 1, 838–841 (2016)
H. Banaee, M.U. Ahmed, A. Loutfi, Data mining for wearable sensors in health monitoring systems: a review of recent trends and challenges (2013). https://doi.org/10.3390/s131217472
F. Barbabella, M.G. Melchiorre, S. Quattrini, R. Papa, G. Lamura, European observatory policy briefs (2017)
S. Barello, S. Triberti, G. Graffigna, C. Libreri, S. Serino, J. Hibbard, R. Giuseppe, ehealth for patient engagement: a systematic review. Front. Psychol. (2016)
D. Betts, R. Gordon, A.M. Egizi, C.B. Cruse, The future of the public’s health (2021), https://www2.deloitte.com/us/en/insights/industry/health-care/the-future-of-public-health.html
Y. Bombard, G.R. Baker, E. Orlando, C. Fancott, P. Bhatia, S. Casalino, K. Onate, J.L. Denis, M.P. Pomey, Engaging patients to improve quality of care: a systematic review. Implement. Sci. 13, 98 (2018). https://doi.org/10.1186/s13012-018-0784-z
J.W.L. Cals, A.M.R. Schols, H.C.P.M. van Weert, F. Stevens, C.G.I.P. Zeijen, G. Holtman, W.A.M. Lucassen, M.Y. Berger, Point-of-care testing in family practices: present use and need for tests in the future. Ned. Tijdschr. Geneeskd. 158, A8210 (2014)
S. Campuzano, M. Pedrero, M. Gamella, V. Serafín, P. Yáñez-Sedeño, J.M. Pingarrón, Beyond sensitive and selective electrochemical biosensors: towards continuous, real-time, antibiofouling and calibration-free devices. Sensors (Basel) 20(12), 3376 (2020)
A.D. Cerbo, N. Quagliano, A. Napolitano, F. Pezzuto, T. Iannitti, A.D. Cerbo, Comparison between an emerging point-of-care tool for TSH evaluation and a centralized laboratory-based method in a cohort of patients from southern Italy. Diagnostics 11 (2021). https://doi.org/10.3390/diagnostics11091590
CISCO: Cisco annual internet report (2018-2023) white paper (2020)
M. Clinic, Remote patient monitoring: comprehensive care at home (2021), https://www.mayoclinichealthsystem.org/hometown-health/speaking-of-health/remote-patient-monitoring-comprehensive-care-at-home
P. Commission, Managed competition in health care (The Commission, 2002), p. 97
G.L. Damhorst, E.A. Tyburski, O. Brand, G.S. Martin, W.A. Lam, Diagnosis of acute serious illness: the role of point-of-care technologies. Curr. Opin. Biomed. Eng. 11, 22–34 (2019)
C. Doherty, C. Stavropoulou, Patients’ willingness and ability to participate actively in the reduction of clinical errors: a systematic literature review. Soc. Sci. Med. 75, 257–263 (2012). https://doi.org/10.1016/j.socscimed.2012.02.056
N. Engel, P. Wolffs, Aligning diagnostics to the point-of-care: lessons for innovators, evaluators and decision-makers from tuberculosis and HIV. BMJ Global Health 5 (2020). https://doi.org/10.1136/bmjgh-2020-003457
R. Erasmus, S. Sahni, R. El-Sharkawy, Connectivity strategies in managing a POCT service. EJIFCC 32(2), 190–194 (2021)
J. Espinoza, N.Y. Xu, K.T. Nguyen, D.C. Klonoff, The need for data standards and implementation policies to integrate CGM data into the electronic health record. J. Diabetes Sci. Technol. 17(2), 495–502 (2023)
G. Fagherazzi, P. Ravaud, Digital diabetes: perspectives for diabetes prevention, management and research. Diabetes Metab. 45, 322–329 (2019). https://doi.org/10.1016/J.DIABET.2018.08.012
V. Foerster, M. Severn, Point-of-care glycated hemoglobin testing to diagnose type 2 diabetes (2017)
A. Ghaffari, R. Meurant, A. Ardakani, COVID-19 point-of-care diagnostics that satisfy global target product profiles. Diagnostics 11 (2021). https://doi.org/10.3390/diagnostics11010115
M. Ghassemi, T. Naumann, P. Schulam, A.L. Beam, I.Y. Chen, R. Ranganath, A review of challenges and opportunities in machine learning for health, in AMIA Joint Summits on Translational Science (2020)
A. Gialamas, L.N. Yelland, P. Ryan, K. Willson, C.O. Laurence, T.K. Bubner, P. Tideman, J.J. Beilby, Does point-of-care testing lead to the same or better adherence to medication? A randomised controlled trial: the poct in general practice trial. Med. J. Aust. 191, 487–491 (2009). https://doi.org/10.5694/j.1326-5377.2009.tb02910.x
G. Graffigna, S. Barello, Spotlight on the patient health engagement model (PHE model): a psychosocial theory to understand people’s meaningful engagement in their own health care. Patient Prefer Adherence 12, 1261–1271 (2018). https://doi.org/10.2147/ppa.S145646
L.A. Hagens, A.R.M. Verschueren, A. Lammers, N.F.L. Heijnen, M.R. Smit, T.M.E. Nijsen, I. Geven, M.J. Schultz, D.C.J.J. Bergmans, R.M. Schnabel, L.D.J. Bos, Development and validation of a point-of-care breath test for octane detection. Analyst 146(14), 4605–4614 (2021)
M. Haghi, S. Danyali, S. Ayasseh, J. Wang, R. Aazami, T.M. Deserno, Wearable devices in health monitoring from the environmental towards multiple domains: A survey. Sensors 21, 1–24 (2021). https://doi.org/10.3390/s21062130, cited by: 3 Export Date: 30 October 2021
M. Harvey, A. Seiler, Challenges in managing a remote monitoring device clinic. Heart Rhythm O2 3(1), 3–7 (2022)
Z. Hosseini, S.J. Whiting, H. Vatanparast, Type 2 diabetes prevalence among Canadian adults—dietary habits and sociodemographic risk factors. Appl. Physiol. Nutr. Metab. 44, 1099–1104 (2019). https://doi.org/10.1139/apnm-2018-0567
M.P. Hudson, R.H. Christenson, L.K. Newby, A.L. Kaplan, E.M. Ohman, Cardiac markers: point of care testing (1999)
P. Jiang, J. Winkley, C. Zhao, R. Munnoch, G. Min, L.T. Yang, An intelligent information forwarder for healthcare big data systems with distributed wearable sensors. IEEE Syst. J. 10(3), 1147–1159 (2016). https://doi.org/10.1109/JSYST.2014.2308324
P. Jørgensen, A. Langhammer, S. Krokstad, S. Forsmo, Mortality in persons with undetected and diagnosed hypertension, type 2 diabetes, and hypothyroidism, compared with persons without corresponding disease—a prospective cohort study; the HUNT Study, Norway. BMC Fam. Pract. 18, 98 (2017). https://doi.org/10.1186/s12875-017-0672-7
S. Kanji, J. Buffie, B. Hutton, P.S. Bunting, A. Singh, K. McDonald, D. Fergusson, L.A. McIntyre, P.C. Hebert, Reliability of point-of-care testing for glucose measurement in critically ill adults. Crit. Care Med. 33(12), 2778–2785 (2005)
S.H. Kaplan, S. Greenfield, J.E. Ware, Assessing the effects of physician-patient interactions on the outcomes of chronic disease. Med. Care 27(3 Suppl), S110–S127 (1989)
D. Kapoor, P. Singh, M. Srivastava, Point of care blood gases with electrolytes and lactates in adult emergencies. Int. J. Crit. Illn. Inj. Sci. 4, 216 (2014). https://doi.org/10.4103/2229-5151.141411
C.J. Kelly, A. Karthikesalingam, M. Suleyman, G. Corrado, D. King, Key challenges for delivering clinical impact with artificial intelligence (2019). https://doi.org/10.1186/s12916-019-1426-2
S. Kennedy, How big data analytics can support preventive health (2022), https://healthitanalytics.com/features/how-big-data-analytics-can-support-preventive-health
M.M.A. Kip, J.M. Hummel, E.B. Eppink, H. Koffijberg, R.M. Hopstaken, M.J. IJzerman, R. Kusters, Understanding the adoption and use of point-of-care tests in Dutch general practices using multi-criteria decision analysis. BMC Fam. Pract. 20(1), 8 (2019)
A.N. Konwar, V. Borse, Current status of point-of-care diagnostic devices in the Indian healthcare system with an update on Covid-19 pandemic (2020). https://doi.org/10.1016/j.sintl.2020.100015
S. Kumar, M. Nehra, S. Khurana, N. Dilbaghi, V. Kumar, A. Kaushik, K.H. Kim, Aspects of point-of-care diagnostics for personalized health wellness (2021). https://doi.org/10.2147/IJN.S267212
D. Kuupiel, V. Bawontuo, P.K. Drain, N. Gwala, T.P. Mashamba-Thompson, Supply chain management and accessibility to point-of-care testing in resource-limited settings: a systematic scoping review. BMC Health Services Res. 19, 519 (2019). https://doi.org/10.1186/s12913-019-4351-3
Labcompare: Point of care devices (POC diagnostic devices) (2022), https://www.labcompare.com/Clinical-Diagnostics/5096-POC-Diagnostic-Devices/
G. Lenaerts, G.E. Bekkering, M. Goossens, L. De Coninck, N. Delvaux, S. Cordyn, J. Adriaenssens, P. Vankrunkelsven, Tools to assess the trustworthiness of evidence-based point-of-care information for health care professionals: systematic review. J. Med. Internet Res. 22(1), e15415 (2020)
H. Li, P. Dauphin-Ducharme, G. Ortega, K.W. Plaxco, Calibration-free electrochemical biosensors supporting accurate molecular measurements directly in undiluted whole blood. J. Am. Chem. Soc. 139(32), 11207–11213 (2017)
D. Lingervelder, H. Koffijberg, R. Kusters, M.J. Ijzerman, Point-of-care testing in primary care: a systematic review on implementation aspects addressed in test evaluations. Int. J. Clin. Pract. 73 (2019). https://doi.org/10.1111/ijcp.13392
F. Liu, P. Demosthenes, Real-world data: a brief review of the methods, applications, challenges and opportunities (2022). https://doi.org/10.1186/s12874-022-01768-6
M. Magnocavallo, G. Vetta, A. Bernardini, A. Piro, M.C. Mei, M.D. Iorio, M.V. Mariani, D.G.D. Rocca, P. Severino, R. Quaglione, G. Giunta, C. Chimenti, F. Miraldi, C.D. Vizza, F. Fedele, C. Lavalle, Impact of COVID-19 pandemic on cardiac electronic device management and role of remote monitoring (2022). https://doi.org/10.1016/j.ccep.2021.10.010
A. Manocha, S. Bhargava, Emerging challenges in point-of-care testing. Curr. Med. Res. Pract. (2019)
J. McKeon, Ai in healthcare poses algorithmic bias, data privacy, security risks (2022), https://healthitanalytics.com/news/biases-in-artificial-intelligence-led-to-
M.P. Mcnerney, Y. Zhang, P. Steppe, A.D. Silverman, M.C. Jewett, M.P. Styczynski, Point-of-care biomarker quantification enabled by sample-specific calibration. Sci. Adv. 5 (2019), https://www.science.org
MEDTEK: 5 important benefits of point-of-care testing (poct) (2022), https://medtek.com.ph/2022/06/03/5
B.B. Nunna, D. Mandal, S. Zhuang, E.S. Lee, A standalone micro biochip to monitor the cancer progression by measuring cancer antigens as a point-of-care (POC) device for enhanced cancer management, pp. 212–215 (2017). https://doi.org/10.1109/HIC.2017.8227622
B. Pais, P. Buluschek, G. DuPasquier, T. Nef, N. Schütz, H. Saner, D. Gatica-Perez, V. Santschi, Evaluation of 1-year in-home monitoring technology by home-dwelling older adults, family caregivers, and nurses. Front. Public Health 8 (2020). https://doi.org/10.3389/fpubh.2020.518957
M.L. Parker, P.M. Yip, L.V. DeCherrie, C. Escobar, A.K. Füzéry, C.P. Price, A. St John, There’s no place like home: exploring home-based, acute-level healthcare. Clin. Chem. 64(8), 1136–1142 (2018). https://doi.org/10.1373/clinchem.2017.283093
A. Plüddemann, C. Heneghan, M. Thompson, N. Roberts, N. Summerton, L. Linden-Phillips, C. Packer, C.P. Price, Prioritisation criteria for the selection of new diagnostic technologies for evaluation. BMC Health Serv. Res. 10(1), 109 (2010)
A.S. Poncette, L. Mosch, C. Spies, M. Schmieding, F. Schiefenhövel, H. Krampe, F. Balzer, Improvements in patient monitoring in the intensive care unit: survey study. J. Med. Internet Res. 22, e19091 (2020). https://doi.org/10.2196/19091
T. Poongodi, R. Krishnamurthi, R. Indrakumari, P. Suresh, B. Balusamy, Wearable Devices and IoT (Springer International Publishing, Cham, 2020), pp. 245–273. https://doi.org/10.1007/978-3-030-23983-1_10
C. Public, Cisco annual internet report (2018)
C.C. Quinn, E.C. Butler, K.K. Swasey, M.D. Shardell, M.D. Terrin, E.A. Barr, A.L. Gruber-Baldini, Mobile diabetes intervention study of patient engagement and impact on blood glucose: mixed methods analysis. JMIR mHealth uHealth 6, e31.2 (2018). https://doi.org/10.2196/mhealth.9265
R. Rajendran, G. Rayman, Point-of-care blood glucose testing for diabetes care in hospitalized patients: an evidence-based review (2014). https://doi.org/10.1177/1932296814538940
M.I. Razzak, M. Imran, G. Xu, Big data analytics for preventive medicine. Neural Comput. Appl. 32, 4417–4451 (2020). https://doi.org/10.1007/s00521-019-04095-y
Research, Markets: Global point of care diagnostics/testing market size, share & trends analysis report, 2019-2025—researchandmarkets.com (2019), https://search.ebscohost.com/login.aspx?direct=true &AuthType=sso &db=bwh &AN=bizwire.c88717437 &site=eds-live &scope=site &custid=s2775460, business Wire (English) Accession Number: bizwire.c88717437; Issue Information; Place of Event: DUBLIN; Document Type: Article
C.R. Rousseau, P. Bühlmann, Calibration-free potentiometric sensing with solid-contact ion-selective electrodes. TrAC Trends Anal. Chem. 140, 116277 (2021). https://doi.org/10.1016/j.trac.2021.116277; www.sciencedirect.com/science/article/pii/S016599362100100X
A.H. Sapci, H.A. Sapci, Innovative assisted living tools, remote monitoring technologies, artificial intelligence-driven solutions, and robotic systems for aging societies: systematic review. JMIR Aging 2(2), e15429 (2019). https://doi.org/10.2196/15429
M. Shephard, A. Shephard, S. Matthews, K. Andrewartha, The benefits and challenges of point-of-care testing in rural and remote primary care settings in Australia. Arch. Pathol. Lab. Med. 144 (2020). https://doi.org/10.5858/arpa.2020-0105-RA
N. Shimizu, K. Kotani, Health information exchange in relation to point-of-care testing in home care: issues in Japan. Clin. Chim. Acta 532, 10–12 (2022). https://doi.org/10.1016/j.cca.2022.05.013
B. Sorensen, S. Hunskaar, Point-of-care ultrasound in primary care: a systematic review of generalist performed point-of-care ultrasound in unselected populations. Ultrasound J. 11(1), 31 (2019)
R. Steinberg, B. Anderson, Z. Hu, T.M. Johnson, J.B. O’Keefe, L.C. Plantinga, R. Kamaleswaran, B. Anderson, Associations between remote patient monitoring programme responsiveness and clinical outcomes for patients with COVID-19. BMJ Open Qual. 10 (2021). https://doi.org/10.1136/bmjoq-2021-001496
M. Stevenson, A situation analysis of the state of supply of in vitro diagnostics in low-income countries. Glob. Public Health 15, 1836–1846 (2020). https://doi.org/10.1080/17441692.2020.1801791
A. Stranieri, S. Venkatraman, J. Minicz, A. Zarnegar, S. Firmin, V. Balasubramanian, H. Jelinek, Emerging point of care devices and artificial intelligence: prospects and challenges for universal health risk assessment. Under review (2021)
E.K.W. Tan, Y.Z. Au, G.K. Moghaddam, L.G. Occhipinti, C.R. Lowe, Towards closed-loop integration of point-of-care technologies. Trends Biotechnol. 37(7), 775–788 (2019)
S. Thukral, S. Vedantham, Clinical medicine catheter-based therapies and other management strategies for deep vein thrombosis and post-thrombotic syndrome. https://doi.org/10.3390/jcm9051439
S. Tian, W. Yang, J.M.L. Grange, P. Wang, W. Huang, Z. Ye, Smart healthcare: making medical care more intelligent. J. Glob. Health 3, 62–65 (2019). https://doi.org/10.1016/j.glohj.2019.07.001
P.J. Turner, A. Van den Bruel, C.H.D. Jones, A. Plüddemann, C. Heneghan, M.J. Thompson, C.P. Price, J. Howick, Point-of-care testing in UK primary care: a survey to establish clinical needs. Fam. Pract. 33(4), 388–394 (2016)
J. Vespa, L. Medina, D.M. Armstrong, Demographic turning points for the united states: population projections for 2020 to 2060 population estimates and projections current population reports (2020), www.census.gov/programs-surveys/popproj
C. Wang, M. Liu, Z. Wang, S. Li, Y. Deng, N. He, Point-of-care diagnostics for infectious diseases: from methods to devices (2021). https://doi.org/10.1016/j.nantod.2021.101092
C.F. Weber, K. Zacharowski, Perioperative point-of-care-Gerinnungsdiagnostik. Deutsches Arzteblatt Int. 109 (2012). https://doi.org/10.3238/arztebl.2012.0369
M.A. Weigelt, R. Sivamani, H. Lev-Tov, The therapeutic potential of cannabinoids for integumentary wound management. Exp. Dermatol. 30, 201–211 (2021). https://doi.org/10.1111/exd.14241
D. Weiss, H.T. Rydland, E. Øversveen, M.R. Jensen, S. Solhaug, S. Krokstad, Innovative technologies and social inequalities in health: a scoping review of the literature. PLoS One 13, e0195447–e0195447 (2018). https://doi.org/10.1371/journal.pone.0195447
J.B. Withall, J.M. Schwartz, J. Usseglio, K.D. Cato, A scoping review of integrated medical devices and clinical decision support in the acute care setting. Appl. Clin. Inform. 13(5), 1223–1236 (2022)
H.Y. Wong, L.G. Marcu, E. Bezak, N.A. Parange, Review of health economics of point-of-care testing worldwide and its efficacy of implementation in the primary health care setting in remote Australia. Risk Manag. Healthc. Policy 13, 379–386 (2020). https://doi.org/10.2147/rmhp.s247774
World Health Organization, More than 700 million people with untreated hypertension (2021), https://www.who.int/news/item/25-08-2021-more-than-700-million-people-with-untreated-hypertension
J. Yao, R. Schmitz, S. Warren, A wearable point-of-care system for home use that incorporates plug-and-play and wireless standards. IEEE Trans. Inf. Technol. Biomed. 9(3), 363–371 (2005)
E.H. Yayan, M. Zengin, A key point in medical measurements: device calibration and knowledge level of healthcare professionals. Int. J. Car. Sci. 13(2), 1346–1354 (2020)
A. Yu, The value of POCT (Point of Care Technology) investing in 2020 (2020), https://www.linkedin.com/pulse/value-poct-point-care-technology-investing-2020-andy-yu/
E. Øversveen, Stratified users and technologies of empowerment: theorising social inequalities in the use and perception of diabetes self-management technologies. Sociol. Health Illn. 42, 862–876 (2020). https://doi.org/10.1111/1467-9566.13066
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Zarnegar, A. (2023). Point-of-Care Devices in Healthcare: A Public Health Perspective. In: Daimi, K., Alsadoon, A., Seabra Dos Reis, S. (eds) Current and Future Trends in Health and Medical Informatics. Studies in Computational Intelligence, vol 1112. Springer, Cham. https://doi.org/10.1007/978-3-031-42112-9_4
Download citation
DOI: https://doi.org/10.1007/978-3-031-42112-9_4
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-42111-2
Online ISBN: 978-3-031-42112-9
eBook Packages: Intelligent Technologies and RoboticsIntelligent Technologies and Robotics (R0)