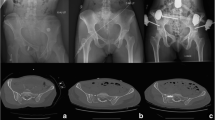
Abstract
Pelvic ring malunions and non-unions can be debilitating for patients and extremely challenging for the surgeon to manage. Even in the best of situations it is difficult to obtain an excellent outcome. Detailed workup of the patient must be performed to identify all modifiable and non-modifiable risk factors. Careful analysis of all imaging is necessary to understand which treatment options and fixation strategies may be of benefit, and which may cause undue harm to the patient. With all of these data gathered and analyzed the surgeon can carefully plan a surgical intervention that will mitigate risk of complication while allowing for healing of the pelvic ring non-union.
In this chapter the workup and management of a morbidly obese male with catastrophic hardware failure resulting in a painful pelvic ring non-union is detailed. It starts with a careful history followed by critical analysis of all lab work and identifies all patient risk factors to determine what can be modifiable prior to surgical intervention. Preferred imaging is reviewed to evaluate for subtle details of the pelvic ring injury. Once all patient factors and imaging are reviewed, only then the different treatment options can be efficiently assessed to determine which will provide the right balance of risk mitigation and fracture fixation.
After taking all these factors into account, a treatment strategy was devised and executed to repair the pelvic non-union in this patient. With thoughtfulness and meticulous planning the pelvic ring went on to heal and the patient was able to have an excellent outcome and return back to pre-injury levels of activity and work.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Holdsworth FW. Dislocation and fracture-dislocation of the pelvis. J Bone Joint Surg Br. 1948;470(8):461–6. https://doi.org/10.1007/s11999-012-2422-4.
Tornetta P III, Matta J. Outcome of operatively treated unstable posterior pelvic ring disruptions. Clin Orthop Relat Res. 1996;329:186–93.
Taguchi T, Kawai S, Kaneko K, Yugue D. Surgical treatment of old pelvic fractures. Int Orthop. 2000;24:28–32.
Papakostidis C, Kanakaris NK, Kontakis G, Giannoudis P, v. Pelvic ring disruptions: treatment modalities and analysis of outcomes. Int Orthop. 2009;33(2):329–38. https://doi.org/10.1007/s00264-008-0555-6.
McLaren A, Rorabeck C, Halpenny J. Long-term pain and disability in relation to residual deformity after displaced pelvic ring fractures. Can J Surg. 1990;33(6):492–4.
Yin Y, Luo J, Zhang R, et al. Anterior subcutaneous internal fixator (INFIX) versus plate fixation for pelvic anterior ring fracture. Sci Rep. 2019;9(1):2578. https://doi.org/10.1038/s41598-019-39068-7.
Vigdorchik JM, Esquivel AO, Jin X, Yang KH, Onwudiwe NA, Vaidya R. Biomechanical stability of a supra-acetabular pedicle screw internal fixation device (INFIX) vs external fixation and plates for vertically unstable pelvic fractures. J Orthop Surg Res. 2012;7(1):31. https://doi.org/10.1186/1749-799X-7-31.
Bi C, Wang Q, Wu J, et al. Modified pedicle screw-rod fixation versus anterior pelvic external fixation for the management of anterior pelvic ring fractures: a comparative study. J Orthop Surg Res. 2017;12(1):185. https://doi.org/10.1186/s13018-017-0688-7.
Carson JT, Shah SG, Ortega G, Thamyongkit S, Hasenboehler EA, Shafiq B. Complications of pelvic and acetabular fractures in 1331 morbidly obese patients (BMI ≥ 40): a retrospective observational study from the National Trauma Data Bank. Patient Saf Surg. 2018;12(1):26. https://doi.org/10.1186/s13037-018-0172-2.
Hupel TM, Mckee MD, Waddell J, Schemitsch EH. External fixation of rotationally unstable pelvic fractures in obese patients. J Trauma. 1998;45(1):111–5.
Dahill M, Mcarthur J, Roberts GL, et al. The use of an anterior pelvic internal fixator to treat disruptions of the anterior pelvic ring: a report of technique, indications and complications. Bone Joint J. 2017;99-B:1232. https://doi.org/10.1302/0301-620X.99B9.
Vaidya R, Colen R, Vigdorchik J, Tonnos F, Sethi A. Treatment of unstable pelvic ring injuries with an internal anterior fixator and posterior fixation: initial clinical series. J Orthop Trauma. 2012;26(1):1–8. www.jorthotrauma.com.
Fritz T, Mettelsiefen L, Strobel F, et al. A novel internal fixation method for open book injuries of the pubic symphysis—a biomechanical analysis. Clin Biomech. 2020;77:105009. https://doi.org/10.1016/j.clinbiomech.2020.105009.
Lange RH, Hansen ST. Pelvic ring disruptions with symphysis pubis diastasis indications, technique, and limitations of anterior internal fixation. Clin Orthop Relat Res. 1985;201:130–7. http://journals.lww.com/clinorthop.
Chip ML Jr, Ms RM. Evaluation of new plate designs for symphysis pubis internal fixation. Injury. 1996;41(3):498–502.
Lu Y, He Y, Li W, Yang Z, Peng R, Yu L. Comparison of biomechanical performance of five different treatment approaches for fixing posterior pelvic ring injury. J Healthc Eng. 2020;2020:5379593. https://doi.org/10.1155/2020/5379593.
Schildhauer TA, Ledoux R, Chapman JR, Bradford Henley M, Tencer F, Routt MLC. Triangular osteosynthesis and iliosacral screw fixation for unstable sacral fractures: a cadaveric and biomechanical evaluation under cyclic loads. J Orthop Trauma. 2003;17(1):22–31.
Sagi HC, Militano U, Caron T, Lindvall E. A comprehensive analysis with minimum 1-year follow-up of vertically unstable transforaminal sacral fractures treated with triangular osteosynthesis. J Orthop Trauma. 2009;23(5):313–21. www.jorthotrauma.com.
Marquez-Lara A, Nandyala SV, Sankaranarayanan S, Noureldin M, Singh K. Body mass index as a predictor of complications and mortality after lumbar spine surgery. Spine (Phila Pa 1976). 2014;39(10):798–804. https://doi.org/10.1097/BRS.0000000000000232.
Jiang J, Teng Y, Fan Z, Khan S, Xia Y. Does obesity affect the surgical outcome and complication rates of spinal surgery? A meta-analysis. Clin Orthop Relat Res. 2014;472(3):968–75. https://doi.org/10.1007/s11999-013-3346-3.
Nicodemo A, Capella M, Deregibus M, Massè A. Nonunion of a sacral fracture refractory to bone grafting: internal fixation and osteogenic protein-1 (BMP-7) application. Musculoskelet Surg. 2011;95(2):157–61. https://doi.org/10.1007/s12306-011-0131-x.
Giannoudis P, Psarakis S, Kanakaris NK, Pape HC. Biological enhancement of bone healing with bone morphogenetic protein-7 at the clinical setting of pelvic girdle non-unions. Injury. 2007;38S4:S43–8.
Lybrand K, Kurylo J, Gross J, Templeman D, Tornetta P. Does removal of the symphyseal cartilage in symphyseal dislocations have any effect on final alignment and implant failure? J Orthop Trauma. 2015;29(10):470–4.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2024 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Olszewski, N., Firoozabadi, R. (2024). Pelvic Fracture Failed Fixation. In: Giannoudis, P.V., Tornetta III, P. (eds) Failed Fracture Fixation. Springer, Cham. https://doi.org/10.1007/978-3-031-39692-2_18
Download citation
DOI: https://doi.org/10.1007/978-3-031-39692-2_18
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-39691-5
Online ISBN: 978-3-031-39692-2
eBook Packages: MedicineMedicine (R0)