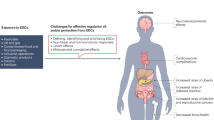
Abstract
Talking with patients and the public about endocrine-disrupting chemicals (EDCs) can be challenging for healthcare providers if they themselves are not well versed with the topic. Scientific and clinical evidence about environmental impacts on reproductive health have escalated exponentially over the past two decades, and this field can no longer be ignored or denied, as the consequences are significant, and many are preventable. EDCs are found in industrial- and e-waste, plastics, pesticides, preservatives, bedding, personal care products, household dust, diesel exhaust, air pollution, and humans and wildlife. They disrupt endocrine processes in the developing fetus, neonates, children, adolescents, and adults. These effects, along with lax toxicity regulations, make a compelling case for healthcare providers to understand the issues for appropriate counseling of patients and the public. Moreover, clinicians can also effectively advocate for change at governmental levels, complementing individual attempts to minimize personal risk. This chapter reviews recent advances enabling healthcare professionals in practice and in training to take an environmental history and talk with patients, the public, and policy makers about EDCs and resources to protect the reproductive health of this and future generations.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
11.1 Scope of the Problem
Over the past 75 years there has been a remarkable rise in noncommunicable diseases globally [1] that threaten reproductive health and capacity directly and indirectly. Genetic mutations at the population level in this timeframe are unlikely, and environmental chemical exposures have been considered as potential contributors due to marked increases in industrial chemical production occurring in parallel with the noncommunicable disease trends [2]. A recent study reports about 350,000 chemicals and mixtures registered globally, although most are unregulated in their production, disposal, and recycling with wide differences across countries and regions [3]. Many of these chemicals are EDCs (i.e., chemicals or mixtures of chemicals that affect any stage of human development [4]). EDCs are part of environmental chemical contaminants that are present in all populations studied [5], and it has been said that “babies are born pre-polluted” [6]. Exposures occur by ingestion, inhalation, trans-dermally, and trans-placentally, with greatest vulnerability pre-conceptually, during in utero development, neonatally, and in the adolescent period [7, 8]. EDCs are distributed widely, contaminating our air, water, soil, and food, and there is now strong experimental and epidemiologic evidence that EDCs harm reproductive health and outcomes—specifically gametogenesis, embryogenesis, reproductive tract development, fertility, pregnancy outcomes, and child neurodevelopment, which may be preventable in some cases by adopting mitigating strategies [8,9,10,11,12].
11.2 Empowering Healthcare Professionals to Talk with Patients and the Public About EDCs
Despite a voluminous amount of experimental evidence from animal models and in vitro cellular studies that provide the mechanistic underpinnings of these observations, as well as human epidemiologic and wildlife field data, EDC effects on reproduction are still not widely appreciated by the public and by healthcare professionals. In 2014, the American College of Obstetricians and Gynecologists (ACOG) published the 2012 survey of its ~50,000 members on the topic of prenatal environmental exposures [13]. Of the 2514 respondents, 78% said they believed they could reduce patient exposures to environmental health hazards through patient counseling. However, 50% reported rarely taking an environmental health history, <20% routinely inquired about exposures commonly found in pregnant women in the United States, and <7% had had any training on the topic. Barriers to counseling included lack of knowledge and uncertainty about the evidence, concerns that patients may not be able to reduce harmful exposures, and fears about provoking patient anxiety [13]. An important message from this survey was that physicians believed they could play a key role in preventing environmental exposures that harm patient health and reproductive outcomes, although they did not feel empowered to do so. Physician education, training, having reliable sources and following evidence-based guidelines, and having access to communication tools were identified as unmet needs that could enhance the impact of physicians talking with patients about environmental exposures and mitigating strategies.
In the intervening years (2012–present), there has been a plethora of educational opportunities for physicians and other healthcare professionals and researchers regarding EDCs and reproductive health. Systematic and narrative reviews, opinions, and white papers on this topic have been issued by leading global organizations (e.g., UNEP-WHO [14]), and professional societies and their committees, e.g., the Royal College of Obstetricians and Gyneacologists [15]; the American College of Obstetricians and Gynecologists [16, 17]; The Endocrine Society [9, 11]; the International Federation of Gynaecology and Obstetrics (FIGO) [7, 18]; and Project TENDR [19], who have acknowledged the need for educating their constituents with information passed to patients and the public at large. These organizations, which are reliable and respected sources, have convened experts and collaborated with patient advocate groups to examine the evidence and provide educational guidance in the form of webinars, scholarly works, systematic reviews, and calls to action about the effects of EDCs on reproductive health. Some are developing educational modules to train the trainers; for example, the Philippine Obstetrical and Gynecological Society (https://pogsinc.org/) Subcommittee on Reproductive and Developmental Environmental Health (RDEH) developed a “Training of Trainers on RDEH” post-graduate course for their Annual meeting in September 2021 that was attended by over 100 participants. Moreover, some institutions are developing courses for undergraduates and medical and graduate students about EDCs and other toxic environmental exposures, laying the ground for a more informed and empowered work force in the future.
11.3 Taking An Environmental Exposure History
In July 2021, ACOG published an update to its Committee Opinion of 2013 [16] that demonstrated remarkable advances in the field and tools for empowering clinicians. Therein, it underscored the importance for obstetrical healthcare providers to be knowledgeable regarding EDCs and presented approaches for exposure risk assessment and risk reduction strategies, as well as clinical counseling [17]. ACOG suggested key elements of an environmental exposure history, reported associations with reproductive health outcomes, and recommended counseling approaches for patients to minimize exposure to toxic environmental agents—most of which are EDCs. Elements in the environmental history included: lead exposures, home environment and lifestyle (e.g., cigarette smoking, flame retardants in foam furniture), cleaning products, pesticides, personal care products, diet, nutrition, produce, food preparation and storage containers, fast foods, and occupational exposures. While the Committee Opinion was focused on obstetric care clinicians, the recommendations and conclusions apply equally well to those contemplating pregnancy and, also, anyone undergoing fertility evaluation and treatment.
The University of California San Francisco (UCSF) Program on Reproductive Health and the Environment (PRHE) hosts an extensive website for clinicians, researchers, patients, and families. Specifically relevant to clinicians are the links to environmental history forms at http://prhe.ucsf.edu/prhe/clinical_resources.html, replete with references and links to additional clinically relevant information. Also key in environmental history taking are several items that complement the ACOG recommendations:
-
1.
Assessing patient risk including toxicant, dose, frequency, duration and route of exposure, timing to vulnerable developmental windows, and comorbidities.
-
2.
Inquiring about hazardous occupations and hobbies.
-
3.
Underscoring behaviors that can reveal possible mitigation strategies during history taking that can help minimize exposures.
Thus, environmental exposure history assessment has expanded the practitioner’s access to risk assessment for individual patients, and some practices have incorporated “smart sets” in electronic medical record as checklists and for efficiency of information gathering.
11.4 Patient (and Clinician) Resources
Several groups have also put together valuable resources for clinicians to provide to patients and their families or to be accessed directly by the public. Some examples are [8]:
-
Patient- and family-friendly information is available on the UCSF PRHE website as down loadable brochures (“Toxic Matters,” “Food Matters,” “Work Matters,” “Pesticides Matter”), in English and Spanish (http://prhe.ucsf.edu/prhe/families.html) (Fig. 11.1a). These can be printed and distributed in waiting rooms, doctors’ offices, or included in new patient information packages and are downloadable, free of charge, from the website.
-
The Environmental Working Group and Skin Deep website has commentaries and updates on current environmental issues and consumer information (http://www.ewg.org/ They host a searchable database of personal care products detailed and ranked by toxicity of ingredients (http://www.weg.org/skindeep/) that is available free of charge.
-
SafetyNest is a personalized health education platform for prenatal care. It has an app that enables clinicians and pregnant women with a toolkit to reduce diseases and adverse events liked to toxic chemical exposures (http://www.nysafetynest.org/).
-
The International Federation of Gynaecology and Obstetrics (FIGO) is a global professional organization that has collaborated with UCSF PRHE and nonprofit organizations, e.g., Health and the Environment (HEAL), the National Resources Defense Council (NRDC) (https://www.nrdc.org/), and the FREIA Project (http://freiaproject.eu/wp/subscribe/) to produce scholarly, evidence-based information about EDCs and mostly reproductive outcomes. Recently, FIGO, HEAL, and PRHE have produced patient infographics regarding EDCs and pregnancy in several languages (https://www.figo.org/reproductive-and-developmental-environmental-health-committee). An example is shown in Fig. 11.1b that can be of value for practical steps patients and the public can take to minimize EDC risk.
Patient educational materials. (a) Patient brochures about environment and reproductive health freely downloadable from https://prhe.ucsf.edu. (b) Patient infographic on toxic chemicals and pregnancy available from https://www.figo.org
11.5 Resources for Healthcare Professionals, Trainees, and Others
While the resources above are valuable for patients and the public, they are equally valuable for healthcare professionals to increase awareness among themselves and their colleagues, as well as for patients and the public. Some additional resources include:
-
The Endocrine Disruptor Exchange (TEDX (http://www.endomcrinedisruption.org/). TEDX has a database of ~10,000 chemicals with endocrine disruption potential and also has an interactive timeline of critical windows of EDC exposures during development of several organ systems based on animal and human studies (http://www.endocrinedisruption.org/prenatal-origins-of-endocrine-disruption/critical-windows-of-development/timeline-test/). This is a valuable resource to clinicians, trainees and others to understand these critical periods of vulnerability to EDC effects.
-
The Collaborative on Health and the Environment (CHE) is a U.S.-based nongovernmental organization whose mission is to engage scientific dialogue on environmental impacts on human health (http://www.healthandenvironment.org/), with the ultimate goal of disease and disability prevention. Their website contains linkages between chemical contaminants and ~ 200 human diseases and disorders that can be searched by disease or chemical (http://www.healthandenvironment.org/tddb/).
-
The UCSF Program for Reproductive Health and the Environment (PRHE) hosts a website (http://ucsf.prhe.edu) replete with references of EDC exposures and effects on reproductive health, as well as updates on health policies mainly in the United States, but also around the globe.
-
The Endocrine Society has published two major scientific statements about EDCs [9, 11] which give abundant, evidence-based information about the chemicals and their effects on all endocrine systems derived from experimental animal models and human epidemiologic studies. Moreover, the Society hosts an up-to-date website about EDCs and human health, of use to researchers, clinicians, and patients (https://www.hormone.org/your-health-and-hormones/endocrine-disrupting-chemicals-edcs).
-
The International Federation of Gynaecology and Obstetrics (FIGO) through its Committee on Reproductive Health and the Environment (name changed in 2021 to the Committee on Climate Change and Toxic Environmental Exposures) periodically issues white papers and publishes in peer-reviewed manuscripts on the effects of EDCs and other environmental toxicants on reproductive health (http://www.FIGO.org). It issued a major treatise on EDCs and reproductive health in 2015 [7] and has a recent publication on climate change with citations about the interplay of climate change, air pollution, and EDCs [18] that is valuable for healthcare professions to know.
-
The American College of Obstetricians and Gynecologists has just updated its Committee Opinion on “Reducing Prenatal Exposures to Environmental Chemicals” available at:
https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2021/07/reducing-prenatal-exposure-to-toxic-environmental-agents. This is a valuable resource for clinicians in practice and those in training.
11.6 Talking with Patients and the Public About EDCs and Risk Assessment and Mitigation
Healthcare providers have multiple options for discussing EDCs and reproductive health with their patients—in the office, providing resources to be accessed online or to be read in hard copy at home, talking at community gatherings, religious events, health fairs, schools, parent meetings, and other venues. Physician voices are respected and carry much weight, and the ability to prevent harm is huge, along with increased patient and public health safety [20]. Using guidelines and recommendations from professional organizations can facilitate healthcare professionals’ knowledge base and comfort level in addressing these issues, which are so important to minimize risk.
11.7 How Healthcare Providers Can Advocate for Change
Some professional societies have assembled white papers, systematic reviews, and other documents to prepare healthcare professionals to advocate for laws that transcend individual, personal behavior in mitigating risks and commit governments to prioritize environmental impacts on health as part of their political and economic agendas. Healthcare providers and scientists have powerful voices in legislative bodies and forums to advocate for changes in health policies to protect the public health from EDCs and other environmental threats. Primers have been developed, e.g., by the Endocrine Society in collaboration with the IPEN, a leading global network of 700 nongovernmental organizations working in more than 100 developing countries and countries with economies in transition [21]. These efforts are essential in parallel to individual efforts to minimize harm for this and future generations.
11.8 What Will It Take for People to Pay Attention to EDCs and Human Health?
The question arises what it will take to get people’s attention (individuals and governments) to prioritize environmental health. A recent commentary suggests that there are three key data elements to quantify the health burden of specific industrial chemicals [22]. These include the relationship between exposures and health outcomes, the prevalence of the exposures, and monetary cost per case of illness [22]. The analytical approaches and quality and accuracy of the data are key for all three areas. Education and dialogue are critical components of raising awareness of the issues and priority setting.
11.9 Summary
Physicians and other healthcare professionals are uniquely positioned to talk with patients about EDCs and reproductive health, and it is essential that patients and the public are aware of EDCs and their effects on reproductive health and children’s health and ways to mitigate these impacts. Also, voices of clinicians and scientists can be powerful in advocating for environmental health policy changes at the local and national levels to protect the public health. Moreover, individuals and groups can also make a huge difference by letting leaders know what health issues are important to them, what the importance of reproductive environmental health is to this and future generations, and why it should be prioritized in local and national health agendas. By so doing, patients, the general public, and professional and political leaders can and should work together toward equitable and impactful solutions for this and future generations.
References
WHO. 2021. https://www.who.int/health-topics/noncommunicable-diseases#tab=tab_1. Accessed 17 Oct 2021.
Kumar M, Sarma DK, Shubham S, Kumawat M, Verma V, Prakash A, Tiwari R. Environmental endocrine-disrupting chemical exposure: role in non-communicable diseases. Front Public Health. 2020;8:553850. https://doi.org/10.3389/fpubh.2020.55385.
Wang Z, Walker GW, Muir DCG, Nagatani-Toshida K. Toward a global understanding of chemical pollution: a first comprehensive analysis of national and regional chemical inventories. Environ Sci Technol. 2020;54:2575–84.
Zoeller RT, Brown TR, Doan LL, Gore AC, Skakkebaek NE, Soto AM, Woodruff TJ, Vom Saal FS. Endocrine-disrupting chemicals and public health protection: a statement of principles from the Endocrine Society. Endocrinology. 2012;153:4097–110.
Woodruff TJ, Zota AR, Schwartz JM. Environmental chemicals in pregnant women in the United States: NHANES 2003–2004. Environ Health Perspect. 2011;119:878–85.
US DHHS. President’s cancer panel 2008–2009 annual report 2010. 2010. https://deainfoncinihgov/advisory/pcp/annualreports/pcp08-09rpt/pcp_report_08-09_508.pdf. Accessed 17 Oct 2021.
Di Renzo GC, Conry JA, Blake J, DeFrancesco MS, DeNicola N, Martin JN, McCue KA, Richmond D, Shah A, Sutton P, Woodruff TJ, van der Poel SZ, Giudice LC. International Federation of Gynecology and Obstetrics opinion on reproductive health impacts of exposure to toxic environmental chemicals. Int J Gynaecol Obstet. 2015;131:219–25.
Giudice LC, Zlatnik MG, Segal T, Woodruff TJ. Environmental factors and reproduction. In: Strauss JF, Barbieri R, Dokras A, Williams CJ, Williams Z, editors. Yen & Jaffe’s Reproductive Endocrinology: Physiology, Pathophysiology, and Clinical Management. 9th ed. Amsterdam: Elsevier; 2021a.
Diamanti-Kandarakis E, Bourguignon JP, Giudice LC, Hauser R, Prins GS, Soto AM, Zoeller RT, Gore AC. Endocrine-disrupting chemicals: an Endocrine Society scientific statement. Endocr Rev. 2009;30:293–342.
Giudice LC. Environmental impact on reproductive health and risk mitigating strategies. Curr Opin Obstet Gynecol. 2021;33(4):343–9.
Gore AC, Chappell VA, Fenton SE, Flaws JA, Nadal A, Prins GS, Toppari J, Zoeller RT. EDC-2: the Endocrine Society's second scientific statement on endocrine-disrupting chemicals. Endocr Rev. 2015;36(6):E1–E150. https://doi.org/10.1210/er.2015-1010.
Segal TR, Giudice LC. Before the beginning: environmental exposures and reproductive and obstetrical outcomes. Fertil Steril. 2019;112:613–21.
Stotland NE, Sutton P, Trowbridge J, Atchley DS, Conry J, Trasande L, Gerbert B, Charlesworth A, Woodruff TJ. Counseling patients on preventing prenatal environmental exposures–a mixed-methods study of obstetricians. PLoS One. 2014;9(6):e98771. https://doi.org/10.1371/journal.pone.0098771.
Bergman A, Heindel JJ, Jobling S, et al. State of the science of endocrine disrupting chemicals 2012. An assessment of the state of the science of endocrine disruptors prepared by a group of experts for the United Nations Environment Programme and World Health Organization, Geneva. 2013. www.who.int/ceh/publications/endocrine/en/.
Royal College of Obstetricians and Gynaecologists. Guideline: chemical exposures during pregnancy (Scientific impact paper 37). 2013. https://rcog.org.uk/guidance/browse-all-guidance/scientific-impact-papers/chemical-exposures-during-pregnancy-dealing-with-potential-but-unproven-risks-to-child-health-scientific-impact-paper-no-37/. Accessed 17 Oct 2021.
ACOG. American College of Obstetricians and Gynecologists Committee on Health Care for Underserved Women, American Society for Reproductive Medicine Practice Committee, The University of California San Francisco & Program on Reproductive Health and the Environment: Exposure to toxic environmental agents. Committee Opinion No. 575 Companion Piece, Washington, DC. 2013.
ACOG. Committee opinion, committee on obstetric practice, DeNicola N, Borders AE, Singla V, Woodruff TJ. No. 832, Washington DC. 2021.
Giudice LC, Llamas-Clark EF, DeNicola N, Pandipati S, Zlatnik MG, DCD D, Woodruff TJ, Conry JA, FIGO Committee on Climate Change and Toxic Environmental Exposures. Climate change, women’s health, and the role of obstetricians and gynecologists in leadership. Int J Gynaecol Obstet. 2021b;155(3):345–56.
Bennett D, Bellinger DC, Birnbaum LS, et al. Project TENDR: targeting environmental neuro-developmental risks the TENDR consensus statement. Environ Health Perspect. 2016;124(7):A118–22.
Sweeney E. The role of healthcare professionals in environmental health and fertility decision-making. J Environ Occup Health policy. 2017;27:28–50.
Gore AC, Crews D, Doan LL, La Merrill M, Patisaul H, Zota A. Introduction to endocrine disrupting chemicals. A guide for public interest organizations and policy-makers. 2014. https://ipen.org/sites/default/files/documents/ipen-intro-edc-v1_9a-en-web.pdf. Accessed 17 Oct 2021.
Woodruff TJ. Making it real–the environmental burden of disease. What does it take to make people pay attention to the environment and health? J Clin Endocrinol Metab. 2015;100:1241–4.
Acknowledgments
The author acknowledges the efforts of individuals and leaders across the globe who have contributed to increasing knowledge and awareness about environmental effects on the reproductive health of this and future generations and strategies to mitigate them.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Ethics declarations
The Robert B. Jaffe, MD, Professorship in the Reproductive Sciences in the Department of Obstetrics, Gynecology and Reproductive Sciences at the University of California, San Francisco, enabled the author’s effort for this contribution.
Conflicts of Interest
The author is Chair of the FIGO Committee on Climate Change and Toxic Environmental Exposures, a voluntary position, and has no financial conflicts of interest related to this manuscript.
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2023 The Author(s)
About this chapter
Cite this chapter
Giudice, L.C. (2023). Talking with Patients and the Public About Endocrine-Disrupting Chemicals. In: Marci, R. (eds) Environment Impact on Reproductive Health. Springer, Cham. https://doi.org/10.1007/978-3-031-36494-5_11
Download citation
DOI: https://doi.org/10.1007/978-3-031-36494-5_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-36493-8
Online ISBN: 978-3-031-36494-5
eBook Packages: MedicineMedicine (R0)